Abstract
Reactive oxygen species (ROS) are key signaling molecules that play an important role in the progression of inflammatory disorders. An enhanced ROS generation by polymorphonuclear neutrophils (PMNs) at the site of inflammation causes endothelial dysfunction and tissue injury. The vascular endothelium plays an important role in passage of macromolecules and inflammatory cells from the blood to tissue. Under the inflammatory conditions, oxidative stress produced by PMNs leads to the opening of inter-endothelial junctions and promotes the migration of inflammatory cells across the endothelial barrier. The migrated inflammatory cells not only help in the clearance of pathogens and foreign particles but also lead to tissue injury. The current review compiles the past and current research in the area of inflammation with particular emphasis on oxidative stress-mediated signaling mechanisms that are involved in inflammation and tissue injury. Antioxid. Redox Signal. 20, 1126–1167.
I. Introduction
I
Within a short period of activation of the innate immune system, the acute inflammatory response is started by immune cells enabling secretion of various cytokines and chemokines in order to recruit immune cells to the site of infection. Neutrophils are the first to adhere to endothelial cells, and they begin to migrate across the vascular wall at the site of infection to engulf the invading pathogens and also secrete vasoactive and pro-inflammatory mediators (222). Most of the early vascular changes observed in acute inflammation are due to inflammatory mediators that are released by inflammatory cells at the site of injury (65). These mediators, including histamine, platelet-activating factors (PAFs), bradykinin, and thrombin, increases vascular permeability followed by fluid accumulation (edema) and leukocyte extravasation. Acute inflammation can be caused by bacterial or viral infection (e.g., as in acute respiratory distress syndrome (ARDS), tissue necrosis (e.g., as in acute myocardial infarction), trauma, radiation, burns, or by any foreign body present in tissue. However, if the innate immune system exceeds its capacity or its defensive function becomes limited, it engages the adaptive immune system, activating specific T and B cells for pathogen clearance (65). If this process is prolonged or inefficient, it progresses to the chronic state of inflammation that is associated with many diseases such as of the heart and rheumatoid arthritis. Chronic inflammation is also associated with persistent bacterial infections such as tuberculosis, ARDS, autoimmune diseases, inflammatory bowel disease, atherosclerosis, and neurodegenerative and metabolic hormonal disorders.
Production of reactive oxygen species (ROS) is central to the progression of many inflammatory diseases. The ROS are produced by cells that are involved in the host-defense response, such as polymorphonuclear neutrophils (PMNs) and promote endothelial dysfunction by oxidation of crucial cellular signaling proteins such as tyrosine phosphatases. The ROS act as both a signaling molecule and a mediator of inflammation. The ROS such as superoxide can rapidly combine with NO at a diffusion limited rate (k=5 to 10×109 M −1s−1) to form reactive nitrogen species (RNS), such as peroxynitrite, and is three to four times faster than the dismutation of superoxide by the superoxide dismutase (SOD) (33). The RNS, in turn, induces nitrosative stress, which adds to the pro-inflammatory burden of ROS. While attempting to be inclusive, this review cannot deal with the role of RNS, and, thus, the reader is advised to refer to the excellent reviews written in this area (401). The major focus of this review is on the ROS-dependent mechanisms of inflammation with a bias toward endothelial mechanisms, and our view that the endothelial cell for good or ill is a dominant orchestrator of inflammation.
II. Sources of ROS and Their Regulation in Inflammation
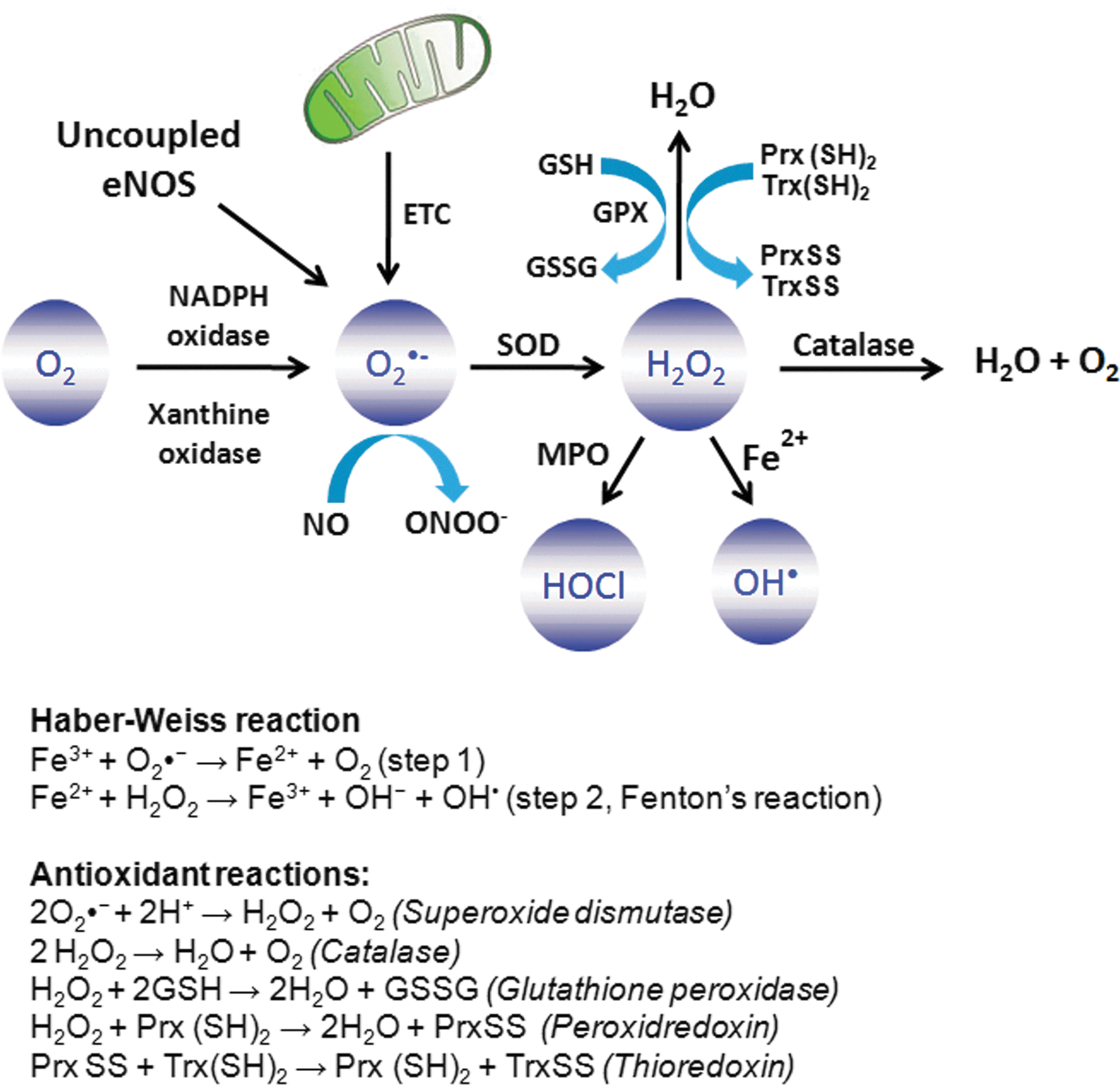
ROS are classically defined as partially reduced metabolites of oxygen that possess strong oxidizing capabilities. They are deleterious to cells at high concentrations but at low concentrations (exact concentrations still remaining to be defined), they serve complex signaling functions. They are injurious, because they oxidize protein and lipid cellular constituents and damage the DNA. At “physiological concentrations,” ROS function as signaling molecules that regulate cell growth, the adhesion of cells toward other cells, differentiation, senescence, and apoptosis (102, 413). The concept of chronic or prolonged ROS production is considered central to the progression of inflammatory disease (155). What are the biologically relevant ROS? The widely studied and understood family members are the superoxide anion (O2
•
O2
•
The role of oxidants in inducing inflammation has been vigorously investigated in all manner of experimental models. The consensus is they are fundamentally involved, but how they contribute to the response and whether antioxidant therapy is a valid means of arresting inflammation in patients remains largely unresolved. Among the commonly used inflammatory mediators used to simulate inflammation are included cytokines (e.g., TNF-α), the stress of hyperoxia, ischemia-reperfusion injury, bacterial toxins (LPS), and mediators that ligate cell surface receptors (PAF, thrombin, histamine, VEGF, and bradykinins). These and other mediators except LPS induce only a subset of changes that are associated with full-blown inflammation.
A. NADPH oxidase-derived ROS in inflammation
NADPH oxidases were first identified in phagocytes for their role in inducing respiratory burst and bacterial killing (19, 376). So far, there are seven described homologs of NADPH oxidase (NOX1–NOX5 and Duox1 and 2) (Fig. 2). NADPH oxidase homologs differ in their structure, expression levels in different tissue, and their activation mechanisms (227, 233). The catalytic core of classical phagocytic NADPH oxidase 2 (NOX2) consists of two membrane-bound subunits, gp91phox and p22phox, which form the flavocytochrome b558 complex. The gp91phox subunit consists of six transmembrane domains, and its C-terminal region contains the binding sites for flavin-adenine dinucleotide (FAD) and electron donor NADPH. All NADPH oxidases, with the exception of NOX5 and Duox1 and 2, share a similar topological structure of the catalytic core of gp91phox. NOX5 carries an additional intracellular N-terminal calcium-binding domain. However, Duox1 and 2, in addition to the catalytic NOX5 structure, carry another N-terminus transmembrane α-helix, which possesses a peroxidase homology domain (Fig. 2) (233). NOX1, NOX2, and NOX4 are the major isoforms of NADPH oxidase that are expressed in the vascular system, and each is strongly implicated in inflammation-induced vascular injury (340).
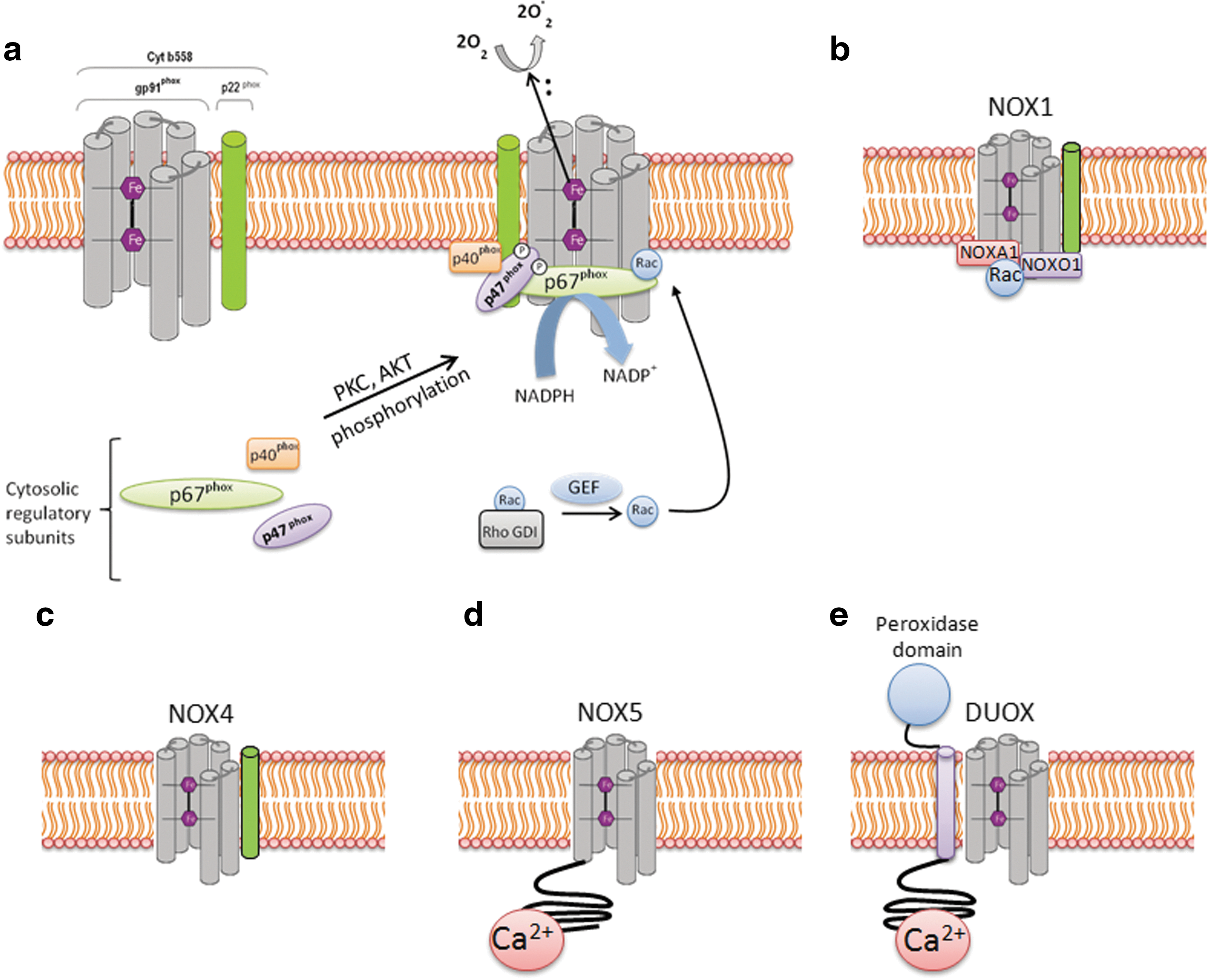
O2
•
p47phox has been documented to be important in the progression of atherosclerosis and pulmonary fibrosis (26, 268). p47phox null mice were protected against formation of atherosclerotic lesions and development of pulmonary fibrosis (26, 268). Mice deficient in p47phox subunit or NOX2 were also protected against TNF-α-induced lung inflammation or sepsis-induced lung microvascular injury (126 469). However, there are also contradictory findings. Zhang et al. (468) reported no difference in LPS-induced acute inflammatory responses in NOX2−/− and p47phox−/− mice compared with the control mice. On the contrary, they observed enhanced gene expression of inflammatory mediators and increased neutrophil recruitment to the lung and heart, resulting in impaired resolution. This discrepancy in the results was attributed to LPS-mediated ROS generation via NADPH oxidases, which also instead contributed to the resolution of inflammatory response (468). The NOX2 expressed in immune cells such as T cells has also been implicated in angiotensin II (Ang II)-induced hypertension (158). Guzik et al. have shown on the basis of adoptive transfer experiments that T cells lacking the AT1-receptor or p47phox subunit resulted in decreased aortic O2 •− production and blunted Ang II-dependent hypertension (158). Moreover, Ang II infusion induced the expression of NOX2, p47phox, and p22phox in the T cells and stimulated superoxide production (158). In a similar study, Wenzel et al. have shown that Ang II infusion stimulated the accumulation of both macrophages and neutrophils in the mouse aorta (450). The depletion of myelomonocytic cells by inducible diphtheria toxin receptor (LysMiDTR mice) attenuated Ang II-induced blood pressure increase and reduced vascular O2 •− formation (450). Moreover, adoptive transfer of wild-type monocytes into depleted LysMiDTR mice re-established the Ang II-induced oxidative stress, and arterial hypertension, whereas adoptive transfer of neutrophils or monocytes lacking NOX2 did not (129). The NOX2 activity has also been implicated in cardiac inflammation and fibrosis. The mice deficient in NOX2 were protected against cardiac remodeling and contractile dysfunction induced by coronary artery ligation (252), aortic banding (153), Ang II infusion (36), or Doxorubicin treatment (471) compared with the wild-type mice. Moreover, in aortic-banding model, the treatment of wild-type mice with N-acetylcysteine resulted in recovery of contractile dysfunction (153). Altogether, these findings highlight the important role of NOX2-derived ROS in cardiac remodeling, which could be prevented by antioxidant treatment.
Rac1 is another important cytosolic subunit that is required for activation of NOX2. Rac1 activation is accompanied by the replacement of GDP residue with GTP by guanine nucleotide exchange factor (GEF), resulting in conformational change of Rac protein by relieving inhibition from Rho GDP-dissociation inhibitor. Rac1 activation promotes binding of p67phox with cyt b558 complex (79). Rac1 activation is induced by a variety of inflammatory stimuli such as TNF-α (453), interleukin-1β (IL-1β), thrombin, VEGF (299), histamine (321), Ang II (384), ischemia-reperfusion injury (216), and shear stress (463). The expression of the active Rac1 mutant V12Rac1 resulted in enhanced ROS production and loss of endothelial barrier integrity (427). Rac1 activation has also been demonstrated in trafficking of inflammatory cells across the endothelial barrier (428). Cross-linking of vascular cell adhesion molecule-1 (VCAM-1) on endothelial cell surface induced Rac1 activation and ROS generation, and resulted in loss of endothelial cell–cell adhesion and transendothelial leukocyte migration (428).
In contrast to NOX2, NOX1 is activated by homologues of p47phox and p67phox, known as NOXO1 (NOX organizer 1) and NOXA1 proteins (NOX activator 1), respectively (23). NOXO1 does not contain an autoinhibitory region and is constitutively active in the cells (410). Co-expression of NOXO1 and NOXA1 with NOX1 in HEK 293 cells was sufficient to generate ROS independent of any stimulus (23, 410). High expression of NOX1 was observed in colon epithelium, and LPS induced the expression of NOX1 and NOXO1 in gastric mucosal cells (208, 410). NOX1 activation was dependent on Rac1 activation, and Rac inhibitor LY-294002 (PI3-K inhibitor) blocked O2 − • generation (208). Mice deficient in NOX1 were protected against hyperoxia-induced acute lung injury (54). Surprisingly, NOX2−/− mice were not protected against hyperoxia-induced lung injury in the same study (54), suggesting that hyperoxia may induce lung injury secondary to NOX1 activation, or NOX1 may compensate for the loss of NOX2. In addition, NOX1-deficient mice were less susceptible to Ang II-induced aortic dissection and aneurysm formation (131). NOX1 was also important in angiogenesis and tumor formation. Mice deficient in NOX1 exhibited impaired angiogenesis and tumor growth (129). Activity of NOX1 was increased in endothelial cells on angiogenic stimulation. However, angiogenesis remained unaffected in NOX2 or NOX4 knockout mice in this study.
NOX4 was first characterized in the kidney as an “oxygen sensor” regulating oxygen-dependent expression of erythropoietin and development of inflammatory processes in the kidney (132). NOX4 has also been termed renal NADPH oxidase (Renox). Activity of NOX4 is largely controlled by expression levels of NOX4 and is independent of the Rac activation or the presence of p47phox/p67phox or NOXO1/NOXA1 proteins (12, 132, 275). However, NOX4 activity required the presence of p22phox (275). The type of ROS generated by NOX4-expressing cells is primarily H2O2, whereas O2 •− was almost undetectable in these cells (383). Recently, another mechanism of NOX4 activation has been reported. Lyle et al. have shown that polymerase (DNA-directed) delta-interacting protein 2 (Poldip2) associates with p22phox to activate NOX4, which regulates cytoskeletal reorganization and cellular migration in an Rho A-dependent manner (257). NOX4 is the predominant homolog expressed in human lung microvascular and human pulmonary arterial endothelial cells compared with NOX1, NOX2, NOX3, or NOX5 (338). Inflammatory stimuli LPS, TNF α, hyperoxia, TGF-β, and hypoxia were demonstrated to enhance ROS generation via NOX4 (29, 191, 242, 295, 335, 338). The expression of intercellular adhesion molecule-1 (ICAM-1), IL-8, and MCP-1 in endothelial cells in response to LPS was demonstrated to be dependent on NOX4 activation (335). Treatment of endothelial cells with NOX4 siRNA decreased LPS induced migration and adhesion of monocytes by 36% and 52%, respectively (335). Increased NOX4 activity is also a reported risk factor in the progression of type-2 diabetic nephropathy, stroke, pulmonary fibrosis, and atherosclerotic lesions (11, 145, 219, 240, 331, 382). However, the contradictory reports in the literature suggest that NOX4 is a vascular protective enzyme rather than a destructive one (415). NOX4 overexpression in the endothelium was found to enhance vasodilation and reduced basal blood pressure, which was related to increased H2O2 production and reduced NO inactivation (415). Moreover, in tamoxifen-inducible NOX4 knockout mice, Ang II-mediated aortic inflammation, vascular remodeling, and endothelial dysfunction were exaggerated, which correlated to a decrease in endothelial nitric oxide synthase (eNOS) expression (415). In addition, NOX4 overexpression was found to increase eNOS protein and promote recovery of ischemic tissue by enhanced angiogenesis and aortic sprouting (415). It is not easy to reconcile all these contradictory reports, and the part of the reason behind these discrepancies may be related to the tissue-specific abundance of different NADPH oxidase homologs and differential regulation of NOX4 in different models.
The expression of NOX5 has been reported in human vascular endothelial cells and smooth muscle cells. NOX5 is not expressed in rodents. Four variants of NOX5 have been identified so far, including NOX5α, NOX5β, NOX5γ, and NOX5δ (34). ROS generation by NOX5 is induced by calcium binding on its N-terminal domain, which has four Ca2+-binding sites (referred to as EF hands). The binding of Ca2+ to NOX5 induced conformational change that enhances ROS generation by NOX5. Unlike other NOX homologs, O2 •− production by NOX5 does not require p22phox. NOX5 has been reported to be induced by thrombin (34), Ang II (300), and platelet-derived growth factor (197). An increased expression level of NOX5 has been implicated in the coronary artery disease patients, which correlates with the oxidative damage observed in atherosclerosis (157). NOX5 has also been reported to be essential for PDGF-stimulated proliferation of vascular smooth muscle cells and proliferation of endothelial cells and angiogenesis (34, 197). Thus, while NOX5 may be important, it is still relatively understudied.
B. Mitochondrial-derived ROS in inflammation
Mitochondria generate high-energy phosphate bonds of ATP by electrochemical proton gradient created by the transfer of electrons through a series of electron carriers embedded in the mitochondrial membrane. There are four electron transport carriers that are spatially organized in order of their increasing redox potential, complex I (NADH-ubiquinone oxidoreductase), complex II (succinate-ubiquinone oxidoreductase), complex III (ubiquinol-cytochrome c reductase), and complex IV (cytochrome c oxidase) (Fig. 3) (163). Transfer of electrons to molecular O2 is a tightly controlled process, and only 1%–2% of electrons that leaked out in this process react with O2, resulting in O2
•
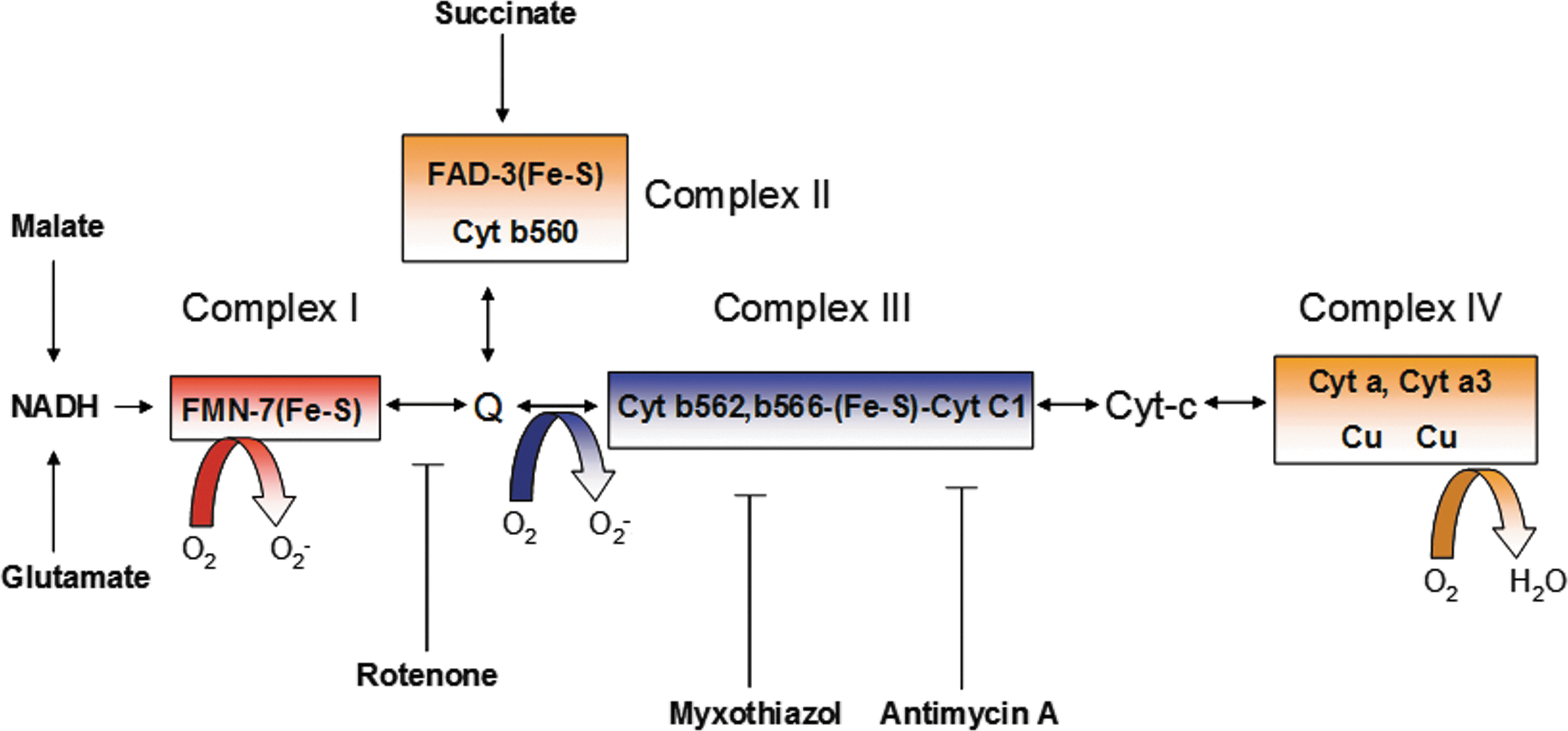
The genetic mutations in mitochondrial respiratory chain can result in a variety of neurological disorders, including Leigh's syndrome, leukodystrophy, paragangliomas, and pheochromocytomas (97). Mitochondrial-derived oxidative stress has also been implicated in chronic inflammation, cancer progression (206), diabetes mellitus (148, 152, 317 –319, 378), and atherosclerosis (21, 258). Mitochondrial-derived ROS (MtROS) also contributes to LPS-mediated production of pro-inflammatory cytokines IL-1β, IL-6, and TNF-α (48). Notably, MtROS have been implicated in ectodomain shedding of cytokine receptor TNF receptor–1 (TNFR1) in endothelial cells, which is important for regulation of inflammatory progression (364). TNF-α-converting enzyme, which mediates cleavage of TNFR1, is activated by ROS (440). Ectodomain shedding of cytokine receptors facilitates diffusion of soluble receptors into the extracellular space, which dampens the inflammatory response by binding and neutralizing the cytokine ligands. Missense mutations in the extracellular domain of the gene encoding TNFR1 lead to inheritable autosomal dominant disorder known as tumor necrosis factor receptor-associated periodic syndrome (TRAPS) (48). TRAPS is an auto-inflammatory disease that is associated with recurrent fevers, peritonitis, migratory rash, myalgia, and arthralgia. Monocytes and neutrophils isolated from TRAPS patients showed elevated baseline levels of mitochondrial ROS compared with healthy donors and also had constitutive and prolonged activation of JNK and p38 MAPK on LPS challenge (48). Consequently, these cells showed enhanced production of cytokines IL-6 and TNF-α on LPS challenge. Inhibition of mitochondrial ROS with MitoQ suppressed p38MAPK activation and production of IL-6 and TNF-α (48). Although the basis by which TNFR1 mutations leads to increased mitochondrial ROS is not clear, possible mechanisms include retention of the mutated protein in the endoplasmic reticulum, which can induce unfolded protein response, triggering calcium release from ER and depolarizing mitochondria by disruption of the mitochondrial ETC (467).
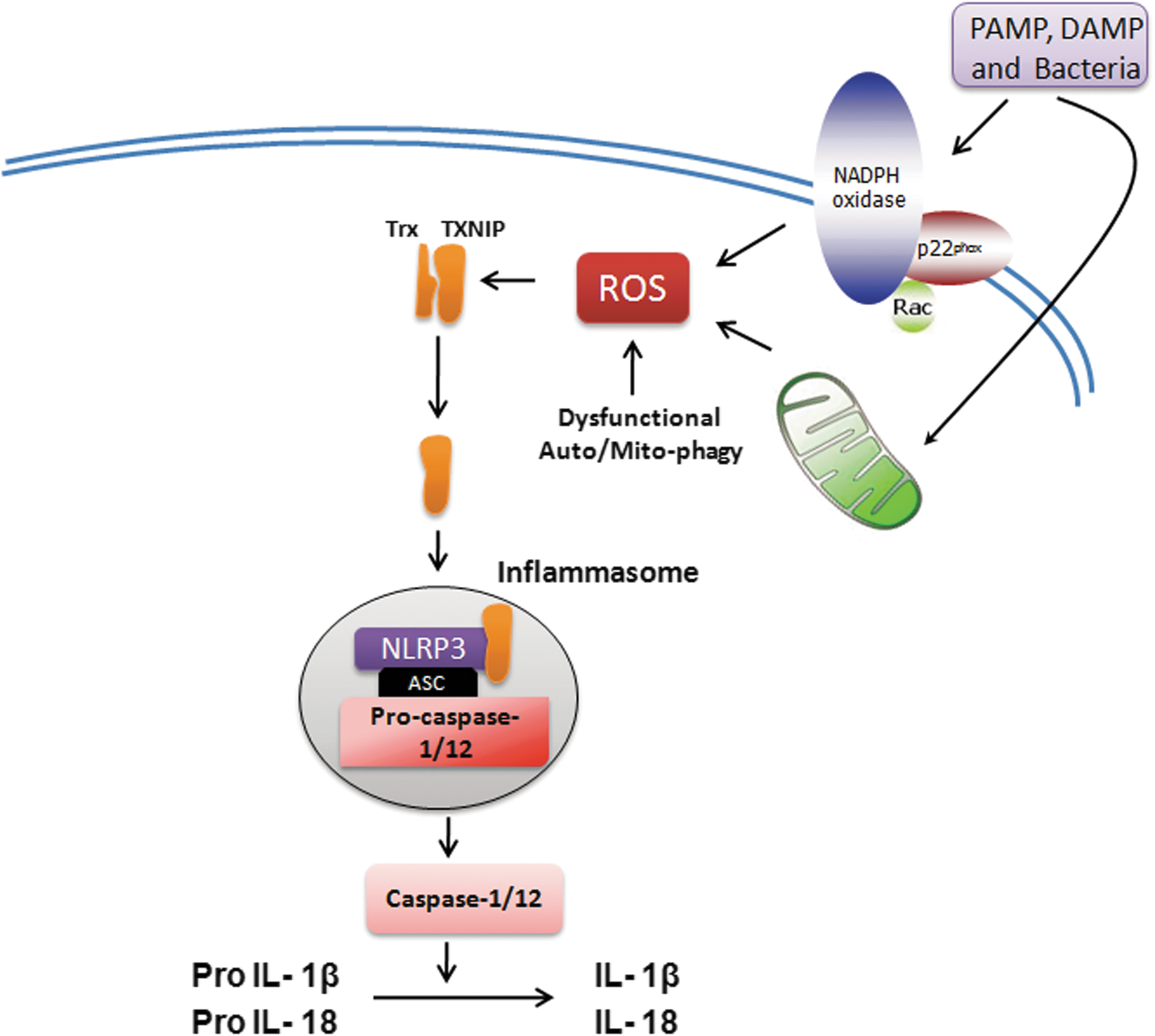
Another important role of MtROS has been recognized in the regulation of inflammasome, the high-molecular-weight complexes that activate inflammatory caspases (caspase-1 and -12) and cytokines (IL-1β and IL-18) in macrophages (274). Three different prototypes of inflammasomes have been recognized: NALP1, NALP3 (also known as NLRP3), and IPAF. NLRP3 inflammasome, the most well-characterized form, is redox sensitive (99, 379). The key components of NALP3 are NLRP3, apoptosis-associated speck-like protein (ASC), and caspase-1. NLRP3 is a cytoplasmic receptor that interacts with ASC and recruits procaspase-1 (379). The NLRP3 inflammasome has been shown to interact with redox-sensitive protein thioredoxin (Trx)-binding protein-2 (TBP-2, also known as vitamin D3 up-regulated protein 1 [VDUP1]). Increased intracellular ROS generation mediates dissociation of TBP-2 from Trx, enabling association with NLRP3 inflammasome and resulting in its activation (Fig. 4) (473). Mice deficient in NLRP3 or ASC on LPS treatment have reduced serum levels of IL-1β and IL-18 and are resistant to LPS-induced lethality (403). ASC-deficient mice were also protected against LPS challenge (403). On activation by ROS, NLRP3 recruited ASC and procaspase-1, which mediated proteolytic cleavage, leading to activation of caspase-1 and IL-1β and IL-18 (473). The MtROS is important in the activation of NLRP3 inflammasome. Inhibition of mitochondrial function by depleting VDAC with shRNA impaired the activation of NLRP3 and cleavage of IL-1β and caspase-1 (474). In addition to direct activation by ROS, the activity of NLRP3 inflammasome is negatively regulated by autophagy/mitophagy (310, 367). Autophagy/mitophagy indirectly regulates intracellular oxidative stress by clearance of dysfunctional mitochondria and damaged proteins (170). Macrophages isolated from mice deficient in the autophagy proteins LC3B and ATG16L1 have enhanced NLRP3 inflammasome activation and produced higher IL-1β and IL-18 on LPS challenge (310, 367). MtROS has also been implicated in increasing oxidative stress through cross-talk with nitric oxide synthases (NOSs) (293). Arginase II, which activates NOS, was shown to promote the macrophage inflammatory response that contributes to insulin resistance and atherogenesis (293).
Recent reports have highlighted an interesting concept of cross-talk between MtROS and NADPH oxidase, which can drive both feed-forward and feedback regulations of NADPH oxidases (73, 96). Ang II-stimulated mitochondrial H2O2 was blocked by NADPH oxidase inhibitor apocynin and protein kinase C inhibitor chelerythrine (96). Moreover, depletion of p22phox with siRNA also inhibited Ang II-mediated MtROS production (100). In contrast, ROS produced by the mitochondria on serum withdrawal has been shown to trigger NOX1 activation (96). Moreover, Ang II-mediated mitochondrial dysfunction has been shown to increase the expression and activity of NOX1 and NOX4 in vascular smooth muscle cells (96). Block et al. have reported the existence of NOX4 in the mitochondria of rat kidney cortex that was induced in rat model of diabetes (42). In an independent study, Ago et al. have similarly reported the localization of NOX4 in cardiac mitochondria with F1F0-ATP synthase as well as the p22phox subunit of NADPH oxidases (3). However, no such localization of NOX4 or any other NADPH oxidase was observed in mitochondria in other reports (100), whereas Gorlach group localized NOX4 to endoplasmic reticulum in endothelial cells and was shown to be essential for endothelial ROS production and proliferation (346). Thus, further investigations are needed to identify the localization of NOX4 and the potential cross-talk between mitochondria and NADPH oxidase. A dysregulation in this relationship may drive the vicious feed-forward cycle of ROS accumulation that can enhance inflammatory response in different diseases (96, 380).
C. Uncoupled NOS-derived ROS in inflammation
NOSs are a family of enzymes that catalyze the production of nitric oxide (NO) from L-arginine. There are three different isoforms of NOS, including neuronal NOS (nNOS), inducible NOS (iNOS), and eNOS. Of these isoforms, only eNOS is the membrane-associated protein and is the predominant source of NO in vascular endothelial cells (121). iNOS and nNOS are soluble isoforms and are present in the cytosol. eNOS exists as a dimer consisting of a c-terminus reductase domain of one monomer connected with the oxygenase domain of the other monomer at N-terminus (Fig. 5a). The reductase domain binds to NADPH, FMN, and FAD, and the oxygenase domain binds to prosthetic heme group as well as the cofactor tetrahydrobiopterin (BH4) and molecular oxygen. The prosthetic heme group connects the two monomers. The electrons are transferred from the bound NADPH in the reductase domain to the heme prosthetic group on oxygenase domain of eNOS. NO is produced by eNOS in two successive mono-oxygenation reactions of arginine, leading to formation of L-citruline (Fig. 5a) (121). The electron transfer in eNOS is a tightly regulated process; however, eNOS uncoupling may lead to transfer of electrons to molecular oxygen rather than arginine, resulting in O2
•− production (121). The superoxide generated by eNOS uncoupling has been implicated in a variety of inflammatory conditions, including acute lung injury (385), diabetes mellitus (178), and Ang II-induced hypertension (298). NO possesses strong anti-inflammatory properties. Dal et al. have shown that iNOS
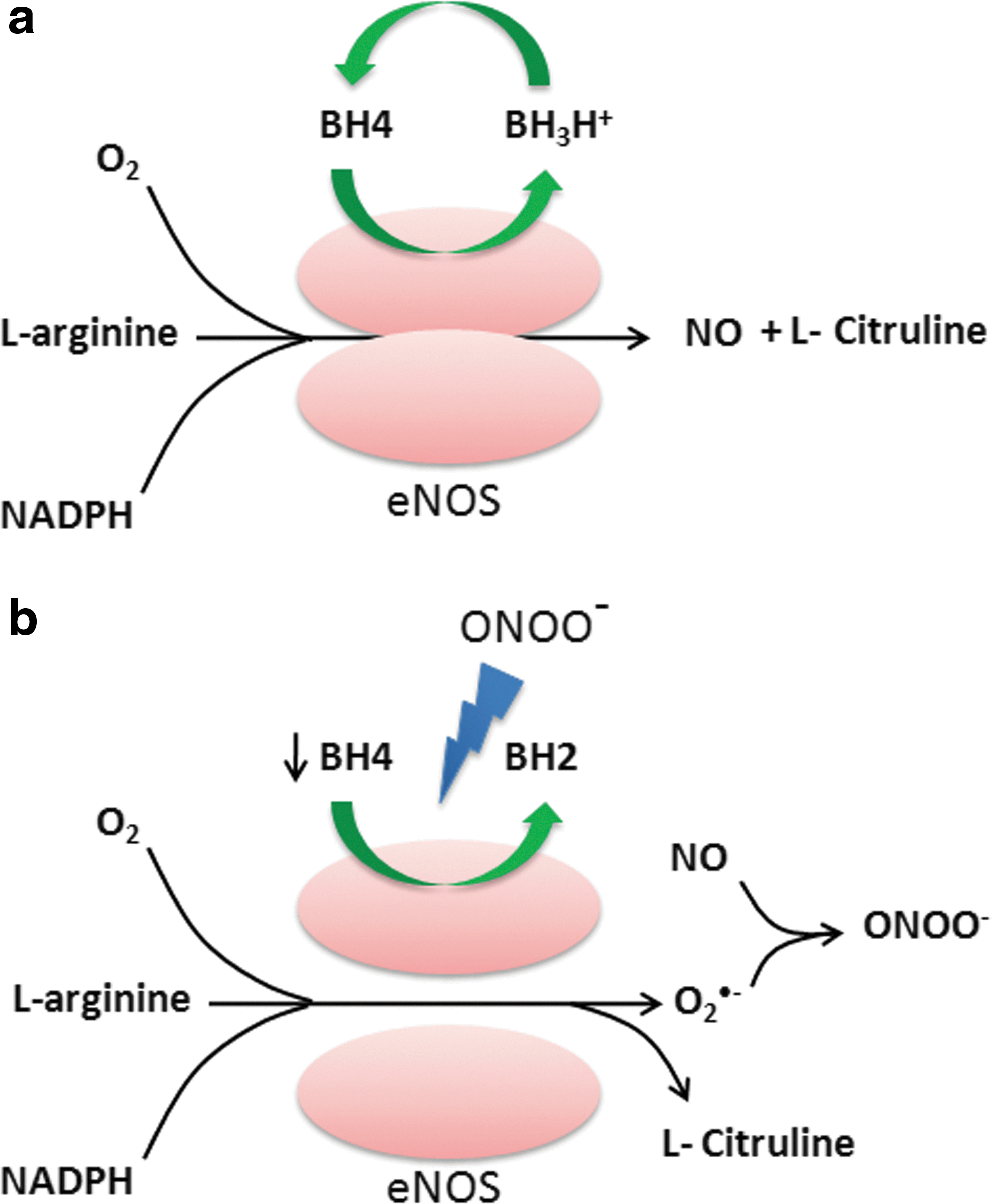
The cofactor BH4 plays a crucial role in maintaining the integrity of the eNOS system by stabilizing eNOS dimers (10). BH4 donates the second electron to the first mono-oxygenation reaction of L-arginine, generating N-hydroxy-arginine as the intermediate The deficiency of BH4 leads to eNOS uncoupling, as the intermediate reacts with molecular oxygen, resulting in O2 •− production (Fig. 5b) (10). The reduced bio-availability of BH4 has been reported to be due to oxidation by peroxynitrite, resulting in the formation of inactive BH2 (237). The oxidative inactivation of BH4 is sufficient to produce eNOS uncoupling. The mice deficient in eNOS did not exhibit an increase in vascular superoxide production when compared with the wild-type mice in the mouse model of desoxycorticosterone acetate (DOCA)-salt hypertension, suggesting that eNOS uncoupling is the major source of endothelial-generated O2 •− (235). In addition, p47phox knockout mice were relatively protected from BH4 oxidation and eNOS uncoupling, suggesting that NADPH oxidase-mediated O2 •− production is an important contributor to oxidative loss of BH4 and eNOS uncoupling (330). Interestingly, the administration of BH4 in eNOS over-expressing mice was found to significantly decrease O2 •− production and reduce the formation of atherosclerotic plaques by preventing eNOS uncoupling (330). Thus, the stoichiometric ration of BH4 to eNOS is critical in eNOS uncoupling.
In addition to BH4, increased levels of asymmetrical dimethyl arginines (ADMA), an endogenous inhibitor of eNOS, reportedly lead to eNOS uncoupling and enhanced O2 •− production (404). Increased levels of ADMA have been reported in endothelial cultures treated with low-density lipoprotein, mouse lung exposed to endotoxin LPS, and septic shock patients (44, 322, 385). ADMA are generated by S-adenosylmethionine–dependent protein arginine methyltransferases that themselves are induced by enhanced oxidative stress (404).
D. XO-derived ROS in inflammation
Xanthine oxidoreductase is a soluble high-molecular-weight (270 kD) enzyme that catalyzes the oxidation of hypoxanthine to xanthine and uric acid. It exists in two forms: xanthine dehydrogenase (XDH) and XO (332). XDH reduces NAD+, whereas the XO is the main superoxide-producing enzyme. An irreversible proteolytic conversion of XDH to XO can be triggered by ischemic conditions (282). The activity of XDH/XO is specifically induced by IFN-γ in lung microvascular endothelial cells and the pulmonary artery endothelial cells. In contrast, IFN-α/β, TNF-α, IL-1 or -6, LPS, and PMA have no effect on the activity of XDH/XO (104). The activity of XO is up-regulated in the airway inflammatory disorders, ischemia reperfusion injury, atherosclerosis, diabetes, and autoimmune disorders such as rheumatoid arthritis (332). The serum samples from rheumatic patients may have approximately 50-fold higher levels of XO compared with healthy donors (289). Moreover, in diabetic rats, the administration of XO inhibitor allopurinol suppressed the NF-κB activation, neutrophil infiltration, and expression of inflammatory cytokines in the liver, suggesting a key role of XO-derived ROS in type I diabetes (363). XO-derived ROS has also been implicated in pulmonary vascular remodeling induced by chronic hypoxia in neonatal rats (196). The serum activity of XO is up-regulated by hypoxia, and administration of allopurinol limited the hypoxia-induced oxidative stress in the lung and pulmonary vascular remodeling; highlighting the critical role of XO-derived ROS in the chronic hypoxia induced pulmonary hypertension (196). Altogether, the XO-derived ROS seems to be important in a variety of inflammatory disorders; however, the therapeutic advantage of XO inhibitors such as allopurinol for other inflammatory diseases and other forms of organ injury remains to be investigated.
E. Regulation of antioxidant defense systems in inflammation
To prevent the damaging effects of oxidants, vertebrate cells have evolved an array of antioxidant defense systems that functions to remove ROS. The antioxidant enzymes SOD (dismutates O2
•
Catalase is a cytoplasmic 240 kD homotetrameric protein and is an important intracellular antioxidant enzyme detoxifying the H2O2 to oxygen and water. The expression of catalase has been reported in alveolar type II cells and macrophages, and highest expression has been reported in the liver and erythrocytes (355). Arita et al. have shown that targeting of catalase directly to the mitochondria in lung epithelial cells protects them from H2O2-induced apoptosis (14). Despite this important physiological link, no increase in the activity of catalase was reported after hyperoxia in endothelial cells (202) and bronchial epithelial cells, which made them more susceptible to hyperoxia-induced injury (110). Moreover, the LPS treatment decreased the expression and activity of catalase in mouse lung, a response preceding NF-κB activation (67). The congenital deficiency of catalase known as acatalasia is benign; however, in certain conditions, increased susceptibility to diabetes has been reported (355). Whether catalase is important in the pathogenesis of inflammation remains an open question.
The family of GPx enzymes serves the similar function of detoxifying H2O2 as catalase. There are four selenium-dependent GPx enzymes (GPx1–4) in mammalian tissue with a wide tissue distribution (270). GPx enzymes are tetrameric 85 kDa protein and carry four atoms of selenium bound in their catalytic core. These enzymes detoxify H2O2 by oxidizing monomeric glutathione (GSH) into dimeric glutathione disulfide (GSSG). Oxidized GSSG is converted back to its monomeric GSH form by glutathione reductase. The expression and activity of GPx is induced by hyperoxia in endothelial cells (202). However, GPx knockout mice showed no hypersensitivity to hyperoxia-induced lung injury, indicating the compensation from other antioxidant enzymes (180). Reduced levels of GSH have been reported in a variety of inflammatory conditions (356), indicative of its important role in the inflammatory response through enhancing oxidative stress.
Peroxiredoxins are a group of related antioxidant enzymes that catalyze the degradation of H2O2 to water. There are six different (Prx1–6) identified so far with molecular weights ranging between 17—and 31 kD (190). All subtypes of Peroxiredoxins are expressed in lung tissue (190). The Prx6 knockout mice exhibit enhanced hypersensitivity to hyperoxia-induced lung injury (439), whereas Prx6 overexpressed mice were resistant to such damage (441). Prx1 knockout mice were also reported to be prone to bleomycin-induced lung inflammation (214) and allergic airway inflammation (187). Further, administration by N-acetyl-cysteine in Prx1 knockout mice was found to protect them against bleomycin-induced acute lung injury, indicating a protective role of Prx1 against oxidative damage in inflammation (214).
Trxs are 10–12 kDa redox-sensitive antioxidant enzymes that maintain the proteins in their reduced state by catalyzing the reduction of proteins disulfides to their corresponding sulfhydryls utilizing the reducing equivalents NADPH (311). Three Trx enzymes have been identified thus far (Trx1, 2, and 3). Oxidized Trx is recycled back to its reduced state by Trx reductase. The protective effects of Trxs as an antioxidant enzyme was reported in a variety of oxidative stress-related diseases such as ishchemia reperfusion injury, inflammation resulting from activation of neutrohils, blemomycin-induced lung injury, and inflammation induced by pro-inflammatory cytokines (311). There are two Trxs interacting proteins discovered so far; TBP-1 or p40phox and TBP-2, also known as VDUP1 (311). The interaction of Trx with p40phox subunit of NADPH indicates that it may also regulate the ROS generation via NADPH oxidases.
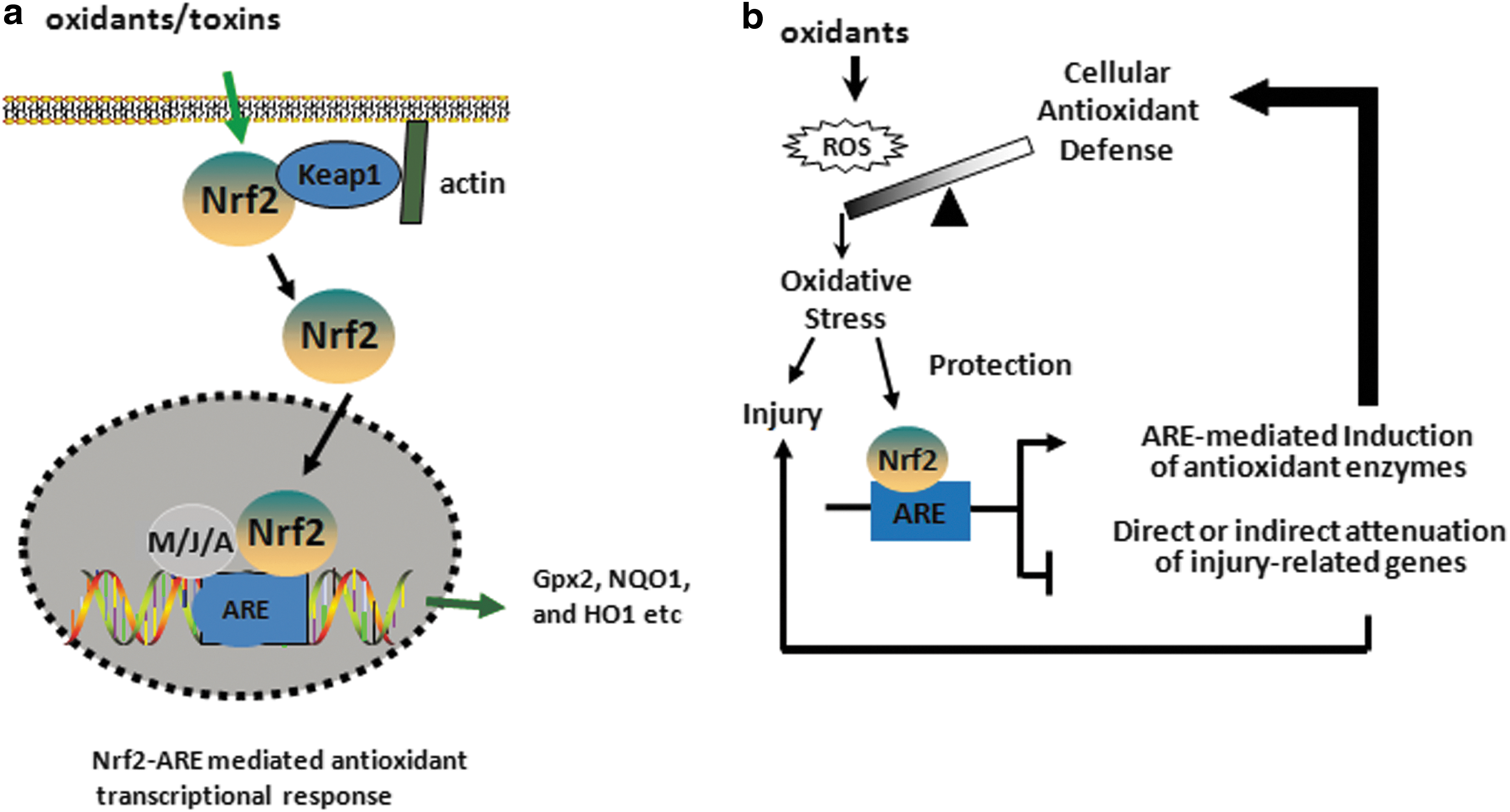
The induction of several antioxidant and cytoprotective genes is mainly regulated by the transcription factor NF-E2-related factor 2 (Nrf2), which is a cap'n’collar basic leucine zipper protein. The Kelch-like ECH-associated protein 1 (Keap1) retains Nrf2 in the cytoplasm and promotes its proteosomal degradation under basal condition (192, 193). In response to oxidative stress, Nrf2 dissociates from Keap1 and translocates into the nucleus, where it dimerizes mainly with the MAF (Maf-G, Maf-F, and Maf-K), JUN (c-Jun, Jun-B, and Jun-D), and ATF (ATF-4) families of bZIP proteins and transactivates a network of genes encoding cytoprotective and antioxidative enzymes containing the antioxidant response element (ARE), 5′-TGAG/CnnnGC-3′ in their promoters such as Gpx, NAD(P)H:quinone oxidoreductase (NQO1), and heme oxygenase-1 (HO1) (Fig. 6). The deficiency of Nrf2 enhances the susceptibility to experimental acute lung injury and impairs the resolution of lung inflammation in mice. Nrf2 activators such as triterpenoids (CDDO-Im) that target cysteine residues of Keap1 have been used to specifically disrupt Keap1:Nrf2 interactions, thereby promoting Nrf2 nuclear accumulation and leading to Nrf2-target gene induction (247) in Nrf2-sufficient but not in Nrf2-deficient cells in vitro and in vivo, suggesting that specific targeting of Nrf2-ARE signaling may provide a novel therapeutic strategy for treating human diseases. We and others have shown reduced levels of acute lung injury and inflammation (360) and emphysema in mice treated with CDDO-Im (402). Recently, triterpenoid analogue, bardoxolone methyl, showed improved renal function in early-stage chronic kidney disease in type 2 diabetes; however, Phase III clinical trial with this compound for very severe-stage patients was halted due to undisclosed safety issues (Reata Phamaceuticals) (ClinicalTrials.gov; NCT01351675). Moreover, the recent study by Zoja et al. has shown that bardoxolone analogues are ineffective in curing diabetic nephropathy in Zucker diabetic fatty rats but instead, the rats receiving such analogues worsen the outcome of the disease (476). While the CDDO-Im potently activates Nrf2 target genes in multiple tissues, proteomic analysis recently revealed that this CDDO-Im interacts with ∼600 different proteins, including many different transcription factors (464). Since Nrf2 confers protection against oxidation-related pathologies and Nrf-2 activation may be a useful antioxidant strategy, it is likely that the unwarranted effects of chronic CDDO treatment may be related to nonspecific off-target effects. Alternatively, it is possible that prolonged activation of Nrf2 signaling may be more complicated because of the possibility of activation compensatory pro-oxidative stress pathways.
III. Cell Adhesion Molecules and Leukocyte Migration Across Transendothelial Barrier
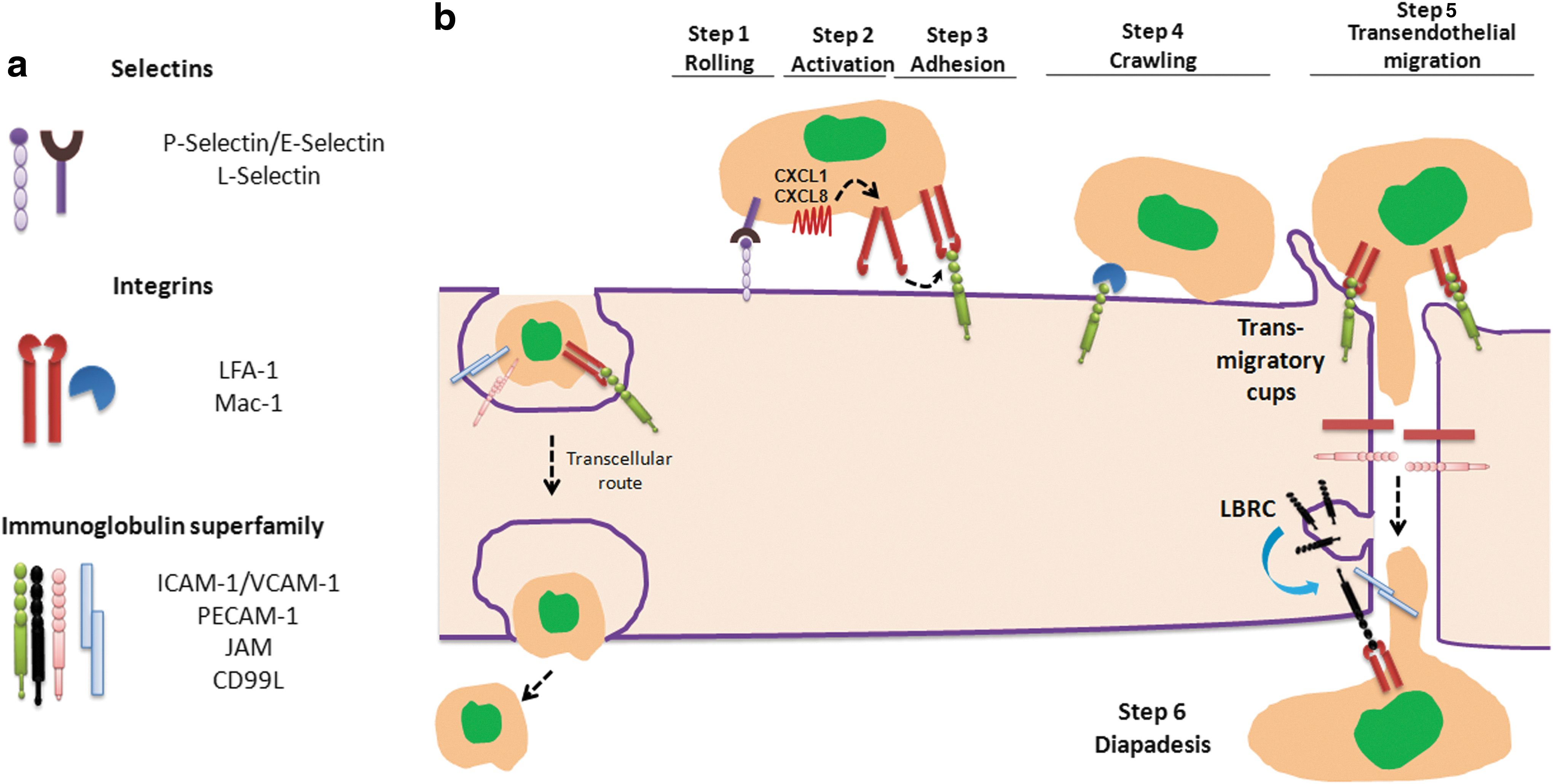
The migration of inflammatory cells across the endothelium of postcapillary venules is mediated by the adhesive interactions between the cell adhesion molecules (CAMs) expressed on activated endothelial and leukocytes. The neutrophils are the first cells to arrive at the inflamed location. The extravasation of neutrophils across the endothelial barrier occurs through endothelial junctions (paracellular pathway) and more rarely through the endothelial cell body (transcellular pathway) (459). The transcellular route is used by 10%–15% of the migrating neutrophils, but it varies greatly among tissues (366, 462). The three families of adhesion molecules that are crucial for leukocyte transmigration are selectins, integrins, and ICAM members of immunoglobulin (Ig) superfamily (Fig. 7a). The process of neutrophil transmigration is mediated by four sequential steps: (i) rolling, (ii) activation directed migration by setting up a chemoattractant gradient, (iii) adhesion to the endothelial cells, and (iv) transendothelial migration (Fig. 7b).
A. Selectins
They are membrane glycoproteins that are expressed in both endothelial cells and leukocytes and are of three different types: P- (expressed in platelets and endothelial cells), L- (expressed in all leukocytes), and E- selectins (expressed in endothelial cells) (27, 466). The initial rolling of neutrophils on endothelial cells in response to inflammatory stimuli is mediated by selectins (Fig. 7b). Selectins are characterized by the presence of a carbohydrate recognition domain known as lectin that allows a low-affinity binding to sialylated carbohydrate moieties of mucin-like CAMs on leukocytes. These residues, known as sialyl Lewis-x (SLex) antigen, play an important role in leukocyte tethering and rolling (466). Inherited defects in intracellular fucose transport impairs the formation of Lewis-x, resulting in leukocyte adhesion deficiency type II (LAD II) that is characterized by recurrent bacterial infection and impaired ability of neutrophils to bind endothelial cells expressing E-selectin (113, 255, 348). Neutrophil rolling on vascular endothelium is the result of sequential formation and the detachment of selectin-mediated bonds between neutrophils and endothelial cells (466). Selectin mediated rolling of leukocytes on endothelial cells greatly reduced velocity of leukocytes from hydrodynamic velocity of 200 to <5 μm/s (137, 466).
In endothelial cells and platelets, P-selectin (also known as granule membrane protein-140 [GMP-140]) is stored within Weibel–Palade bodies from which it is rapidly recruited to the cell surface during neutrophil migration; whereas E-selectin is up-regulated due to protein synthesis induced by activation of E-selectin gene in response to inflammatory stimuli such as IL-1β, LPS, or TNF-α (154, 166). P-selectin glycoprotein ligand-1 (PSGL-1) is constitutively expressed in neutrophils and T lymphocytes and binds to both P and E-selectin; however, affinity of E-selectin for PSGL-1 is 50 times lower compared with P-selectin (301). E-selectin binds to ligand E-selectin ligand-1 (ESL-1) that is expressed in neutrophils and plays a key role in neutrophil rolling (395, 466). The ligands for L-selectin include PSGL1, P-selectin, and E-selectin as well as Glycam-1, CD34, and MAdCAM-1, which are highly expressed in high endothelial venules (HEVs) and help in the homing of T lymphocytes in lymph nodes (466). On leukocyte activation, L-selectin is rapidly shed from the cell surface via a protease-dependent mechanism, which is important in the mechanism of transmigration and has also been implicated in mediating inflammation (159).
B. Integrins
They are heterodimeric proteins, consisting of alpha and beta chains, and are expressed in leukocytes and many other cell types (114). They facilitate firm adherence to the vascular endothelium. β2-integrins are the primary adhesion molecules that are expressed in leukocytes, and they bind to Ig superfamily member ICAM-1 which is expressed on the endothelial cell surface (114). β2-integrins are involved in firm adhesion strengthening and transendothelial migration of leukocytes (114). In contrast to selectin-mediated adhesion, which leads to the rolling of neutrophils, adhesion of leukocytes by β2 integrins is firm and is regarded an essential step for trans-endothelial migration of inflammatory cells. β2-integrins are activated by chemokines such as CXCL1 (stored in small cytoplasmic granules) and CXCL8 (stored in Weibel–Palade bodies), which are secreted by endothelial cells (456, 465). The binding of chemokines to chemokine receptors (CXCR1 and CXCR2) changes the conformation of integrins from bent to fully extended high-affinity configuration, enabling neutrophil arrest by binding to ICAM-1 that is expressed in endothelial cells (Fig. 7b) (465).
β2 integrins are grouped into the categories according to the β subunit they contain. The β2 integrins include leukocyte function-associated antigen 1 (LFA-1 or αLβ2) and Mac-1 (αMβ2) and β1 integrins such as very late antigen 4 (VLA4 or α4β1), α9β1, and α5β1 are common antigens that are expressed in leukocytes (114, 181). LFA-1 is the principal adhesion molecule in neutrophils that binds to ICAM-1 in endothelial cells and mediates transition from rolling to adhesion on the endothelial cell surface (350). Mac-1 also binds to ICAM-1 and mediates crawling of neutrophils along endothelial cells to the entry of endothelial junctions for paracellular migration (350). There is a 10-fold decrease in crawling displacement in Mac-1 null neutrophils, which forces them to transmigrate close to the initial site of adhesion and leads to transmigration (350). The activation of LFA-1 is induced by the activation of chemokine receptors on neutrophils by ligands that are secreted by endothelial cells such as CXCL1 (465). Fully activated LFA-1 mediates the stop of rolling and makes firm adhesion along with Mac-1 (175). Deficiency of β2 integrin chain causes Leukocyte Adhesion Deficiency Type 1, an inherited disorder that is characterized by inability of leukocytes to undergo adhesion-dependent migration (49). These patients suffer from recurrent bacterial infections. β2 integrin Mac-1 favors paracellular migration of leucocytes and in Mac-1−/− (CD11b) mice, neutrophils predominantly emigrate transcellularly (through endothelial cells) and were delayed by 20–30 min compared with the more rapid paracellular emigration route (351). In contrast to β2 integrins, the β1 integrin family mediates neutrophil adhesion to extracellular matrix proteins such as fibronectin and VLA4 or α4β1 integrin. The coating of fibronectin in an in vitro migration assay can greatly enhance the migration of human PMNs (115). VLA4 or α4β1 integrin in murine neutrophils mediates leukocyte adhesion to endothelial cells by interacting with VCAM-1 (9). However, VLA4 is not expressed in human neutrophils, but its function instead is served by α9β1 integrin. α9β1 integrin is a major β1 integrin that is induced on neutrophil activation which mediates binding to VCAM-1 (265). However, β1-integrin-mediated adhesion has a limited role in adhesion and transendothelial migration of neutrophils compared with β2 integrins (265). After β2-integrin-mediated neutrophil arrest, there is a polarization of neutrophils at the leading edge referred to as lamellipodium that orchestrates receptors for chemokines and phagocytosis. Polarization of neutrophils, which is important for efficient transendothelial migration, is mediated by the organization of filamentous actin (F-actin) cytoskeleton at the leading edge (375, 461).
C. Ig superfamily
It consists of CAMs that have an Ig-like domain and are expressed in endothelial cells, platelets, and leukocytes. Included in this family are members of inter-cellular adhesion molecules (ICAM-1 and -2), vascular cell adhesion molecule (VCAM-1), platelet endothelial cell adhesion molecule (PECAM-1 or CD31), junctional adhesion molecules (JAM-A, -B and -C), CD99 antigen-like 2 (CD99L2), and endothelial cell-selective adhesion molecule (ESAM) (45). The expression of ICAM-1 and VCAM-1 is increased on activated endothelium (166). At the time of neutrophil transmigration, ICAM-1 and VCAM-1 are recruited in specialized preformed tetraspanin-enriched microdomains (TEMs) and promote nano-clustering of adhesion receptors to increase leukocyte binding to endothelium (25). These specialized TEM domains have been termed endothelial adhesive platforms and are formed independent of ligand binding and actin cytoskeleton anchorage (25). The binding of LFA-1 integrin on neutrophils with ICAM-1 on endothelial cells generate signals that activate Rho A, leading to actin polymerization and formation of transmigratory cups (423). Transmigratory cups are microvilli-like projections that surround leukocytes and help in efficient transendothelial migration of leukocytes (24, 52). The adaptor proteins of ERM family (ezrin, radixin, and moesin) link ICAM-1 and VCAM-1 with actin cytoskeleton and help in reorganization of actin cytoskeleton and formation of transmigratory cups (25). The deep penetration of neutrophils between endothelial cells is mediated by JAM-A (Fig. 7b), as neutrophils accumulate deeper down the junctions in JAM-A
D. High endothelial venules
The postcapillary vascular endothelium of all the secondary lymphoid organs except spleen is constitutively enriched in CAMs. These regions were classified as HEVs, enabling circulation of naive lymphocytes between the blood and lymph node. Approximately 25% of all the lymphocytes circulating in HEVs bind and emigrate into a single lymph node (via HEVs) every second (134). In addition to commonly expressed CAMs in normal venules, HEVs abundantly express highly glycosylated and sulfated forms of adhesion molecules, including glycosylation-dependent cell-adhesion molecule 1 (GLYCAM1), CD34, MAdCAM-1, and peripheral LN addressin (PNAd), which are commonly referred to as vascular addressins, enabling rapid homing of lymphocytes in lymphoid organs (296). Certain chronic inflammatory conditions such as rheumatoid arthritis, psoriasis, Hashimoto's thyroditis, Crohn's disease, ulcerative colitis, and multiple sclerosis are accompanied by development of HEVs in normal organs, facilitating a large influx of lymphocytes that contribute to chronic inflammation (8, 231). This de novo formation of organized lymphoid tissue in chronic inflammation diseases has been termed lymphoid neogenesis. Lymphotoxin-α, a member of TNF family, has been implicated in the development of secondary lymphoid organs in these diseases (179). Psoriasis is a common cutaneous inflammatory disorder in which the dermal microvasculature undergoes distinctive changes, including HEV formation, which facilitates trafficking of lymphocytes to the skin (253). There is an interesting correlation between Ang II-mediated activation of the immune system and hypertension (158, 450) with the increased risk of hypertension and cardiovascular mortality in psoriasis patients that is associated with elevated levels of Ang II (253, 285).
E. Regulation of CAMs by oxidative stress
There is considerable evidence indicating that extravasation of leukocytes in response to inflammatory stimuli is regulated by oxidative stress that is produced by leukocytes. The adhesion of neutrophils to the surface of endothelial cells has been demonstrated to elicit a biphasic response that is related to endogenous ROS production in endothelial cells (221). Oxidative stress can regulate the expression of endothelial CAMs by a direct activation of CAMs that presents on the surface and also by a transcription-dependent mechanism involving redox-sensitive transcription factors (i.e., NF-κB and AP-1). In this regard, Patel et al. (337) demonstrated that external application of H2O2 or t-butylhydroperoxide as early as 1 h in HUVECs was accompanied by transcriptional-independent surface translocation of P-selectin, leading to increased PMN adherence. Treatment of cells with an antibody against P-selectin or antioxidant treatment abolished neutrophil adhesion to endothelial cells. Antibodies directed against P-selectin abolished an O2
•
The promoter region of ICAM-1 contains binding sites for inducible redox sensitive transcription factors such as NF-κB and AP-1 (239, 361). H2O2 increases the transcripts of ICAM-1 in HUVECs within 30 min, the response was sustained for approximately 2 h, and antioxidant treatment (catalase) or application of ICAM-1 antibody abrogated the H2O2-induced PMN adhesion (251). TNFα-induced NF-κB activation and ICAM-1 expression in endothelial cells is dependent on oxidants that are generated by the PMN NADPH oxidase complex (117). In p47phox−/− mice, TNFα-induced NF-κB activation and ICAM-1 expression were significantly attenuated as compared with the wild-type mice (117, 432). Moreover, PMNs from p47phox−/− mice showed markedly reduced adhesion to mouse lung vascular endothelial cells, indicating the essential role of oxidant signaling in NF-κB activation and ICAM-1 expression in endothelial cells (117). Oscillatory shear stress (OS) induces endothelial expression of ICAM-1, and monocyte adhesion is also dependent on ROS that is produced from NADPH oxidases (393). ECs obtained from p47phox−/− mice showed impaired adhesion to monocytes in response to OS and were restored when the cells were transfected with p47phox plasmid. Furthermore, OS increased mRNA levels of NOX2 and NOX1, and monocyte adhesion was shown to be blocked by siRNA against NOX1. Interestingly, Matheny et al. have shown that VCAM-1 ligand binding induced ROS generation via NADPH oxidases in endothelial cells and promoted lymphocyte migration by actin restructuring in endothelial cells (278). Inhibiting NADPH oxidase activity with DPI or Apocynin blocked lymphocytic migration across mouse endothelial cells to greater than 65% (278). Expression of VCAM-1 in HUVECs was up-regulated by cytokine IL-1β and enhanced ROS generation. Treatment with antioxidant pyrrolidinedithiocarbamate (PDTC) and N-acetyl cysteine (NAC) repressed greater than 90% of the IL-1β-induced increase in VCAM-1 expression (276). Increased expression of ICAM-1 and P-selectin was also observed in the mouse model of acute pancreatitis that was dependent on enhanced ROS production (412). In the mouse model of atherosclerosis, Ang II-induced expression of VCAM-1 was dependent on mitochondria-derived ROS (354). In addition, in patients suffering from obstructive sleep apnea, an increased expression of adhesion molecules CD15 (a counter-receptor for selectins on ECs), CD11c (counter-receptor for ICAM-1 on ECs) on monocytes was correlated to increased ROS generation (105, 381). These monocytes showed increased adherence in culture to human endothelial cells and generated more intracellular ROS compared with control subjects (105). Continuous positive airway pressure treatment of these patients decreased basal ROS production in monocytes and concomitantly decreased the expression of CD15 and CD11c on monocytes (105). The circulating levels of ICAM-1, VCAM-1, and E-Selectin are elevated in hyperlipidemic and hyperglycemic and noninsulin-dependent diabetic-patients in direct correlation with increased oxidative stress (58, 69, 86, 313, 352). Reducing oxidative stress by GSH administration or NAC or low-fat diet improved the circulating levels of adhesion molecules (5, 57, 85, 86). All of these reports indicate that increased expression of CAMs induced by oxidative stress can contribute to the pathogenesis of the inflammatory disorders.
IV. Structural Basis of Endothelial Integrity
The vascular endothelium lining the blood vessels forms a continuous, semi-permeable restrictive barrier enabling the passage of macromolecules, inflammatory cells, and fluid between the blood and interstitial space. There are two different routes of transport across the endothelial barrier, transcellular (across the cell) and paracellular (between the cells). The transcellular route is adopted by the larger solute macromolecules having molecular radius >3 nm (284). The plasma protein albumin is actively transported by transcellular route by binding to a docking protein gp60 present in caveoli that transport it across the endothelium (284). The solute molecules (such as urea, glucose, amino acids, and certain ions) having Mr <3 nm and inflammatory cells take a paracellular route of transport across endothelium. The paracellular route is tightly controlled by inter-endothelial junctions (IEJs) and TJs, which provides an unperturbed restrictive barrier to the endothelium (Fig. 8). The paracellular permeability is the major route of vascular leakage observed in a variety of inflammatory states. The paracellular permeability was first described by Majno and Palade in rat cremaster muscle microvessels treated with a subcutaneous injection of histamine. They found that treatment with histamine leads to the formation of 0.1–0.8-μm-wide gaps along venular endothelium (262, 263). Paracellular permeability enables the extravasation of protein-rich fluid from the luminal to abluminal side of the endothelium though gaps formed between endothelial cells. The resulting protein-rich fluid leads to edema formation, which is a characteristic feature of most of the inflammatory conditions. Many of the permeability enhancing agents such as VEGF, thrombin, and PAF exert their actions by forming gaps between endothelial cells. The composition of TJs and IEJs and their regulation by oxidative stress and permeability-enhancing agents is described next:
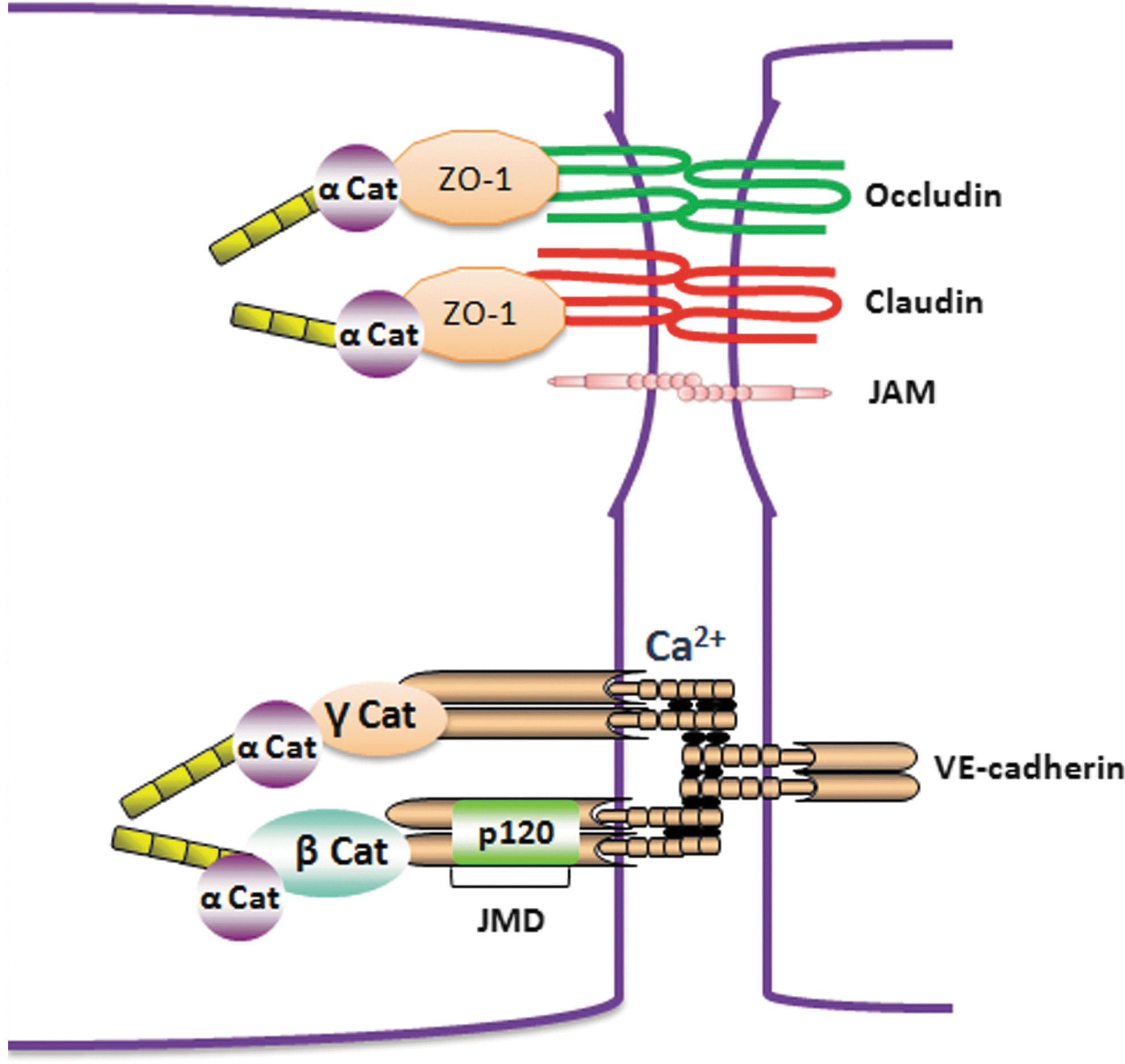
A. Tight junctions
TJs are composed of transmembrane proteins occludins, claudins, and JAMs. The transmembrane proteins of TJs are connected to actin cytoskeleton by cytoplasmic adaptor proteins (zonula occludens [ZO]-1, -2, and -3, AF6, and cingulin). TJs in endothelial cells represent ∼20% of all the junctional complexes (454). The tightness of TJs depends on the protein composition and varies in different tissues ranging from almost complete tightening of the paracellular cleft for solutes (e.g., as in the blood brain barrier) to the formation of paracellular pores for specific ions. All transmembrane proteins of TJs, including occludins, claudins, and JAMs, possess a PDZ (postsynaptic protein disc large ZO-1)-binding motif in the C-terminal that binds to cytoplasmic adaptor proteins containing PDZ domain. Occludin consists of four transmembrane domains and two extracellular loops that enable a homotypic interaction with other occludin molecules and contributes to the TJ assembly. Arterial endothelial cells that are less permeable compared with vein endothelial cells have almost 18-fold greater expression of occludin (211). The C-terminal of occludin is linked to actin cytoskelton by cytoplasmic adaptor protein ZO-1. The role of occludin in maintaining TJ stability is not clear. In vitro studies showed that disruption of occludin function using antisense oligonucleotide or peptide antagonists against occludin molecules decreased transendothelial electrical resistance, whereas occludin
Claudins are transmembrane proteins of TJs that are similar to occludins and possess four transmembrane domains, two extracellular loops, and an N-terminal and C-terminal cytosolic domains. At least 24 claudins are identified in humans. Similar to occludin, the PDZ domain in the c-terminus of claudin interacts with ZO-1 and connects claudins with actin cytoskeleton. The composition of claudins varies in different endothelial barriers and, hence, determines whether the barrier is selectively permeable (e.g., the ion selective pores in the kidney) or impermeable (e.g., blood–brain barrier) (328). Pore-forming claudins such as claudin 2 (Cldn-2) form pores that are specific to monovalent cations and water and are found in Madin–Darby Canine Kidney (MDCK) cells. The claudins involved in the sealing of TJs include claudin 1, 3, 5, 11, and 19 (328). Of these claudins, claudin 5 is highly expressed in the blood–brain barrier, and claludin 5−/− null mice die within 10 h after birth (320). Although in these mice the development and morphology of blood vessels were not altered and showed no brain edema, however, it selectively increased the permeability to small molecules with MW <800 D (320).
JAMs belong to Ig superfamily of proteins consisting of a single-pass membrane protein with a long extracellular domain. At least three different isoforms of JAMs are known, including JAM-A, JAM-B, and JAM-C (18). The expression pattern of the JAMs varies significantly in different cell types. JAM-A is more widely distributed in epithelial cells, endothelial cells, monocytes, and neutrophils. The expression of JAM-C is exclusively restricted to endothelial cells, whereas JAM-B is more abundant in HEVs of lymphatic organs (16 –18). The homophilic interaction between different JAMs contributes to the tightness of the TJs. Studies show that expression of JAM-A or JAM-C in CHO cells reduced the paracellular permeability to FITC dextran (17, 273). Moreover, antibodies directed against JAM-A significantly delayed the recovery of transepithelial electrical resistance during TJ reformation in epithelial cell monolayers (246). Orlova et al. (325) showed that JAM-C was mainly localized intracellularly in quiescent microvascular endothelial cells, and was recruited to junctions on stimulation with VEGF or histamine. Notably, disruption of JAM-C function decreased basal permeability and prevented the further increase in permeability induced by VEGF and histamine in human dermal microvascular endothelial cells in vitro and skin permeability in mice. JAMs are also known to interact with different integrins on adjacent cells. This heterophilic interaction regulated leukocyte–endothelial cell and leukocyte–platelet interactions (326, 329, 373).
ZOs belong to a membrane-associated guanylate kinase (GUK) homologue protein family. There are three ZO subtypes (ZO-1, -2, -3), and all of them possess three domains: PDZ, an Src homology 3 (SH3), and GUK (140, 305). ZO is an acronym for ZO. ZO-1 was the first TJ-specific protein identified (398). ZO1 acts as a scaffolding protein, as it interacts directly with claudins and also binds to the other Adherens junction (AJ) proteins such as α-catenin and to connexins in gap junctions (228). Through their PDZ, SH3, and GUK domains, ZOs are critical in recruiting signaling molecules to TJs, and thereby linking TJ proteins to the actin cytoskeleton (140).
B. Adherens junctions
AJs are composed of the cadherin family of transmembrane adhesion proteins that are anchored to the cytoskeletal network by intermediate cytoplasmic proteins from the catenin family, including α-, β-, γ-, and p120 catenins (31). There are two types of cadherins present in endothelial cells: VE-cadherin (vascular endothelial cadherin) and N-cadherin (N for neuronal) (315). Although both are abundantly expressed in endothelial cells, VE-cadherin mainly promotes the homotypic interaction between endothelial cells, and when present, it excludes N-cadherin from those sites (315). VE-cadherin is a homophilic binding protein that mediates the interaction of endothelial cells in a calcium-dependent manner. It has five cadherin-like repeats in its extracellular domain that oligomerize in a cis- and trans-manner with other VE-cadherin molecules between the same and adjacent cells (Fig. 8). The cytoplasmic tail of VE-cadherin contains two functional domains: juxtamembrane domain (JMD) and C-terminal domain (CTD). JMD of VE-cadherin binds p120-catenin, whereas CTD binds β-catenin and γ- catenin (also known as plakoglobin) (Fig. 8) (31). α-catenin by binding to β- and γ- catenin links the catenin-cadherin complex to the actin cytoskeleton. Both the N- and C-terminus of VE-cadherin are essential in the regulation of endothelial barrier function. Monoclonal antibodies targeted against N-terminus of VE-cadherin prevented the formation of IEJs and increased the microvascular permeability (70, 71). Interestingly, the C-terminal-truncated mutant of VE-cadherin in CHO cells did not impair the ability of cells to form aggregates; however, it greatly enhanced the intercellular junction permeability to high-molecular-weight molecules (56, 314). This finding suggests that the N-terminal region of VE-cadherin is required for cell–cell adhesion, whereas the C-terminal provides a tight restrictive barrier regulating paracellular permeability. VE-cadherin is essential for the development of endothelial barrier in embryos, and VE-cadherin knockout mice die in the embryonic stage due to abnormal vascular development (53). Moreover, expression of dominant negative VE-cadherin mutants also resulted in leaky junctions and an increase in microvascular permeability (430). Homotypic binding of VE-cadherin molecule between endothelial cells is stabilized by calcium, and chelation of calcium using EDTA destabilized the junctions and increased transendothelial permeability (125).
Catenins are equally important in regulating the stability of AJs by connecting them with actin cytoskelton. Deletion of β-catenin binding site on VE-cadherin caused lethality at 9.5 days of gestation (53). Similarly, conditional deletion of β-catenin in cultured endothelial cells reduced the ability of endothelial cells to maintain intercellular contacts and increased paracellular permeability (55). p120 catenin regulated the surface expression of VE-cadherin, and the depletion of p120 by siRNA decreased the VE-cadherin expression and increased the junctional permeability. In addition, p120 catenin acted as a scaffold protein by binding with two different tyrosine phosphatases, including Src homology 2 domain-containing tyrosine phosphatase-1 (SHP-1) and protein tyrosine phosphatases (PTPμ), which regulated VE-cadherin phosphorylation and stability of the junctions (210, 271, 477) (see next section).
C. Regulation of endothelial junctional proteins and associated cytoskeleton by oxidative stress
Oxidative stress produced by leukocytes at the site of inflammation plays a crucial role in initiating junctional disassembly. At the site of inflammation, AJs are disrupted by several mediators that are released by inflammatory cells, including ROS, cytokines, chemokines, thrombin, histamine, PAF, VEGF, and bradykinins. Most of these molecular mechanisms converge on mediating disruption of AJs and TJs, leading to gap formation between cells. These pathways in relation to oxidative stress are described next.
1. Regulation of TJs by oxidative stress
Among the TJ proteins, occludins have been well documented to be redox-sensitive proteins. Increased oxidative stress has been related to down-regulation of occludin expression, reduced membrane localization, and reduced tightness of the junctional barrier (229, 261). The C-terminal of occludin contains a coiled-coil (CC)-domain which carries cysteine residues that are essential for oligomerization of occludin by forming disfulfide bonds (280, 433, 434). Masking of free sulfhydryl groups or the presence of DTT prevented occludin dimerization, suggesting the formation of intermolecular disulfide bridges. The dimerization of full-length human occludin can also be prevented by the replacement of its cysteine 409 by alanine in the cytosolic C-terminal CC-domain (433). Oligomerization of occludin is modulated by the ratio of intracellular GSH/GSSG (433). Under physiological conditions, there is a 30- to 100-fold greater GSH than GSSG, thus maintaining a cytosolic reduced state (183, 184). Almost equal number of occludin monomers and oligomers are detected under physiological conditions (433). During inflammation, enhanced oxidative stress can drastically alter the GSH/GSSG ratio toward glutathione GSSG, which prevents oligomeric assembly of occludin. Along this line, inflammation or hypoxia/reoxygenation-induced oxidative stress resulted in reduced occludin oligomerization (279, 281). Mice and rat deficient in SOD1 also have decreased expression of occludin, claudin-5, and ZO-1 correlating with excessive ROS generation (260, 261, 472). These mice exhibited symptoms of amyotrophic lateral sclerosis-linked neurodegeneration (472). Similar to the in vivo studies, compounds such as 2,3-Dimethoxy-1,4-naphthoquinone (DMNQ), which enhance intracellular ROS generation or hypoxia/reoxygenation, were associated with decreased occludin expression and disruption of cadherin-β-catenin complex formation in cultured cerebral endothelial cells (229).
In addition, occludin is regulated by tyrosine phosphorylation in C-terminal region by enhanced oxidative stress. In the mouse model of atherosclerosis, Oxidized-1-palmitoyl-2-arachidonoyl-sn-glycero-3-phosphorylcholine (OxPAPC) reduced the total occludin protein and increased occludin phosphorylation in aortic endothelial, which was associated with enhanced O2
•
2. Regulation of AJs by oxidative stress
The effects of oxidative stress and other inflammatory agonists such as thrombin and VEGF on AJ proteins are mediated by phosphorylation of key serine/tyrosine residues of VE-cadherin, β-catenin, and p120 catenin, which induce junctional disassembly. There are at least five known tyrosines (Y645, Y658, Y685, Y731, and Y733) and one serine residue (S665) in VE-cadherin that are targeted phosphorylation sites for permeability-enhancing agents. Tyrosine phosphorylation of VE-cadherin induces junctional disassembly by preventing interaction with its cytoplasmic binding partners and actin cytoskelton. Phosphorylation of these residues differs according to the inflammatory mediator used. The residues Y645 and Y658 located in the p120-catenin binding site and Y731 and Y733 located in the β-catenin binding site are the targeted phosphorylation sites during leukocyte trafficking (Fig. 10) (7, 418). Allingham et al (7) demonstrated that co-incubation of leukocytes and human endothelial cells enhanced tyrosine phosphorylation of VE-cadherin, specifically on residues Y658 and Y731, which was essential for trans-endothelial migration of leukocytes by inducing junctional opening (Fig. 9). Similar to this study, Turowski et al. (418) demonstrated that lymphocyte trafficking across the endothelial barrier is mediated by phosphorylation of Y645, Y731, and Y733 of VE-cadherin. Point mutations of these residues with phenylalanine suppressed the lymphocyte trafficking across endothelial monolayers by preventing junctional opening (7, 418). The agonist VEGF increased endothelial permeability by phosphorylating VE-cadherin at S665 by p21-activated kinase (PAK) and at Y658 and Y685 by c-Src kinase (130, 299). Phosphorylated S665 residue in VE-cadherin recruited β-arrestin to the site, resulting in clathrin-dependent endocytosis of VE-cadherin and junctional disassembly (130). Phosphorylation of Y685 prevented the binding of c-Src tyrosine kinase (CSK), which is an inhibitor of c-Src activity (30). VEGF-induced phosphorylation of VE-cadherin is dependent on enhanced ROS production and Rac activation in microvascular endothelial cells (299). Inhibitors of ROS generations such as DPI and NAC prevented phosphorylation of VE-cadherin at Y658 (299). In addition, double-point mutants of VE-cadherin Y658F, Y731F, suppressed VEGF-induced vascular permeability (299). In a similar study, van Wetering et al. (427) demonstrated that expression of a constitutively active form of Rac in HUVECs enhanced ROS production by activation of NADPH oxidases, resulting in tyrosine phosphorylation of VE-cadherin and α-catenin, leading to junctional disassembly. Moreover, endothelial junctional disassembly induced by blocking antibodies against extra-cellular domains of VE-cadherin also resulted in Rac activation, enhanced ROS generation, and tyrosine phosphorylation of β-catenin, which was dependent on Pyk2 activation (424). In another study, Tai et al. (407) demonstrated that enhanced ROS production by shear stress in endothelial cells activated PYK2, which can induce junctional disassembly. Similar to VEGF, thrombin is known to increase endothelial permeability by promoting tyrosine phosphorylation of VE-cadherin and associated proteins β-catenin, γ-catenin, and p120-catenin (419).
The low level of tyrosine phosphorylation of VE-cadherin under physiological conditions is regulated by the association with VE-protein tyrosine phosphatases (VE-PTP) that localized at cell–cell adhesion sites (316). Several PTPs, including PTP1B, SHP-2, and density-enhanced phosphatase-1 (DEP1)/CD148, are sensitive to inactivation by enhanced ROS production. The cysteine residue at the catalytic site of classical PTPs is sensitive to oxidation and is the target of specific inhibitors such as pervanadate (91, 287). All of these reports suggest that ROS-mediated activation of tyrosine kinases (c-Src and PYK2) is involved in phosphorylation of junctional proteins, resulting in junctional disassembly.
Independent of tyrosine kinases, oxidative stress during inflammation can also lead to generation of secondary by-products that enhance intracellular ROS generation and affect AJ assembly. One of such a by-product is 4-hydroxy-2-nonenal (4-HNE), which is generated by peroxidation of membrane lipids during inflammation and modifies AJ proteins by forming Michael adducts (421). The levels of 4HNE accumulate certain tissues ranging from 10 μM to 4 nM concentrations. Treatment of bovine lung microvascular endothelial cells to 4-HNE-induced ROS generation modified AJ proteins VE-cadherin and β-catenin by forming 4HNE adducts (Michael adducts) and decreased the transendothelial resistance (421).
3. Regulation of actin cytoskeleton by oxidative stress
The actin cytoskeleton of endothelial cells plays an indispensable role in maintaining endothelial cell morphology, junctional stability, and endothelial motility. According to Ingber et al (186), endothelial cells maintain a state of “tensegrity” in which the centrifugal tension generated by interconnected AJs, microtubules, and focal adhesion resist the centripetal tension generated by actomyosin cytoskeleton. The morphology of the cell, therefore, depends on the force that dominates. Thus, a decrease in the resistive force due to the loss of endothelial junctions results in rounded morphology of endothelial cells.
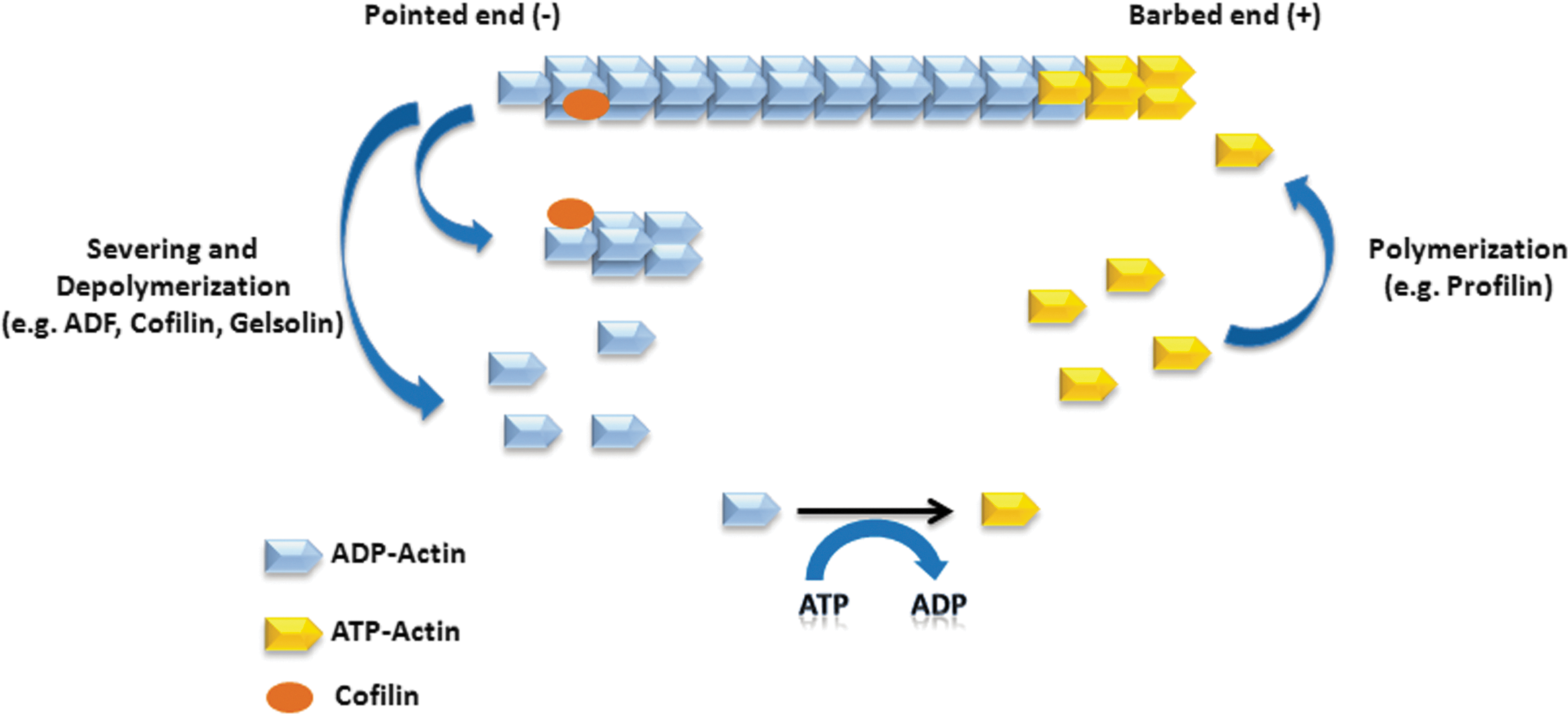
Oxidative stress and inflammatory agonists are well-known inducers of actin cytoskeleton reorganization in endothelial cells, leading to junctional opening and gap formation between endothelial cells. Actin is a 42-kDa protein that can be present either as a free monomeric form known as G-actin or as a part of a linear polymer microfilament called F-actin (Fig. 9). A direct effect of exogenous application of H2O2 on remodeling of actin cytoskeleton of endothelial cells has been documented in several reports. Endothelial monolayer treated with inflammatory agonists such as thrombin, histamine, and VEGF or directly with H2O2 correlated with decreased cortical actin and formation of polymerized F-actin (61, 182). Reorganization of actin ctyoskelton into F-actin increased centripetal tension and induced gap formation in endothelial cells (103, 349, 397).
Oxidative stress can affect actin cytoskeleton reorganization in two different ways: (i) a direct effect on actin cytoskeleton or actin regulatory proteins by oxidative modification and (ii) indirectly by influencing the signaling networks intrinsic to endothelial cells affecting polymerization of actin cytoskeleton. Both pathways are influenced by inflammatory agonists and oxidative stress. Oxidation of actin monomers (G-actin) by H2O2 alters its polymerization ability as well as its interaction with actin regulatory proteins filamin and α-actinin (77). H2O2 is known to induce actin polymerization at doses ranging from 0.2 to 5 mM with an effective dose (ED50) at 1 mM H2O2 (198, 324, 411). The cysteine and methionine residues in G-actin are particularly susceptible to oxidation. Exposure of G-actin to tert-butyl hydroperoxide (t-BH) in 1–20 mM concentration induced oxidation of Cys-374 of G-actin and altered the kinetics of actin polymerization (78), while treatment with H2O2 induced oxidation of Cys374 as well as Met44, Met47, Met176, Met190, Met269, and Met35 of actin monomers. Of all the residues studied, Cys-374 was the earliest target of H2O2-induced oxidation (291). The oxidative modification of these residues alters conformations of subdomain 1 (which regulates binding to actin-binding proteins) and subdomain 2 (regulates polymerization of actin filament) of actin (291). Interestingly, treatment with H2O2 did not increase actin polymerization at the barbed ends; however, it enhanced polymerization at the pointed end (Fig. 10) (297, 324). Inhibitors of ROS generation DPI or SOD mimetic (MnTmPyP) decreased the number of exposed barbed ends and reduced actin polymerization (297).
In addition, oxidative stress can influence cytoskeletal dynamics by direct modification of actin and actin-associated regulatory proteins through phosphorylation, nitration, carbonylation, disulfide formation, and glutathionylation (108, 109). s-glutathionylation of actin, in particular, has been detected in cells exposed to oxidative stress (59, 76, 123, 362). Moreover, actin was found to be the most abundant s-glutathionylated protein in PMNs and platelets in response to exposure to oxidants (59, 76). Actin-associated regulatory proteins affected by oxidative stress include cofilins, gelsolin, and filamin (Fig. 9). Cofilins or actin depolymerizing factor (AC/ADF) is a class of small (13–19 kDa) actin-binding proteins that regulates actin turnover in the cells through depolymerization of actin filaments. Cofilins exist in cells as both monomers and oligomers. The monomers exhibited the known severing activity, whereas the oligomers exhibited reduced severing activity but increased actin bundling activity (347). The transition from monomers to oligomers was regulated by reversible intermolecular disulfide bond formation between Cys39 and Cys147 of two adjacent cofilin units (347). Gelsolin regulated actin turnover in the cells by severing the barbed ends and capping actin filaments. Gelsolin is an unusual actin-binding protein that functions in two different redox environments. Plasma gelsolin functions in a Ca2+-rich, oxidizing environment and regulates the actin scavenger system of the blood. In contrast, cytoplasmic gelsolin works in Ca2+-poor, reducing environment of the cytoplasm (448). Under basal conditions, plasma gelsolin contains a disulfide bond between cysteines 215 and 228. This alters its sensitivity to calcium and the rate of severing F-actin, which includes binding to actin monomers and nucleation of actin polymerization (6, 448). Enhanced oxidative stress induced by Rac activation resulted in dissociation of gelsolin from actin filaments, exposing more barbed ends for actin polymerization (13, 167). Filamin is a 280 kDa actin-binding protein that plays a significant role in connecting F-actin with plasma membrane glycoproteins. In resting endothelial cells, filamin is constitutively phosphorylated by PKA, which protects it against calpain-mediated proteolysis. Treatment of HUVECs with 100 μM of H2O2 caused dephosphorylation of filamin by inhibiting PKA activity. This subsequently induced translocation of filamin from the membrane to the cytosol within 1 min and was accompanied by gap formation, which was attributed to rearrangement of the dense peripheral band of F-actin (168, 169). The translocation of filamin was inhibited by antioxidants such as TEMPO (nonspecific free radical scavenger) and Deferoxamine (iron chelator) (168). Altogether, enhanced intracellular oxidative stress is the major inducer of actin stress fiber formation, leading to junctional disassembly and gap formation between endothelial cells.
V. Signaling Mechanisms of Endothelial Barrier Disruption by Oxidative Stress
A. Altered intracellular Ca2+ regulation
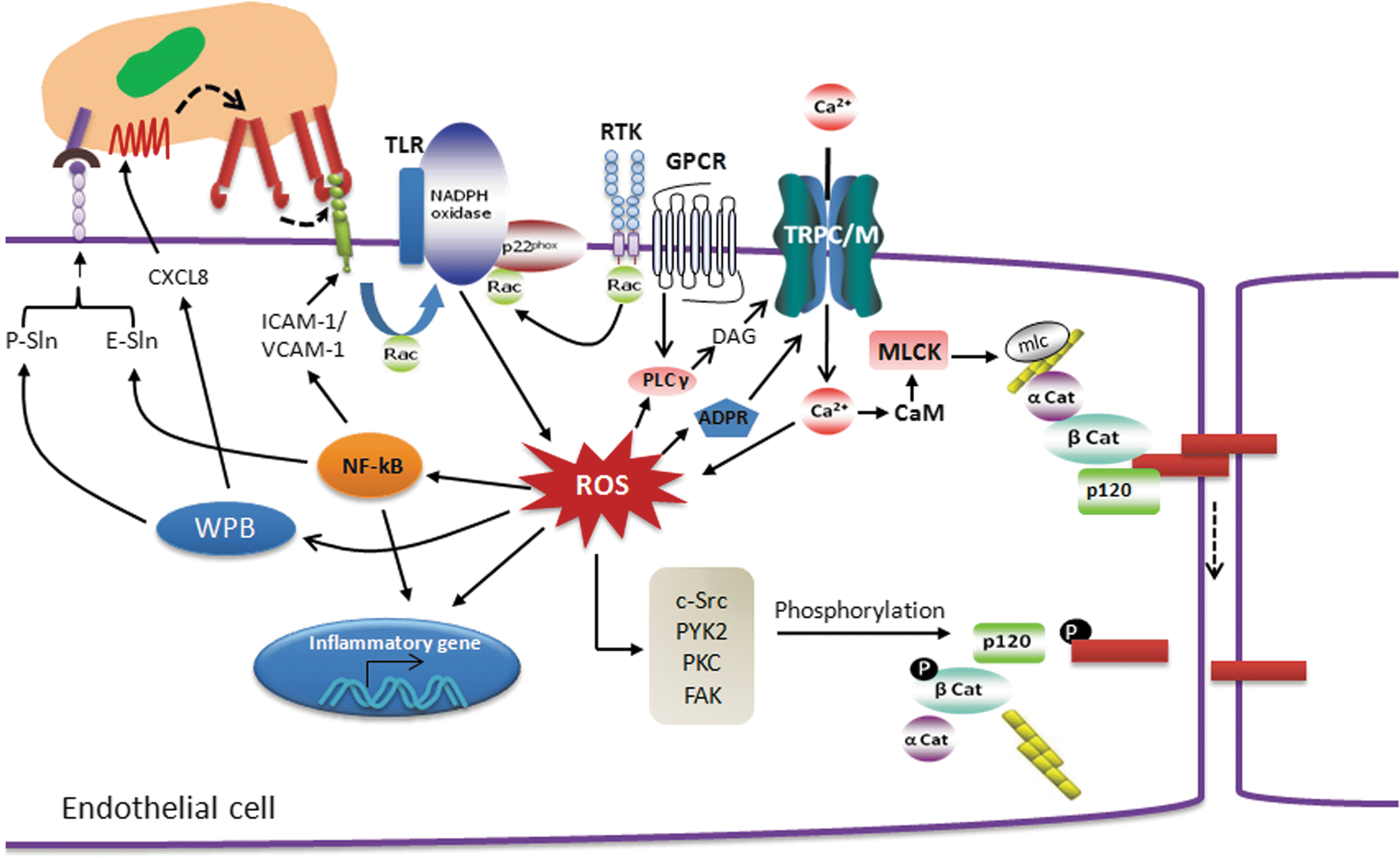
Endothelial barrier integrity is formed by tight cell–cell and cell–matrix adhesions, and it is coupled to cytosolic Ca2+ levels (284). Increases in [Ca2+]i induced formation of inter-endothelial cell gaps and vascular hyperpermeability through different signaling pathways (Fig. 10) (256, 264, 371). Several reports suggest that an increase in [Ca2+]i leads to activation of Ca2+/calmodulin-dependent myosin light chain kinase (MLCK), which facilitates reorganization of actin cytoskeleton to induce changes in endothelial cell shape. Increasing cytosolic Ca2+ by thapsigargin (which depletes ER Ca2+ store) and calcium ionophore increased permeability in an HUVEC-derived cell line ECV304 (103, 127). Interestingly, thapsigargin induced activation of PKC-α, and phosphorylation of VE-cadherin-associated proteins was prevented by PKC inhibitor, calphostin C. These findings suggest that activation of PKC-α is critical in Ca2+-mediated increase in endothelial permeability (370, 371). An increase in [Ca2+]i has also been associated with activation of small GTPase RhoA. The inflammatory mediator such as thrombin is known to induce receptor-mediated Ca2+ entry followed by RhoA activation, thereby resulting in increased endothelial permeability (390).
In addition, evidence indicates that ROS activates Ca2+ signaling and influences different cellular events which trigger inflammation. Chelation of extracellular Ca2+ by BAPTA suppressed H2O2 formation (312). An increase in intracellular Ca2+ was associated with enhanced H2O2 generation (101). The converse is also true. H2O2 caused a dose-dependent rise in [Ca2+]i of endothelial cells (172). ROS-mediated regulation of intracellular free Ca2+ concentration is a major mechanism of increased vascular permeability, the hallmark of inflammation. However, to date, little is known about the mechanism of ROS-induced Ca2+ entry in endothelial cells and how this relationship promotes the loss of endothelial barrier integrity.
The principal Ca2+ entry pathway in endothelial cells is via store-operated calcium (SOC) channels and receptor-operated calcium (ROC) channels. Since transient receptor potential (TRP) channels are believed to underlie the molecular makeup of many ROC channels (TRPC3, 6 and 7) and at least some SOC channels (TRPC1 and 4) (333), it is logical to presume that TRPC proteins are sensitive to regulation by ROS. TRPC7 (also known as transient receptor potential melastatin 2 (TRPM2), TRPC6, and TRPC3/TRPC4 have been shown to be regulated by ROS in the endothelium (156, 408). In one study, Balzer et al. (22) provided strong evidence for a central role of TRP channels in oxidant-induced vascular pathophysiology. They showed that expression of a dominant negative fragment of TRPC3 suppressed oxidant-induced membrane currents in endothelial cells. To further analyze the role of TRPC3 as a redox sensor, Poteser et al. (353) stably transfected HEK293 cells with TRPC3, and these cell types displayed a large increase in membrane conductance in response to cholesterol oxidase. Generation of redox cation conductance by over-expression of TRPC3 suggests that TRPC3 is an important redox-sensitive cation channel. Using immunoprecipitation and Forster Resonance Energy Transfer (FRET), it was shown that TRPC4 interacts with TRPC3 to form heteromers, representing a potential redox-sensitive channel complex. The requirement of TRPC3/C4 heteromerization to serve as a sensor for cellular redox state was further evident by the finding that redox-activated TRPC3 cation conductance was inhibited by expression of dominant negative mutants of TRPC4 (353).
Recent studies have demonstrated that TRPC6 also represents a target of ROS in different disease models (98, 443, 446). Using lung ischemia–reperfusion edema (LIRE) model, Weissmann et al. (446) elegantly showed that NOX2-mediated O2 •− activates TRPC6 and thereby induces Ca2+ influx in endothelial cells. They also found that NOX2−/− and TRPC6−/− mice were equally protected against ischemia-induced lung injury. Thus, TRPC6 also represents a target for ROS in different pathophysiological conditions.
TRPM2, of the melastatin subfamily, originally named TRPC7 (307), is no longer considered a member of the TRPC subfamily. The TRPM subfamily only exhibits limited homology to the other TRP family ion channels, and functional channels comprising members of this subfamily are believed to be homotetramers (277). CTD of TRPM2 share 39% sequence identity to the human nucleoside diphosphate-linked moiety X-type motif 9 (NUDT9) ADPR pyrophosphatase (173, 343, 372, 386) Despite significant homology with NUDT9 ADP pyrophosphate, TRPM2 has low levels of ADP-ribose (ADPR) pyrophosphatase activity (343, 372). Intracellular application of ADPR, the substrate of the NUDT9 enzyme, specifically induced TRPM2 gating (343). A further mode of TRPM2 activation is through oxidative stress (164, 392, 445). Different mechanisms have been proposed for H2O2-mediated TRPM2 gating. Perradud et al. (344) showed that oxidative stress activates production of ADP-ribose in mitochondria, which are then released to the cytosol and function as a second messenger to stimulate TRPM2 gating. In contrast, Hara et al. (164) demonstrated that TRPM2 is a Ca2+-permeable cation channel and can be activated by H2O2 via action of NAD+. Direct oxidation of TRPM2 by H2O2 has also been reported as a mechanism of activation of the channel (445).
Hecquet et al. (171) showed that H2O2 induced TRPM2-like cation current that was increased by over-expression of TRPM2 and by 3-deaza-cADP ribose but inhibited by a specific TRPM2 small interfering RNA and by PARP inhibitors in human pulmonary artery endothelial cells (Fig. 11). These data clearly favor an indirect mechanism of activation of TRPM2 channels by H2O2 via the formation of ADPR. Using Ca2+ add-back protocol designed to rule out indirect effects of H2O2 on Ca2+ entry via Ca2+ store depletion, Hecquet et al. also showed that H2O2 increased intracellular Ca2+ by stimulating Ca2+ entry without provoking Ca2+ store depletion. More importantly, this study showed the importance of TRPM2 in mediating the H2O2-induced increase in endothelial permeability, which could be prevented partly by application of TRPM2 small interfering RNA and TRPM2-specific antibody (171). The short variant of TRPM2, which lacks the pore domain and acts as a dominant-negative form by inhibiting the formation of functional homotetrameric channels, also significantly reduced H2O2-mediated microvascular hyper-permeability (171). In another article, Di et al. (95) addressed the role of TRPM2 in phagocytic cells and showed a protective role for TRPM2 in LPS-induced lung inflammation. This involved the influx of cations via TRPM2, which prevented membrane depolarization induced by transfer of electrons from NADPH to NADPH oxidase. Therefore, the net effect of TRPM2 activation was to reduce the production of ROS, which, in turn, modulated the lung inflammatory response to E. coli.
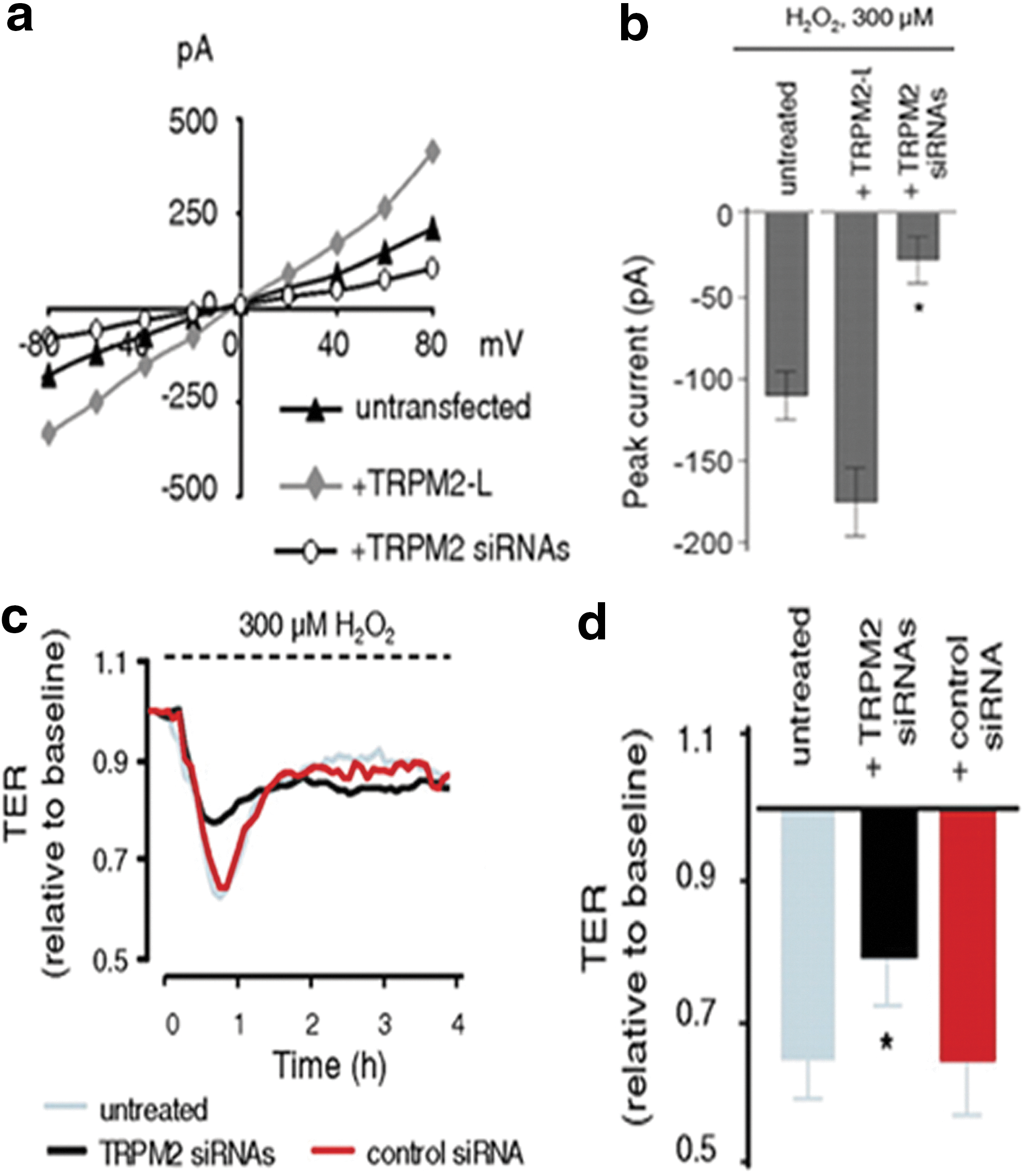
B. Myosin light chain kinase
Endothelial cells contain contractile machinery, which includes actin and myosin. Phosphorylation of regulatory myosin light chain (MLC) leads to activation of the endothelial contractile elements and disrupts endothelial barrier function. (127). Permeability increasing mediators such as thrombin, histamine, and H2O2 enhance MLC phosphorylation, which precedes the onset of endothelial contraction (Fig. 10) (303, 387, 470). The myosin phosphorylation in the endothelial cells is regulated by two enzymes: nonmuscle MLCK and myosin-associated protein phosphatase. Activated MLCK directly phosphorylates MLC at Thr-18 and Ser-19 site, which induced isometric tension development and actin polymerization in endothelial cells (136). Zhao et al. (470) reported that H2O2 also induced MLC phosphorylation in endothelial cells. Though the inhibition of MLCK blocked H2O2-induced MLC phosphorylation, yet it did not affect H2O2-induced actin and myosin assembly. Therefore, MLC phosphorylation does not appear to regulate H2O2-induced actin and myosin assembly but may play a role in induced actin rearrangement. The role of MLCK was also studied in hyperoxia-induced lung injury model (422). This study demonstrated that NADPH oxidase-mediated ROS generation during hyperoxia was inhibited by silencing nmMLCK in lung endothelial cells. In addition, nmMLCK
Depletion of MLCK by using siRNA was also shown to reduce LPS-induced phosphorylation of mono and diphospho-MLC and restored barrier function (43). Inflammatory mediators are known to inactivate myosin-associated phosphatases, which further promoted MLC phosphorylation (111, 112). Phosphorylation of MLC phosphatase subunit (MYPT1) was increased by ROS followed by cell contraction (199). Taken together, ROS-mediated activation of MLC kinase contributes to actin reorganization in endothelial cells.
C. The Ras superfamily of GTPases
The Ras family of small GTP-binding proteins are activated by a variety of agonists, growth factors, TNF-α, G-proteins, and ROS and regulate a wide range of biological processes, including reorganization of the actin cytoskeleton, co-ordinated migration, proliferation, tumorigenesis, and cell barrier functions (2, 32, 147). This small GTPases superfamily is subdivided into five subfamilies: Rho, Ras, Rab, Ran, and Arf (394). These proteins act as switches by cycling between active (GTP-bound) and inactive (GDP-bound) conformations. The activation state of these small molecules is regulated by: GEFs, which promote exchange of GTP for GDP; GTPase-activating proteins (GAPs), which inactivate G proteins by enhancing the GTP-hydrolysis; and guanine-nucleotide-dissociation inhibitors, which bind to GDP-bound small proteins and regulate translocation between membranes and the cytosol (394). The active form of these small molecules interacts with their downstream targets and mediates their biological functions.
The mammalian Rho GTPase family consists of more than 20 distinct members, while the Ras family has 36 members. In this section, we focus on the regulation of endothelial barrier functions by the best-characterized members of RhoGTPase family: RhoA, Rac1, and CDC42 and Ras family GTPase Rap1 (449). RhoA activation downstream of several endothelial permeability-increasing mediators causes loss of endothelial junctions by enhancing actomyosin contractility and increasing isometric tension at the cell margins (426). However, Rac1 and Cdc42 are required for the assembly and maturation of endothelial junctions, and their activity increases during junction formation (144, 226, 234, 449). In contrast, other studies showed that activation of Rac1 downstream of VEGF and other growth factors increased endothelial permeability (226, 234). This points to the notion that an optimal level of Rac activity is required to maintain the stability of endothelial junctions and either inhibition or hyper-activation can disrupt the AJs.
Sundaresan et al. (400) showed that activated Rac1 increased the ROS generation in fibroblasts. This was further confirmed by multiple reports in response to different stimuli in endothelial cells (92, 463). Over-expression of active Rac1 induced tyrosine phosphorylation of VE-cadherin and increased endothelial permeability in an ROS-dependent manner (427). Contrary to this, active RhoA induced pronounced stress fiber formation but did not induce loss of cell–cell adhesion, indicating that Rac-mediated ROS generation was specifically involved in loss of cell–cell adhesion (427).
The role of RhoA family GTPases has also been investigated in endothelial cells under hypoxic condition. Rac1 and RhoA oppose each other during changes in oxygen tension. In addition, expression of dominant negative Rac1 (N17Rac1) strongly inhibited RhoA and NADPH oxidase activity, suggesting that Rac1 acted upstream of RhoA during hypoxia/reoxygenation stress (427, 455). Interestingly, there are also other mechanisms through which ROS can directly affect RhoA activity and RhoA-mediated cytoskeletal rearrangement. Campbell et al. (176) found that the treatment of purified recombinant GTPase with superoxide in vitro resulted in guanine nucleotide dissociation. Furthermore, using cysteine to alanine mutants, Aghajanian et al. (2) demonstrated that ROS-mediated activation of RhoA was dependent on cysteines 16 and 20.
It has been known for several years that Cdc42 activation is required to maintain endothelial barrier function. Barrier-stabilizing effect of oxidized phospholipids was blocked by siRNA targeting Cdc42 (38), and expression of constitutively active Cdc42 abolished LPS-induced lung vascular permeability in vivo (357). These studies suggest an obligatory role of Cdc42 for barrier maintenance. Although there is little information regarding the direct effects of ROS on Cdc42 function, studies showed the involvement of Cdc42 in ethanol-induced NOX activation and ROS generation and subsequently, reorganization of actin filaments in endothelial cells (437). Further studies are needed to fully understand the mechanisms by which this important modulator of the cell cytoskeleton regulates endothelial barrier function under oxidant stress conditions.
D. PKCs
The PKC isoforms are divided into three subclasses according to their structure, activation, and substrate requirements. The calcium-dependent conventional or classical PKC isoforms (α, β1/2, and γ) are regulated by diacylglycerol (DAG) or phosphatidylserine (PS), whereas the novel PKCs are Ca2+ independent (δ, ε, η, θ, and μ) and activated by DAG or PS. The atypical PKCs (ζ, λ) are regulated by PS and are independent of DAG and Ca2+ (250, 334). The PKC activity is regulated by its translocation to the membrane and phosphorylation and generally denotes enzyme activation (334). PKC is the target for multiple tyrosine phosphorylations by various tyrosine kinases, including Src family kinases (304, 396). These modifications further increase kinase activity of PKC (243). Several PKC inhibitors such as staurosporine, H7, calphostin C, bisindolylmaleimide, and chelerytherine inhibited endothelial hyper-permeability in response to different pro-inflammatory agents (133, 200, 341, 358, 460). A number of studies have demonstrated that membrane translocation and activation of the atypical isoforms of PKCζ is required in thrombin-mediated increase in endothelial permeability (244, 294). Depletion of PKCζ by siRNA or overexpression of dominant negative mutants of PKCζ abolished thrombin-induced hyper-permeability by inhibiting phosphorylation of MLC and activation of RhoA (294). In agreement with these findings, PKC-α was shown to induce phosphorylation of p120-catenin in response to thrombin or LPS, which reduced p120-catenin binding affinity for VE-cadherin and subsequently disrupted endothelial junction integrity (429). TNF-α-mediated endothelial barrier dysfunction was shown to be dependent on an increase in PKC-α activity. Furthermore, the antisense of PKC-α reduced the TNF-α-induced increase in endothelial permeability (120). Other studies have reported that VEGF can increase vascular permeability through activation of PKC-β in vivo and, importantly, oral administration of PKC β-isoform-selective inhibitors partially inhibited VEGF-induced vascular permeability (4). Moreover, Titchenell et al. (414) have shown that pseudo-substrate peptide inhibitors of atypical PKC isoform such as aPKC-I-PD and aPKC-I-diCl can inhibit VEGF-induced endothelial permeability. These studies support a prominent role of different PKC isoforms in microvascular leakage associated with different pro-inflammatory mediators. Increased PKC activity has also been associated with various vascular disorders such as atherosclerosis, hypoxia, and ischemia reperfusion (138, 174, 286, 447).
In the endothelium, H2O2 is also known to activate multiple PKC isoforms (224, 225). There are different mechanisms through which ROS can activate PKC. All PKC isoforms contain redox-sensitive cysteine residues in both regulatory and catalytic domains, which are required for autoinhibition and catalytic activity, respectively. Direct oxidative modification of the regulatory domain results in increased PKC activity (143). ROS can also regulate PKC activation by generating different mediators and cofactors, including PLC and PLD (267, 438). Oxidant-mediated activation of PKC also occurred through phosphorylation of distinct residues of different PKC isoforms (224). Several lines of evidence suggest that PKC is likely to play a permissive role in H2O2-mediated endothelial permeability and lung edema (200, 389, 470). Johnson et al. (200) showed that H2O2-induced lung edema and stress fiber formation in ECs were inhibited by protein kinase blocker H-7. Another study demonstrated that the selective inhibition of PKC by calphostin C abolished H2O2-mediated myosin light-chain phosphorylation in ECs (470). Taher et al. (406) demonstrated H2O2-inducing translocation of PKC from cytosol to membrane and increased membrane-associated PKC activity. Thus, PKCs act as a key mediator of inflammation and microvascular hyper-permeability under stimulated conditions.
E. Toll-like receptors
TLRs are a subset of pathogen-associated pattern recognition receptors family that are classified on the basis of homology to the cytoplasmic domain of the interleukin-1 receptor (IL-1R) family, also known as the Toll/IL-1R (TIR) domain (391). A total of 10 and 14 TLRs have been identified in human and mouse, respectively (63, 405). TLRs are expressed in a wide range of immune cells, including DCs, macrophages, PMNs, and certain nonimmune cells such as endothelial and epithelial cells (28, 220). Among all members, TLR4 is the most widely characterized and well-established receptor for LPS signaling. LPS-binding protein recognizes the lipid-A moiety of LPS and brings LPS to the cell surface to form a ternary complex with CD14, which facilitates the transfer of LPS to TLR4 and MD-2 (306). This complex then initiates intracellular signals through two adaptor proteins, TRIF and myD88, which recruit multiple cytoplasmic signaling molecules TRAF6, TIRAP and the kinases RICK and IRAK, and activates downstream signaling components involving JNK, p38, and NF-κB (84). A number of studies showed that LPS-TLR4 axis is involved in endothelial barrier disruption by different pathways. LPS-mediated TLR4 activation induced tyrosine phosphorylation of junctional proteins, including VE-cadherin, p120-catenin, and γ-catenin through activation of Src family kinases to open the endothelial paracellular pathway (139). Liu et al. (248) showed that LPS/TLR4 signaling activated Src family kinases by enhancing the interaction of TRAF6 with cSrc and Fyn and promoting transendothelial albumin flux. In another study, Wang et al. (442) reported a direct role of p120-catenin in the regulation of LPS-mediated increase in endothelial permeability. They showed that the inhibition of p120-catenin expression in endothelial cells increased MyD88 and TLR4 association, ICAM-1 expression and enhanced the severity of LPS-induced lung inflammation.
Increasing evidence suggests that enhanced ROS generation is central in the activation of TLR-mediated signaling pathways. Ryan et al. (365) showed that ROS are involved in LPS/TLR4-mediated IL-8 signaling. Antioxidant treatment decreased LPS-induced nuclear translocation of NF-κB as well as IL-8 production in human monocytes. Park et al. (336) have proposed a direct mechanism through which TLR4 regulates ROS formation. They demonstrated that TLR4 interacted with the COOH-terminal region of NOX4 in HEK293 cells, and knockdown of NOX4 inhibited LPS-mediated NF-κB activation (335). NOX4 was also shown to be required for LPS-induced ROS generation and NF-κB activation in endothelial cells (335). Knockdown of NOX4 significantly inhibited LPS-induced MCP1 production, ICAM-1 expression, and adhesion of monocytes to endothelial cells (335). TLR4 also induced TLR2 expression in human endothelial cells in an NF-κB-dependent manner (119). A unique mechanism of cross-talk between TLR4/TLR2 has been proposed; that is, the role of PMN NADPH oxidase complex in mediating the cross-talk between TLR4 and TLR2 (116). Impairment of PMN NADPH oxidase markedly decreased the LPS-induced NF-κB activation and TLR2 up-regulation in endothelial cells (116). In addition, LPS did not up-regulate the TLR2 expression in TLR4 knockout mice, indicating that PMN NADPH oxidase mediates TLR2 up-regulation in endothelial cells and is an important mechanism that is responsible for amplifying PMN transmigration to the site of infection (118).
VI. Oxidative Stress and Tissue Injury
Accumulation of activated macrophages at the site of injury is the characteristic feature of chronic inflammatory diseases (236). Macrophages are evolutionary “designed” to eliminate pathogens by producing excessive oxidative stress, which, if excessive and unchecked, can lead to tissue damage. However, the current literature has shown that macrophages after undergoing a phenotypic shift also help in tissue repair. According to current classification, there are two distinct populations of macrophages: M1 or classically activated macrophages, which contribute to tissue injury by releasing large quantities of highly reactive cytotoxic oxidants to destroy pathogens and M2 or alternatively activated macrophages, which suppress inflammation and help in wound resolution by phagocytizing dead neutrophils and synthesizing molecules that are responsible for tissue remodeling such as TGFβ, VEGF, and EGF (236, 302). Both classes of macrophages have a distinct cytokine profile that distinguish their behavior; M1 macrophages produce excessive oxidative stress and secrete pro-inflammatory cytokines TNFα, IL-1, and IL-6, whereas M2 macrophages secrete anti-inflammatory cytokines IL-4, IL-10, and IL-13 (236). The classically activated macrophages induce tissue injury by releasing chemokines and reactive oxidants that induce cell death by activation of cell death receptors, culminating in caspase activation via either an extrinsic pathway (i.e., mitochondria independent) or an intrinsic pathway (i.e., mitochondrial dependent) (64). In addition, oxidative stress produced by macrophages can induce cell death through creating an imbalance in antioxidant GSH equilibrium (64). Activation of caspases appears to be central to most of the pathways of cell death.
A. Extrinsic pathways of cell death and regulation by ROS
The extrinsic pathway of cell death is mediated by cell death receptors, which after binding with their ligands initiate protein–protein interactions, resulting in activation of the initiator caspases. There are four major cell death receptors, including TNF receptor 1 (TNFR1), TNF-related apoptosis-inducing ligand receptor 1 (TRAIL-R1), TRAIL receptor 2 (TRAIL-R2), and Fas receptor. The ligands that bind to these receptors belong to TNF superfamily of cytokines TNFα, Fas ligand, and TRAIL (64). TNF-α-induced cell death has been attributed to excessive ROS generation-sustained JNK activation and caspase activation (Fig. 12) (90, 369, 457). TNF-α is a principal plieotropic cytokine that is secreted by activated macrophges which possesses a variety of biological properties such as production of inflammatory cytokines, cell proliferation, and cell death. It was first defined by William Coley in his findings that cancer patients have necrotic tumors when they developed bacterial infections and was formally referred to as Coley's toxins (452). The active component inducing cell death in tumors was later identified as a cytokine secreted by macrophages and hence, termed tumor necrosis factor (68). TNFR1 signaling under resting conditions is inhibited by association with a 60-kD cytoplasmic protein known as silencer of death domains (SODD). Within minutes of TNFR1 activation by TNF-α, this auto-inhibition is released, the adaptor proteins TNFR1-associated death domain (TRADD) and Fas-associated death domain (FADD) are recruited, and the collective death-inducing signaling complex (DISC) is internalized. Release of endosomal DISC to the cytosol further recruits initiator procaspase-8, resulting in its activation (64). Similar to TNFR1, the apoptosis induced by FasR has been attributed to enhanced ROS generation via NADPH oxidases and caspase activation. The apoptosis induced by FasR likewise depends on the recruitment of FADD and pro-caspase-8 activation. A key feature of FasR-mediated apoptosis is regulation by FLICE inhibitory protein (FLIP), which inhibits apoptosis by preventing the binding of procaspase-8 to FADD (189). The enhanced ROS generation down-regulates FLIP protein and executes FasR-dependent apoptosis (436). The extent of caspase-8 activation is an essential determinant of cells undergoing mitochondrial independent or dependent apoptosis (377). Extensive caspase-8 activation directly activated effector caspases such as caspase-3 and induced cell death, whereas low caspase-8 activation activated an amplification loop that was dependent on the mitochondria (described in the next section).
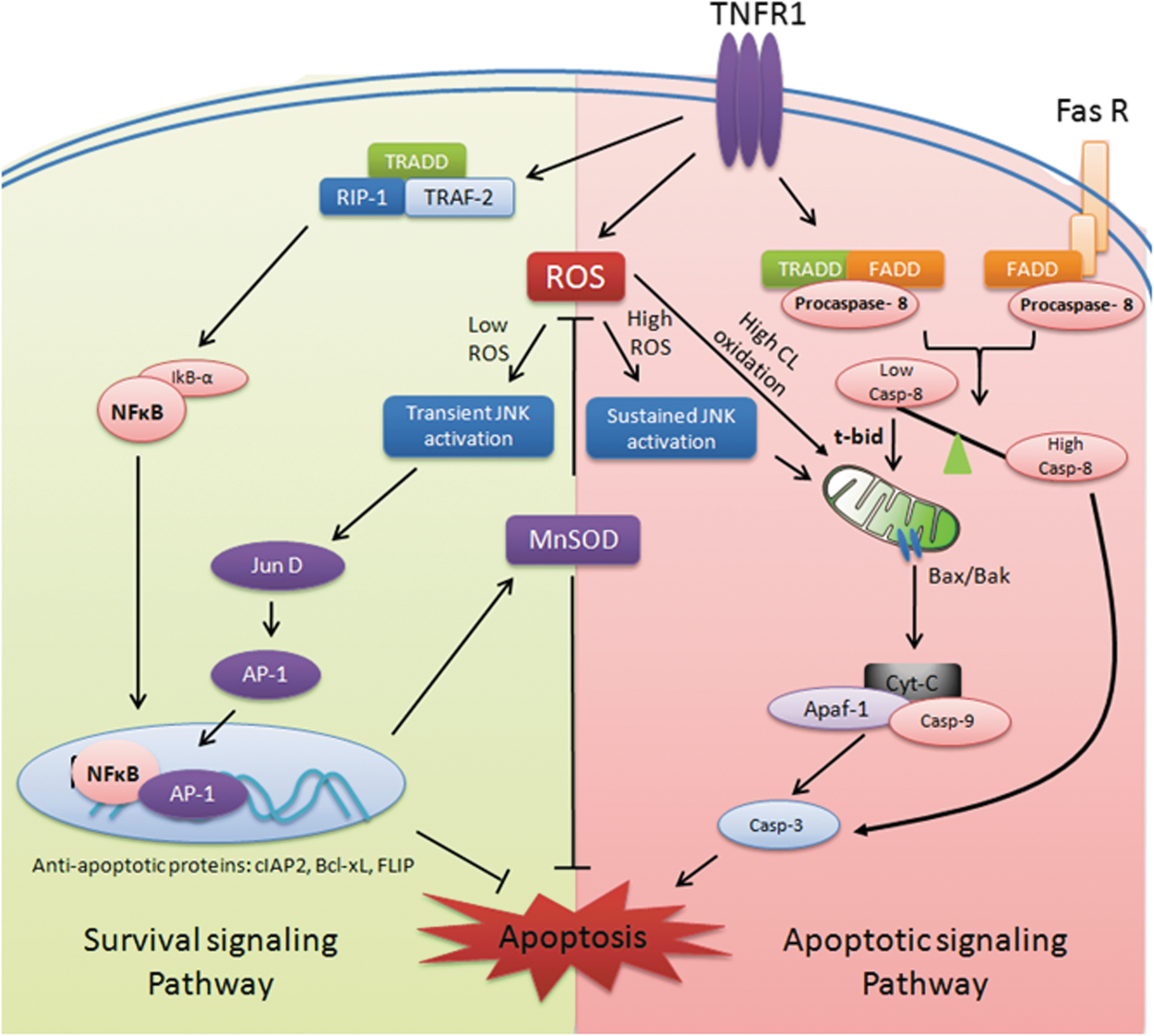
However, TNF-α does not always induce apoptosis in all cells, because it can alternatively activate at least two cell survival pathways (Fig. 12). TNF-α activates NF-κB by recruiting TNFα-receptor-associated factor 2 (TRAF2) and receptor-interacting kinase 1 (RIP1), which has pro-survival effects by induction of anti-apoptotic proteins (e.g., anti-apoptotic proteins of Bcl2 family and caspase inhibitors) and suppressed TNF-α induced ROS generation by enhancing expression of MnSOD (205, 369). Further, TNF-α mediated an early and transient activation of JNK/Jun, which contributed to cell survival in conjunction with NF-κB by activation of the AP-1 transcription factor (232). In the absence of NF-κB, a massive accumulation of H2O2 leads to prolonged activation of JNK kinase, which induced cell death (90, 205, 369).
Although caspase activation and enhanced ROS generation are central to the mechanism of apoptosis, there are reports suggesting no significant role of ROS in the progression of apoptosis and showing that reduced ROS generation is, in fact, the cause of apoptosis (15, 122). This is surprising, as the efficacy of pharmacological antioxidants such as GSH, NAC, deferoxamine (283, 420, 425), and antioxidant enzymes such as catalase or GPx (149, 283) in preventing apoptosis have been shown by several groups. Other studies, however, were unable to demonstrate any role of antioxidants in preventing apoptosis (15, 66, 122). These differences may be ascribed to the use of different cell types, different methods of measuring ROS, and the particular antioxidants tested. In addition, plasma membrane permeability of different cell types to antioxidant enzymes can greatly influence the analysis.
B. Intrinsic pathways of cell death and regulation by ROS
The intrinsic pathways of cell death are dependent on increased mitochondrial outer membrane permeability (MOMP), which causes mitochondria-to-cytosol release of apoptogenic proteins such as Cytochrome-c (Cyt-c), Smac/Diablo, apoptosis-inducing factor (AIF), and endonuclease G, which trigger cell death in either a caspase-dependent or -independent manner (Fig. 12) (151, 230). This phenomenon of increased MOMP can be induced by excessive calcium entry, high oxidative stress, and compounds, which result in mitochondrial membrane depolarization (417). The released Cyt-c then binds to apoptosis activation factor-1 (Apaf-1) and recruits initiator pro-caspase 9, which undergoes auto-activation. This whole complex is collectively known as “apoptosome” (151) (Fig. 12). Caspase-9 then activated the effector caspases such as caspase-3. Smac/Diablo also facilitates the activation of effector caspases by removing the blockage by inhibitor of apoptosis proteins (IAPs) (417). AIF, on activation, induced DNA condensation and cleavage (50). EndoG-mediated DNA fragmentation is the final event in the apoptosis. The mitochondrial release of Cyt-c is considered the major determinant of cell death.
The pro-apoptotic member of Bcl-2 family such as Bid (BH3 interacting-domain death agonist) can enhance MOMP by cleavage with caspase-8. The truncated bid after caspases cleavage then induces oligomerization of pro-apoptotic proteins Bax/Bak, which then integrated in the outer mitochondrial membrane and triggered Cyt-c release (342). However, recombinant oligomeric Bax protein alone contributed only 18% of Cyt-c release from brain mitochondria (342). When combined together, recombinant Bax and complex I inhibitors (which is known to induce oxidative stress) induced approximately 65% of the mitochondrial Cyt-c release (342), indicating that oxidative stress is the major trigger in Cyt-c release from mitochondria. The release of Cyt-c further enhanced ROS generation from mitochondria because of uncoupling of ETC. An anionic phospholipid specific to mitochondria known as cardiolipin (CL) helps in anchoring of Cyt-c to the inner mitochondrial membrane. Enhanced oxidative stress leads to oxidation of CL, which decreases the affinity binding with Cyt-c (218, 388). A growing number of reports have strongly implicated the role of oxidized CL in Cyt-c release (64, 203, 309, 327). The content of oxidized CL was increased in mitochondria isolated from ischemic myocardium, which potentially contributed to the ischemia/reperfusion injury (345). However, the mechanism of oxidized CL-mediated Cyt-c release is not yet clear. According to Gonzalvez et al. (141, 142), oxidized CL is translocated to the outer mitochondrial membrane provided a docking site for tBid, enabling mitochondrial outer membrane permeabilization and Cyt-c movement. However, contradictory reports indicate that oxidized CL does not play a role in Bax-mediated pore formation (194, 195). Interestingly, Kagan et al. showed that a pool of CL-bound mitochondrial Cyt-c functions as a peroxidase that catalyzes peroxidation of CL (204). The peroxidase activity of Cyt-c can be stimulated at a lower H2O2 concentration when bound to CL-containing membranes compared with unbound (35), suggesting that increased oxidative stress can enhance the peroxidase activity of Cyt-c, enabling CL peroxidation and execution of cell death.
Independent of apoptosis by Bcl-2 family members, the mitochondrial permeability transition (MPT) induced by the opening of mitochondrial permeability transition pore (mPTP) can also lead to cell death. Unlike MOMP, mPTP enhances permeability of inner mitochondrial membrane and is independent of Cyt-c release. The opening of the mPTP causes mitochondrial swelling due to massive influx of solute and water, resulting in mitochondrial depolarization and cessation of ATP synthesis (215). mPTP is the underlying event in primary necrosis. However, apoptotic cells can undergo secondary necrosis if their removal is delayed. In contrast to primary necrosis, mitochondrial depolarization in secondary necrosis can be coincident or followed by Cyt-c release. mPTP is a megapore spanning the inner and outer mitochondrial membranes, which is hypothesized to consist of at least three components (72): outer membrane channel known as VDAC, inner membrane channel known as adenine-nucleotide translocase (ANT), and cyclophilin-D (CypD) present in mitochondrial matrix. CypD, although present in the mitochondrial matrix, becomes associated with the inner mitochondrial membrane during the MPT (72, 160). Although MOMP and mPTP appear to be distinct pathways, a cross-talk has been reported between them. Mice deficient in Bax/Bak render cells resistant to mPTP opening and necrosis (451). Superoxide-induced mitochondrial Cyt-c release in HepG2 cells depends on VDAC, and blockers of VDAC inhibited the release (259). ANT and cyclophilin D are also targets of oxidative stress, and their oxidative modification has been implicated in an increase in mitochondrial permeability and Cyt-c release (20, 135). Mice deficient in CypD were protected from ischemia/reperfusion-induced cell death in vivo and primary hepatocytes and fibroblasts isolated from CypD null mice were protected from Ca2+ overload and oxidative stress-induced cell death (20). Therefore, it seems that there is an intricate relationship between these two pathways which is likely modulated by oxidative stress during inflammation.
VII. Conclusion and Future Remarks
Intensive research into the mechanisms of inflammation in the last decade has described the outlines of the intricate relationship between oxidative stress and inflammation. Clearance of pathogens from the body is the principle objective of inflammation for which ROS produced by phagocytic cells plays a fundamental role. The ambient levels of ROS are important for homeostasis of cells; whereas excessive ROS are important in killing pathogens. If ROS are not controlled by an array of sophisticated antioxidant mechanisms, it leads to inflammatory tissue injury. The antioxidant machinery of the cell, thus, plays an essential role in setting up this intricate balance. Despite an understanding of the role of oxidants in the inflammatory progression, treatments utilizing a variety of antioxidant approaches have not yet been successful. Failure of antioxidant clinical trials (207) indicates gaps in our general understanding whether oxidative stress is salutatory or detrimental in inflammation. Since oxidants have homeostatic and well-calibrated signaling functions in cells, untargeted antioxidant therapy may not prove to be efficacious or may be efficacious under unique circumstances. It is also possible that the distribution of antioxidants at specific sites in specific cells will be effective as opposed to a generalized alteration in the redox balance. A related issue is the compartmentalized nature of ROS production that is not easily accessible to antioxidants (146, 213). While it is clear that ROS are important to the pathogenesis of inflammation and tissue injury, much remains to be learned about how ROS function physiologically and how they contribute to the mechanism of inflammation and tissue injury.
Sources of Funding
This work was supported by the AHA Midwest affiliate Postdoctoral fellowship (13POST16640000) to M.M., U.S. National Institutes of Health grants P01 HL77806, P01 HL 060678, R01 HL 045638, and R01 HL 090152 to A.B.M. and HL66109 and ES11863 to S.P.R.
