Abstract
Chicken liver has been implicated in several reported U.S. illness outbreaks, probably caused by inadequate cooking and pathogen contamination. To identify commonalities among these outbreaks that could represent targets for prevention, we describe chicken liver–associated U.S. outbreaks during 2000–2016 reported to the Food Safety and Inspection Service, to the Centers for Disease Control and Prevention, and in published literature. We identified 28 outbreaks (23 [82.1%] were campylobacteriosis only, 3 [10.7%] were salmonellosis only, and 2 [7.1%] were caused by both pathogens), with 18 (64.3%) occurring during 2014–2016. Common outbreak features included blended chicken liver dishes (e.g., pâté; 24 [85.7%]), inadequate cooking (26 [92.8%]), and preparation in foodservice settings (e.g., sit-down restaurants; 25 [89.3%]). The increasing frequency of reported outbreaks highlights chicken liver as an important food safety problem. Public health partners should collaborate on prevention measures, including education on proper foodservice preparation of blended chicken liver dishes.
Introduction
Chicken liver has been recognized as an important vehicle for foodborne infections (Geissler
FSIS and the Food and Drug Administration (FDA) recommend cooking poultry products to an internal temperature of 165°F (FDA, 2013; FSIS, 2015). However, some food writers recommend using livers that have not been fully cooked (e.g., “still rosy pink inside”) when preparing chicken liver dishes (The Dallas Morning News, 2013; Los Angeles Times, 2015). Recipes that call for the use of partially cooked chicken liver are readily available (The New York Times Company, 2018; Food Network, 2018).
Cooking to recommended internal temperatures is especially important for foods known to contain pathogens. Like other chicken products, chicken liver has been found to be contaminated with
Consumption of inadequately cooked chicken livers contaminated with pathogens can lead to illnesses and outbreaks. To better understand the characteristics of such outbreaks to identify opportunities for prevention, we reviewed and described chicken liver–associated outbreaks in the United States during 2000–2016.
Materials and Methods
We reviewed outbreaks reported to FSIS and the Foodborne Disease Outbreak Surveillance System (FDOSS) of the Centers for Disease Control and Prevention (CDC, 2017a) and in published literature to identify outbreaks of illness associated with chicken liver during 2000–2016 in the United States. An outbreak was defined as the occurrence of two or more cases of similar illness resulting from ingestion of a common food. We included an outbreak in the study if: (1) chicken liver or a food containing chicken liver (e.g., chicken liver pâté) was implicated; and (2) at least one of the case-patients in the outbreak had a laboratory-confirmed foodborne infection. We described outbreaks by several characteristics, including illness-onset dates; etiologies; case-patient demographics; reported illnesses, hospitalizations, and deaths; implicated food vehicles; food-preparation settings; and contributing factors. For outbreaks with incomplete information about certain characteristics, we attempted to obtain the information from relevant state and local health departments. We compared median numbers of illnesses per outbreak using the Wilcoxon rank-sum test in SAS version 9.4 (SAS Institute, Cary, NC).
Results
During 2000–2016, a total of 28 reported outbreaks associated with chicken liver were identified (Table 1). The frequency of identified outbreaks increased throughout the study period, particularly during its last few years (Fig. 1); for example, there were 4 (14.3%) outbreaks during 2000–2010, 6 (21.4%) during 2011–2013, and 18 (64.3%) during 2014–2016. The outbreaks were clustered geographically, by state of case-patient residence, in northeastern, western, and upper midwestern states (Fig. 2).
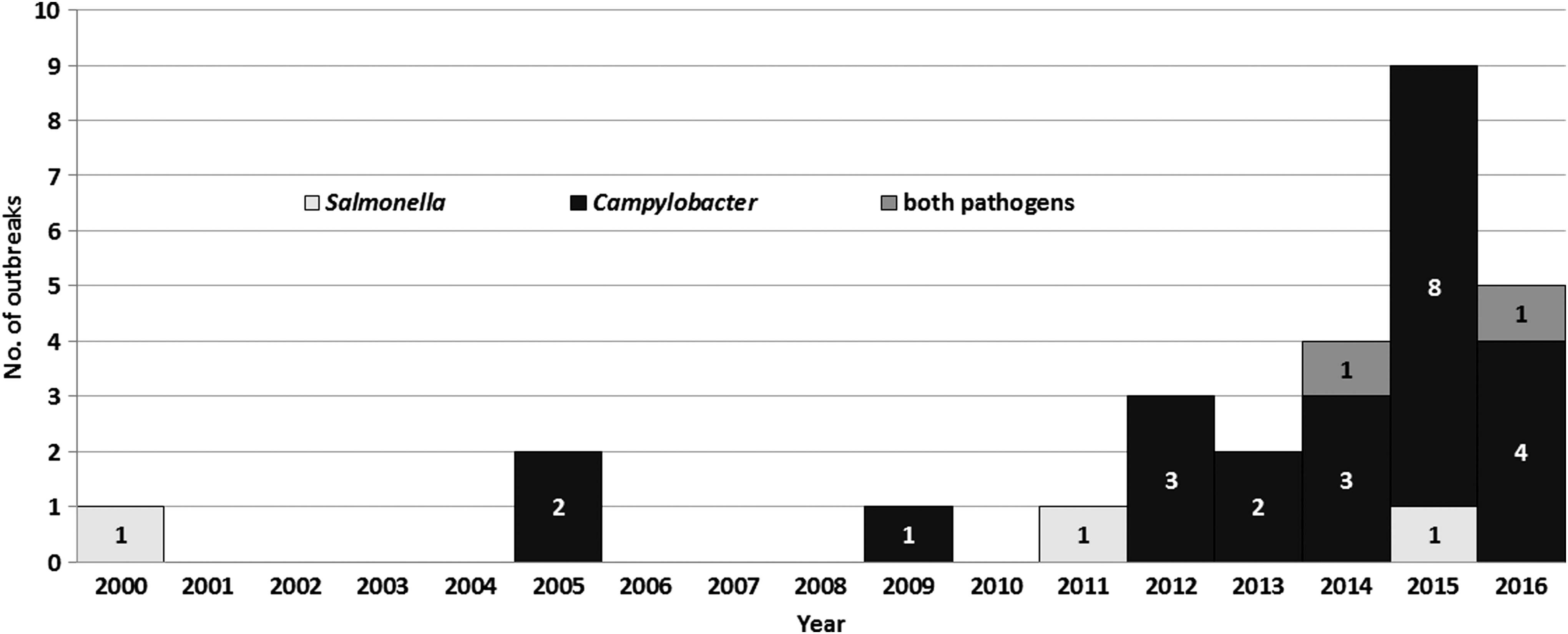
Chicken liver–associated campylobacteriosis and salmonellosis outbreaks (
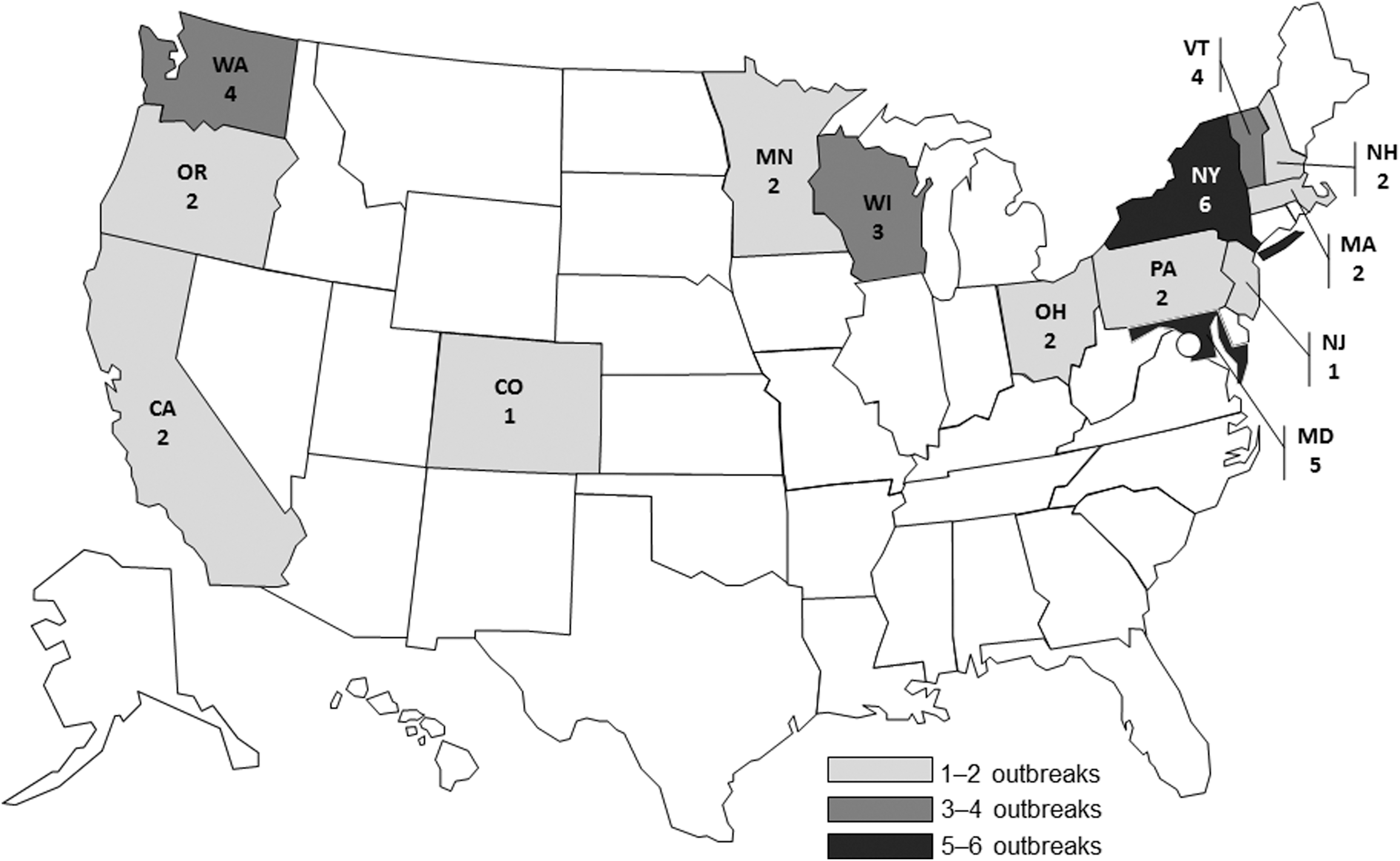
Chicken liver–associated campylobacteriosis and salmonellosis outbreaks (
Includes confirmed and probable/suspect case-patients.
Hospitalization status was not reported for each case-patient. No deaths associated with these outbreaks were reported.
Not all potential contributing factors were known or listed.
Product was labeled “broiled” and appeared, but was not, fully cooked.
Published report 1: Hanson
Published report 2: Tompkins
One case-patient in this outbreak consumed raw, pill-sized pieces of chicken liver that had been prescribed by a naturopathic physician.
Published report 3: Scott
In this outbreak,
In this outbreak, both
Published report 4: Glashower
FDOSS, Foodborne Disease Outbreak Surveillance System (Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention; data received on December 8, 2017); FSIS, United States Department of Agriculture, Food Safety and Inspection Service; NOS, not otherwise specified.
The 28 outbreaks resulted in a total of 361 illnesses, 46 (12.7%) hospitalizations, and no deaths. The median number of illnesses per outbreak was 5.5 overall (range, 2–190). In general, later outbreaks had fewer illnesses per outbreak; for example, the median number of illnesses per outbreak significantly decreased from 9 during 2000–2013 to 4.5 during 2014–2016 (
Of the 28 outbreaks, 23 (82.1%) were caused by
Discussion
The frequency of restaurants as a food-preparation location observed among outbreaks in this study (78.6% of total and 75% of campylobacteriosis) is higher than that among all foodborne outbreaks of campylobacteriosis (142/451 [31.5%]) and salmonellosis (1039/2297 [45.2%]) reported to FDOSS during 2000–2016 (CDC, 2018). The predominance of foodservice preparation settings in reported chicken liver–associated outbreaks indicates there may be value in targeting restaurants, particularly sit-down restaurants, and other places where chicken liver dishes are commercially prepared for prevention efforts, especially with regard to cooking adequacy. FSIS (2016a) encourages cooking of chicken liver dishes to an internal temperature of 165°F, as measured by a food thermometer, before consumption. Assisted living or senior citizen institutions were noted as food-preparation settings among the outbreaks in this study; special care should be taken to not serve inadequately cooked chicken livers to the elderly or other higher risk populations. Food safety partners from local, state, and federal agencies, academia, and industry should collaborate to develop ways to encourage foodservice workers and consumers to properly cook chicken liver.
Establishments that produce chicken liver for human consumption (e.g., chicken slaughter facilities) should address food safety hazards associated with chicken liver through their Hazard Analysis and Critical Control Points (HACCP) systems. Freezing is an intervention that has been shown to reduce, but not eliminate,
To increase the availability of data on chicken liver–specific prevention strategies, In July 2016, FSIS (2016b) included in its list of food safety research priority items specific to chicken liver. Given that inadequate cooking was a common contributing factor among the outbreaks in this study, an important research need is to develop and validate a method of cooking chicken liver, particularly blended chicken liver (e.g., pâté), that is safe to consume and well accepted by both chefs and consumers. FSIS is collaborating with the Agricultural Research Service and universities on chicken liver–related studies to improve understanding of chicken liver contamination with pathogens and of consumer and chef preferences, practices, and knowledge of risk.
Recent FSIS sampling results are consistent with other data demonstrating pathogen contamination in chicken liver. In November 2016, FSIS (2016c) began sampling and analyzing chicken livers from FSIS-regulated establishments for
The observed predominance of campylobacteriosis over salmonellosis outbreaks is noteworthy. Both
The observed increase in reported chicken liver–associated outbreaks, particularly campylobacteriosis, is consistent with a concurrent increase in foodborne campylobacteriosis outbreaks overall (CDC, 2018). One explanation for the increase observed in this study is that these outbreaks could actually have begun to occur more frequently. Alternatively, a number of illness surveillance factors might also have promoted outbreak recognition and reporting in the latter years of the study, including: higher index of suspicion for chicken liver as an illness vehicle after published reports of outbreaks since 2011 (Tompkins
The geographic outbreak clustering observed in this study may reflect regional differences in consumption of inadequately cooked chicken liver dishes. Data regarding chicken liver consumption and preparation patterns are currently lacking, but may help focus prevention efforts. Another explanation for the observed geographic differences in number of outbreaks is that, because of variability in
Illnesses associated with reported outbreaks represent only a small proportion of the true illness burden. According to FoodNet data, <1% and 6%, respectively, of reported
Conclusions
The increasing numbers of reported outbreaks in recent years highlight chicken liver as an important foodborne illness vehicle. The consumption of inadequately cooked chicken liver dishes noted in this study poses a food safety concern made greater by the strong evidence suggesting the presence of pathogens inside chicken liver. To address this problem, public health officials and stakeholders should collaborate to pursue multipronged prevention strategies, including enhancing illness and outbreak surveillance, pursuing needed research, and encouraging food preparers to fully cook chicken liver dishes.
Footnotes
Acknowledgments
The authors thank the local, state, and federal officials who investigated and reported these outbreaks. The authors completed this study during the course of their employment with the U.S. Federal Government. No other financial support was received for this study.
Disclaimers
The findings and conclusions in this preliminary publication have not been formally disseminated by the U.S. Department of Agriculture and should not be construed to represent any agency determination or policy.
The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of the Centers for Disease Control and Prevention.
Disclosure Statement
No competing financial interests exist.
