Abstract
Introduction:
Lipedema is an abnormal deposit of subcutaneous fat most often involving the lower limbs symmetrically. The physiopathology is poorly understood, but its peak of the almost exclusively female involvement and its peak of appearance at puberty, during pregnancy or at menopause orient toward a hormonal involvement, whereas other elements are in favor of a strong genetic predisposition. Klinefelter syndrome (KS) is a genetic disease linked to aneuploidy resulting in a karyotype 47 XXY most of the time. There is a substantial variation in clinical presentation, but it often features infertility, firm testicular hypotrophy, hypergonadotropic hypogonadism, gynecomastia, and learning difficulties. Many other pathologies are associated with KS, but lipedema is never mentioned and there are no data in the literature linking these two pathologies.
Observation:
We report the cases of a 55-year-old man (146.8 kg, body mass index [BMI] 40.96 kg/m2) whose diagnosis of KS was known when hospitalized for lipedema, and of a 62-year-old man (198.1 kg, BMI 68.55 kg/m2) whose diagnosis of KS was made after the hospitalization for lipedema.
Discussion:
The concomitant presence of these two rare pathologies encourages the construction of an epidemiological study to support this association. It is also an element that can feed the research on the physiopathology of these two affections. Finally, the clinician must know how to suspect the possibility of lipedema in a patient with KS presenting an enlargement of the lower limbs and should know how to evoke a diagnosis of KS in front of a lipedema aspect in a man.
Introduction
Lipedema occurs almost exclusively in overweight or obese female patients.1–3 Although it is not considered as a hereditary condition, a family history is found in 16–64% of cases. 4
The prevalence of lipedema is difficult to estimate because it is underdiagnosed.2,4 The prevalence has been estimated to be 1 in 72,000 in the general UK population but could represent between 8% and 18% of the causes of lower limb enlargement in patients hospitalized in specialized services. 5
Lipedema is an enlargement of the limbs due to abnormal subcutaneous fat deposition that is symmetrical and mostly in the lower limbs. It is sensitive to pressure and touch and has little or no true edema. Unlike lymphedema, Stemmer's sign (inability to pinch the back of the base of the second toe) is always negative because lipedema spares the feet.1,3,4 Lipedema is associated with a tendency for hematomas, whereas it does not increase the risk of bacterial dermohypodermatitis. Nor compression alone, by bandage or stocking, neither diuretic treatment 6 or elevation 1 has influence on the limb's volume.
The differential diagnosis between lymphedema and edema due to venous insufficiency is clinical in most cases. However, in the most difficult cases, ultrasound can be helpfull.6,7 There are mixed lipedemas, because other causes of edema may coexist (venous insufficiency in 20% of cases of lipedema 1 ), and lipedema may be complicated by lymphedema in the most severe cases, resulting in lipolymphedema. 4
The underlying mechanism of lipedema is poorly understood. 5 There is a strong heredity suggesting a genetic cause. Weight gain aggravates lipedema and points to a mechanical or inflammatory cause. A pathway mediated by microangiopathy and angiogenesis has also been suggested. 4 In addition, because it affects almost exclusively females and appears during puberty, pregnancy, or menopause hormonal mechanisms could be involved.1–4,8
Klinefelter syndrome (KS) is the most common genetic cause of infertility. The prevalence is estimated to 0.1–0.2% in the general population and at least to 3% of the infertile population (10% in case of azoospermia).9–11
Eighty percent of cases are related to a chromosomal formula of type 47 XXY, whereas the remaining 20% are related to an aneuploidy of another type (mosaic 46, XY/47, XXY, or structural abnormality of the X chromosome for example and more rarely a karyotype 48, XXXY, 48, XXYY or 49, XXXXY). The aberrant X is of either paternal or maternal origin. 11 Between 50% and 75% of KS are undiagnosed according to recent reviews.9,10 The pathophysiology of the syndrome is poorly understood and involves both hypogonadism and aneuploidy by the presence of a supernumerary X chromosome. 11
Cardinal features of the syndrome include infertility, firm testicular hypotrophy, hypergonadotropic hypogonadism, gynecomastia, and learning disabilities. 10 Phenotypic variability is high and the diagnosis is made by karyotype analysis.9,10
Lipedema is not described in KS. A study that found 78 pathologies overrepresented in KS does not describe either lipedema or edema of the lower limbs (in the event of a misdiagnosis). 12
When PubMed was searched for “lipoedema or lipedema” and “Klinefelter,” no occurrence was found.
We report these cases with an internal review board approval.
Case 1
A 56-year-old man with KS (karyotype 47, XXY) was referred to an overweight unit for medical management of his morbid obesity. He weighed 146.8 kg for 1.85 m, that is, a body mass index (BMI) of 41.8 kg/m2.
KS was diagnosed at 54 years, whereas hypogonadism (not investigated) had been discovered at 29 years in a context of infertility. Hormone replacement has not been implemented so far due to intolerance even at low doses (aggressiveness and insomnia). His total testosterone was 1.33 ng/mL (4.6 nmol/L, N: 8.7–34.7) compared with a high gonadotrophin (follicle stimulating hormone [FSH] 22.1 IU/L and luteinizing hormone [LH] 12.5 IU/L).
His weight has progressively increase since adolescence. His weight was 90 kg when he was 14 (i.e., BMI 26 kg/m2, between International Obesity Task Force [IOTF] 25 and IOTF 30) and reached the maximum of 158 kg (BMI 46 kg/m2) at the age of 54 years. This morbid obesity was complicated by mechanical joint pain of the right knee and the right ankle, but fasting blood glucose was 1.01 g/L (5.6 mmol/L), triglycerides were 1.1 g/L, high density lipoprotein cholesterol was 0.51 g/L, and low density lipoprotein cholesterol was 1.35 g/L, whereas the liver assessment was normal and without gamma-glutamyl transferase elevation (20 IU/L, norms: 12–64). The homeostasis model assessment-estimated insulin resistance was 4.7 (<2), in favor of insulin resistance.
He was suffering from venous insufficiency with a history of dermohypodermatitis and an appearance of ochre dermatitis that only partially responded to venous compression. In addition, the lower limbs were enlarged and sensitive with symmetrical involvement (Figs. 1 and 2). Stemmer's sign was negative, whereas we did not find any argument for a secondary cause for this enlargement of the lower limbs: thyroid stimulating hormone was 1.92 IUU/mL (0.35–4.94), albumin 43.5 g/L (35–50), and brain natriuretic peptide (BNP) was 13 pg/mL (<100).
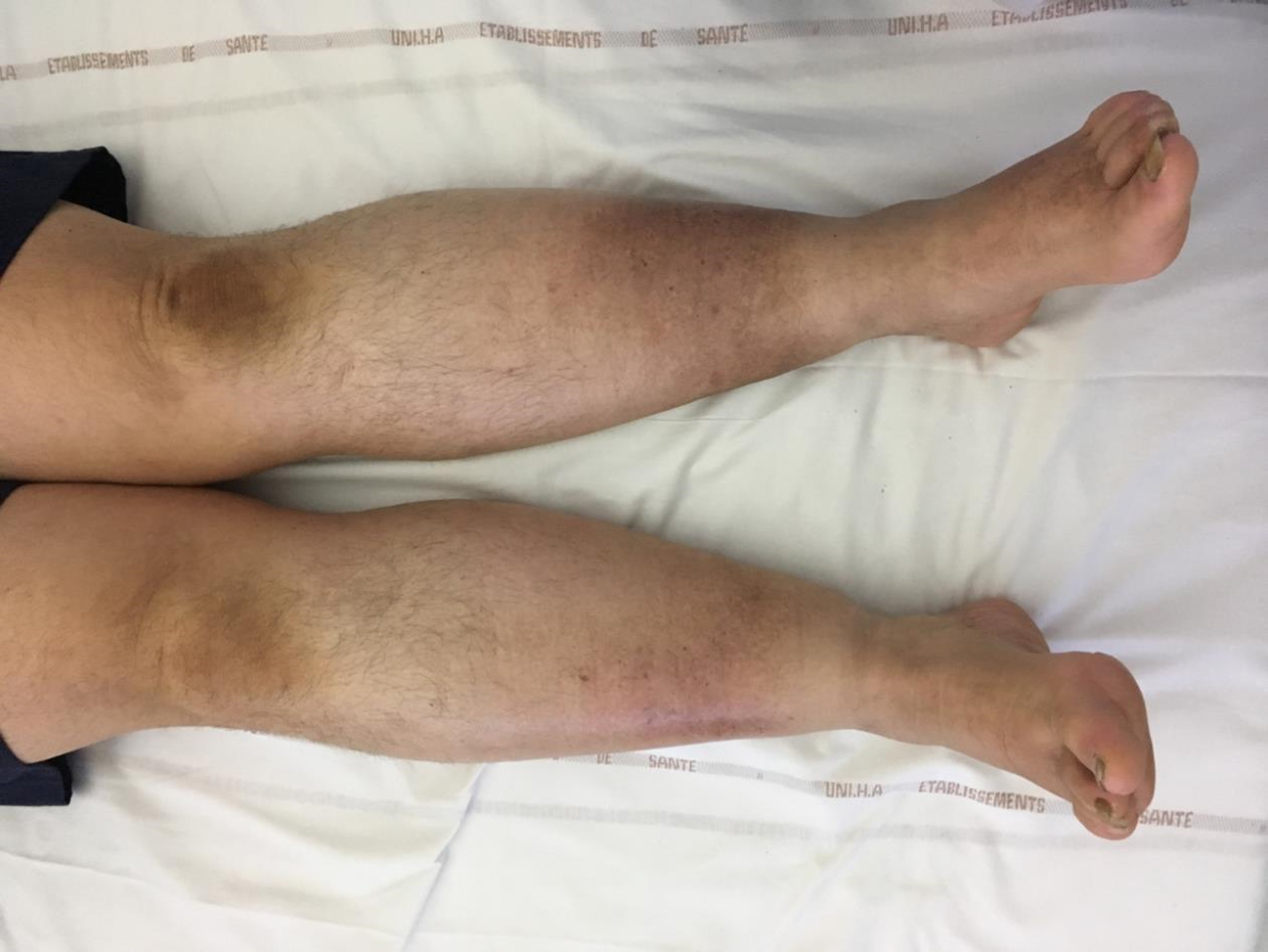
Picture of lower limbs, front view case 1.

Picture of lower limbs, from the back case 1.
An ultrasound scan of the lower limbs showed an increased thickness of the hypodermis without any associated abnormality of the dermis (effective venous restraint; Fig. 3). The thickness of the dermis was identical in the arm and the leg (Fig. 4).

Ultrasound of the left leg of case 1.

Ultrasound of the right arm of case 1.
These elements lead us to the diagnosis of stage 1 lipedema of the lower limbs associated with venous insufficiency effectively treated by elastic compression evolving in a context of morbid obesity and KS. Despite weight loss during the follow-up (135 kg at the last visit), the enlargement of the lower limbs was clinically stable.
Case 2
A 62-year-old man was referred to the department for management of his severe obesity (198.1 kg for 1.7 m, i.e., a BMI of 69 kg/m2).
His obesity had begun during adulthood. At the age of 21 years his weight was 76 kg corresponding to a BMI of 26.3 kg/m2). The maximum weight of 208.2 kg, that is, BMI of 72 kg/m2 was reached at the age of 59 years. He was also suffering from type 2 diabetes, hypertension, permanent atrial fibrillation, ventral hernia, and venolymphatic insufficiency.
The lower limbs were asymmetrically enlarged. Lymphatic insufficiency at the elephantiasis stage with papillomatosis was diagnosed at the right lower limb. This condition happened since he was 50 years old after his second erysipelas of the right lower limb. In addition to lymphatic insufficiency venous insufficiency and bilateral lipedema were diagnosed in vascular medicine department of our hospital at the age of 58. The first available picture are from the age of 59 (Figs. 5 and 6). The patient was maintained on specialized treatment, but the compliance was low and the evolution was not favorable as shown by the current clinical aspect (Figs. 7 and 8). Indeed, two hospitalizations for volume reduction did not result in any significant effect on the volume of the lower limbs, although there was a decrease in skin induration.

Front view of the lower limbs at age 59 years of case 2.
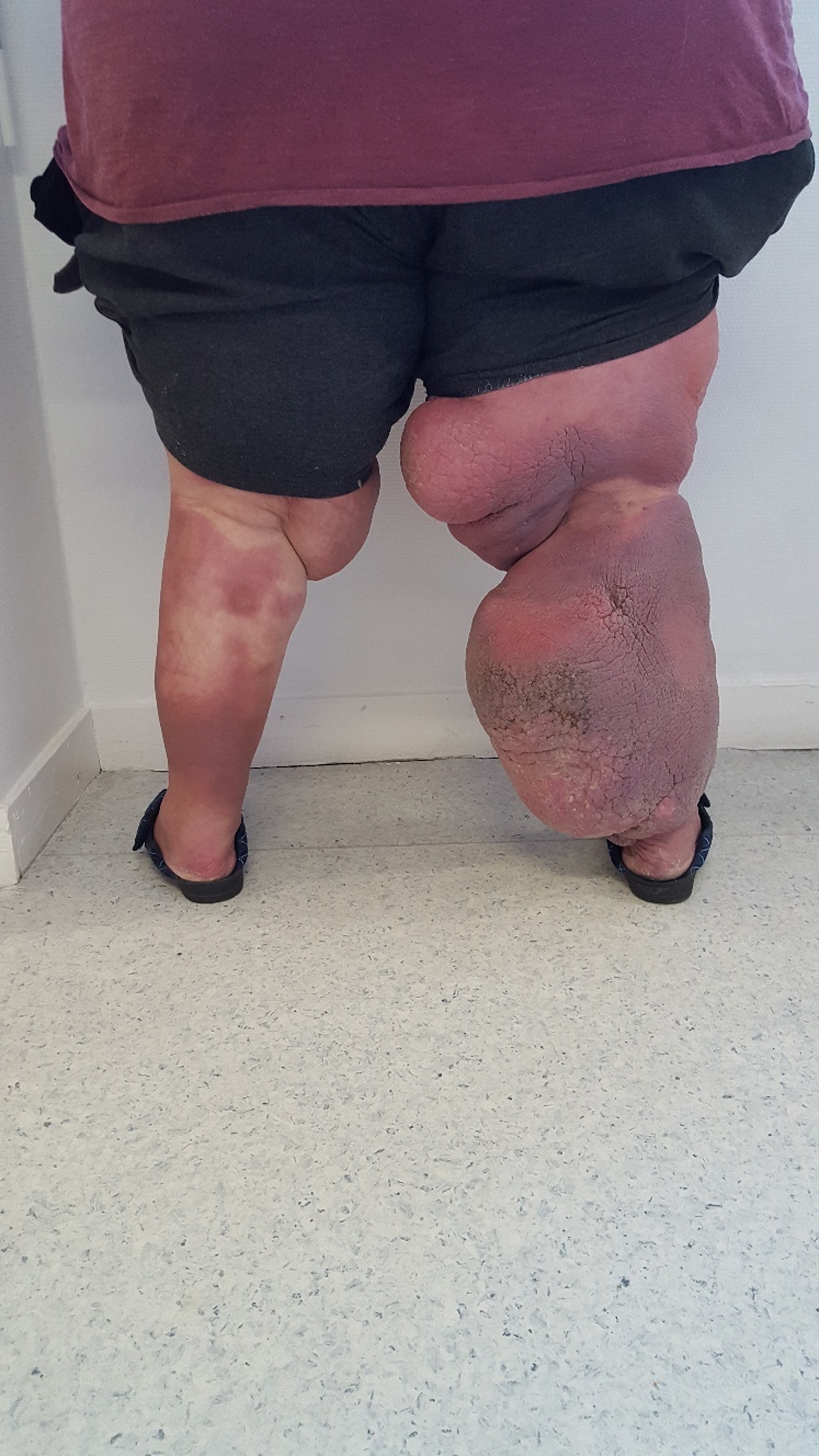
Picture of the lower limbs from the back to 59 years of age of case 2.

Front view of the lower limbs at age 63 years of case 2—left foot is spared.

Picture of the left lower limb at age 63 years of case 2—foot is spared.
There was no history of lipedema among women in the family. Stemmer's sign was negative on the left side, whereas the toes of the right foot were cubic. The lower limbs were moderately tender.
We have no evidence for a secondary cause of edema. There was no significant hypoalbuminemia (albumin 35 g/L) and no clinical or biological heart failure (BNP 47 pg/mL [<100]). Thyroid stimulating hormone is normal. No obstruction of the lymphatic tract was found on computerized tomography scan.
He displayed a sexual dysfunction, a severe bilateral testicular hypotrophy with an estimated volume of each testicle of 3–4 mL and hypergonadotropic hypogonadism (total testosterone 0.48 ng/mL = 1.66 nmol/L[N 5–24], FSH 19.2 IU/L and LH 15.4 IU/L). The diagnosis of KS was confirmed by a chromosome analysis that revealed a karyotype 47, XXY. Hormone replacement has only been introduced for a year and no effect has been demonstrated on his lipedema to date.
We, therefore, diagnosed a lipedema of the lower limbs associated with bilateral venous insufficiency and lymphedema at the elephantiasis stage of the right lower limb evolving in a context of grade 3 obesity and KS.
Discussion
To our knowledge, we report in this study for the first time the occurrence of lipedema in patients with KS.
In 1 year, two patients referred to our center for obesity had both lipedema and KS. The rarity of these two pathologies reduces the risk of coincidence of their association. Moreover, contrary to the majority of studies or series published on lipedema, our observation does not come from a specialized center in venolymphatic pathologies. We do not have the hindsight to report the possible effect of hormone replacement on lipedema.
The first case of a man with lipedema to be reported in the English literature was in 2004, but the cause is undescribed. 13 One study reports the case of a 23-year-old man with a pituitary transcription factor 1 mutation (responsible for congenital hypogonadism) with lipedema. 14 Since then, the rare cases of lipedema reported in men have been in patients with hypogonadism with or without hepatocellular insufficiency. 2
It should be noted that KS is associated with venous pathology of the lower limb such as varicose veins and venous ulcers in 1 case out of 3. 9 The relative risk of venous insufficiency is estimated at 5. 12 In addition, the relative risk of obesity in KS is estimated to be 4 in one study. 15 Therefore, we can assume that some lipedema may have been misclassified as venous insufficiency or obesity in KS.
The association between lipedema and KS is an argument for a role of hormones in lipedema. However, the supernumerary X chromosome may be involved, pleading for a genetic cause. We did not find any data in the literature dealing with the effect of estrogen or testosterone treatments on lipedema.
A retrospective cohort study conducted in England found a higher prevalence of autoimmune pathology in patients with KS compared with a group of male controls. 12 The association was statistically significant for 7 of the 30 autoimmune diseases analyzed, including hypothyroidism, multiple sclerosis, lupus, Sjogren's syndrome, rheumatoid arthritis, and Addison's disease, which have a higher prevalence in the female population. There was no association with Goodpasture's syndrome and ankylosing spondylitis, which are autoimmune pathologies more frequent in men. However, type 1 diabetes, with a sex ratio of 1 in the general population, was also found more frequently in patients with KS. However, the pathophysiology is uncertain and the higher prevalence of these autoimmune diseases in women may be mediated by both hormonal and genetic factors located on the X chromosome.
There are key differences between males and females in adipose tissue distribution and expansion, but the independent roles of gonadal hormones and sex chromosomes have not been fully understood. The presence of two X chromosomes has been associated with increased adiposity and dyslipidemia in Four Core Genotypes mouse model (consisting of XX mice with either ovaries or testes, and XY mice with either ovaries or testes). The enhanced expression of genes that escape X chromosome inactivation may contribute. 16 XXY men have also hormonal abnormality and our two cases had significant hypogonadism so the X chromosome as well as hypogonadism may be involved here.
We report only two cases of lipedema in patients suffering from KS. However, as previously said, lipedema may have been underdiagnosed in this situation and an observational study in a population with KS searching for lipedema (e.g., using ultrasound) could allow us to rule on the presence of this association between these two rare pathologies.
In addition, our observation indicates that the existence of lipedema should be investigated in front of an enlargement of the lower limbs in an obese patient suffering from KS and the clinician should know how to suspect a diagnosis of KS in front of a lipedema aspect in a man.
Footnotes
Authors' Contributions
O.C. and C.L.M. conceived the idea of this case report. O.C. wrote the draft of the article in French. C.L.M., L.B., M.M., E.P., M.M.-H., and B.G.-C. provided critical feedback. M.M. and B.G.-C. provided the English translation. All authors discussed the results and contributed to the final article.
Acknowledgments
We thank the Bordeaux University Hospital for allowing this study. We also thank the two subjects who gave their informed consent for the publication.
Author Disclosure Statement
The authors do not have any conflicts of interest to disclose.
Funding Information
This research did not receive any specific grant from any funding agency in the public, commercial, or not-for-profit sector.
