Abstract
Abstract
Background:
Small intestine perforations in adults occur usually as a result of obstruction and ischemia, hernia strangulation, or trauma. When patients are found to have small intestine perforations, the location of the defect is commonly described as the distance from the ligament of Treitz, which is the suspensory ligament of the duodenum that landmarks the duodenojejunal junction. Few cases exist in which perforations occur right at the ligament of Treitz. Here, we report a rare case of an occult small intestine perforation at the ligament of Treitz in a patient with cirrhosis.
Case Presentation:
A 75-year-old Caucasian male with Child-Pugh class B alcoholic cirrhosis presented to the emergency department with acute abdominal pain caused by a recurrent umbilical hernia. On physical examination, he had a moderate amount of ascites and a tender mass to the right of the umbilicus. The patient was taken to the operating room (OR) for open reduction and umbilical repair. A fat-containing hernia with a small defect was reduced and 2.5 L of clear ascites was drained. Six hours after the surgery, the patient developed abdominal pain and bilious content began to drain. With differential diagnosis of inadvertent enterotomy or duodenal ulcer perforation, he was urgently taken back to the OR. No clear perforation was found: there was no duodenal ulcer, no diverticular perforation, and no inadvertent enterotomy. An intra-operative gastroscopy was undertaken and an intra-abdominal water test was performed with air insufflation. Bubbling was observed from a 5 mm perforation at the ligament of Treitz. The location of the perforation and its distance from the hernia repair excluded the possibility of iatrogenic perforation.
Conclusion:
This case is a reminder to examine the ligament of Treitz when searching for a perforation and that the use of intra-operative endoscopy can be useful in diagnosing occult intestinal perforations.
Small intestine perforations in adults occur usually as a result of obstruction and ischemia, hernia strangulation, or trauma [1]. When patients are found to have small intestine perforations, the location of the defect is described commonly as the distance from the ligament of Treitz, which is the suspensory ligament of the duodenum that landmarks the duodenojejunal junction. Here, we describe a rare case in which an occult perforation of the small bowel occurred right at the ligament of Treitz.
Case Report
A 75-year-old Caucasian male who had a history of end-stage alcoholic liver cirrhosis presented to the emergency department with acute right-sided abdominal pain with associated nausea and vomiting. In addition to Child-Pugh class B cirrhosis, ascites, and portal hypertension, he also had coronary artery disease with previous myocardial infarction, hypertension, aortic repair, Barrett esophagus, rheumatoid arthritis, and hypothyroidism. His past surgeries included laparotomies for perforated and bleeding duodenal ulcers, umbilical hernia repair, and coronary artery bypass grafting (CABG). Physical examination revealed a tender incarcerated umbilical hernia. Investigations including three views of abdominal radiograph and blood work were of no significance except for an elevated international normalized ratio (INR) of 1.6. An attempt to reduce the hernia under conscious sedation in the emergency department was unsuccessful, so the patient was brought urgently to the OR for a recurrent umbilical hernia repair. The hernia sac was dissected from the surrounding subcutaneous tissue through an infra-umbilical incision and opened. It contained a small amount of fat, no bowel, and 2.5 L of clear ascites was drained. The ascites was sent to microbiology and showed no microbial growth. Primary fascial repair was performed, and a 10 mm Jackson-Pratt (JP) drain was placed in the pelvis to drain the ascites and protect the fascial repair. The pathology returned later showing chronic inflammation and cystic changes.
Six hours after the operation, the patient was found to have a distended abdomen, peritoneal signs, and bilious drainage from his JP drain. With a differential diagnosis of inadvertent enterotomy or perforated duodenal ulcer, the patient was returned to the OR for an exploratory laparotomy. During the second surgery, extensive lysis of adhesion was performed. The small and large bowels were inspected thoroughly twice and there was no obvious perforation despite the large amount of intra-peritoneal enteric bilious content. Because the patient had a history of upper gastrointestinal (GI) bleeding and perforated duodenal ulcer, an upper GI endoscopy was performed. An intra-operative gastroscopy was performed with a leak test (placing saline in the abdomen during the endoscopic insufflation). Gastric and duodenal mucosa appeared normal but there was some bubbling through the small bowel mesentery and upper abdomen. With a more focused exploration, the small bowel was lifted and a 5 mm perforation at the duodenojejunal junction right at the ligament of Treitz was found (Fig. 1). A biopsy of the perforation was not performed to avoid a more complex repair. The repair was done with two layers of absorbable sutures and two JP drains were placed in the pelvis near the repair. Because the initial ascites culture showed no bacterial growth and the anatomic location of the perforation was far from the hernia repair, the possibility of iatrogenic injury was excluded, and this was diagnosed post-operatively as an occult small bowel perforation.
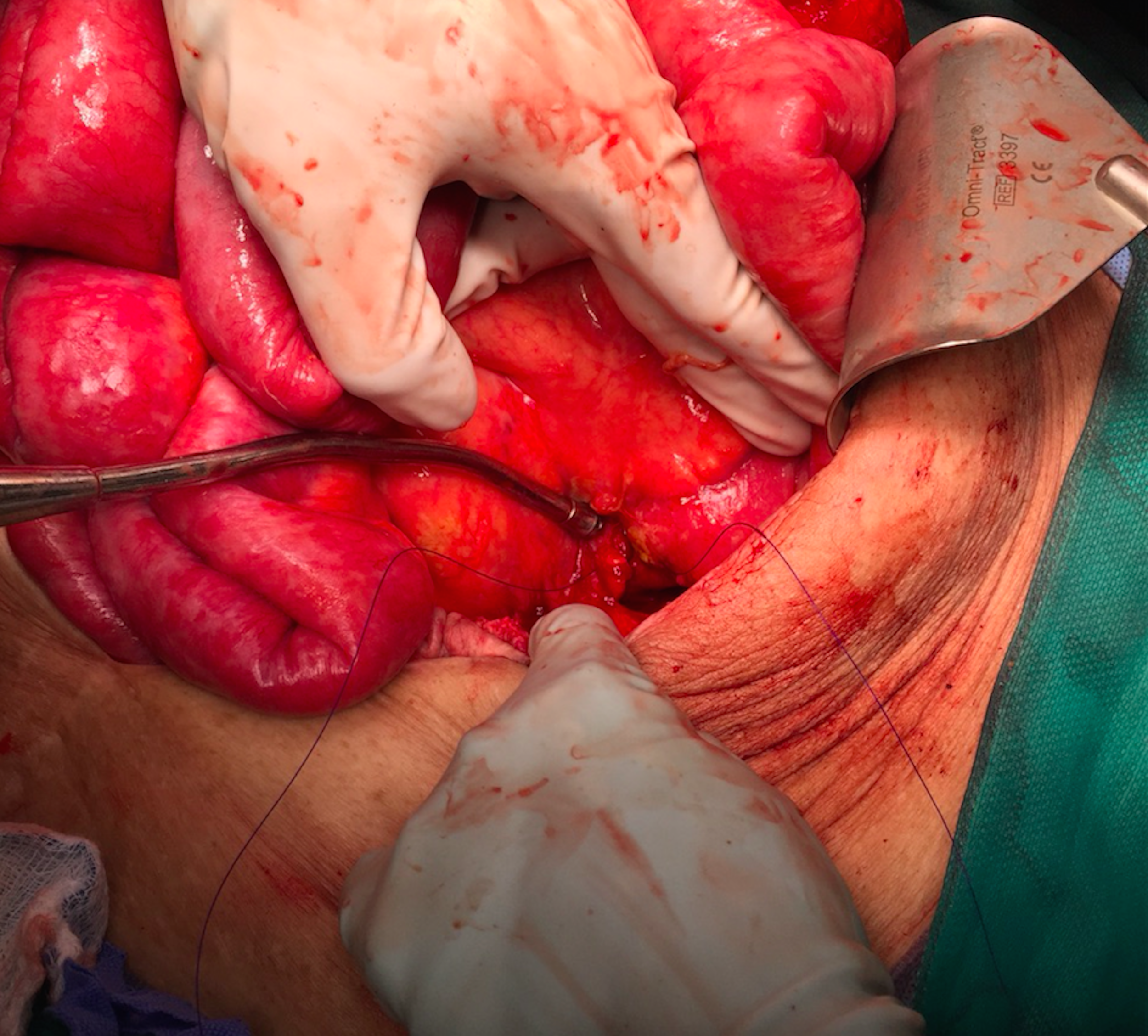
Intra-operative photo of the 5 mm occult small intestine perforation at the ligament of Treitz. The suction tip marks the location of the ligament and perforation.
The patient was started immediately on empiric piperacillin-tazobactam and fluconazole. Unfortunately, he developed severe catecholamine-resistant septic shock. Cultures of the bilious fluid later showed Klebsiella pneumoniae, Enterococcus species, Candida albicans, and Candida glabrata. On post-operative day six, he became acutely tachycardic and hypotensive and developed atrial fibrillation that was unresponsive to cardioversion and digoxin administration. His abdomen was painful and chest radiograph revealed a pneumoperitoneum (Fig. 2). The drains also started to leak enteric content, again suggesting another intestinal perforation or leak. Because of his comorbidities, a goals of care discussion took place and the patient was transitioned to total compassionate care.

Chest radiograph revealing a pneumoperitoneum.
Discussion
Umbilical hernias occur commonly in patients with cirrhosis and ascites [2,3]. This is believed to be caused by the presence of ascites increasing intra-abdominal pressure, weakness of the abdominal wall, and portal pressure transmission to the umbilicus [4,5]. Hernia repair in these patients carries a substantial risk of morbidity, mortality, and recurrence [6]. A study done by Leonetti et al. [6] found morbidity to be 16.6%, mortality 8.3%, and recurrence 16.6% after umbilical herniorrhaphy in such patients. This is likely because these patients often experience major complications such as ascites leakage, abdominal wall necrosis causing ulcers, strangulation, rupture, or infections [6,7]. The patient in the present study had a long history of cirrhosis and uncontrolled ascites and presented with a recurrent umbilical hernia. Given this information and the fact that the patient experienced serious complications just hours post-herniorrhaphy, it was assumed that his complications were caused by the surgery and he was diagnosed clinically with an inadvertent small bowel injury caused by the hernia repair. It was therefore unusual to find a spontaneous small bowel perforation at the ligament of Treitz, far from the herniorrhaphy site (Fig. 1).
Small intestine perforations in adults occur usually as a result of obstruction and ischemia, hernia strangulation, or trauma [1]. Although the patient in the present case had a hernia, none of these common causes were responsible for his perforation, making it a rare presentation. The most interesting rarity in this case was the location of his perforation—the ligament of Treitz. It is rare for perforations to occur at this exact location; in fact, perforations often are described in terms of location as the distance from the ligament of Treitz. To demonstrate the rarity of the present case, a review of the English literature was done to find cases of adult patients with cirrhosis and non-iatrogenic perforations near the ligament of Treitz. The search was limited to the duodenum and jejunum to pick up the cases with perforations closest to the ligament. Only cases that described the location of the perforation in specific terms were included. Overall, 12 cases were found and none reported the ligament of Treitz as the location of a perforation, supporting this finding as rare and potentially unique (Table 1). However, because much of the language used to describe the locations of the perforations in many of the studies found was vague, it is possible that there are other cases similar to the present. Regardless, this study still serves as an important reminder to examine the ligament of Treitz when experiencing difficulty locating a perforation. For example, because the ligament of Treitz is such an unusual location for a perforation, it was not the first place explored in the present case: the duodenum, small bowel, and large bowel were examined thoroughly twice and an upper GI endoscopy was applied before the perforation was located. Therefore, this case is presented to emphasize the fact that the ligament of Treitz is a potential location for small bowel perforations and bring awareness to it.
Reported Cases of Non-Iatrogenic Duodenal and Jejunal Perforations in Adults with Cirrhosis
Only cases with specific descriptions about perforation distance from the ligament of Treitz were included.
Abdominal sepsis is a common complication after intestinal perforation, particularly in patients with cirrhosis who are especially susceptible to bacterial infection [19]. The cultures from the drainage fluid revealed Klebsiella pneumoniae, Enterococcus species, Candida albicans, and Candida glabrata, which have been documented in the abdominal fluid of patients with gastroduodenal and small intestine perforations [20]. Large amounts of this infectious fluid continued to drain from this patient and he was believed to have likely not healed his repair on post-operative day six. Given the patient's comorbidities and uncontrolled sepsis, the perforation at the ligament of Treitz was the cause of his death. It is an unusual and important area of small bowel perforation that can be missed easily.
Patients who present with distal duodenal ulcers, multiple, or refractory peptic ulcers should always prompt the possibility of relatively rare conditions such as Zollinger-Ellison Syndrome. The patient reviewed in this study had a previous history of a perforated and bleeding duodenal ulcer and now a very distal duodenal ulcer perforation. So, not having succumbed to this severe septic insult, more investigations including a fasting serum gastrin level would have been warranted.
Conclusion
In conclusion, although it is rare, occult perforation of the small bowel at the ligament of Treitz should be considered in patients with suspected perforation. The use of intra-operative endoscopy can be helpful in localizing unclear sites of intestinal perforation.
Footnotes
Acknowledgments
We would like to thank Dr. Saifee Rashiq for the intra-operative photograph, the University of Alberta's Department of Surgery and Wynne Rigal Award for funding, and Ms. Linda Slater for help with the literature review.
Author Disclosure Statement
No competing financial interests exist.
