Abstract
Abstract
Background:
Clostridium septicum is a gram-positive, anaerobic, spore-forming bacilli found in the gastrointestinal tract. It rarely causes spontaneous infections that are associated with high mortality. Association of Clostridium infection with colorectal malignancies or immunosuppression have been reported previously, tumors of the ascending colon are described in most cases. The anaerobic glycolysis of the tumor produces an acidic, hypoxic environment favoring mucosal ulceration and bowel into bloodstream translocation, leading to fulminant sepsis, infected liver metastases, and hollow viscous perforation presenting as pneumoperitoneum.
Case Presentation:
We report a case of a 61-year-old male with type 2 diabetes mellitus and chronic lymphocytic leukemia who presented with five-day generalized abdominal pain and fever. His symptoms were caused by colon cancer with liver metastases infected with Clostridium septicum. The clinical outcome and management of the case is reported.
Conclusion:
In patients with hematologic or colorectal cancer and gas-forming liver abscesses, the possibility of Clostridium septicum infection and metastatic cancers should be considered. The aim of this case is to stress the importance of maintaining a high suspicion of Clostridium septicum infection in patients with underlying colonic malignancy.
We report a case of a 61-year-old male who had significant comorbidities including type 2 diabetes mellitus, chronic lymphocytic leukemia (with good prognostic factors that did not need any treatment), and chronic gastritis. He had not undergone any surgical interventions previously. His medications included esomeprazole 20 mg every 24 hours, metformin, iron, and lorazepam.
The patient was admitted as an emergency with a five-day history of progressively worsening right upper and lower quadrant pain associated with diarrhea and fever (39°C). He did not have any nausea or vomiting and had not noticed any urinary or respiratory symptoms.
On examination, he was pyrexial (temperature, 39°C), with tachypnea (respiratory rate, 24 breaths per minute), and tachycardia (heart rate, 165 beats per minute). His blood pressure was 99/63 mm Hg and his Glasgow Coma Scale score was 15/15. Deep palpation of the upper and lower abdominal right quadrants caused pain and a mass was felt.
The patient's blood tests revealed the following: alanine aminotransferase (ALT) 284 U/L (5–41); creatine kinase (CK) 393 U/L (0–195); procalcitonin 30.76 ng/mL (> 10 ng/mL high probability of severe sepsis); leukocytes 40,000 per microliter (4.5×103–11×103); neutrophils 24.6% (43–65); and prothrombin index 35% (65–120); international normalized ratio (INR) 2.21; functional fibrinogen 779 mg/dL (200–450); D-dimer 13.3 mcg/mL (< 0.5).
The computed tomography (CT) scan showed several 8–9 cm collections at the V and VI segments of the right hepatic lobe. Those collections seemed to be filled with necrosis and gas and were suggestive of abscesses. Inflammation and perforation of the cecum, free intra-peritoneal fluid, pneumoperitoneum, portal pneumatosis, and sub-diaphragmatic gas were also reported (Figs. 1–3).

Axial computed tomography (CT) view showing the metastases with gas and pneumoperitoneum.

Axial computed tomography (CT) view showing the metastases with gas and pneumoperitoneum.
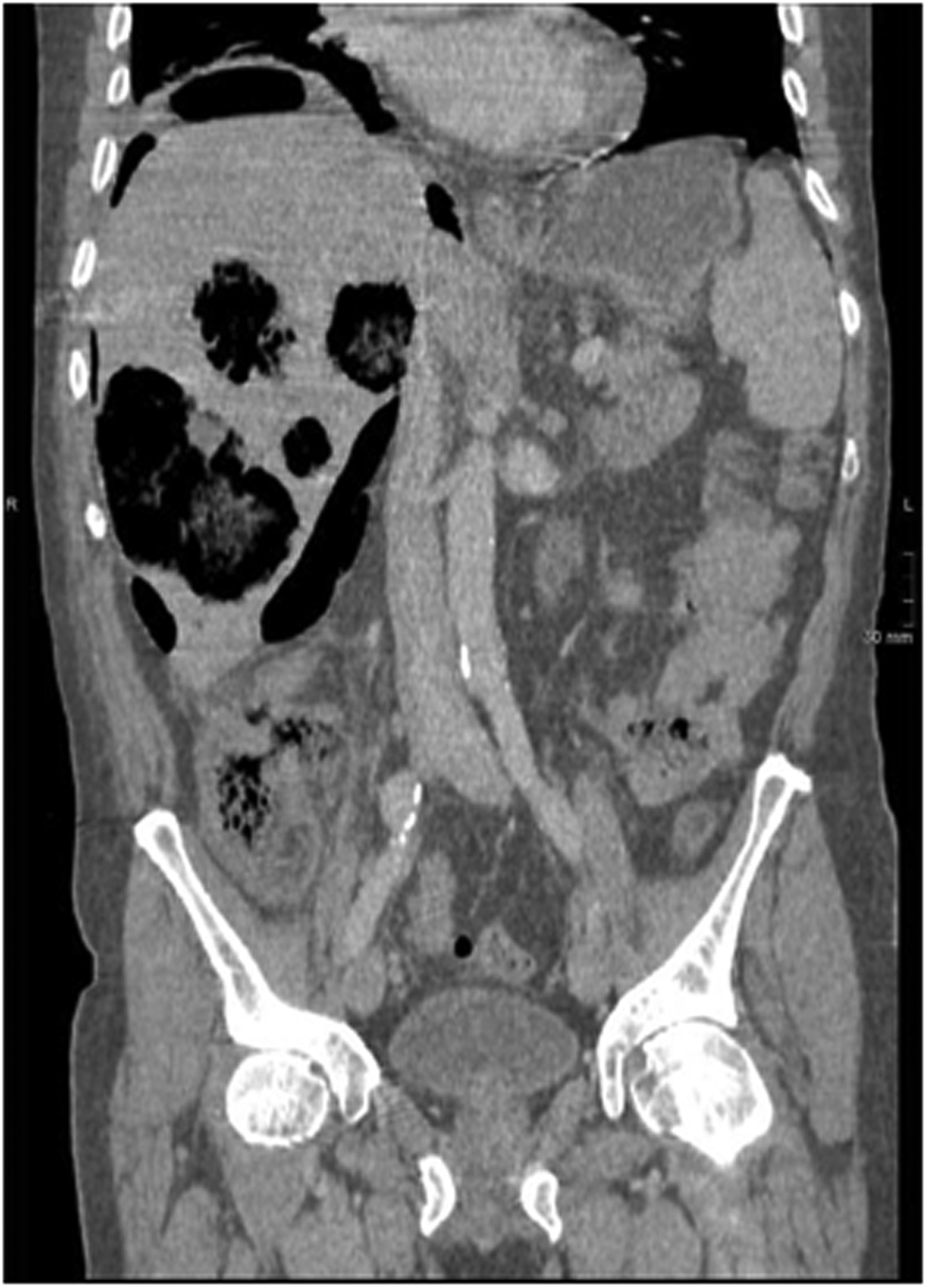
Coronal computed tomography (CT) view showing the metastases with gas and pneumoperitoneum.
Initially, piperacillin/tazobactam 4/0.5 g, paracetamol 1 g, 250 ml bicarbonate 1 M, and 2,000 ml crystalloids were administered intravenously, based on the Surviving Sepsis Campaign protocol. In view of the clinical and radiologic findings, the patient underwent transcutaneous drainage of the liver abscesses as well as emergency right hemicolectomy and terminal ileostomy. Intra-operatively, an inflammatory perforated mass was identified in the cecum.
The abscess cultures showed presence of Clostridium septicum and coagulase-negative staphylococci. The anatomo-pathologic examination of the right hemicolectomy specimen revealed an intestinal adenocarcinoma stage G3a pT4a pN1b L1 V1 Pn. The hepatic lesions were suspected to be metastases so a biopsy was performed, confirming metastatic disease (M1).
During the post-operative period, new transcutaneous drains were inserted and the initial broad-spectrum antibiotic regimen of intravenous piperacillin/tazobactam was changed to meropenem and clindamycin. Finally, after 27 days of hospital stay the patient was discharged with home hospitalization for intravenous treatment and incision care. The patient followed up with the oncologist for palliative chemotherapy.
Discussion and Literature Review
Clostridium septicum is a gram-positive, anaerobic, spore-forming bacilli found in the gastrointestinal tract. Rarely it causes spontaneous infections that are associated with high mortality. Association of Clostridium infection with colorectal malignancies, hematologic disease, diabetes mellitus, or immunosuppression has been reported previously, with tumors of the ascending colon being described in most cases [1].
Kornbluth et al. [2] reviewed 162 cases of Clostridium septicum infection, demonstrating that 81% of patients had an associated malignancy, of whom 40% had an associated hematologic malignancy and 34% had an associated colonic carcinoma [2]. Therefore, in the absence of hematologic malignancy, colonoscopy is warranted to evaluate the presence of colonic carcinoma [3].
In our case there was a history of diabetes mellitus type 2, chronic lymphocytic leukemia, and previously undiagnosed colorectal cancer with liver metastases. Liver abscesses typically complicate large metastases that have become ischaemic leading to an ideal anaerobic environment for the growth of Clostridium septicum. This may result in rupture into the sub-diaphragmatic space causing gas-forming liver abscesses and pneumoperitoneum [4–6].
The treatment of Clostridium septicum bacteremia consists of early broad-spectrum antibiotic therapy and surgical debridement [7,8]. Blood cultures should be obtained promptly to achieve a timely diagnosis and aid in future antibiotic regimens. The empirical antibiotic treatment of choice includes intravenous piperacillin/tazobactam 4/0.5 g every 6 hours and intravenous metronidazole 500 mg every 8 hours [9].
Conclusion
In conclusion, in patients with hematologic or colorectal cancer and gas-forming liver abscesses, the possibility of Clostridium septicum infection complicating metastatic disease should be considered.
