Abstract
The microbiome of the human body represents a symbiosis of microbial networks spanning multiple organ systems. Bacteria predominantly represent the diversity of human microbiota, but not to be forgotten are fungi, viruses, and protists. Mounting evidence points to the fact that the “microbial signature” is host-specific and relatively stable over time. As our understanding of the human microbiome and its relationship to the health of the host increases, it is becoming clear that many and perhaps most chronic conditions have a microbial involvement. The oral and gastrointestinal tract microbiome constitutes the bulk of the overall human microbial load, and thus presents unique opportunities for advancing human health prognosis, diagnosis, and therapy development. This review is an attempt to catalog a broad diversity of recent evidence and focus it toward opportunities for prevention and treatment of debilitating illnesses.
Introduction
The interconnected network of microorganisms (bacteria, viruses, fungi, and protists) that live in and on our body take up residence mainly in the oral and nasal cavities (oral microbiota), on the skin (skin microbiota), in the gastrointestinal (GI) tract (gut microbiota), and in females, in the genital tract (mostly as vaginal microbiota) (Fig. 1).1–8 Mounting data show that for each individual, the collective composition of their microbiota (microbiome)3,9,10 is host-specific and relatively stable over time.4,11–13
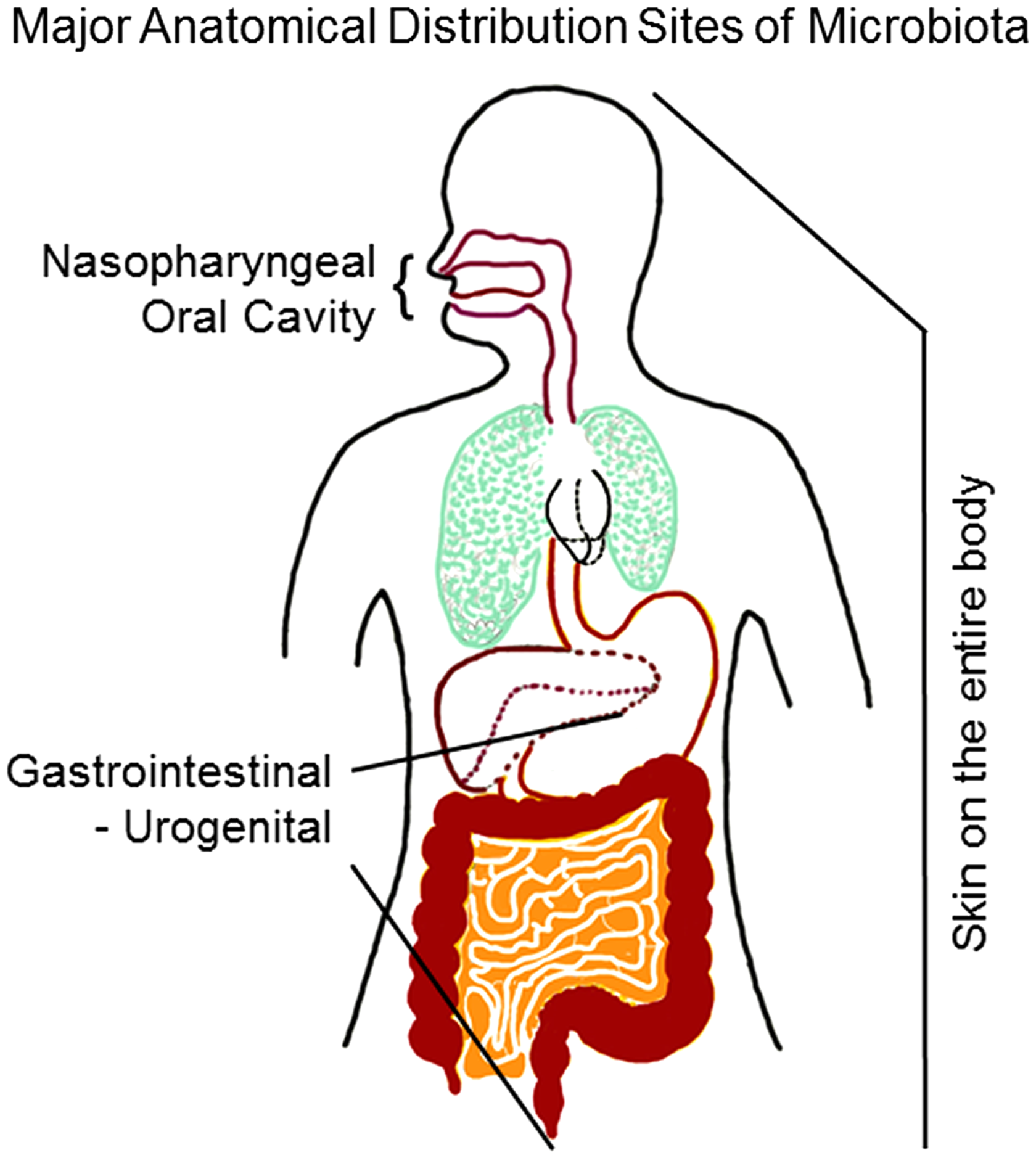
Interconnected network of microorganisms: Major regions of the human body where bacteria, viruses, fungi, and protists live in or on.
Of the different ecosystems of flora that inhabit the human body, the gut microbiota system is emerging as the preeminent “microbial organ” of study, and there is great expectation that by better understanding the complexity of the role of microbiota, our microbiome will become an indispensable and integral part of our personalized healthcare in preventing and/or treating diseases more effectively and in a more precise and targeted clinical approach.3,14–19 Indeed, gaining a better understanding of the gut microbiota system may help to enable a revolution in precision medicine20,21 across a wide range of diagnostic, preventive, and therapeutic approaches.15,17
Of the 100 trillion or so microorganisms that make up the human microbiome (accounting for 1–3% of a person's body weight),22,23 approximately half (1–2 kg) reside in the GI tract, which hosts the largest and most diverse collection.22,24 A symbiotic host–flora relationship25,26 has evolved between them and us, and as a result, we are dependent on our gut microbes to perform many functions that are essential to our health and survival. They chemically transform and metabolize xenobiotics, which we take willingly (e.g., pharmaceuticals) and/or unwillingly (e.g., environmental chemicals in the air we breathe and extraneous additives in our foods),27–29 they play a fundamental role in the induction, basic development, training, and function of our immune system,26,30–33 and in the process of helping us digest fibrous foods, they produce short-chain fatty acids25,26,34 that inhibit inflammation35–37 and affect epigenetic regulation of gene expression by influencing multiple regulatory mechanisms (Table 1). Importantly, these regulatory mechanisms include acetylation of DNA-associated histone proteins and methylation of DNA.10,33,38–41
Symbiotic Host–Flora Relationship: Examples of Important Roles That Gut Microbes Play in Functions Essential to Human Health and Survival
SCFA, short-chain fatty acid.
Consequently, it should not be surprising that gut dysbiosis (also called dysbacteriosis or gut microbial imbalance or maladaptation) can profoundly affect our wellbeing, 42 lead to the manifestation of neuropsychiatric symptoms and conditions,43–46 and underlie a multitude of immune-related disorders (gut–brain-immune axis).47–50 Gut dysbiosis may also exacerbate the progression of a number of common and often chronic diseases. Allergies, atherosclerosis, colorectal cancer, diabetes, inflammatory bowel disease, neurological conditions, and obesity are some examples.50–54
An association between aberrant mental states and digestive disturbances was described by Hippocrates 55 and is the single consistently linked comorbidity reported in the medical literature from ancient times to the present. 56 Diet figures prominently in maintaining or altering the commensal homeostasis composition of the GI microbiota,10,14,54,57–59 and the formulation of diets rich in functional medicinal foods (food-drugs) 60 is driving the emergent field of (neuro)regenerative nutrition.61,62 Although the mechanistic pathways remain mostly obscure, numerous studies show that through reciprocal interactions with the gut–brain axis51,63–67 the gut microbiome can influence neural development, cognition, and behavior.43,46,54,68–70 In turn, changes in behavior can alter the gut microbial composition.43,67,71,72 Consuming the Mediterranean diet in particular has been demonstrated to improve the health of patients with various chronic diseases26,73–78 (presumably by altering the gut microbiome)26,79–83 and can help mitigate with some degree of efficacy abnormal behavior associated with neuropsychiatric conditions. 68 Thus, opting to incorporate a tailor-made diet plan in the overall treatment of neurologic conditions, including autism and schizophrenia, is increasingly common practice.10,41,68,71,72,84–86 However, for microbiota to play a clinical role in nutritional interventions for maintaining (brain) health,68,87 a reliable diagnostic determination of the gut microbial composition is wanting88–91 —hence, the focus of this forward-looking review article.
Fecal-Derived Microbiota
The majority (∼60%) of the bacterial species residing in the GI tract (primarily the stomach, small intestine, and large intestine) 92 are reported to be unculturable. 93 In addition, gut microbiota are not readily accessed, 52 and characterization of intestinal microbiota currently relies on analysis of the microbial composition in patient-derived fecal (stool) samples,94,95 using DNA-based culture-independent methods as a surrogate representation.71,93,94,96,97 However, the method of sample collection, laboratory handling, analysis, bioinformatic processing of the data, and other factors can greatly affect microbiome study findings.93,98–100 When a healthy state of the gut microbiota is altered, opportunistic bacteria such as Clostridium difficile (sometimes referred to as C. diff.) can grow and cause an infection that is difficult to treat.101,102 Orally administered capsules containing an ecology of bacteria in spore form enriched from stool donations obtained from healthy, screened donors103,104 are being used in an increasing number of clinical trials (www.clinicaltrials.gov). The hope is that such bacterial preparations will be successful in treating various conditions, including C. difficile infection.103,105,106 The composition of fecal microbiota as a valid surrogate representation of the eubiotic (normal) gut microbiome system aimed to be reconstituted71,103,104,107,108 is also gaining greater scrutiny,104,109 particularly if antibiotics were taken within 12 months before stool collection. 98 Indeed, because of resulting alterations in a patient's microbiome, the impact of antibiotics on the life-saving potential of powerful new therapeutic approaches, including immuno-oncology checkpoint inhibitors and other state-of-the-art immune system modulators, is currently a hot topic in medical practice.110,111
Oral Cavity-Derived Microbiota
There is mounting evidence that the spectrum of microbial species living in the mouth is, both in diversity and in composition, a close representation of the microbiota inhabiting the upper GI tract. In a study to evaluate the influence of proton pump inhibitors on the luminal microbiota in the GI tract reported by Tsuda et al., 112 an analysis of microbial samples taken from the oral cavity (saliva), the stomach (gastric fluid), and the colon (stools) of 45 individuals found that the bacteria are similar in overall species richness among the three microbiota irrespective of their different habitats (Fig. 2). Importantly, however, the bacterial composition of the fecal microbiota was shown to be different from those of salivary and gastric fluid microbiota. 112 Furthermore, the interindividual variability of fecal microbiota was much higher compared with that of salivary and gastric fluid microbiota as might be expected with the colon habitat being completely different from the other two habitats with respect to their biological and ecological features. 112 Curiously, in a seemingly unconnected relationship, the placental microbiome 8 is also reported to share similarity with that of the oral cavity and not those of the more proximal vaginal or gut flora.113–116
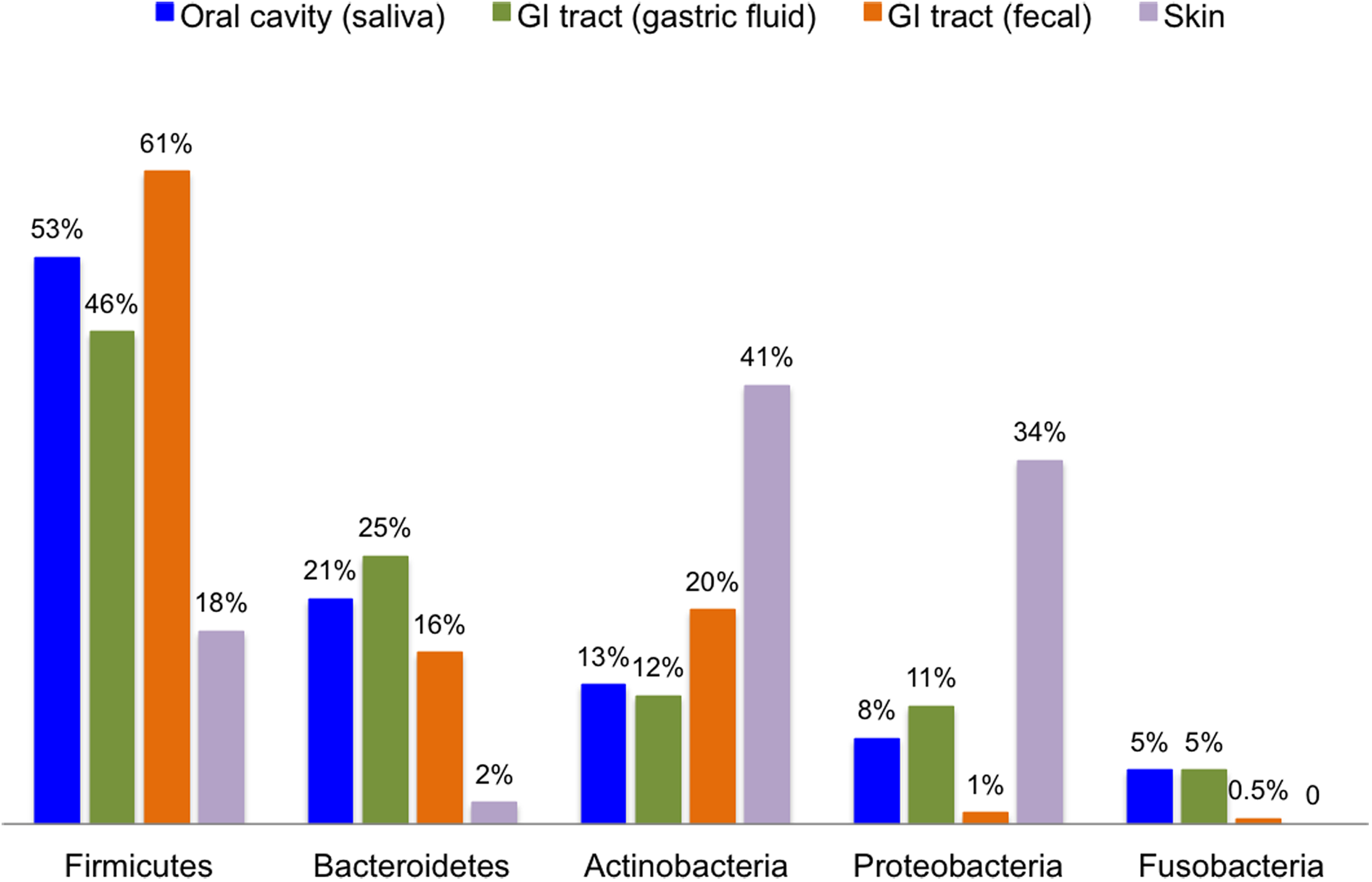
Relative Composition (%) of the major phyla of bacteria found in microbiota samples. Data for Oral cavity, GI tract (gastric fluid), and GI tract (fecal) were from Tsuda et al. 112 Skin microbiota composition was obtained from van Rensburg et al. 117 Genital tract (vagina) information, from Miles et al., 8 is highly variable (Firmicutes > Proteobacteria > Bacteroidetes > Actinobacteria >> other) and is not plotted. GI, gastrointestinal.
Rapid advances in genome sequencing technologies have given rise to user-friendly commercially available kits with buccal swabs for collecting genomic material. 118 (It is worth noting the current lack of standards, accessible control data, and variable results from one commercial provider to another; nonetheless, our expectation is that standardization and suitable comparisons of data and results would quickly follow once the practice is adopted and dentists are more fully engaged.) Located at the entrance of the digestive apparatus feeding into the GI tract, the mouth (oral cavity) also provides a convenient, accessible site for swabbing microbial samples.118–121 The surfaces of teeth, however, accumulate distinct biofilms (Fig. 3) in comparison to mucosal surfaces in the oral cavity,120,122,123 and some species of microbes from dental biofilms may not be well represented in saliva alone, particularly dental caries-causing bacteria.124,125 Nonetheless, a growing body of evidence suggests that alterations in the oral microbiome have potential in sentinel diagnostic and prognostic applications.102,110,118,120–122,125–129

The major salivary glands and the periodontium.
The healthy human mouth hosts a complex and durable ecosystem of hundreds of different species of microbes that are largely living on the surfaces of teeth as dental biofilms.122,130,131 When microbial homeostasis in the oral cavity is perturbed (as with excessive and frequent consumption of sugar), opportunistic pathogens can selectively grow to dominate dental biofilms (dysbiosis) and predispose the oral cavity to inflammation, infection, and tooth decay.132,133 Although rare, there are reported cases in which a life-threatening bacterial infection from a tooth abscess has spread intracranially to the brain. 134 Better precedent is the apparent link between periodontal health and cardiovascular disease.135–137 Undeniably, antibiotics tend to be overused,138,139 and because antibiotics kill microbes indiscriminately, their misuse in treating infections due to viruses and not bacteria 140 is a leading cause of antibiotic resistance. During antibiotic therapy, unlike the oral and upper gut microbiomes that resist induced perturbation of their eubiotic state, the microbiota in the colon habitat are vulnerable,98,112 and recent exposure to antibiotics is an exclusionary criterion in screening donors for fecal microbiota transplantation. 104
An evolving alternative to antibiotics for selectively killing odor-causing bacteria in the mouth, including pathogenic bacteria that could seed growth in the gut, is a technique that exposes the oral cavity to blue light for a short period of time.141–144 The bacterial compositions in the human oral and gut microbiomes are closely related to each other. 112 Interestingly, a corroborative analogy from the agricultural sector comes into play here. The oral microbiomes of dairy cattle are also similar in constitution with respect to their individual gut microbiomes, and oral samples are routinely taken as noninvasive proxies for assessing the health and potential pathogenic growth of bacteria in the microbial community of their rumen. 145 Another major contributor to antibiotic resistance is the widespread use of antibiotics in animal feed 146 —prompting a legislated ban of all food animal growth-promoting antibiotics in Sweden that has been in effect since 1986. A little more than a decade later the European Union also banned such antibiotic use as a “Precautionary Principle.” 147 However, the total withdrawal of this class of antibiotics is now associated with a deterioration in animal health, including increased diarrhea, weight loss, and mortality due to Escherichia coli and Lawsonia intracellularis in early postweaning pigs and clostridial necrotic enteritis in broilers. 147 To compensate, in the hope of providing a means for reducing the superfluous use of such drugs in our food-production chain in general, agricultural businesses are investigating oral exposure to blue light as a potential replacement for classical antibiotic prophylaxis in food animals.148,149
Leveraging the Oral Microbiome in Diagnosing and Treating Disease
Although the oral cavity is continuously subjected to a barrage of host and environmental insults, the oral microbiome remains relatively stable over time in healthy people.122,131,150,151 Given this fact, changes in the profile of the oral microbiome may provide correlative insight into the onset, progression, and recurrence of disease.102,118,120–122,125–129,152 For example, in a retrospective clinical assessment, Zawadzki et al. 152 examined the oral environment in different human populations and compared and determined the pathogenicity of the resident oral microbiota linked to health complications in three distinct patient groups. A total of 95 patients who required dental or surgical interventions were evaluated for oral cavity microbiota risk factors associated with general or local infections. This included individuals with masticatory system malformations (30 patients), recipients of kidney allografts (30 patients), and a control group of subjects without surgical needs (35 patients) treated conservatively. Using standard microscopy and in vitro culture techniques, differences were noted in bacterial strains between the patient groups requiring surgical treatment and the generally healthy subjects from the control group. The results of this study strongly support the notion that preventive oral cavity microbiota assessment should be performed on patients requiring oral surgery because they are at risk of pathogenic bacterial colonization and infections that have the potential to spread. In general, an examination of the oral cavity environment for infectious microbiota could help reduce surgical complications and also support and/or guide the surgical treatment.
Additional evidence reinforcing similarities between the oral and gut microbiomes is observed in their reciprocal exchange of bacterial pathogens. Diabetes is a systemic chronic illness intimately associated with periodontal disease.131,133,153 Dysbiosis of the oral microbiome can lead to periodontitis,136,153 which promotes pathogenic bacterial growth and facilitates dissemination of oral bacteria systemically.131,153 A causative link between oral pathogens and changes in the composition of the gut microbiota as well as inflammatory changes in various tissues and organs has been demonstrated in mice.154–157 Conversely, emerging evidence shows that diabetes, a chronic disease linked to alterations in the gut microbiome,18,50,52,54,102,158,159 causes a pathogenic shift in the oral microbiome with increased bone loss and inflammation in the mouth that ultimately give way to periodontal disease. 160 Suppressing the growth of opportunistic pathogens in the oral cavity is important in reducing the systemic dissemination of oral bacteria and crucial in the daily practice of good oral hygiene, especially in the management of diabetes.131,153 Oral photo-inactivation is a promising nonobtrusive and nonantibiotic method that may have advantage in this effort.144,149,161
While inconclusive and speculative, there are sporadic reports in the literature that imply the chronic oral infection of periodontitis may be a risk factor for Alzheimer's disease (AD) and Parkinson's disease (PD).162–164 Elevated antibodies to periodontal disease bacteria in subjects were observed years before the onset of symptoms in people suffering from AD,164,165 inferring that there was an increased translocation of bacteria and/or bacterial toxins from the mouth into the bloodstream. 162 An investigative study by Pereira et al. 163 identified differences in beta diversity (which quantifies community composition similarity between samples) and abundances of individual bacterial taxa in oral microbiota of PD patients and control subjects. However, an increase in the abundance of opportunistic oral pathogens was detected in males, both with and without PD. Nonetheless, the measured differences argue for further exploration of oral microbiota as a possible biomarker for PD. 163
Rheumatoid arthritis (RA) is an inflammatory autoimmune disease strongly associated with periodontal disease. 166 In a study by Zhang et al., 167 dysbiosis was evident in the gut and oral microbiomes of RA patients, and there was a concordance between the two microbiomes. Differences in the gut and/or oral microbiomes distinguished individuals with RA from healthy controls and were used to stratify individuals according to their response to therapy. 167 The altered composition of the gut or oral microbiomes in individuals with RA correlated with the prognosis and diagnosis of the disease. 167 Moreover, in two separate and unrelated double-blind randomized placebo-controlled clinical trials168,169 aimed to evaluate the benefit of oral probiotic supplements as an adjunct microbial therapeutic intervention, the RA patients who received daily capsules of the probiotic Lactobacillus casei 01 over a 2-month period had statistically significant improvements in their disease activity and inflammatory status compared with controls.166,168,169
Concluding Remarks
Obesity is an expanding healthcare issue worldwide170,171 and is a leading risk factor to a plethora of chronic conditions and diseases associated with dysbiosis in the oral and gut microbiomes—cardiovascular, cancer, diabetes, periodontitis, and RA are principal examples.18,50,59,172 Although the science exposing how the human microbiome influences the development and maintenance of the human body is still in the embryonic stage, the existing data show unequivocally that microbiota and our wellbeing are intimately linked. As noted in this review, the gut microbiome is the preeminent microbial organ of study for association, diagnosis, prognosis, and treatment of disease. Sampling the gut microbiota requires intervention for direct access. The oral cavity microbiome is proving to be a relevant surrogate representation of gut microbiota. The mouth is a psychologically more palatable and more easily accessed body site for microbial sampling by the patient as well as by the healthcare professional. With the ever increasing pressure to lower healthcare costs, prevention of disease has the greatest impact. Saliva and mucosal swabbing, including sampling of dental biofilms, could be made part of the routine dental exam. This scenario is likely to become common practice in preventive medicine, if not more so than giving a blood-sample. 173 Furthermore, capitalizing on the growing insights in this field, both new therapies and novel ways to make old therapies more effective are likely to emerge. The human microbiome may even find itself at the very center of the future of medicine—precision, personalized, and ever safer and more efficacious. 4 The food industry is already shifting toward developing microbiota-directed foods 174 and the U.S. Food and Drug Administration is considering classifying these altered foods as medical foods that may need to be regulated.174,175
In closing, we note that the cosmetic industry has begun to explore the relationship between the human microbiome and healthy skin to help correct skin microbe imbalances that are believed to play an underlying role in skin conditions such as acne and eczema as well as more minor maladies such as dryness and wrinkles. 23 Moreover, diabetic retinopathy, age-related macular degeneration, glaucoma, and cataracts are eye diseases that cause visual impairment and ultimately blindness, affecting millions of people worldwide. 176 The eye is an immunologically privileged site, and dysregulation of the endogenous microbiota can have profound effects on host immune function. 177 The surface of the eye is believed to harbor its own unique and immunoprotective commensal ecosystem (ocular microbiome), and it has barely begun to be explored.178–180
Although the encompassing mechanisms and pathways are not fully recognized or elucidated, and there is much work yet to be done as we apply our growing understanding of the human microbiome, microbiome medicine (the potential of the microbiome in treatment and diagnosis) clearly has clinical implications that no longer can be ignored.17,181,182
Footnotes
Acknowledgments
The authors thank the MitoCure Foundation for their generous financial support, and Drs. Carl A. Pinkert (The University of Alabama, Tuscaloosa, AL), Michael H. Irwin (Auburn University, Auburn, AL), and Robert J. Zamboni (McGill University, Montreal, QC, Canada) for their invaluable advice and helpful discussions in the preparation of this article.
Authors' Contributions
All authors contributed to the writing of this article and agreed to its final content.
Author Disclosure Statement
K.S. owns shares in PhenoMatriX, Inc. No competing financial interests exist.
