Abstract
The rapid growth of telehealth for healthcare delivery has exposed the lack of training available in North America to prepare all levels of clinicians for this modality. Issues range from care coordination to legal and ethical implications to new ways of engaging patients. This article describes a comprehensive curriculum for telehealth training developed at Thomas Jefferson University. The core curriculum is intended for all levels of clinicians as telehealth facilitators and uses the Jefferson Interactive Curricula Experience (iCE) Platform and Application. A targeted curriculum has been developed for a fellowship in emergency medicine to prepare high level researchers and leaders in telehealth.
The Growth of Telehealth
The anticipated shift from fee for service to value-based care has created the need to develop new care delivery models that encompass both the provision of chronic care as well as acute unscheduled (or on-demand) care. The JeffConnect telemedicine program at Thomas Jefferson University (TJU) includes patient-friendly solutions around the whole continuum of care: whether the patient is seeking chronic care while at their baseline; is becoming “a little sick,” while falling off the baseline; or requiring acute care interventions in a distant setting. Next generation providers will need to be able to deliver next generation medical care, including telehealth.
This is one of the first ever publications of a comprehensive academic curriculum for training clinicians, fellows and students in telehealth. We're proud to offer it as the first peer-reviewed manuscript in Healthcare Transformation.
Developing a Telehealth Curriculum
To address this shift in healthcare practice and care coordination, we describe a series of training programs to facilitate incorporation of knowledge of telehealth into medical training. In this article, we focus predominantly on the telehealth facilitator certificate program, but also briefly describe other programs being offered within our university.
“Research shows that Telehealth can enhance quality of care.”
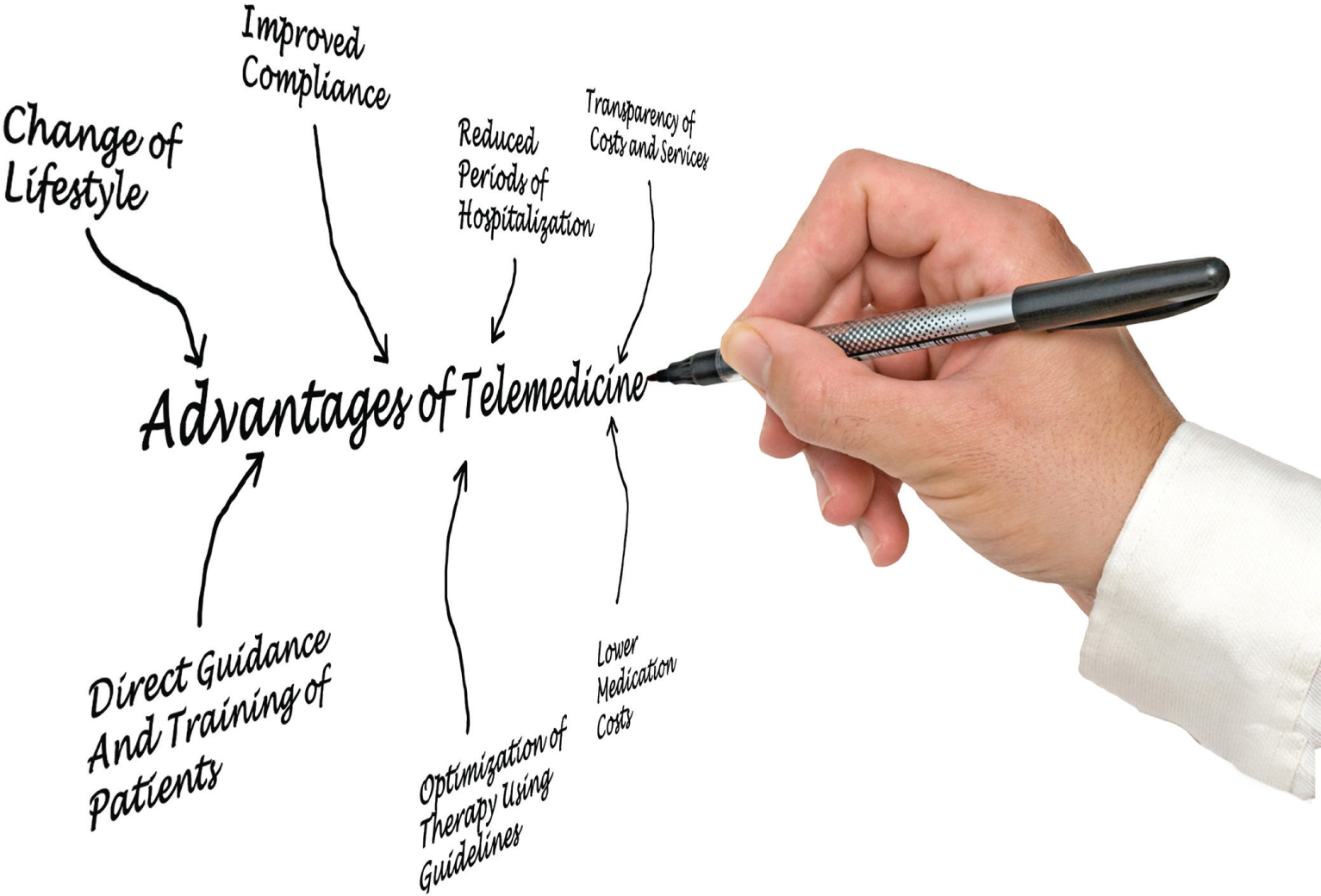
Domestic and international healthcare organizations, practitioners, patients, families, policy makers and legislators are increasingly recognizing the value added by the integrated use of telehealth. The major benefits are threefold: (1) this powerful means of healthcare delivery has the potential to significantly broaden access to healthcare; (2) increase efficiencies and reduce costs; and (3)enhance patient safety, quality of care, and ultimately, patient outcomes. As outlined in Telehealth Benefits and Adoption: Connecting People and Providers across Canada commissioned by Canada Health Infoway in 2011:
Research shows that telehealth can enhance quality of care by better supporting chronic disease management, application of best practices, and improvements of knowledge and skill development in local care providers and improvement of care coordination. Telehealth demonstrated improvements in timeliness of care, leading to improved outcomes. Furthermore, there were numerous examples of telehealth being the catalyst for leading practice changes which result in better quality of care (p. 8).
The 2020 health report Healthcare without Walls: A framework for delivering telehealth at scale (2010) adds, “…through a comprehensive redesign of care pathways, international and local evidence suggests that ‘full function’ telehealth can enable an incredible 40% reduction or more in the level of unplanned hospital admissions” (p. 7).
Given the high impact potential of telehealth, RNCOS Business Consultancy Services predicts that it will experience an 18.5% annual growth through 2018, inevitably resulting in spiking demand for training and coordination. The 2020 health report states, “ … the introduction of new telehealth and telemonitoring requires new skills and inevitably new ways of working that will change roles and responsibilities and create new groups of staff” (p. 48). The Canada Health Infoway study validates this assertion, naming professional development as a critical factor in the ability of telehealth to achieve its massive potential and noting that new roles and training are essential. Yet, strategic thinking about and implementation of such redesign and preparation of the workforce remains woefully underdeveloped, as does formalized training for clinical staff on assessing telehealth needs (2020health, 2010).
It was in response to this accumulating evidence in support of new telehealth roles and education that Thomas Jefferson University developed the telehealth facilitator training program. With experience in piloting telehealth successfully and little competition to prepare a skilled telehealth workforce to meet rapidly growing demand, TJU is well-primed to corner the market to equip tomorrow's telehealth professionals with the required tools to fulfill the potential of telehealth both locally and nationally.

The Unmet Need
To date, there are few academic programs that offer training and/or certificate programs in telehealth. The University of Alaska Southeast (in partnership with Alaska Federal Health Care Access Network) is one of the few institutions in the U.S. that offers a telehealth certificate program (for continuing education). The University of Arizona, University of California-Davis Health System, and Waldo County General Hospital (Maine) also run similar programs, but to our knowledge, do not award certificates. Other non-accredited, short-term training and educational resources exist, most notably through the Cal Telehealth Resource Center (also for CE credit) and the American Telemedicine Association (ATA). There are no sizeable general telehealth programs in the northeast United States. It is predicted that there will be a growing market for telehealth training given trending demands in the United States.
The Telehealth Facilitator Certificate Program
The Telehealth Facilitator Certificate Program, developed and offered by the National Academic Center for Telehealth (NACT) at Thomas Jefferson University, is an instructional training program that was designed for current affiliates of healthcare or health-related fields interested in further developing their careers by acquiring the skills needed to facilitate clinical telehealth encounters at their respective organizations.
Through a series of five self-directed, self-study, online learning modules, students enrolled in the Telehealth Facilitator training program learn how to improve patient healthcare access, efficiency, and safety, as well as improve patient outcomes, by acquiring an arsenal of telehealth skills enabling them to successfully facilitate, evaluate, and advocate for telehealth within their respective healthcare organizations. Students are immersed in modules that promote the skills needed to support clinical telehealth encounters, including, but not limited to, using telehealth in inpatient and outpatient settings, and providing technical assistance when needed. Through a hands-on practicum module, students have the opportunity to deliberately practice skills covered in previous modules, as well as circumvent common troubleshooting encounters and/or resolve common issues faced during typical telehealth encounters.
Paramount to the successful delivery of telehealth is the application of effective interpersonal and communication skills required to assume the role of telehealth facilitator on the interprofessional healthcare team. These concepts are a recurrent theme across all modules. On completion of the program, participants receive a certificate of completion and continuing education credits. Participants also have the option to complete subsequent coursework, which will further build upon the telehealth facilitator skillset.
Learning Objectives: The Telehealth Facilitator Training Program
While the NACT's Telehealth Facilitator Training Program was conceived as a basic introduction to the practice of telehealth, several lower- and higher-order learning outcomes are expected to take place in learners upon completion of the course. Learning outcomes are listed in Table 1 (below).
Upon completion of the Telehealth Facilitator Certificate Program, learners will be able to:
Theoretical Considerations for Pedagogical Selection
The platform selected to host the modules for the Telehealth Facilitator Certificate Program is the Jefferson Interactive Curricula Experience (iCE) Platform and Application (described below). Unlike other learning platforms (i.e., Blackboard), iCE is primarily a self-directed learning platform for learners enrolled in the program. Consequently, the iCE platform leverages learners' self-directedness throughout the program, and may be used as an exemplar for self-directed learning in adult education.
“Educational research has identified self-directed learning as an important skill for medical and healthcare graduates.”
Educational research has identified self-directed learning as an important skill for medical and healthcare graduates. In a field in which the half-life of information and skills may be ten years or less, close to half the information a physician acquires at the age of 30 may be obsolete by the time he/she is 40 (Ramnarayan and Hande; 2005). With this in mind, self-directed learning addresses one of the most enduring problems in medical and healthcare education: the exponential growth in medical knowledge. “Medical courses cannot teach everything that [health providers] consider relevant, and continued additions can lead to curriculum hypertrophy” (Abrahamson, 1978). Self-directed learning has been suggested as the methodology of choice to prevent this hypertrophy (Murad et al., 2010; p. 1057). If telehealth is to join this compendium of evolving healthcare practices, it only seems intuitive to have self-directed learning approaches embedded in telehealth skills acquisition.

Knowles also explained that effective learning occurs in self-directed and problem-oriented processes for adults, tapping into an intrinsically oriented motivation to learn (Knowles, as cited by Tagawa, 2008; p. 381). To be a life-long learning health provider, therefore, self-directed learning is an essential factor for continued development. While the format chosen for the TJU training program represents an ideal delivery of information for telehealth for learners in the healthcare industry, it also prepares its learners to adopt the skills that would lend to developing competence as self-directed learners.
The literature suggests that self-directed learning is a successful theoretical framework for training program development for adult learners in healthcare education. In a study by Pololi et al. (2001), investigators designed a three-day interprofessional course for medical school faculty to promote self-directed learning, teaching skills, personal awareness, and collegiality. Results indicated that the three-day course was highly effective in initiating a long-term faculty development process.
Based on a Web-based survey of medicine and pediatric residents that asked participants to report barriers to and strategies for achieving self-directed learning goals, Li et al. (2010) proposed a conceptual model for self-directed, lifelong learning. Their model allows for the creation of learning goals and plan development based on individual reflection and self- assessment, and continued revision of goals and/or plans based on degree of goal attainment.
“We believe qualified telehealth providers will be in demand.”
A systematic review by Murad et al. (2010) suggests that “self-directed learning in health professions education is associated with moderate improvement in the knowledge domain compared with traditional teaching methods, and may be as effective in the skills and attitude domains in physicians.”
The Interactive Curricula Experience (iCE) Platform
In 2015, the Center for Teaching and Learning launched the interactive Curricula Experience Platform and Application (iCE) through a collaboration with Digital Wave. iCE is a web-based platform and application that allows for interprofessional collaboration on course development throughout the TJU academic community. It allows content to be delivered to enrolled learners through a user-friendly iPad application. Faculty members across the six colleges at TJU are currently in the process of building modules and coursework on the platform.
Faculty members have the opportunity to share course materials (i.e., lectures, presentations, interactive quizzes, videos, and articles) on the iCE platform. Additionally, iCE fosters cross-campus collaboration among the faculty in the six colleges at TJU, further promoting interprofessional collaboration. The platform creates a central repository where faculty can create or download resources, edit resources to match the needs of their students, and package resources into courses. Resources are then shared to students based on their course registration.
Modular Design
Content for the certificate program was developed and spread across five asynchronous modules. Each self-directed learning module is expected to take anywhere from 90 to 120 minutes to complete. At the end of each module, a link directs the learner to an assessment. The format for the assessments are a combination of multiple choice and free response questions on module content. Learners must pass each assessment before moving on to the next module. Additionally, there is an opportunity for learners to ask questions and engage in a dialogue with one another via chat threads in the Blackboard Learning Management System (linked to the iCE platform).
The five modules for the Telehealth Facilitator Certificate Program include:
1) An Introduction to Telehealth
2) A Deeper Dive into Telehealth
3) Settings for Telehealth Facilitation and Delivery
4) Troubleshooting in the Telehealth Experience *
5) The Essence of Telehealth Facilitation
Innovative Curricular Application of Telehealth to Graduate Medical Education Programs: Focus on non-ACGME Fellowships
In parallel with programs developed in the NACT, and to complement the University's efforts to immerse telehealth skills into various facets of health delivery, Thomas Jefferson University is proud to offer four new robust training programs for post-graduate trainees that offer the opportunity for telehealth skills acquisition in the graduate medical education (GME) program: 1) the Telehealth Fellowship Program; 2) the Emergency Medicine Medical Education Fellowship; 3) the GME Telehealth Elective, and 4) Medical Student Telehealth Elective. We provide brief overviews of these programs in this manuscript.
The Telehealth Fellowship Program
Because we believe qualified telehealth providers will be in demand, and given the scarcity of training for telehealth providers, we created our one-year fellowship program. We are aware of only two programs that offer telehealth fellowships on a small scale and are specific to provider specialty.
The mission of the Telehealth Leadership Program is to train physicians in the knowledge, skills, and attitudes necessary to become independent telehealth researchers and leaders. The program is guided by the belief that through experiential learning, mentorship, and a rigorous academic curriculum, the fellow will graduate with the ability to successfully conceptualize, develop, and implement telehealth programs, while building the evidence-based literature on telehealth.
Utilizing team-based learning, hands-on application of knowledge, and simulation training, curriculum is informed by the principles of experiential and self-directed learning theories to foster knowledge in four core areas of study. These core areas and their associated competencies continuously complement one another and work to build a foundation of telehealth and leadership success. These areas include: (1) Leadership & Management Skills, (2) Entrepreneurship, (3) Research & Education, and (4) Clinical Skills.
The curriculum is tailored to the fellow's personal interests, allowing for individualized concentrations of research and knowledge application, as well as the option to complete an advanced degree or certificate.
“Development of robust training models to assist tomorrow's physicians in the care of patients is essential.”
To demonstrate their acquisition of knowledge, skills, and attitudes throughout the duration of the program, fellows will be required to complete a capstone use-case, applying the core competencies of the program. The capstone will complement the entrepreneurial rotations, as the fellow builds financial and marketing models alongside developing the legal supporting documentation.
The Emergency Medicine Medical Education Fellowship
The Department of Emergency Medicine at Thomas Jefferson University Hospital began its one-year Medical Education Fellowship for graduating emergency medicine residents in the Fall of 2015. The fellowship program was conceptually designed for motivated residents seeking to advance their training in adult learning theory, instructional design, and design thinking. The overarching goal of the fellowship is to prepare the fellow for a highly successful career as an educational leader in academic emergency medicine.
Informed by the principles of Experiential Learning Theory, Transformative Learning Theory, and Self-Directed Learning Theory, the Medical Education Fellowship offers potential fellows the skillset to adapt to an ever-changing learning environment and educational landscape. The fellowship provides structured opportunities for formalized training in adult learning in clinical and academic medicine. It uses simulation, telehealth, and patient safety and clinical quality tools as vehicles to inform educational initiatives in undergraduate and graduate curricula, as well as faculty development programming and continuing medical education. In addition, the fellow has the opportunity to identify a specific area of academic interest in the realm of education, and is given the resources and time to develop his/her productivity within this specified domain.
While fellowship programs of this type are offered at other institutions and departments across the country, the fellowship program at TJU is unique in its inclusion of telehealth, which serves as a vehicle for the application of educational concepts covered. Fellows have the unparalleled opportunity to work with interprofessional health delivery teams across the hospital system to develop and support educational training curricula, as well as train telehealth providers.
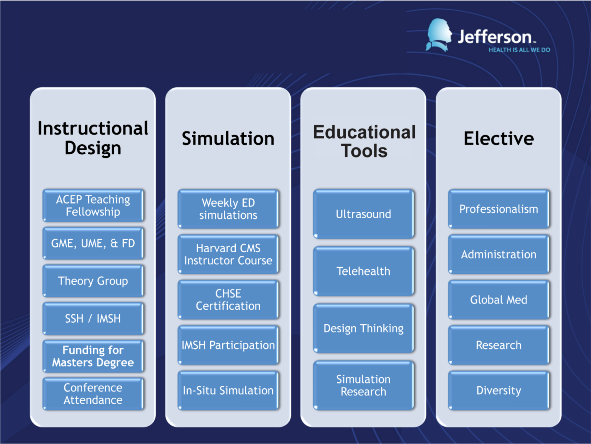
Through involvement in the undergraduate and graduate medical education programs and the faculty development program within the Department of Emergency Medicine, the fellow will gain experiences across three thematic areas: instructional design, simulation and educational tools, and from fellow-specific elective specialization (Table 2).
Academic Expectations
Alongside these academic responsibilities, the education fellow works clinically as an attending physician in the Emergency Departments of Thomas Jefferson University Hospitals.
“The mission of the Telehealth Leadership Program is to train physicians in the knowledge, skills, and attitudes necessary to become independent telehealth researchers and leaders.”
The Telehealth Elective for Resident Physicians and Medical Students
This elective for residents and medical students is a 4-week (minimum) rotation designed for those wanting to explore all aspects of novel care delivery systems. There is a base educational curriculum with an opportunity for learners to further pursue interests appropriate for their degree of training. In addition to basic readings and an interactive curriculum specifically tailored for their level of education, all learners will participate in conception, development, and implementation of various telehealth use cases throughout the health system, regional Accountable Care Organizations (ACOs), and large community groups. In addition to broad exposure to telehealth operations, learners will also be given the option to choose an area of focus be it administrative, clinical, or research.
All learners will participate in all major telehealth-related work group meetings, including the monthly enterprise-wide leadership committee; weekly team strategy meetings; weekly innovation committee meetings; and biweekly research-in-progress meetings. They will receive formal training in provision of telehealth services, as well as participate as an instructor in telehealth training sessions.
Learners will spend 12-24 hours per week providing/observing telehealth care in a variety of use cases (i.e., virtual rounds, on-demand urgent care, and scheduled outpatient appointments) and performing follow-up surveys on select groups of patients/family receiving telehealth interventions.
Conclusion
Reimbursement and healthcare delivery models are changing from ones that have thrived in a fee for service model, to ones that are value based. Telehealth is an avenue to both improve access and deliver high value care in a patient-centered manner. Development of robust training models to assist tomorrow's physicians in the care of patients is essential. We described one model that aims to train all individuals working within the delivery system, including providers, staff, residents, and students.
Footnotes
Readers interested in more information about any of our training opportunities should reach out to the JeffConnect team at