Abstract
The inability of the avascular region of the meniscus to regenerate has led to the use of tissue engineering to treat meniscal injuries. The aim of this study was to evaluate the ability of fibrochondrocytes preseeded on PLDLA/PCL-T [poly(L-co-D,L-lactic acid)/poly(caprolactone-triol)] scaffolds to stimulate regeneration of the whole meniscus. Porous PLDLA/PCL-T (90/10) scaffolds were obtained by solvent casting and particulate leaching. Compressive modulus of 9.5±1.0 MPa and maximum stress of 4.7±0.9 MPa were evaluated. Fibrochondrocytes from rabbit menisci were isolated, seeded directly on the scaffolds, and cultured for 21 days. New Zealand rabbits underwent total meniscectomy, after which implants consisting of cell-free scaffolds or cell-seeded scaffolds were introduced into the medial knee meniscus; the negative control group consisted of rabbits that received no implant. Macroscopic and histological evaluations of the neomeniscus were performed 12 and 24 weeks after implantation. The polymer scaffold implants adapted well to surrounding tissues, without apparent rejection, infection, or chronic inflammatory response. Fibrocartilaginous tissue with mature collagen fibers was observed predominantly in implants with seeded scaffolds compared to cell-free implants after 24 weeks. Similar results were not observed in the control group. Articular cartilage was preserved in the polymeric implants and showed higher chondrocyte cell number than the control group. These findings show that the PLDLA/PCL-T 90/10 scaffold has potential for orthopedic applications since this material allowed the formation of fibrocartilaginous tissue, a structure of crucial importance for repairing injuries to joints, including replacement of the meniscus and the protection of articular cartilage from degeneration.
Introduction
Leisure activities, sports activities, and certain work conditions are frequently associated with accidental tissue injury. 1 Of particular concern are knee injuries that affect the meniscus of the joint. The knee menisci are semilunar-shaped fibrocartilagenous structures interposed between the femoral condyle and tibial plateau and are essential for proper performance of the knee joint. 2 The functions of the meniscus include body weight distribution, pressure resistance, shock absorption, the lubrication and adjustment to tibial surfaces, modulation of femoral condyle shape, and joint stabilization during flexion and extension. 3 These functions, which are essential for joint protection and the prevention of injuries and osteoarthritis, are guaranteed by the specific organization of the extracellular matrix cells of this tissue. 4
The susceptibility of this tissue to injury and its limited regenerative capacity have led to different strategies aimed at restoring meniscus function. 5 The use of natural autologous materials for this purpose has yielded unsatisfactory results because of unfavorable mechanical properties and the difficulty in obtaining these natural substitutes.6–8 With regard to the use of prostheses, there are still no artificial materials with mechanical properties similar to those of the original meniscus. 9 Although nonabsorbable synthetic materials allow cell invasion, collagen I and II deposition, and the formation of new tissue with fibrochondrocyte-like characteristics, 10 they are unable to confer long-term protection to articular cartilage after long periods. 11
Given these difficulties, the use of hydrolytically degradable polymers to regenerate the meniscus has been extensively studied.12–14 The biodegradability and bioreabsorption characteristics of poly(α-hydroxy acids) 15 make this polymer a promising option for tissue regeneration and have led to this compound's widespread use for biomedical purposes, particularly because of its biocompatibility. 16
The copolymer PLDLA [poly(L-co-D,L-lactic acid)] has similar mechanical properties to poly(lactic acid) without the long degradation time associated with this homopolymer due to the greater degradation of poly(D,L lactic acid). 17 The addition of low molecular weight molecules such as PCL-T [poly(caprolactone-triol)] to PLDLA yields a more hydrophilic polymer with greater chain mobility and results in characteristics that enhance interaction with cells and tissues. 18
Cell cultivation on polymer substrates and subsequent implantation can improve the healing process in cartilage injuries when efficient materials such as bioreabsorbable fiber polymers and other porous structures are used.19–23 However, the usefulness of coculture on PLDLA/PCL-T for meniscus regeneration following medial meniscectomy has not been investigated, and the ideal cell type for such use has not been determined. Autologous and allogeneic meniscus cells, articular chondrocytes, fibrochondrocytes, fibroblasts, and mesenchymal stem cells represent possible sources of cells for such regeneration. 24
The aim of this study was therefore to assess the usefulness of primary cultures of rabbit meniscus fibrochondrocytes grown on PLDLA/PCL-T (90/10) scaffolds for meniscus regeneration. Specifically, we examined the allogeneic cultivation of these cells and the influence of this material on tissue regeneration and its effects on degeneration of the articular cartilage of the medial femoral condyle in vivo.
Materials and Methods
Preparation of polymeric scaffolds
PLDLA (70:30) was synthesized in the Laboratory of Biomaterials (Pontifical Catholic University of Sao Paulo [PUC-SP]), MW 265.028 g/mol Poly(caprolactone triol, PCL-T®) was supplied by Solvay® (CAPA 3091), MW 900 g/mol.
Solutions of PLDLA/PCL-T (90/10, w/w) were prepared by diluting the polymer in chloroform (Merck®) to a final concentration of 10% (w/v) at 25°C. After complete polymer dissolution, 50% (w/v) sucrose (Synth®) was added and the granulometry was maintained at 250–500 μm. The solutions were poured into silicone molds of the same dimensions as the rabbit menisci. After solvent evaporation and removal of the sucrose in polyvinyl alcohol, the scaffolds were disinfected with 70% ethanol overnight and sterilized by UV radiation.
Compression tests
Compression tests were done on cylindrical PLDLA/PCL-T scaffolds (diameter of 5.0 mm; height of 6.0 mm) at 1 mm/min up to a strain level of 0.7 mm/mm (70%). All of the tests were done on three-dimensional scaffolds in a dry state using an INSTRON 5566 testing machine. The compressive modulus was calculated as the slope of the initial linear region of the stress–strain curve.
Isolation of rabbit meniscus fibrochondrocytes
Fibrochondrocytes were isolated from a pool of menisci (n=16) essentially as described by Figueiredo and Joazeiro. 25 Four male New Zealand white rabbits (∼90 days old) were sacrificed. The fibrocartilages were removed by sectioning the joint capsule and the medial and lateral menisci of both legs were collected and placed in Dulbecco's modified Eagle's medium (DMEM; Cultilab®) containing gentamicin (Sigma®, 50 mg/L) and amphotericin B (Sigma, 2.5 mg/L). In a sterile environment, the fibrocartilages were fragmented and subjected to enzymatic digestion (3 h at 37°C) in DMEM supplemented with 1 mg of type IA collagenase/mL (Sigma). The cell suspension was then centrifuged (216 g, three times, 5 min) and the pellet resuspended in DMEM supplemented with 10% fetal calf serum (FCS). Cell viability was assessed by the Trypan blue exclusion test. The fibrochondrocytes (∼106 cells/mL) were seeded directly onto the scaffolds in DMEM 10% FCS and incubated at 37°C in a humidified atmosphere containing 5% CO2. The cells were allowed to adhere and proliferate for 21 days.
Surgical technique and scaffold implantation
All of the procedures involving animals described in this study were approved by the Ethics Committee in Animal Research at the Universidade do Vale do Paraíba (UNIVAP; protocol no. UNIVAP A047/CEP/2009). Twenty-four New Zealand white rabbits (150 days old, both sexes) were used essentially as described by Cardoso et al. 14 The rabbits were anesthetized with ketamine hydrochloride (35 mg/kg, intramuscular [IM]) and xylazine hydrochloride (5 mg/kg, IM) and then positioned on an operating table in supine position.
A medial longitudinal parapatellar incision (∼5 cm long) was followed by dissection of the subcutaneous tissue, medial parapatellar capsulotomy, lateral dislocation of the knee extensor (quadriceps and patellar tendon), sectioning of the medial collateral ligament in the joint line, and careful in toto resection of the medial meniscus, without damaging the medial femoral condyle articular cartilage; this was followed by scaffold implantation (Fig. 1).

Surgical procedure for implanting cell-free scaffolds and scaffolds preseeded with fibrochondrocytes. The medial parapatellar approach was used for meniscectomy and implant insertion.
The implant was fixed with monofilament 5-0 nylon suture, with two stitches (one anterior and another peripherally) in the middle portion of the device. The suture involved the polymeric scaffold and the perimeniscal capsular tissues. After implantation, separate stitches with nylon suture 4-0 were used for the capsule and medial collateral ligament repair and continuous sutures for the skin. The postoperative bandage consisted of sterile gauze. The animals were placed in individual suspended cages immediately after surgery and received food and water ad libitum.
Groups
The rabbits underwent total meniscectomy in both knees joints, right leg and left leg, totaling two medial menisci per animal. Twelve and 24 weeks indicating the number of weeks between surgery and euthanasia. The rabbits were divided into three groups of four animals (n=8 medial menisci) each. In group A, rabbits received an allogeneic implant; i.e., a scaffold seeded with fibrochondrocytes obtained from other conspecific individuals. In group B, the rabbits received a cell-free polymeric implant (pure PLDLA/PCL-T scaffold). The third group was the negative controls, in which meniscectomy was done in both legs (right and left) via a medial parapatellar incision, without any subsequent implant (empty defect). With this it is possible to analyze the conditions of the femoral condyle without the presence of the meniscus as it occurs in menisectomia procedures.
For comparison with the treatments, a positive control group (three rabbits, n=6 condyles) with no surgical intervention or scaffold implant was used to obtain normal menisci and condyles for histological and histomorphometric analysis.
Tissue sampling and processing for histological analysis
Twelve and 24 weeks after surgery the “neomenisci” were removed via a medial parapatellar incision (device and surrounding tissue) and the respective medial femoral condyles of both knees were collected. The tissues were photographed and then immediately placed in Bouin and fixed for 24 h. The condyles were decalcified for 14 days in an EDTA decalcifying solution.
The samples were subsequently processed for histological analysis and embedded in paraffin or historesin. Five-micrometer-thick sections were cut on a microtome (Leica RM2245®) and stained with hematoxylin and eosin (HE), Masson's trichrome (MT), and Picrossirus red and were examined under polarized light (Eclipse E800 microscope, Nikon®). For tissue included in historesin, 2-μm-thick sections were stained with 0.1% toluidine blue (TB) in 1% borax.
Histomorphometric analysis of the condyles
Sections from condyles were examined and photographed (Eclipse E800 microscope, Nikon®), and the number of chondrocytes in the hyaline cartilage was quantified with NIS software from Elements Advanced Research. Five fields per sections were examined using a 40× objective (total area: 0.63 mm2) and eight slides were examined per treatment (total area, 25.20 mm2; n=40 per treatment). The results for the different groups were compared using ANOVA followed by the Tukey test, with p<0.01 indicating significance.
Results
In this study, we examined the tissue repair after total meniscectomy of the medial meniscus in rabbits treated with a combination of bioreabsorbable material and allogenic fibrochondrocytes.
The mechanical performance of the PLDLA/PCL-T scaffolds was assessed through compression tests. The stress–strain curves showed a linear region, which was well evident at low values of strain and thus highlighted an initial stiff mechanical response. This region was followed by a region with lower stiffness and finally another stiff portion of the stress–strain curve (Fig. 2A). Figure 2B shows the mechanical behavior up to a strain level of 0.06 mm/mm (6%).

These results were similar to those of flexible foams and rapid prototyped PCL scaffolds. 26 A compressive modulus of 9.5±1.0 MPa (mean value±standard deviation) was calculated as the slope of the linear region of the stress–strain curve. The behavior was initially linear up to a strain of 0.003 mm/mm (0.3%). A maximum stress of 4.7±0.9 MPa was also evaluated at a strain value of 0.7 mm/mm (70%).
We compared regeneration using implants of cell-free PLDLA/PCL-T scaffolds and of PLDLA/PCL-T scaffolds preseeded with fibrochondrocytes. The scaffold dimensions were unaltered for 21 days by culture with fibrochondrocytes. All of the treated rabbits survived until euthanasia and showed similar behavior (normal agility and movements) to that of nonoperated rabbits. There were no postsurgical complications.
Macroscopic evaluation showed that all rabbits had complete healing of the incision, with no external scar (Fig. 3A). There were no clinical differences between cell-free and cell-seeded implants.

Macroscopic appearance of the knee joint during the removal of implants after 24 weeks.
On withdrawal, the implanted scaffolds were found to be well adapted to the surrounding tissues, with no apparent rejection, infection, or chronic inflammatory response (Fig. 3B). In seven of eight control rabbits, the presence of fibrous tissue connecting the femoral condyle to the tibial plateau was observed (Fig. 3C). This tissue was also found inside the defect, although most of it was empty or partially filled with adipose tissue.
After 12 and 24 weeks, the neotissue that formed around the polymer scaffold implants retained its biological features, regardless of whether the scaffolds had been seeded with fibrochondrocytes or not. Highlighting the results after 24 weeks, neomenisci formed from the seeded PLDLA/PCL-T scaffold showed anatomical features similar to those of normal (biological) menisci (Fig. 3B). This was not observed in control rabbits since the newly formed tissue was fixed to the tibial plateau in the posterior region and did not fill the entire area formerly occupied by the meniscus.
Morphology of normal menisci and condyles
Figure 4 shows the histomorphological characteristics of the normal medial meniscus and condyle of rabbits. The outer zone of the meniscus and the horns (tips) consisted mainly of thin circumferentially oriented collagen fibers and also some radially oriented fibers, both with only a few elongated cells similar to those of fibrous tissue (Fig. 4A). More internally, corresponding to the central portion of the meniscus, there were numerous fibrochondrocytes with a round morphology, as well as axial isogenic groups permeated by a collagen matrix usually with parallel lines (Fig. 4B). These features are characteristic of fibrous cartilage (fibrocartilage), which has a thicker, more abundant matrix that is richer in collagen type I compared to hyaline cartilage.

Twelve weeks after implantation. Scale bar=100 μm unless otherwise indicated.
The term fibrochondrocytes was introduced in 1985 to describe the peculiar characteristics of this population of cells in joint tissue. 27 The fibrochondrocytes inside the meniscus are round or oval and are located in the avascular area; these cells are strongly associated with the matrix and an intense presence of pericellular proteoglycans. Fibroblasts are located in the peripheral region of the meniscus (vascular portion). 28 A third type of cell in the meniscus consists of slightly spindle-shaped cells referred to as “cells of the superficial zone of the meniscus”. 29 These cells have no cytoplasmic extensions. 29
The biological knee joint, i.e., one with a normal natural meniscus and no surgical intervention, served as a positive control for the femoral condyle. Comparison between this joint and the operated joints makes it possible to determine the morphological changes in response to the polymeric material with and without associated cells.
Large quantities of well-organized hyaline cartilage populated by chondrocytes were observed in all areas of the joint (Fig. 4C). In addition, cell morphology and density, collagen fiber concentration, diameter and orientation, water concentration, and the presence of glycosaminoglycans vary with the depth of the joint layer. Based on variations in these characteristics, articular cartilage can be divided into superficial, middle, deep, and calcified cartilage zones. 30
The complex organization of each of these zones and the interaction between extracellular matrix components and the solid and liquid components of articular cartilage are directly related to the biomechanical function of the joint. 31
Twelve weeks after implantation
Figure 4D–4F shows photomicrographs of knee joints after the implantation of cell-free PLDLA/PCL-T scaffolds. In all cases there was a foreign body granulomatous reaction that consisted of giant and mononuclear cells along with polymer fragments, indicating that the material had not yet been completely degraded (Fig. 4D). This reaction was also observed around the suture site. Blood vessels and adipose tissue were also detected. The presence of blood vessels indicating good irrigation in the newly formed conjunctive tissue was an important feature for the inflammatory response, the migration of mesenchymal cells, nutrition, and consequent tissue regeneration. The presence of fibrocartilage-like tissue was also noted (Fig. 4E). Areas with this type of tissue showed no vascularization since a low level of oxygen is a key factor for fibrochondrocyte differentiation. 32 Staining with MT revealed dense collagen arranged in fibers (data not shown). Histological analysis of the condyle showed an abundance of chondrocyte-like cells and early disruption of the upper superficial layer (Fig. 4F).
In cell-seeded implants, a fibrocartilage-like tissue resembling that of a normal meniscus was observed (Fig. 4G); this tissue contained more fibrochondrocyte-like cells than did cell-free implants. Likewise, there was evidence of giant cell reactions in response to a foreign body. The arrangement of cells in line to resemble isomorphic groups (Fig. 4H) suggested recent fibrocartilage formation. Metachromasia was observed in images of TB-stained sections obtained from tissue embedded in historesin (data not shown). The change in dye color from blue to pink reflected the presence of sulfated glycosaminoglycans, a feature of fibrocartilage. According to Angele et al. 33 metachromasia in the extracellular matrix is most pronounced between the anterior horn and the pars intermedia of the meniscus, which contains mainly type II collagen and glycosaminoglycans, and distinguishes this region from the outer zone and posterior region. Histological examination of the condyles revealed an extracellular matrix containing embedded chondrocytes and no signs of cell disruption (Fig. 4I).
In the control group, adipose tissue and numerous blood capillaries were observed within the newly formed tissue (Fig. 4K). Small central areas of fibrocartilage-like tissue with few cells embedded in the matrix were also observed (Fig. 4J); there was no foreign inflammatory reaction since these control joints had received no implants. Condyle histological examination revealed a less organized extracellular matrix and cell disruption, with chondrocytes being present in only a few of the upper (outer) layers (Fig. 4L). The onset of cartilage loss and morphological alterations in the matrix were also observed.
Twenty-four weeks after implantation
After 24 weeks, joints that received cell-free implants contained fibrocartilage-like tissue with disorganized fibrochondrocytes-like cells and irregularly arranged collagen fibers. The synovium had a delicate, vascular appearance and was easily recognized. There were peripheral blood capillaries, a small amount of hyaline cartilage with a basophilic stroma and fibrochondrocytes that were either solitary or arranged in isogenous groups of two cells (Fig. 5D); metachromasia was also observed (Fig. 5E), as were foreign body granulomatous reactions and peripherally located adipocytes. The condyles contained numerous chondrocytes, although in some regions it can be seen that the extracellular matrix has small areas of the joint surface irregularities (Fig. 5F).
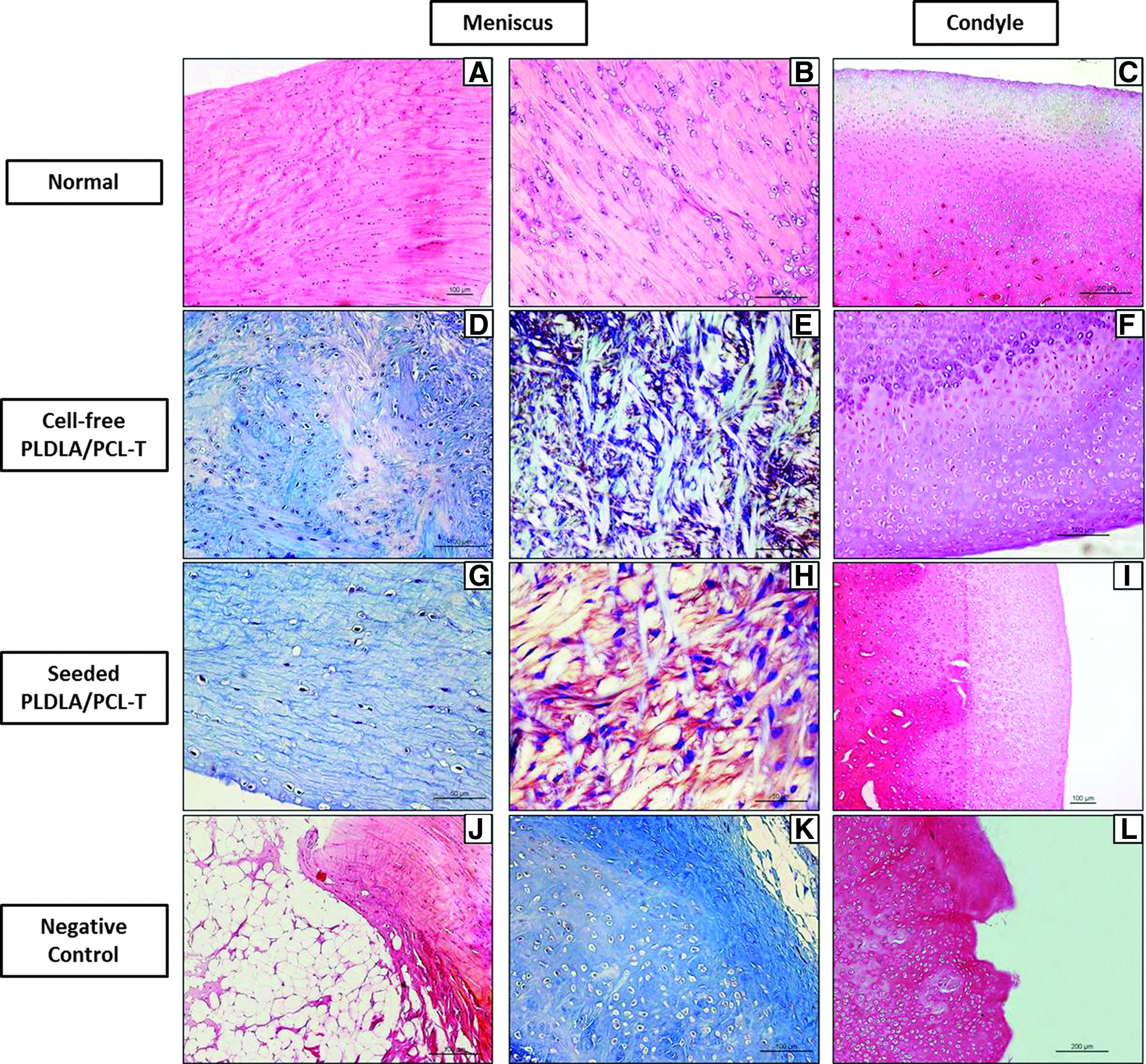
Twenty-four weeks after implantation. Scale bar=100 μm unless otherwise indicated.
In joints that received preseeded implants, the fibrocartilage was mature and organized, which suggested recuperation of the original meniscus morphology, with type I collagen fibers arranged in parallel and fibrochondrocytes immersed in the matrix (Fig. 5G). In three of five cases, small foreign body granulomas were seen in contiguity with the normal lateral synovial membrane in peripheral areas. Metachromasia was present in all animals examined (Fig. 5H). The condyles contained chondrocytes and the extracellular matrix was organized and evenly distributed in all layers (Fig. 5I).
Control rabbits showed the presence of fat and fibrosis in small fibrocartilage-like areas at the periphery (Fig. 5J), as well as the formation of central hyaline cartilage during wound healing (Fig. 5K). The control condyle contained chondrocytes irregularly distributed in the matrix with obvious signs of loss and matrix degeneration (Fig. 5L) and in some areas the presence of fibrous tissue along the upper were also observed.
Histomorphometry
Figure 6 shows the average number of chondrocytes per field in each of the experimental groups studied. Twelve and 24 weeks after the implant, all groups showed significantly more cells in the extracellular than the negative control (p<0.01). There was no significant difference between cell-free and cell-seeded scaffolds, and both of these were similar to the normal condyle (positive control; p>0.05).
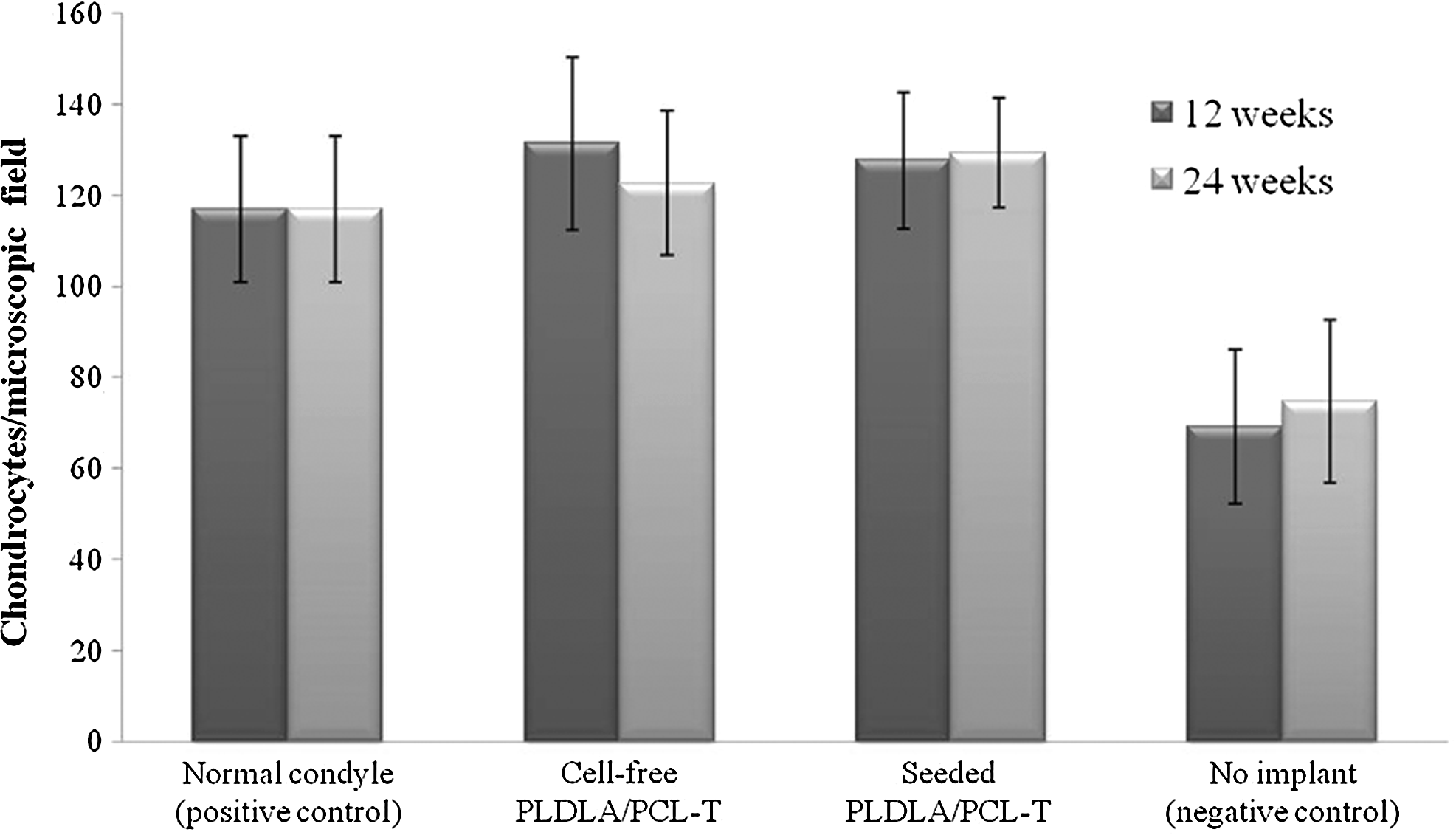
The average number of chondrocytes per microscopic field in each of the groups studied. The columns represent the mean±SD. All groups showed significantly more cells in the extracellular than the negative control (p<0.01). Assessment data showed negligible joint degeneration in the positive control (normal condyle). Rabbits treated with cell-free and cell-seeded scaffold implantation achieved similar results to the normal condyle group (p>0.05). No significant difference between cell-free and cell-seeded scaffolds was found (p>0.05).
Discussion
The current challenge for tissue engineering is to develop devices capable of interacting with body tissues to stimulate regeneration. Even though advances in the development of novel artificial matrices have been made, attempts to engineer cartilaginous tissues, such as meniscus and articular cartilage, have led to tissue with mechanical properties and biological/biochemical features different from to those of the native tissue. 34
The compressive mechanical properties of the PLDLA/PCL-T scaffolds were found to be better than those of the polyglycolic acid (PGA) scaffolds mechanically stabilized by bonding adjacent PGA fibers with PLGA that were proposed for meniscus regeneration. 35 Furthermore, PLDLA/PCL-T scaffolds have a compressive modulus (9.5±1.0 MPa) that falls in the range of those reported for macro/microporous silk fibroin scaffolds that were proposed to be suitable for articular cartilage and meniscus tissue engineering applications. Specifically, the dry state compressive modulus of the above mentioned scaffolds increased from 0.81±0.29 to 15.14±1.70 MPa, depending upon the silk fibroin concentration. 36
Surgical intervention always results in mechanical trauma. The tissue response to such aggression begins with inflammation and proceeds through the healing steps. In the presence of an implant, there may also be a “foreign body reaction” in response to the recognition of foreign material in the host. 37 With regard to this study, although the foreign body granulomatous response is commonly observed with implants, its occurrence has no major significance on the neoformation of fibrocartilage. Many studies have shown that bioreabsorbable polymers based on poly (α-hydroxy acids), which are widely used for tissue regeneration, produce similar foreign body inflammatory reactions that usually disappear after complete polymer degradation12–14,18,38–39 as occurred in this case.
When amenable, the regeneration of the meniscus is initially characterized by the formation of vascularized fibrous tissue that differentiates into phenotypically fibrocartilagenous tissue after a few months. 40
The results described here regarding the control defect agreed with the findings of others showing that rabbit menisci have no intrinsic recovery response and are only capable of forming fibrous cicatrization tissue.33,41–43 Likewise, when injured in the inner and middle portions, the human meniscus does not undergo spontaneous regeneration and there are currently no surgical methods to promote this. 12 This limitation is also related to the low vascularization of this tissue.
The presence of hyaline cartilage in the inner portion of newly formed tissue of the control defect was also observed in rabbits by Kang et al. 35 Their results indicated a greater amount of type II collagen in the inner portion of the meniscus (a feature of hyaline cartilage), while the outer zone of the new tissue was fibrous and consisted almost entirely of type I collagen.
The limited capacity of meniscal tissue for regeneration and the fact that fibrocartilage injuries usually result in slow, difficult cicatrization make tissue-engineering techniques a promising alternative for repairing injured menisci in order to preserve tissue functions and prevent degenerative joint diseases. 44 The construction and maintenance of an appropriate interface for the formation of fibrocartilaginous tissue is therefore critical for the successful use of implants in tissue engineering, particularly since this approach involves the proliferation of viable cells on biomaterial substrates.
Scaffold porosity is an important feature that can facilitate the formation of meniscus fibrocartilage-like tissue.45,46 Furthermore, the time required for fibrocartilage formation should be considered when selecting the appropriate material since scaffolds are incubated with cells in liquid culture medium prior to use and degradation may therefore begin before implantation. Elema et al. 47 reported that fibrocartilaginous formation in humans requires approximately 20 weeks, a rather long period. Recently, preseeded scaffolds have been used to enhance healing during meniscus regeneration.19,21–23,33,48
Weinand et al. 22 examined the use of autologous and allogeneic chondrocytes, cultured with commercial bioreabsorbable PLGA scaffolds (Vicryl®, Ethicon Inc.) and later used as implants. Their results indicated that preseeding the scaffolds promoted lesion regeneration in an avascular meniscal region in pigs. Fluorescent staining of these precultured cells demonstrated their presence in neotissue that integrated with the native meniscus after 12 weeks. There was no lymphocytic infiltration (which would have been indicative of cellular rejection) and no significant difference in the repair obtained with autologous and allogeneic cultures.
Kang et al. 35 have also evaluated meniscus regeneration in rabbit meniscus with total medial meniscectomy. They used a porous PLGA structure reinforced with PGA fibers and preseeded with meniscus cells. Their results indicated the formation of fibrocartilage-like tissue with similar histological features to those of normal meniscus. However, histological analysis of the adjacent tibial articular cartilage showed that the neomeniscus did not prevent the degeneration of articular cartilage after 36 weeks.
Regarding the cell type selected as cell source in this study Figueiredo 49 demonstrated the feasibility of culturing fibrochondrocytes. These cells can be reproducibly isolated from fibrocartilage and maintain their phenotypic characteristics (cell properties and extracellular matrix synthesis) in culture. Araujo 50 showed that fibrocartilage cells cultured in vitro do not lose their intrinsic ability to initiate a repair response when directly seeded onto substrates. Moreover, we have previously shown that a PLDLA/PCL-T 90/10 scaffold provides a suitable substrate for the growth of rabbit fibrocartilaginous cells in vitro; the cells proliferated and infiltrated the scaffold, creating a three-dimensional arrangement. 51
The results described here for 12 weeks after implantation showed that, regardless of whether they had been preseeded with cells, the PLDLA/PCL-T scaffolds produced a much better response than the control group (empty defect). At this time interval, there was no significant qualitative difference in the production of fibrocartilage-like tissue by scaffolds with or without cells. Twenty-four weeks after implantation the “neomeniscus” was more organized than the fibrocartilaginous tissue seen after 12 weeks. Mature fibrocartilage with organized fibers was seen after 24 weeks, primarily with implants precultured with allogeneic fibrochondrocytes. This was confirmed by staining with HE and MT, which showed type I collagen fibers arranged circumferentially in the extracellular matrix of the neomenisci, as also occurs in the normal meniscus. The presence of sulfated glycosaminoglycans in neotissue was also an important parameter for assessing regeneration.
In this study, there was no direct immune response during the regeneration of meniscus tissue with allogeneic cells when compared to cell-free implants. This finding agrees with studies that have reported no immune rejection with allogeneic cells22,23,35 or with cryopreserved menisci for transplants. 52 The decision to use allogeneic cells in this study reflected the ease with which allogeneic meniscal fibrochondrocytes can be obtained since these cells are more accessible than autologous cells for transplants. In addition, performing a biopsy to obtain cells would generate a cicatrization response that would reduce tissue regeneration after the surgery required for scaffold implantation. A biopsy would also yield a lower number of cells and this would in turn require weeks of culture to allow sufficient expansion of the cell population for later seeding. 23
Another important aspect that has to be considered is whether or not the meniscus engineered construct presents any consequence within the articular cartilage. In knees submitted to meniscectomy the contact area can be reduced by approximately 50%. 53 This loss of area increases the load per unit area in articular cartilage and results in damage and cartilage degeneration, causing arthritis, osteoarthritis, and pain. 54 The degree of osteoarthritis after meniscectomy is directly proportional to the amount of meniscus removed. 55 Truly, the main aim of using polymeric scaffolds for tissue regeneration is to replace the lost or damaged meniscus, thereby avoiding severe medium and long-term injury to the articular cartilage.
Histomorphometric analysis indicated that the knee joint cartilage was preserved by the polymeric implants. This protection was reflected in the higher percentage of chondrocytes in rabbits treated with polymeric scaffolds and in the positive controls when compared with the negative controls, which showed cellular disarray (indicative of degenerative osteoarthritis) after 12 and 24 weeks.
Most recently, similar results were found by Kon et al. 56 showing that osteoarthritic changes were significantly less in the cell-seeded group than in the meniscectomy group, even though results were not significantly superior to those of the cell-free scaffold. Additionally the study confirms the role of cells for increasing the tissue regeneration capacity, providing a better fibrocartilaginous tissue formation. These results supported by the results presented in this paper and the literature suggest the potential of bioresorbable scaffolds and tissue engineering approach for total meniscal substitution.
Finally, although the scaffolds and protocols used here resulted in quicker fibrocartilage formation compared to previous studies, these findings need to be confirmed by immunological analyses and longer post-implantation intervals. Despite the limitations of this study, the results described here demonstrate that regeneration of the meniscus, an important fibrocartilaginous structure, can be achieved using bioreabsorbable polymer scaffolds and allogeneic cells.
In conclusion, the PLDLA/PCL-T 90/10 polymeric scaffold has potential for biomedical applications since this material allowed the formation of fibrocartilaginous tissue, a structure of crucial importance for repairing injuries to joints, including replacement of the meniscus and the protection of articular cartilage from degeneration.
Footnotes
Acknowledgments
This work was supported by Fundação de Amparo à Pesquisa do Estado de São Paulo (FAPESP, grant no. 2008/01963-9). The authors thank the Institutional Program for Scientific Scholarship Council Research and Education PUC-SP (PIBIC-CEPE/CNPq) for scholarships. The authors would like to thank the Institute of Composite and Biomedical Materials, National Research Council of Italy for the opportunity and collaboration.
Author Disclosure Statement
No competing financial interests exist.
