Abstract
Background:
Noma is a gangrenous infection of the face that results in severe facial deformity, occurring primarily in malnourished and impoverished populations.
Objective:
To assess clinician- and patient-reported outcomes (PROs) before and after reconstructive surgery for patients with noma in northwest Nigeria.
Methods:
Objective outcomes were recorded using the noma-specific NOITULP (nose, outer cheek, inner cheek, trismus, upper/lower lip, particularities) classification system. PROs were recorded using a locally developed tool. Postsurgical changes were assessed by Wilcoxon signed-rank testing. Linear regression was used to look for associated risk factors. The inter-rater reliability (IRR) of the NOITULP score was assessed using the weighted kappa statistic.
Results:
Forty-nine patients (median age 25 years, 71% male) underwent local/regional flap reconstruction and/or trismus release. Twelve complications were reported. Univariate analysis showed a 3.20 change in PRO score (95% confidence interval 0.59 to 5.81, p = 0.018) per kilogram the patient underwent at time of surgery. The NOITULP score improved from a presurgery median of 3.5 to 2.3 (p < 0.0001), however, the IRR was poor (kappa = 0.0894, p < 0.0001). The PRO score also improved from a median of 7.0 to 12.0 (p < 0.0001).
Conclusions:
Facial reconstructive surgery improves the NOITULP score and PROs in patients with noma in northwest Nigeria.
Clinical Trial Registration: OCA017-63.
KEY POINTS
Introduction
Noma, or cancrum oris, is a devastating gangrenous infection of the mouth occurring primarily in malnourished children. Mortality rates without treatment approach 85–90%.1,2 The disease begins as necrotizing gingivitis and can rapidly progress to destroy the tissues of the mouth, cheek and facial bones.3,4 Although the exact etiology remains unknown, noma is associated with a lack of access to quality health care including absence of childhood vaccinations, chronic malnutrition, poor oral hygiene, and low socioeconomic status.5,6 Those who survive the acute stages of noma are left with variable degrees of facial disfigurement, speech and eating difficulty, and trismus (Fig. 1).2,4,7
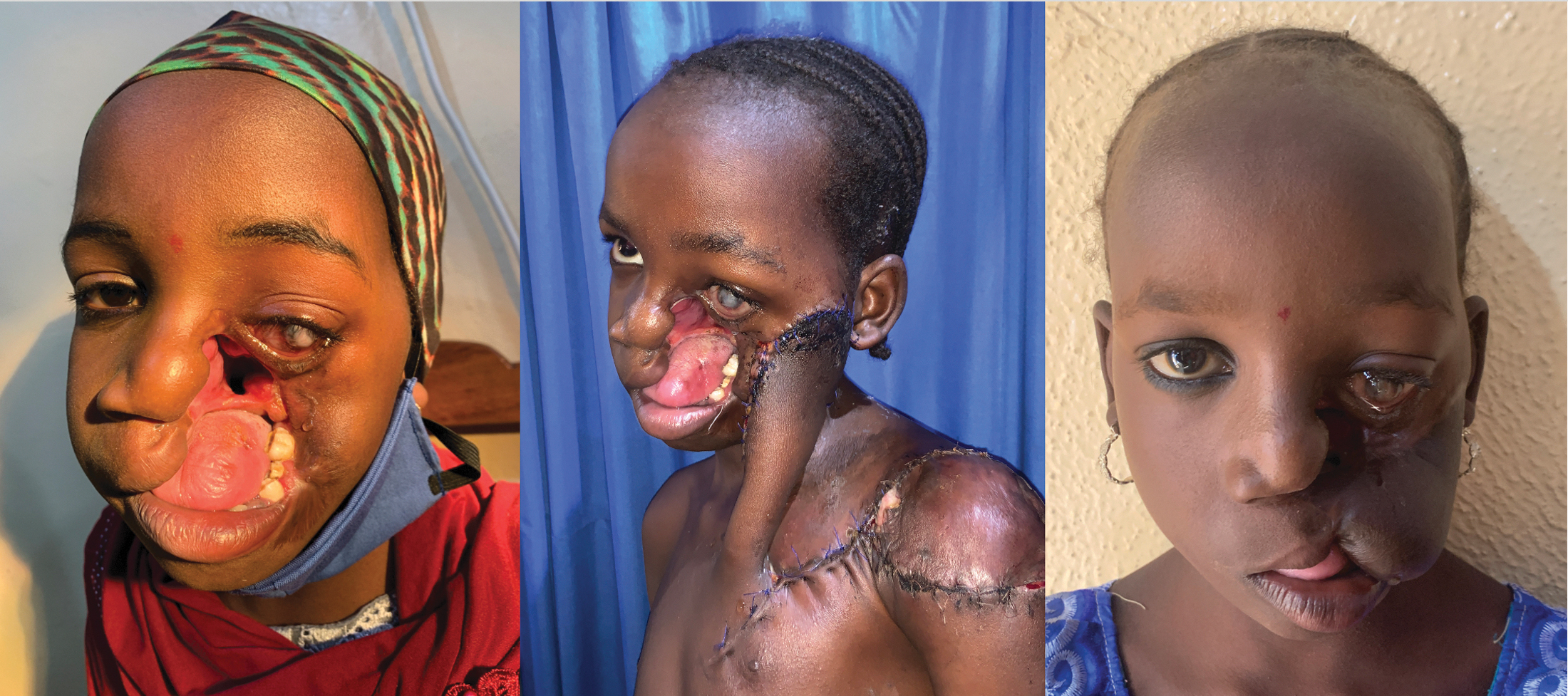
Thirteen-year-old female patient who survived acute noma, now presenting with an extensive left cheek and midface defect. The patient underwent staged, prelaminated, waltzed deltopectoral flap, lip reconstruction, and oral fistula closure in a district hospital setting. (preoperative NOITULP score: 13, postoperative NOITULP score: 5).
Noma reconstructive surgery aims to restore facial form, oral competence, and mastication (Fig. 1). Care is multidisciplinary and surgical reconstruction often necessitates multiple staged procedures in areas with few surgical resources.2,8,9 A variety of setting appropriate surgical techniques for noma have been described including deltopectoral flaps, 10 supraclavicular flaps, 11 myocutaneous submental artery flaps, 12 Gillies fan flaps, 13 and free tissue transfer.14–16 Trismus surgery necessitates soft tissue and bony release.14,17 Nonetheless, surgery rarely restores normal aesthetics or a return to full function.8,18–20 Prior studies are mainly case reports and series with short-term follow-up, but none have prospectively assessed outcomes using an objective grading system.8,18–20
In 1998, Marck et al. introduced the NOITULP classification (“A” in Table 1) for the planning and evaluation of noma reconstructive surgery.10,18 Although noma severity (NOITULP score) correlated with operative time, 18 no prospective studies with NOITULP exist, and few examined patient-reported outcomes (PROs).21,22
Objective (A) and subjective (B) outcome measures
The NOITULP scoring system where the percentage of tissue loss is estimated for each anatomic region (except for trismus that is measured) and converted into a numerical score.
The PRO outcome tool developed at NCH.
PRO, patient-reported outcome.
Since 2015, Médecins sans Frontières (MSF) (Doctors Without Borders) has supported a comprehensive noma treatment program at The Noma Children's Hospital (NCH) in Sokoto State, Nigeria. The purpose of this study was to prospectively assess whether there are meaningful improvements in clinician and PROs for patients with noma undergoing reconstructive surgery, using the NOITULP score and a PRO tool.
Methods
Between May 2018 and May 2019, patients with stage 5 noma who presented to NCH were included. Consent was obtained directly from patients ≥18 years and from caretakers for those <18 years. Assent was sought for patients 7 to 18 years of age. Ethical review boards approval from MSF (1829), Sokoto (040/018), and Kebbi (104:3/2018) State Ministries of Health, and the Usmanu Danfodiyo University Teaching Hospital (671) were granted.
Although several validated PRO measures for head and neck surgery exist, none are available in Hausa language.23–25 MSF created a PRO tool in both Hausa and English that assesses eating, drinking, speech, appearance, social interaction, community inclusion, stigmatization, and psychosocial development (“B” in Table 1). Given that this was the first time the NOITULP and PRO tools were being used in the literature, no power analysis was performed.
Outcomes were assessed on admission, 1–2 days before the first surgical encounter, at discharge, and at 6- and 12-month follow-up. Height, weight, middle upper arm circumference (MUAC), mouth opening, NOITULP, and the PROs were recorded at each time point. The following surgical data were recorded: procedure(s), type of anesthesia, American Society of Anesthesia (ASA) score, surgery duration (minutes), and complications.
Noma surgery technique
Reconstructive surgery is only performed in patients who have healed months to years after acute noma. No patients with acute noma were included in this study. Locoregional flaps were performed for soft tissue repair of the lips, cheek, nose, palate, and oral lining. Flaps include deltopectoral, temporal parietal fascia, cervicofacial rotation, Estlander, Abbe, submental island, forehead, visor, and palatal flaps. Grafts included split, full, conchal, composite, and costal. Prelamination and delay techniques were used (Figs. 2 and 3).
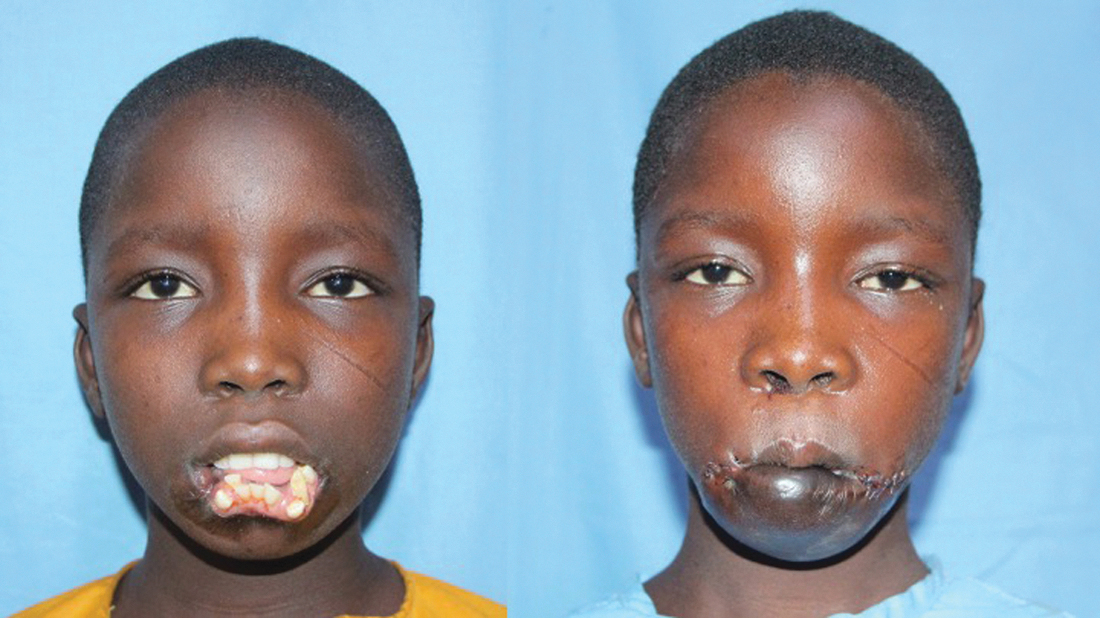
Twelve-year-old male patient after surviving acute noma at the age of 5 years, now with near total loss of his lower lip with dental anarchy (unrestricted dental growth). The patient underwent dental extraction and total lower lip reconstruction with deltopectoral flap and fascia lata suspension to the piriform apertures (preoperative NOITULP score: 4, postoperative NOITULP score: 1).
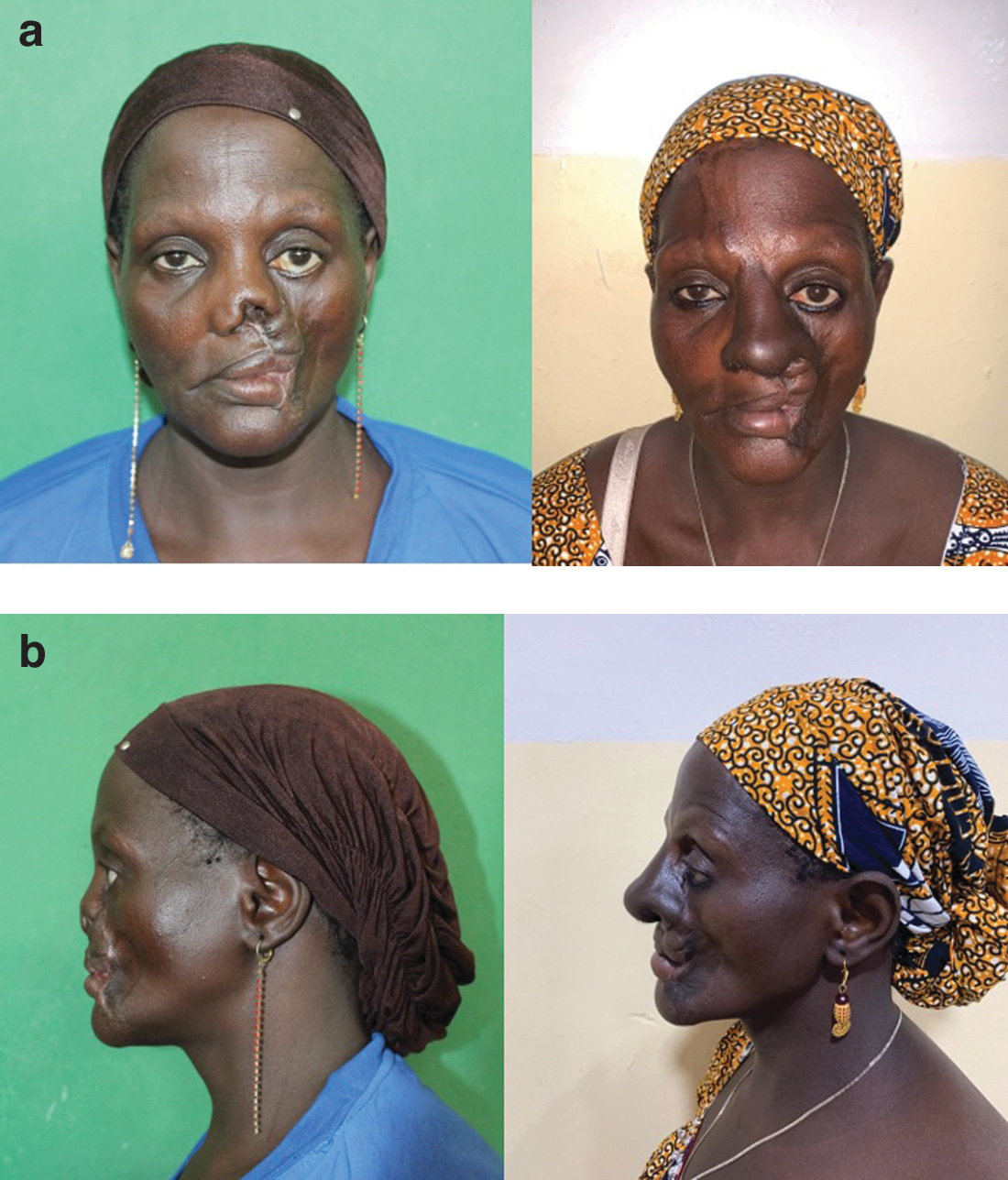
Forty-one-year-old female patient with noma-related nasal defect since childhood. The patient underwent total nasal reconstruction with turn in flaps for lining, autologous rib cartilage, and forehead flap in single stage procedure followed by flap division. Image
Surgery for trismus included coronoidectomies and ankylosis release with or without interposition grafting using free fat, fascia, or temporopareital fascia flap. Surgical approaches included intraoral, direct, and preauricular. Surgery was performed under general anesthesia, with awake fiberoptic intubation. The NCH is a Nigerian Ministry of Health District Level Hospital without an intensive care unit setting. No free tissue transfer was performed in our setting.
Data analyses
All data analyses were carried out in STATA version 15 (StataCorp LP, College Station, TX). As most data were nonparametric, median and interquartile ranges (IQRs) are presented. Categorical variables are presented as numbers and percentages. Patients were placed into the binary categories of underweight or nonunderweight, using the following definitions of underweight: for individuals ≤5 years of age: MUAC <125 mm; 6–15 years of age: body mass index (BMI) ≤5th percentile; 16 years and older: BMI <18.5 kg/m2. 26 No patients were obese.
For the NOITULP classification, three noma surgeons (R.W., A.O.T., D.A.S.) independently estimated the score for the nose, outer cheek, inner cheek, upper lip, and lower lip categories from a standardized series of photographs. 27 Trismus was determined from mouth opening measurements recorded in the database. The complete NOITULP score of each grader was calculated by adding the individual anatomic area classifications from that grader with the common trismus score. The mean of the complete scores from all of the available graders was used as the final NOITULP score. To assess the score for a single anatomic area, the mean of the available grades was used.
For the PRO score, each category was assigned a 0 to 2 score (0 being the most negative answer, 2 being the most positive). The categories were converted to a 0- to 14-point scale with higher values representing more positive responses. The presurgery score was determined 1–2 days before surgery; the postsurgery score was the latest available follow-up score. The median and IQR were calculated pre- and postsurgery for every component category of both scores along with the complete composite scores. The difference in medians pre- and postsurgery was assessed using the Wilcoxon signed-rank test.
Linear regression was performed to evaluate for association between the score changes and each risk factor including age, gender, underweight status, duration of surgical encounter, having more than one procedure, ASA score, complications, and trismus surgery. Linear regression was used to assess whether there was a relationship between the two scores. For patients who had more than one surgical encounter, the mean duration of all surgical encounters was used. A multivariate linear analysis was performed using any variable that showed a possible association (p ≤ 0.05) based on univariate analysis; only patients with data for all relevant variables at both time points were included.
To assess inter-rater reliability (IRR), the weighted kappa statistic was calculated for the NOITULP score and the raw percentages of tissue loss. The kappa statistic was interpreted as follows: >0.75 is excellent agreement, 0.4 to 0.75 is fair to good agreement, and <0.4 is moderate to poor agreement. 28
Results
Demographics
Of 104 patients, 49 were surgical candidates (Table 1) who underwent 94 procedures (range: 1 to 5; mean: 1.9), during 69 surgical encounters (range 1 to 5). Sixty-two (93% of procedures were performed under general anesthesia and 5 under local (7%). The mean duration of a surgery was 94 min (standard deviation 48 min).
Twelve complications were recorded, including tooth injury (n = 2), hypothermia postoperatively (n = 1), an issue with intubation or unanticipated difficult airway (n = 2), wound dehiscence (n = 2), cautery burn to the lip (n = 1), and need for revision surgery due to failure of the initial surgery (n = 4). The most common surgical procedures were the deltopectoral flap (any stage, n = 15, 16%), trismus release (n = 14, 15%), cheek rotation flap (n = 11, 12%), commissuroplasty (n = 10, 11%), and Estlander flap (n = 8, 9%).
Evolution of outcome measures over time
The median duration of follow-up was 405 days (IQR 220 to 844, range 12 to 1067 days). Only 8 patients had follow-up of <140 days. Both the NOITULP and PRO scores had improvement from the preoperative baseline at all postoperative time points (Table 2). The NOITULP scores at admission had a median score of 3.7 (IQR 2.3 to 5.3) and a preoperative median score 3.5 (IQR 2.0 to 5.0). The PRO scores showed a median of 7 before surgery (IQR 4.5 to 9.0). Wilcoxon sign rank testing revealed evidence of an improvement in NOITULP from a median of 3.5 to 2.3 after surgery (p < 0.0001), with a median change of −1.6 points (IQR −2.2 to −0.33, range −6.3 to −1.3).
Change in NOITULP and patient-reported outcome score categories over time
The changes in outcome measures before and after surgery.
p < 0.05.
IQR, interquartile ranges.
There was evidence for improvement in the outer cheek, inner cheek, and upper lip scores postoperatively (Table 2). Similarly, the PRO score showed evidence of improvement from a median of 7 preoperatively to 12 after surgery (p < 0.0001). All domains within this score had strong evidence for improvement postoperatively except stigmatization, which was not reported as a major issue before surgery. The most striking change occurred in the appearance category that went from a median score of 0 preoperatively to a score of 2 postoperatively.
Risk factors associated with the change in NOITULP score
In the univariate analysis, male gender, longer duration of surgery, and having had trismus surgery were associated with an improvement in NOITLUP score (“A” in Table 3, left). However, in the multivariable model, only male gender was associated with an improvement in NOITULP (“A” in Table 3, right). In this model, male gender was associated with an improvement of −1.08 points (95% confidence interval [CI] −2.06 to −0.095). Of the 34 patients included in this analysis, 25 were male, and the median preoperative NOITULP scores between males and females were similar (3.3 vs. 3.7, respectively).
Risk factors associated with outcome scores
Univariate and multivariate analyses of the risk factors associated with the change in NOITULP score.
Univariate and multivariate analyses of the risk factors associated with the change in PRO score.
p < 0.05.
ASA, American Society of Anesthesia; CI, confidence interval.
Risk factors associated with changes in PRO score
Univariate linear regression showed an association between the change in PRO score with being underweight, the duration of surgical encounter(s), and having had a trismus release (“B” in Table 3, left). However, the final model provided evidence for only trismus release to be associated with change in PRO score, with those having had surgery experiencing an improvement of 3.76 points (95% CI 0.62 to 6.89).
IRR of the NOITULP score
The IRR of the overall NOITULP score was poor with a weighted kappa statistic of 0.0894 (p < 0.0001). Table 4 shows the IRR for the scoring of each anatomic area. Inner cheek loss had the poorest IRR (kappa = 0.0801, p = 0.0021) while the nose loss category was most reliable (kappa = 0.5437, p < 0.0001). As expected, the IRR of the estimation of the percentage of tissue loss was worse for all anatomic areas than when categories of percentage loss were used.
Inter-rater reliability of NOITULP scores and percentages per anatomic area
The IRR of the NOITULP score and direct estimation of percentages per anatomic area.
p < 0.05.
IRR, inter-rater reliability.
Discussion
This study is the first to prospectively evaluate the results of noma reconstructive surgery using PRO measures and the NOITULP score. Our results showed improvement in both scores after surgery, however, the NOITULP score did not normalize. Since the IRR of the NOITLUP system was poor, its utility as an objective outcome measure is questionable, as is the validity of our risk factor analysis.
Marck et al. reported 23 patients with a mean preoperative NOITULP of 6.618; whereas Hartman et al. had 3 patients with scores of 6, 9, and 16. 11 In these prior series, the operating surgeons determined the NOITULP scores in person at the time of surgery. In our series, NOITULP scores were lower than previous studies. The use of photographs may have resulted in an underestimation in defect severity. Alternatively, the participants may have sought care earlier and, therefore, had less severe noma, as our surgical program includes an outreach component focusing on prevention and early detection. 29
Considering the poor IRR of the NOITULP score, we question whether this score should be used as an outcome measure, as the score was originally developed for preoperative planning.10,18 However, the possibility remains that the IRR of scores determined by physical examination or live video examination would be more accurate. Furthermore, dedicated training on how to use the score, with discussion of cases among practitioners, may improve its reliability. Huijing et al. proposed a five category system of outcomes measure for facial reconstruction in low-resource settings 30 that was used for noma outcomes by Bouman et al., but the IRR was not investigated. 8
The improvement in PRO score was similar to prior retrospective analysis performed in the same setting. 22 Although the PRO score used in this study does not represent a validated PRO tool, it includes similar domains as the validated measures (such as aesthetics, quality of life (QOL), and function) while covering a broader range of these domains than any single existing tool. Importantly, the tool is practical for use in our study setting; it was administered verbally by community health workers and easy for patients to understand critical factors when working with patient populations with varying levels of literacy.
Prior complication rates for noma surgery have been reported at >50%, making the complication rate here of 24% lower than other reports.8,30 Programmatic guidelines for infection control, medical staff education, and focused antibiotic usage according to established protocols are employed. Alternatively, it is possible the complication rate was under-reported as a minority of patients were discharged home before the 30-day monitoring period.
Despite male and female patients having similar preoperative NOITULP scores, we found an association between being male and having an improvement in NOITULP postsurgery. This association may exist because male children are more likely than female children to have access to better nutrition and hygiene, or more attention from their caregivers. Multivariable analyses also showed evidence for an association with improvement in PRO score and having had a trismus release. This result makes sense since trismus is a debilitating condition that can affect both function and social interactions.
Noma requires further surgical and QOL measurement tools to improve outcomes research. Although the WHO recently translated the abbreviated version of its QOL assessment into Hausa, this assessment does not specifically assess speech, eating/drinking, and appearance. 31 Similarly, an existing tool called “Patient Outcomes of Surgery—Head/Neck” was designed for skin lesions and is not as useful a measure for noma, which also involves bony structures and functional deficits. 25 FACE-Q, although validated,23,32–34 does not include domains on social inclusion or stigmatization. 29 Better tools are needed.
Although this study was limited to northwest Nigeria, the results should be generalizable to other populations affected by noma, since risk factors such as poor nutritional status, lower socioeconomic status, and poor oral hygiene are present in all of these populations.5,7,35,36
These data must be interpreted in the context of the study design. The number of patients included in the study was limited; thus, we had limited power. Although there were >100 eligible patients in the study, approximately half declined surgery for a variety of reasons (comorbidities, active malaria, pregnancy, farming seasons, and approval of the family), meaning we cannot exclude selection bias. Furthermore, the NOITULP classification itself may be inadequate to describe such a complex facial defect pattern such as noma, and thus unable to accurately capture surgical improvements.
Alternatively, the surgical techniques relied upon may be wholly inadequate for noma surgery itself. Major advances in multidisciplinary care, free tissue transfer, and complex staged reconstruction are all required to achieve the gold standard of treatment in countries where noma exists. Equal to surgeon training is the imperative that governments embrace meaningful health care for their citizens.
Noma reconstructive surgery consists of a series of diverse, creative, and staged procedures often performed in settings of extreme poverty or insecurity. Research to explore the nuanced deformities of the face, eyes, lips, and oral lining will assist surgeons in the treatment of this inexcusable disease. With hope, the eradication of noma on the global scale will make this research unnecessary.
Conclusions
Noma is a devastating oral–facial gangrene that afflicts malnourished and impoverished populations. There are improvements in clinician and PROs for patients with noma undergoing reconstructive surgery, however, the IRR of the NOITULP score was poor.
Footnotes
Acknowledgments
The authors thank the research and outreach team in Sokoto Children's Hospital for their contributions to this study.
Authors' Contributions
M.A. contributed to conceptualization (equal), methodology (equal), formal analysis (lead), and writing original draft (lead). M.O. carried out data curation (lead) and project administration (equal). B.O. was in charge of funding (lead) and project administration (equal). A.L. took charge of conceptualization (equal), methodology (equal), and writing review and editing (equal). C.O. was involved in formal analysis (supporting) and methodology (equal). E.F. carried out conceptualization (equal), methodology (equal), data curation (supporting), and project administration (equal). R.W., A.O.T., and D.A.S. were involved in conceptualization (equal), investigation as surgeon grader (equal), and writing review and editing (equal). All authors have reviewed and approved this article before submission.
Author Disclosure Statement
No competing financial interests exist.
Funding Information
This study was funded by Medecins Sans Frontieres Operational Centre Amsterdam.
