Abstract
Abstract
Background:
Curvularia is a black mold that resides primarily in the soil of warm tropical environments and infects plant species. Reports of human disease and infection caused by this organism are rare, primarily occur in immunocompromised patients, and have a high incidence of mortality. To date, there has only been one case report of Curvularia infection published in burn patients.
Case Presentation:
We describe a case series of two early, invasive Curvularia infections in burn patients treated at the Regional Burn Center in Mobile, Alabama. Both patients were Caucasian males between 50 and 60 years of age, married, insured, with 50%–60% total body surface area (TBSA) second- and third-degree burns. Flames were reportedly extinguished using stagnant water and mud, respectively. Both patients presented from the Gulf Coast, one from Florida and the other from Mississippi, over a span of 15 months. No patients were excluded from this study or have been lost to follow-up. A review of the literature related to the treatment of this uncommon infection was also conducted.
Results:
After suffering Curvularia infections, both patients included in this study survived. We believe morbidity was improved by early identification of cutaneous manifestations and clinical symptoms of invasive fungal infection. Identification lead to urgent surgical debridement and use of intravenous (IV) and topical antifungal agents that aided in the complete resolution of disease resulting in limited morbidity. Both patients were discharged to rehabilitation centers before returning home.
Conclusions:
Aggressive wound surveillance, routine quantitative tissue cultures, and early excision and closure are imperative in the prevention of invasive, life-threatening fungal colonization. Upon suspicion of fungal infection, urgent treatment with IV antifungal agents, topical antifungal soaks, and excision is imperative. Best practices regarding prophylaxis with stagnant water and environmental exposures are unknown.
Curvularia infection complicating the treatment of burns has only been reported once in the burn literature [1]. However, over the course of 15 months, our Regional Burn Center on the Gulf Coast in Alabama treated two patients with such an infection. Also unusual for most burn centers, we have become accustomed to treating Vibrio and Aeromonas infections in our patients. A study of dematiaceous fungal keratitis along the Gulf of Mexico demonstrated a causal pathway linking climate, environmental mycoflora, and keratomycosis indicating that it is likely the humid air, mix of salt and fresh water, and rich soil that provides a natural environment to these bacterial and fungal species [2].
Curvularia species belongs to the hyphomycete class of fungi. Mostly found in tropical regions, it is a facultative pathogen of many plant species and of the soil, but can also be isolated from air, animals, and humans [3]. Curvularia species is characterized further as a dematiaceous mold that can cause human infection usually involving the skin, subcutaneous tissue, eyes, and occasionally the paranasal sinuses or central nervous system [3,4]. Infection occurs through direct inoculation via intravascular devices or by inhalation [4]. Such infections are referred to collectively as phaeohyphomycoses. Histopathologically, the lesions show brown-walled septate hyphae or yeast, or a combination of both. Presentations vary including papulonodules, verrucous, hyperkeratotic or ulcerated plaques, cysts, abscesses, pyogranuloma, and non-healing ulcers or sinuses [3].
This study presents two cases of early, invasive Curvularia infection in burn patients from the Gulf Coast region and reviews the literature related to the treatment of this uncommon infection. Both patients were Caucasian males between 50 and 60 years of age, married, insured, with 50%–60% total body surface area (TBSA) second- and third-degree burns. Flames were reportedly extinguished using stagnant water and mud. Both patients presented from coastal cities in Florida and Mississippi over the span of 15 mo. No patients were excluded from this study or were lost to follow-up.
Case Presentation
The first case is a 52-year-old Caucasian male who presented with 52% TBSA deep partial and full thickness burns to his face, extremities, and trunk secondary to a welding shop explosion on the Gulf Coast. The flames were extinguished reportedly using stagnant water from a dog's water bucket. The patient had no significant comorbidities. On hospital day four, he developed dematiaceous, circular lesions to his right lower leg eschar (Fig. 1).
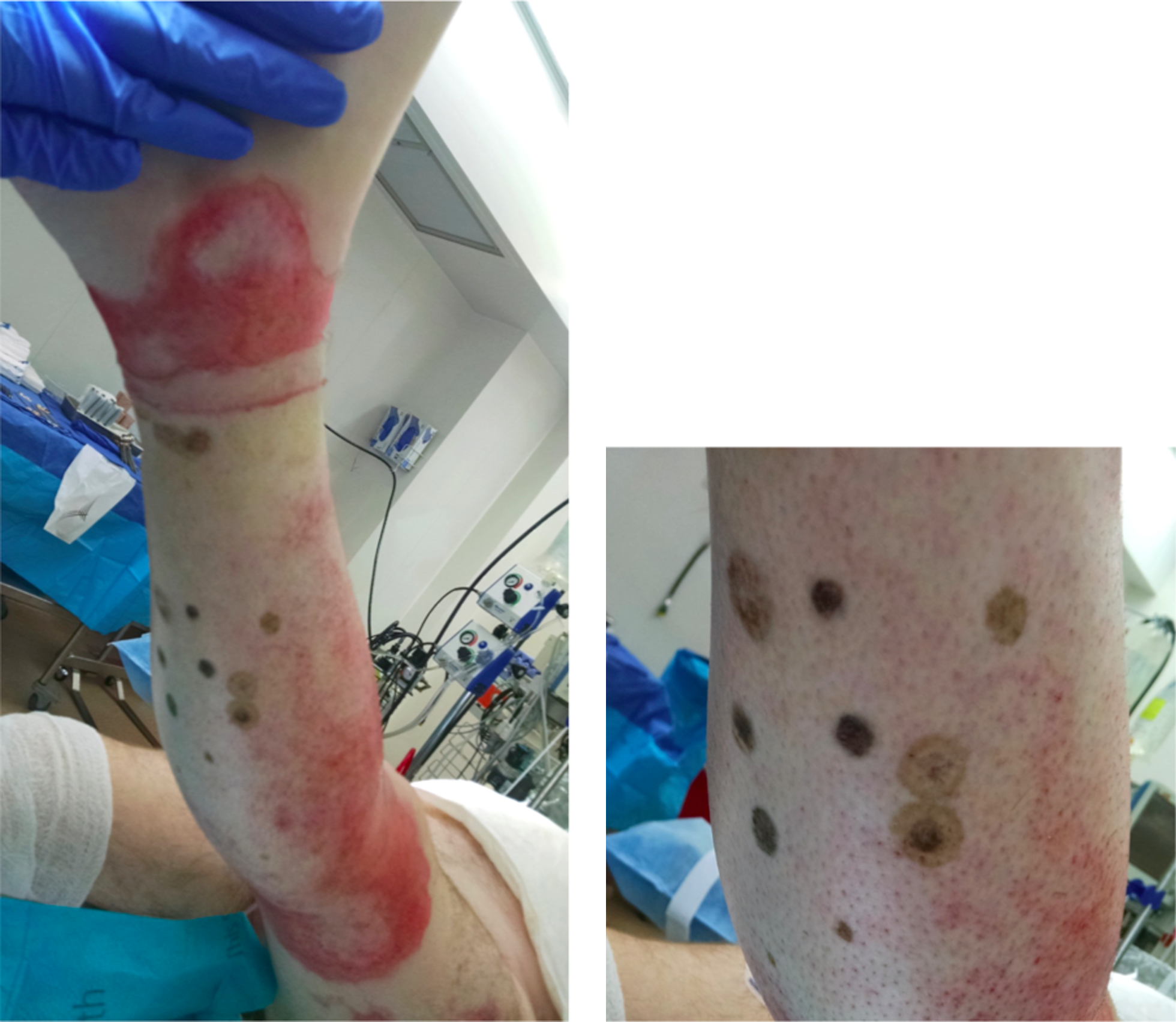
A 52-year-old male with 52% total body surface area (TBSA) burns and dematiaceous, circular lesions of his right lower extremity representing invasive Curvalaria infection.
Aggressive management of the suspected fungal infection was initiated, including immediate excisional debridement of the bilateral lower extremities, topical and systemic amphotericin B administration, and intravenous meropenem and vancomycin. Amphotericin-B and sulfamylon soaks were applied four times each day. Initial stains revealed no fungal elements. On hospital day six, the patient exhibited a leukopenia and increasing insulin requirements. Serum antigens were positive for (1-3)-beta-d glucan but negative for galactomannan and acid-fast bacteria. Voriconazole was added to cover for Fusarium. On hospital day seven, fungal re-growth was noted and the patient underwent urgent re-excision of the bilateral lower extremities to fascia. As he stabilized, the remainder of his burns were excised and underwent staged, serial autografting. On day 17, fungal culture revealed Curvularia. The patient was treated with a two-week course of antifungal agents dated from the time of source control. Although slow to recover, the patient was discharged for ongoing outpatient rehabilitation on hospital day 69.
The second case is a 60-year-old previously healthy Caucasian male who presented from the scene of a trash fire explosion on the Gulf Coast with 56.5% TBSA deep second- and third-degree burns to his neck, bilateral upper extremities, right hand, anterior and posterior trunk, scrotum, and bilateral lower extremities. The patient reportedly rolled in mud to extinguish himself. On arrival, the patient was hemodynamically stable with an endotracheal tube in place. Bronchoscopy was negative for evidence of inhalation injury.
The wounds were debrided and treated with hypochlorous acid soaks. Staged excision and grafting began on hospital day four. His wounds appeared to have some biofilm and he was empirically administered vancomycin and meropenem. Quantitative cultures obtained at that time eventually revealed Staphylococcus aureus. On hospital day six, the laboratory identified mold in the cultures and micafungin was added. Serum for (1-3)-beta-d glucan and galactomannan were negative. On hospital day 11, the wounds appeared colonized, and the patient was taken to the operating room for debridement of his right lower extremity. Wounds were treated with topical amphotericin B and mafenide soaks four times each day with twice daily dressing changes. Final fungal culture results revealed Curvularia species on hospital day 12. After Curvularia was identified, voriconazole was added to micafungin for a total course of two weeks of antifungal agents. His skin grafts healed well with more than 95% graft take. The patient convalesced and was discharged to a skilled nursing facility for further rehabilitation on hospital day 40.
Discussion
Although infections with environmental molds are rare, there are an increasing number of reports in the literature of opportunistic fungal pathogens causing disease in immunocompromised patients over the past decade [4,5]. A high mortality rate is associated with disseminated phaeohyphomycoses caused by rare dematiaceous molds, thus early diagnosis and high clinical suspicion are critical [4]. Invasive infections can manifest quickly, whereas cultures can take weeks to confirm diagnosis. Serum markers for (1-3)-beta-d glucan and galactomannan can be utilized in early identification and treatment of invasive fungal infections. Although not definitive for diagnosis, the chromogenic assay of for (1-3)-beta-d glucan offers a non-invasive method for potential diagnosis because this is a key component of fungi cell walls. Similarly, galactomannan antigen is an Aspergillus-specific antigen used in conjunction with other diagnostic procedures to aid in the diagnosis of invasive Aspergillus.
As a result of limited data, the prevalence of invasive Curvularia infection is unknown. A large restrospective study found that over a 15-y period there were 39 patients with proven or probable invasive dematiaceous fungal disease, of which eight were associated with Curvularia. All skin lesions were located on the limbs. Of the nine patients who had skin infection in the context of hematogenously disseminated phaeohyphomycosis, all had growth in fungal culture from skin biopsy allowing for identification of the causative organism. Treatment algorithms differed and included surgery and amphotericin B combined with either a triazole or an echinocandin. Despite treatment, 33% of the 39 patients died within 12 wks after receiving a diagnosis of phaeohyphomycosis infection. After another review involving 72 cases of disseminated phaeohyphomycosis yielded only five cases attributed to Curvularia. Of the 72 cases, fever was the most common symptom occurring in 76% of patients and cutaneous lesions were seen in 33% of patients, while blood cultures were positive in only 50% of patients. While multiple antifungal agents were utilized in treatment, amphotericin B was the most common. However, no single drug was associated with improved outcome [4].
Another recent study analyzed experimental data on the efficacy of antifungal drugs, specifically amphotericin B, posaconazole and voriconazole, using murine models of disseminated infection caused by the two species that are most commonly involved in human infection, Curvularia spicifera and Curvularia hawaiiensis [5]. Irrespective of the infecting strain, all treatments significantly prolonged survival compared with the controls, however, only the azoles reduced fungal burden with statistical significance [5]. In a 2016 case published in the Journal of Cutaneous Pathology, a patient with acute myeloid leukemia taking prophylactic fluconazole reportedly developed a cutaneous fungal infection from Curvularia species [4]. The patient was treated with intravenous voriconazole for four days and then transitioned to the oral formulation [4]. The patient's initial lesion and distant nodules from dissemination regressed. She received a total of 20 wks of voriconazole and at her 24 wk follow-up the patient had not developed any new fungal nodules, despite continued immunosuppressive treatment for relapsed acute myeloid leukemia (AML) [4]. Three case reports of phaeohyphomycosis infection in India were treated with oral itraconazole for four months and surgical excision was curative with no recurrence of lesions in six months.
Conclusion
Invasive infection is the primary cause for death and morbidity after a burn injury, accounting for 51% of burn-related mortalities [6]. Although clear guidelines have not been established, strict infection control measures remain key to prevention of invasive fungal infection. Fever, tachycardia, and leukocytosis are poor indicators of infection because of the altered metabolism of burn patients. Instead, one must rely on increasing blood glucose, increasing ventilator requirements, and wound appearance among other clinical and physical exam findings. Aggressive wound surveillance, and early excision and closure are imperative in the prevention of invasive, life-threatening infection. Upon recognition of fungal infection, urgent treatment with intravenous antifungal agents, topical antifungal soaks, and excision is imperative. As a result of limited data surrounding the treatment and scarcity of reported clinical cases, a single, standard treatment has not yet been established [3,5]. However, the cornerstones of treatment of invasive fungal infection remain systemic mono- or dual therapies along with topicals and surgical excision [7]. In addition, best practices regarding prophylaxis with stagnant water and environmental exposures are unknown and need to be studied further.
Footnotes
Author Disclosure Statement
No competing financial interests exist.
