Abstract
The Global Health Security Agenda aims to improve countries' ability to prevent, detect, and respond to infectious disease threats by building or strengthening core capacities required by the International Health Regulations (2005). One of those capacities is the development of surveillance systems to rapidly detect and respond to occurrences of diseases with epidemic potential. Since 2015, the US Centers for Disease Control and Prevention (CDC) has worked with partners in Sierra Leone to assist the Ministry of Health and Sanitation in developing an Integrated Disease Surveillance and Response (IDSR) system. Beginning in 2016, CDC, in collaboration with the World Health Organization and eHealth Africa, has supported the ministry in the development of Android device mobile data entry at the health facility for electronic IDSR (eIDSR), also known as health facility–based eIDSR. Health facility–based eIDSR was introduced via a pilot program in 1 district, and national rollout began in 2018. With more than 1,100 health facilities now reporting, the Sierra Leone eIDSR system is substantially larger than most mobile-device health (mHealth) projects found in the literature. Several technical innovations contributed to the success of health facility–based eIDSR in Sierra Leone. Among them were data compression and dual-mode (internet and text) message transmission to mitigate connectivity issues, user interface design tailored to local needs, and a continuous-feedback process to iteratively detect user or system issues and remediate challenges identified. The resultant system achieved high user acceptance and demonstrated the feasibility of an mHealth-based surveillance system implemented on a national scale.
During the 2014-2016 West African Ebola epidemic, the US Centers for Disease Control and Prevention (CDC) initiated multiple activities in Sierra Leone under the Global Health Security Agenda (GHSA). 1 The purpose of GHSA is to improve countries' ability to prevent, detect, and respond to infectious disease threats through core capacities required by the International Health Regulations (IHR 2005). 2 GHSA efforts are categorized into 11 “action packages” that correspond to specific technical areas.1,3 In the “real-time surveillance” and “reporting” action packages, CDC and the World Health Organization (WHO) supported the Sierra Leone Ministry of Health and Sanitation (MoHS) and partners to revitalize an Integrated Disease Surveillance and Response (IDSR) system in 2015.4,5 Originally, IDSR was paper-based. The ministry and partners implemented electronic reporting, including mobile-device–based reporting, beginning in 2016. 6
The use of mobile devices for health applications—whether for surveillance, reference, or clinical guidance—is commonly described as “mHealth.” Although previous literature has documented effective implementation of mHealth for public health surveillance,7-11 including IDSR, 12 most reports have described pilot programs or small-scale implementations (fewer than 50 sites). A 2013 review observed that there is “a lack of [literature documenting] mHealth applications and services operating at scale in low- and middle-income countries.” 13 Based on our successful implementation of a nationwide system, this report contributes an answer to that deficit.
Methods I: System Development/Implementation
Initially, IDSR was a paper-based system implemented at health facilities including hospitals and peripheral health units across Sierra Leone. An IDSR focal person at each health facility completed a paper weekly reporting form, compiling total suspected cases of 26 priority diseases or conditions (Table 1) from the health facility's clinical (paper) register. Focal persons submitted IDSR data via telephone or hard copy to the district surveillance officer at their district health management team office. District surveillance officers would compile reports from all health facilities into a weekly summary, which was submitted to the national surveillance program by email.
Integrated Disease Surveillance and Response (IDSR) priority diseases and conditions reported weekly in Sierra Leone
Source: Sierra Leone Technical Guidelines for Integrated Disease Surveillance and Response
To increase timeliness and completeness of reporting and to facilitate analysis, the Ministry of Health and Sanitation initiated electronic IDSR (eIDSR) in 2015 with support from CDC, WHO, eHealth Africa, and other partners. eIDSR was rolled out in 2 phases:
Phase 1: Computers, internet, and data entry staff were placed in district health management teams. A national web-based surveillance database was developed on the open-source District Health Information System 2 (DHIS2), 14 and district health management team personnel were trained to enter weekly data into a secure eIDSR website. Only the district team used eIDSR during Phase 1; health facility focal persons continued to use paper forms until Phase 2.
Phase 2: eIDSR was implemented at the health facility level using Android tablets for data entry with district-level review of submissions. Health facility–based eIDSR is the first at-scale use of mobile systems for healthcare (mHealth) in Sierra Leone.
eIDSR Mobile App Development
Development of health facility–based eIDSR was overseen by a technical working group consisting of representatives from the Ministry of Health and Sanitation, CDC, WHO, and eHealth Africa. The technical working group developed initial requirements for health facility–based eIDSR (Table 2 and Figure 1). The requirements specified that the mobile application would enable data entry directly from health facilities to the national database, incorporate data validation, and have the capacity to transmit data both via internet and text messages using short message service (SMS) or short message peer-to-peer (SMPP) communication modes.
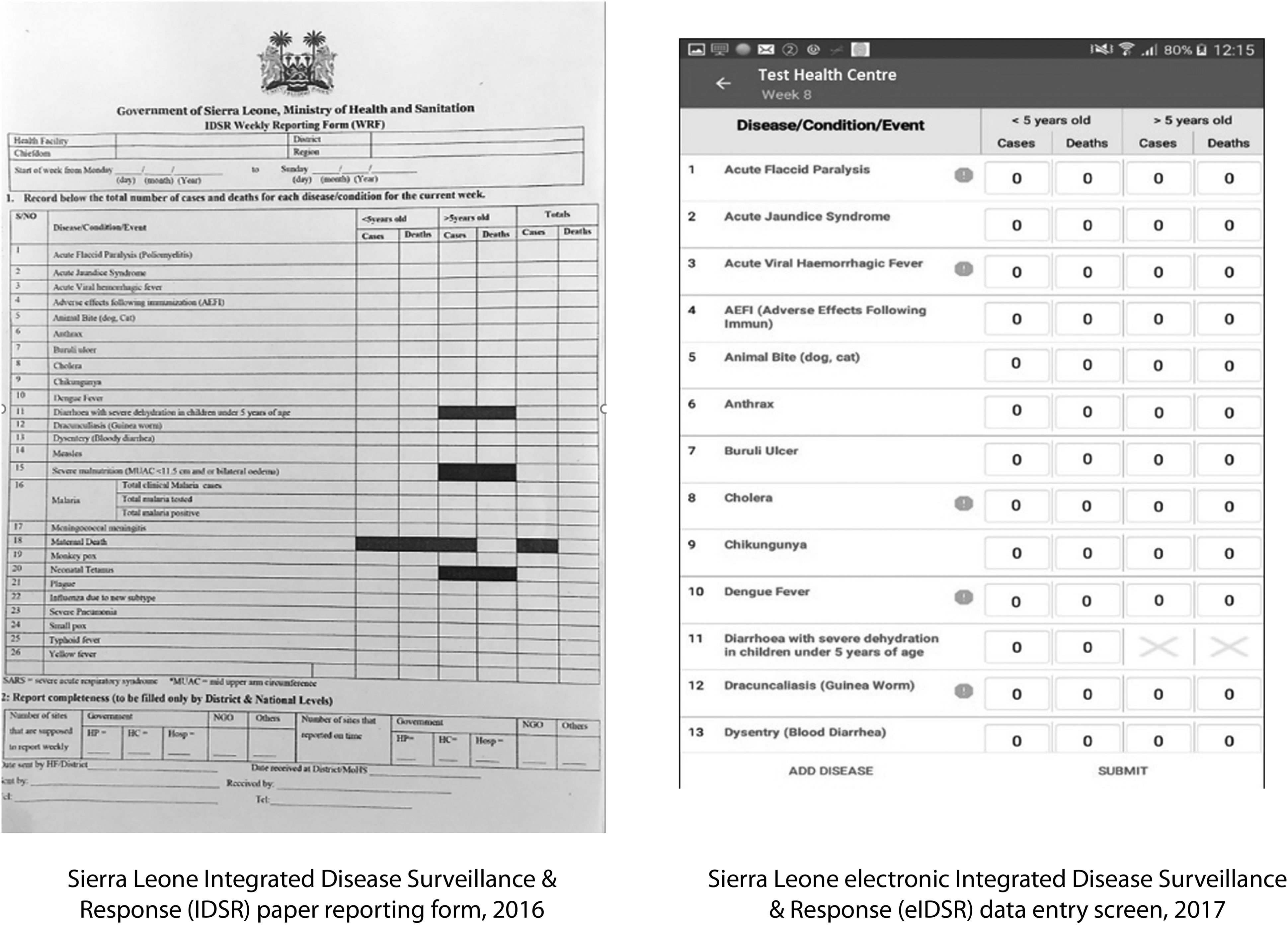
IDSR Paper Form and Health Facility–Based eIDSR App Entry Screen, Sierra Leone, 2017
Initial Requirements for the Health Facility–based Electronic Integrated Disease Surveillance and Response (eIDSR) Mobile Application
While DHIS2 remained the foundation for health facility–based eIDSR, incorporating the requirements outlined in Table 2 required substantial custom programming, including a new mechanism to receive SMS/SMPP messages. eHealth Africa performed these modifications for Sierra Leone, and all code has been submitted to DHIS2 repositories.
Health facility–based eIDSR was first implemented at 6 health facilities in the Port Loko district during November and December 2016. Subsequent cohorts were initiated in April and May 2017. National rollout to the remaining 13 districts began in April 2018 and was completed in June 2019.
Personnel from all IDSR-reporting health facilities were trained on eIDSR applications and procedures. They were issued tablets with software and mobile data installed. Trained health facility personnel reported in parallel, using both paper and the mobile application, and were monitored until the district achieved quality metrics set by the technical working group. Once approved, health facility–based eIDSR became the sole reporting method.
Methods II: System Assessment/Data Analysis
A mixed-methods approach was employed to assess system performance. Continuous-feedback monitoring during development and throughout deployment provided rapid visibility into operational issues and permitted iterative improvements. Usability, user acceptance, and data quality were assessed among pilot users, and results were returned to the continuous-feedback process. Finally, overall system performance was assessed through centralized data analysis.
Continuous Feedback
System performance and user experience were continuously assessed through technical support calls and direct observation of users in training and at their work locations. As issues were identified, they were addressed through iterative updates to both the eIDSR application and the back-end system (Table 3).
Continuous-Feedback Implementation for Sierra Leone Electronic Integrated Disease Surveillance & Response (eIDSR) mobile system: Issues and Solutions
Usability/User Acceptance Assessment
In July 2017, a usability/user-acceptance assessment was conducted in Port Loko. Of 112 health facilities that were then operational for facility-based eIDSR, 47 were assessed. Facilities were selected to represent varying levels of mobile connectivity, physical accessibility, and frequency of recent reports to the IDSR database in DHIS2.
Methodology consisted of a structured interview and direct observation of each user demonstrating basic operational tasks and completing a mock eIDSR report submission. The user was asked interview questions and answered using a 5-point Likert scale from “strongly agree” to “strongly disagree.” For operational tasks and data entry, observers rated each user as showing no experience, novice (limited experience), intermediate (demonstrated practical ability to use the application), or expert (demonstrated full and confident ability) capacity.
Assessments were conducted at the health facility where the focal person normally worked, except for 6 health facilities that were inaccessible because of flooding during this period. On-site assessments permitted observation of functionality issues, such as app and network performance, that were not readily apparent in training locations. Issues observed were incorporated into the continuous-feedback process described above.
Data Quality
Data quality was assessed simultaneously with user acceptance. Data were collected from weekly reporting forms, health facility–based eIDSR application logs, and the national DHIS2 database. Numbers reported for suspected malaria cases and deaths from June 5 to July 2, 2017, were compared among all 3 sources. Malaria was chosen because it is the only condition for which cases reported are consistently greater than zero.
System Performance
To assess overall system performance, data on eIDSR submissions from April 9 to June 16, 2019, were exported from DHIS2 and analyzed using R 3.6.0. 15 Communication mode for reports was categorized as manual (paper-based), mobile internet, or mobile SMS/SMPP.
Results
Continuous Feedback
This process identified multiple issues with the health facility–based eIDSR application as initially implemented. Issues detected and solutions implemented appear in Table 3.
Usability and User Acceptance
Of 47 users assessed, 43 (91%) reported preference for tablet-based eIDSR over paper-based reporting. A total of 46 (98%) agreed or strongly agreed with the statement, “I find the eIDSR mobile application easy to navigate,” and all 47 (100%) agreed or strongly agreed with the statement, “I feel very confident using the eIDSR mobile application.” Of the 47 respondents, 35 (74%) were evaluated by the observers as expert, 6 (13%) as intermediate, and 6 (13%) as novice.
Data Quality
Of 188 reports assessed for data quality, 138 (74%) had complete records in paper logs, health facility–based eIDSR application, and DHIS2. Of these 138 reports, 126 (91%) were identical in all 3 sources, and 12 (9%) had at least 1 disagreement between sources. Discordant records showed disagreement between paper-based report and health facility–based application reporting log. Five of 138 (3.6%) also showed disagreement between the application and DHIS2.
System Performance
As health facility–based eIDSR rolled out nationally, the proportion of IDSR submissions from health facilities through paper forms (manual) decreased and mobile submissions increased (Figure 2), while the number of facilities reporting remained roughly constant. The proportion of submissions using mobile-internet compared to mobile-SMS/SMPP modes fluctuated with varying network conditions.
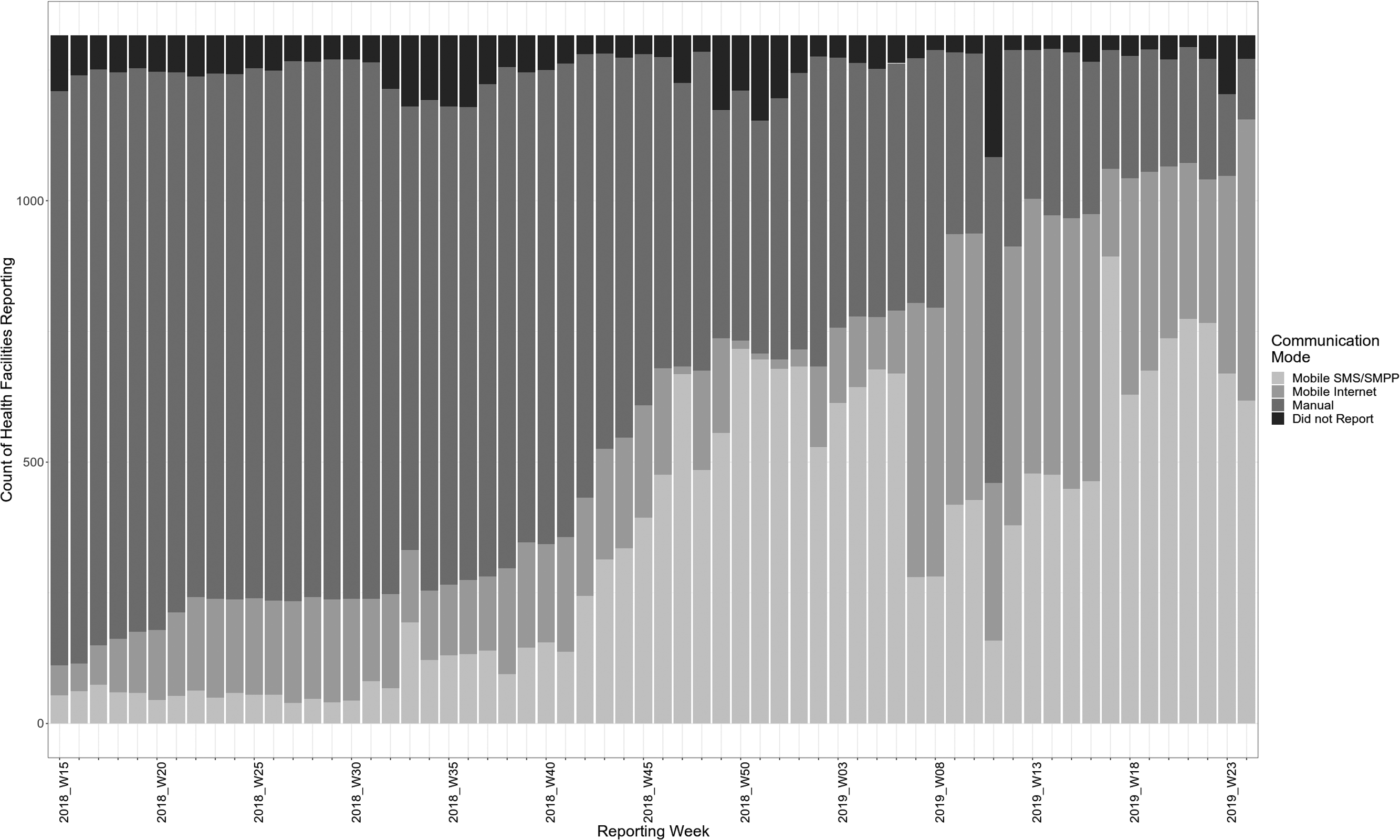
Weekly Electronic Integrated Disease Surveillance and Response (eIDSR) Submissions from Health Facilities, by Communication Mode, Sierra Leone, April 9, 2018 through June 16, 2019
As of June 10, 2019, a total of 1,316 health facilities from all 14 Sierra Leone districts had been trained in health facility–based eIDSR. On that date, of these health facilities, 1,156 (88%) submitted reports using the mobile application, 116 (9%) by manual reporting, and 44 (3%) failed to report. Of the 1,156 that reported through the eIDSR application, 538 (47%) submitted by internet and 618 (53%) by SMS/SMPP.
Discussion
Sierra Leone successfully implemented health facility–based electronic reporting of IDSR data on a national scale, with nearly 90% of health facilities reporting through eIDSR. In November 2016, the official Joint External Evaluation (JEE) of Sierra Leone's GHSA targets scored indicator D.2.2, an “interoperable, interconnected electronic real-time reporting system,” at level 2 out of 5 (limited capacity). 16 In the future, eIDSR may help Sierra Leone reach IHR compliance and potentially raise the JEE D.2.2 score.
A major strength of our assessment is that it covers the countrywide implementation of Sierra Leone's health facility–based reporting system. Multiple studies have discussed the usefulness of mHealth in improving healthcare delivery or reporting in lower-income countries, but they tend to describe small-scale interventions.7-12 With more than 1,100 health facilities in all 14 districts reporting via mobile health facility–based eIDSR, Sierra Leone has demonstrated successful scaling of an mHealth application in public health surveillance.
Several publications have reported health workers' ability to use mHealth applications, even with little or no prior computer experience.17,18 Our user-acceptance assessment reported high (>90%) acceptance of the mobile eIDSR application, and over 80% of users demonstrated at least intermediate skill in its use. Braun and colleagues describe the value of in-software guidance to users. 19 Through the continuous-feedback process, we observed that user-guidance and confirmation-of-submission modifications markedly improved usability of the application for health facility–based end-users.
Continuous-feedback design was vital to the success of health facility–based eIDSR and helped to identify issues of usability and function. Although not commonly described in public health literature, the principle of continuous user feedback is well known in software development.20-22 As Kazi and colleagues observed, “… iterative development with early and continuous engagement of end users ensures that the final product is efficient and usable, both key to widespread adoption.” 11 We concur with this observation and would add that monitoring users' experience in their actual work environments also provides vital insights into real-world operational issues and identifies needs for additional training.
The importance of improving internet connectivity for global health has been described elsewhere.5,23,24 Phalkey and colleagues 24 observed that ineffective communication and transport systems adversely affect surveillance systems. Coverage throughout Sierra Leone ranges from locations with stable mobile data, to locations where only voice or SMS are accessible, to locations where there is no signal at all. In some remote health facilities, focal persons reported having to walk or ride some distance to a spot where they could obtain a signal. Furthermore, mobile connectivity in Sierra Leone is supplied by several providers, and the geographic coverage for each provider is variable. It is crucial to monitor shifts in connectivity that may happen during the life of a program, which may affect reporting rates. Mitigation strategies described here may become less important as network infrastructure improves.
Diwan and colleagues 25 observed that functionality to store data for later transmission helps to address network limitations, and the Sierra Leone experience supports this observation. Our innovation in capacity to transmit by both internet and text may be a useful adaptation to consider in locations with connectivity challenges. Our results demonstrate that SMS/SMPP capacity remains an important conduit for eIDSR in Sierra Leone, even among facilities that sometimes have mobile internet access.
Our text compression modification was of vital importance to system functionality. Initially, the mobile app coded a single report into a series of 6 to 7 text messages transmitted in sequence; however, in areas with a weak signal, reports sometimes failed when not all messages were successfully transmitted. Compression to a single text message mitigated risk of transmission failure. In-app confirmation to users of submission success or failure and reminders for unsubmitted reports are also important.
This work is subject to a few limitations. First, this report is restricted to technical aspects of system implementation and operation and does not address eIDSR effectiveness for public health surveillance. Data quality as addressed in this report refers to completeness and concordance between data at health facilities and that reported to the system. A more robust evaluation according to CDC surveillance evaluation guidelines 26 would include measures of actual disease reports and outbreaks detected. Such an evaluation would require additional on-site assessments beyond the scope of and resources available to this project and is recommended as a future strategy.
Second, usability and data quality were assessed at only 47 early-implementation health facilities, which may not be representative of all health facilities. While we believe the large scale of present implementation implies high user acceptance, additional evaluations could confirm our results and reassess data quality.
The final limitation is the question of sustainability. Continued success of health facility–based eIDSR in Sierra Leone depends on ongoing support for technical staff to maintain, update, and troubleshoot the system. Sierra Leone's technical innovations have been shared with the DHIS2 community, and incorporation into the core software may mitigate future support costs; however, continued financial support for mobile data contracts and software subscriptions is necessary.
Although the Ministry of Health and Sanitation strongly supports the eIDSR initiative, both staffing and financial requirements currently depend on external partners. 27 As with any innovation in a low-resource environment, long-term ownership and sustainability depend on reconciliation of many priorities competing for limited funds.
Conclusion
The Sierra Leone health facility–based eIDSR system successfully receives and consolidates eIDSR reports from more than 1,100 health facilities in 14 districts. Staff at these facilities have demonstrated the ability to learn and operate tablet-based reporting software. Other countries implementing electronic surveillance or mHealth activities in resource-constrained settings may benefit from several lessons learned:
1. mHealth depends on reliable network connectivity. Adverse impacts of limited or variable connectivity can be mitigated through:
Functionality to store data for transmission when on-network;
Capacity to transmit data by multiple modes, such as internet and SMS/SMPP;
Data compression to limit size and quantity of transmitted messages; and
Use of multiple data providers to maximize coverage.
2. An application that is easy to use is more likely to be accepted and used successfully. mHealth application design should incorporate features such as context-specific data checks and feedback messages adapted to end-users. Error messages should highlight specific actions required and be validated through field-testing with end-users.
3. Continuous user feedback and rapid integration of modifications can enhance overall system quality and user acceptance.
The success of eIDSR in Sierra Leone demonstrates the feasibility of national-scale, facility-based, mHealth surveillance systems in limited-resource settings. Other countries may consider similar efforts to enhance their surveillance and reporting for global health security purposes.
Footnotes
Acknowledgments
The authors acknowledge the contributions of Regan Hartman for manuscript review and Adaeze Ogee-Nwankwo for user-acceptance data collection. We further acknowledge the many public health professionals whose labor has supported and continues to support eIDSR in Sierra Leone.
