Abstract
Patients with pulmonary arterial hypertension (PAH) often require parenteral prostanoids to improve symptoms and signs of PAH. Complications of parenteral prostanoids—such as catheter-related infections and intolerable adverse effects—may develop, prompting transition to inhaled prostanoids. We report a prospective, protocol-driven transition from parenteral prostanoids to inhaled prostanoids with monitoring of exercise gas exchange and acute hemodynamics. Three PAH centers recruited patients transitioning from parenteral prostanoids to inhaled trepostinil. Rigid inclusion criteria were used, including parenteral prostanoid dose < 30 ng/kg/min, New York Heart Association functional class (FC) < 3, and pulmonary vascular resistance (PVR) < 6 Wood units. Of the 9 patients meeting initial inclusion criteria, 3 were excluded. In the remaining patients, the parenteral prostanoid was reduced and the inhaled prostanoid was increased over 24–36 hours with continuous hemodynamic monitoring. Exercise capacity and FC were measured at baseline and weeks 1, 4, and 12. All patients were successfully weaned from parenteral prostanoids. An acute PVR decrease was seen with most inhaled prostanoid doses, but PVR varied throughout the transition. Patients tolerated inhaled prostanoids for 9–12 breaths 4 times a day with no treatment-limiting adverse events. At week 12, FC was unchanged, and all patients continued to receive inhaled prostanoids without serious adverse events or additional PAH therapy. In 5 of 6 patients, 6-minute walk distance and peak V̇O2 were within 10% of baseline. Using a strict transition protocol and rigid patient selection criteria, the parenteral prostanoid to inhaled prostanoid transition appeared safe and well tolerated and did not result in clinical deterioration over 12 weeks. Hemodynamic variability noted acutely during transition in our study did not adversely affect successful transition. (Trial registration: ClinicalTrials.gov identifier: NCT01268553)
Patients with pulmonary arterial hypertension (PAH) suffer from pulmonary vascular disease and progressive right ventricular dysfunction, with dyspnea and reduced exercise tolerance. These patients often require parenteral prostanoid therapy to improve their signs and symptoms of PAH, particularly when oral treatments have failed to produce clinical improvements or after patients worsen, despite initial improvement. 1
Patients receiving parenteral prostanoids may develop complications, such as catheter-related infections and/or intolerable adverse effects, potentially limiting their use. 2 The potential burden of these complications on the healthcare system, including costs associated with the drug delivery systems, can be significant.2,3 With the approval of inhaled iloprost4,5 and inhaled treprostinil 6 as additional options to treat PAH patients with prostanoids, efforts to transition appropriate PAH patients from parenteral to inhaled prostanoids have been reported.7,8 These retrospective studies demonstrated the feasibility of the transition process; however, they did not report the acute hemodynamic responses of the transition or the effects on cardiopulmonary gas exchange during exercise. We report the results of a prospective, protocol-driven transition from parenteral prostanoids to inhaled treprostinil, with continuous invasive hemodynamic monitoring during transition, pre-/postexercise gas exchange measurements, and quality of life (QoL) before and after transition.
METHODS
Three PAH specialty referral centers (Harbor-UCLA Medical Center; University of California, San Francisco; and University of Arizona) with experience in the diagnosis and management of PAH—including specific expertise in the use of parenteral and inhaled prostanoids—participated in this open-label prospective study (Fig. 1). We recruited stable World Health Organization (WHO) group 1 PAH patients receiving long-term parenteral prostanoids in whom a clinical decision to transition from parenteral to inhaled treprostinil was made by the treating physician before consideration for any clinical study. The reason for transition in the patients receiving subcutaneous treprostinil was infusion site pain, and the reasons for transition in the patients receiving intravenous epoprostenol was pragmatic (daily mixing of medication and maintenance of central venous catheter and infusion pump).
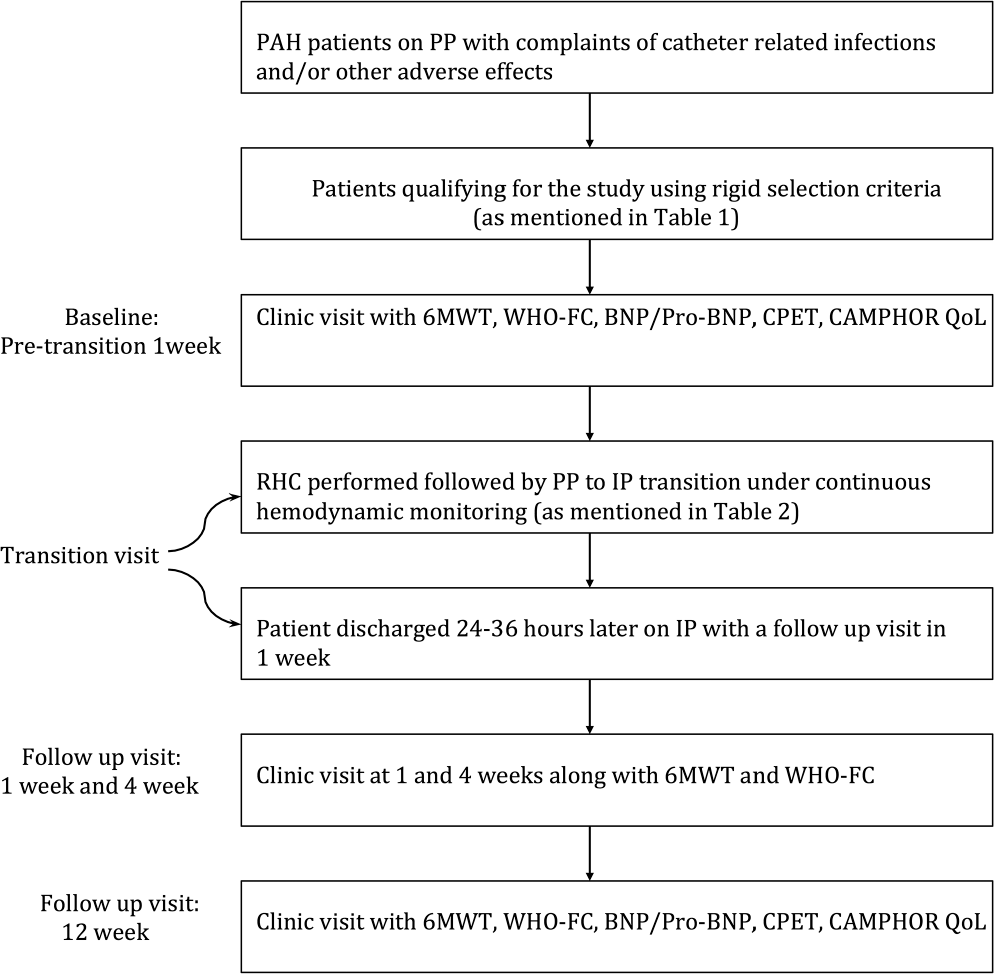
Study protocol. 6MWT: 6-minute walk test; BNP: B-type natriuretic peptide; CAMPHOR QoL: Cambridge Pulmonary Hypertension Outcome Review quality of life; CPET: cardiopulmonary exercise testing; IP: inhaled prostanoids; PAH: pulmonary arterial hypertension; PP: parenteral prostanoids; RHC: right heart catheterization; WHO-FC: World Health Organization functional class.
In addition, to ensure study safety, rigid inclusion criteria (derived from expert consensus) had to be met to qualify for the transition: parenteral prostanoid dose < 30 ng/kg/min, New York Heart Association functional class (FC) < 3, and pulmonary vascular resistance (PVR) < 6 Wood units (WU). Additional inclusion and exclusion criteria are shown in Table 1.
Inclusion and exclusion criteria
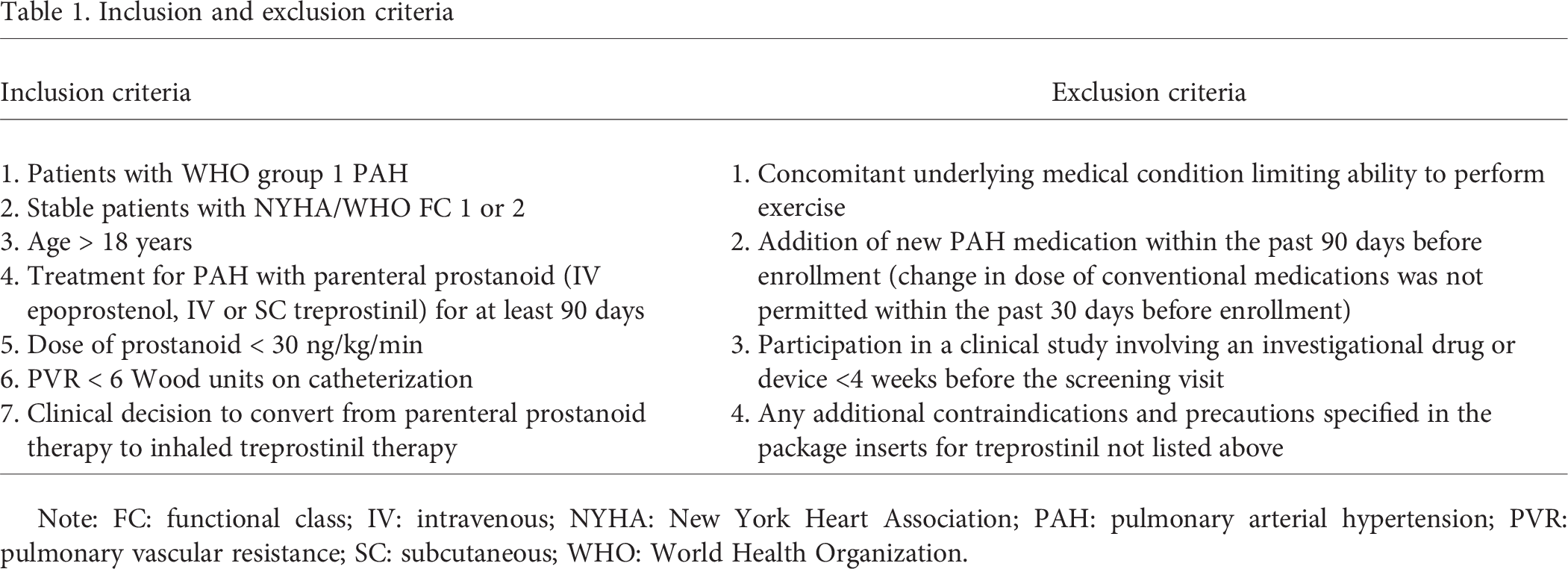
Note: FC: functional class; IV: intravenous; NYHA: New York Heart Association; PAH: pulmonary arterial hypertension; PVR: pulmonary vascular resistance; SC: subcutaneous; WHO: World Health Organization.
The primary outcome measurement in this study was safety—with secondary end points of PVR, 6-minute walk distance (6MWD), peak V̇O2 (oxygen consumption), and V̇E/V̇CO2 (ratio of minute ventilation to CO2 output)—measured noninvasively with cardiopulmonary exercise testing (CPET), B-type natriuretic peptide (BNP) or N-terminal pro-BNP levels, and QoL (Cambridge Pulmonary Hypertension Outcome Review [CAMPHOR] questionnaire). Additional data collected included patient demographics, clinical history and physical examination, and medication history.
Transition protocol. After the QoL questionnaire was administered in the PAH clinic and baseline 6-minute walk test (6MWT) and CPET were performed, patients were admitted to the hospital for right heart catheterization (RHC) and overnight monitoring. Serial hemodynamics were recorded throughout the inpatient transition process (at baseline and before and after each treprostinil inhalation session). Each patient's parenteral prostanoid dose was initially titrated down to 10–15 ng/kg/min over a period of 2–4 hours, followed by a 3-breath inhalation of treprostinil once the target parenteral prostanoid dose was reached. Additional down-titrations of approximately 5 ng/kg/min were performed approximately every 4–6 hours, with the goal of maximizing the number of inhalations (minimum goal of 6 breaths per session, maximum of 12 breaths per session) while reducing the parenteral prostanoid dose to 0 over approximately 12 hours. At each time point, hemodynamic and clinical data were obtained, and the decision to continue or terminate the transition was made. Patients were kept in the hospital with the right heart catheter in place until approximately 24 hours had passed (usually the next morning), at which time the parenteral prostanoid was discontinued and the patient was tolerating a maximum of 6–12 breaths every 4–6 hours (Table 2).
Transition protocol (dose changes)

Note: In addition to down-titration and up-titration of prostanoids, invasive hemodynamics were recorded before and after inhaled prostanoid therapy. Changes in the hemodynamics are shown for each patient in Figure 2. BL: baseline; PA: pulmonary artery.
During the inpatient transition, patients received instruction on their inhaled treprostinil dosing. At discharge, patients were provided with contact information for a specialty pharmacy nurse overseeing the initiation and maintenance of the inhaled treprostinil, with a scheduled home visit within 1 week of discharge.
At weeks 1, 4, and 12, patients returned to the PAH clinic for a physician and nurse visit, which included vital signs, a history and physical examination, medication history, and WHO FC. In addition, a repeat 6MWT was measured at these visits. Additionally, at week 12, a repeat CAMPHOR questionnaire was administered, a serum BNP or N-terminal BNP was obtained, and a repeat CPET was performed. Adverse and serious adverse events were captured.
The transition from parenteral prostanoids to inhaled treprostinil was considered successful if the patient tolerated the transition (including the newly started inhaled prostanoids) without serious adverse events, maintained stable hemodynamics throughout the transition, and did not need to be transitioned back to parenteral prostanoids.
Descriptive statistics are presented for safety data and for before-and-after data, since no control group was used. This study protocol was reviewed and approved by the respective institutional review boards at each participating institution. Informed consent was obtained from all patients before participation.
RESULTS
Of the 9 patients meeting initial inclusion and exclusion criteria on screening, PVR was >6 WU in 2 patients, who were then excluded from study participation and continued receiving parenteral prostanoid therapy. An additional patient had a baseline PVR of <6 WU; however, during transition, her PVR increased to 10 WU. A decision to discontinue further transition efforts was made, and the patient resumed parenteral prostanoid therapy. Finally, one patient had a PVR of 5.2 WU on RHC performed for study qualification on the morning of transition. Once her transition began, the PVR increased to 8.41 WU, and a decision to continue the transition was made; in this patient, the higher PVR was used as a baseline for studying the hemodynamics changes. All patients were screened and enrolled over a time period of 2.4 years.
Demographic data for all 9 patients are shown in Table 3. During the transition, all 6 patients were successfully weaned off their parenteral prostanoids over 24–36 hours, while the inhaled trepostinil was titrated up to 12 breaths 4 times a day over the same 24–36 hours, with continuous hemodynamic monitoring.
Baseline demographics
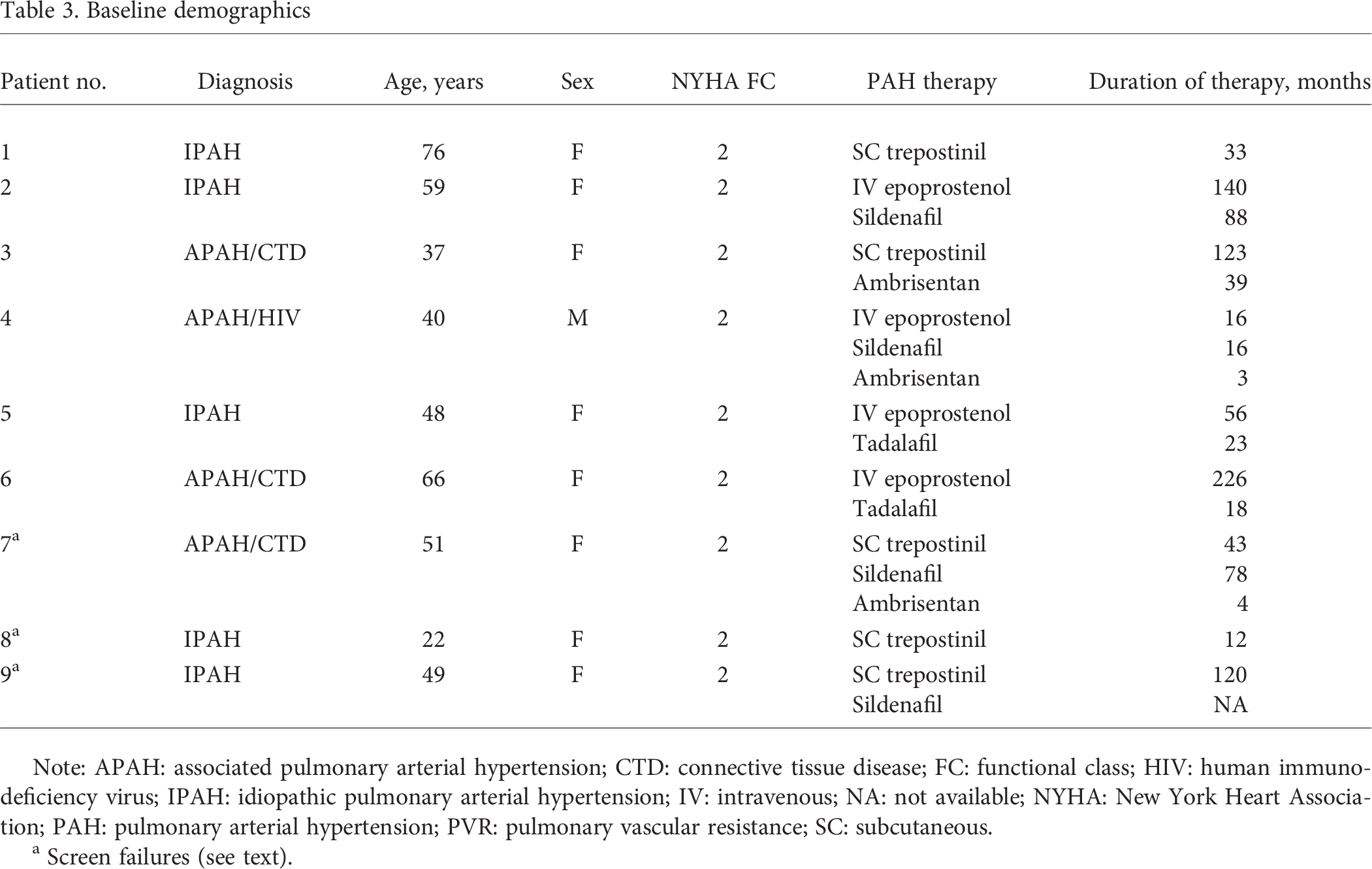
Note: APAH: associated pulmonary arterial hypertension; CTD: connective tissue disease; FC: functional class; HIV: human immunodeficiency virus; IPAH: idiopathic pulmonary arterial hypertension; IV: intravenous; NA: not available; NYHA: New York Heart Association; PAH: pulmonary arterial hypertension; PVR: pulmonary vascular resistance; SC: subcutaneous.
Screen failures (see text).
With most inhaled trepostinil doses, PVR acutely decreased but varied throughout the transition periods (Fig. 2). By the end of transition, preinhalation PVR was 10%–47% lower in 3 patients and 6%–48% higher in 3 patients (Table 4).
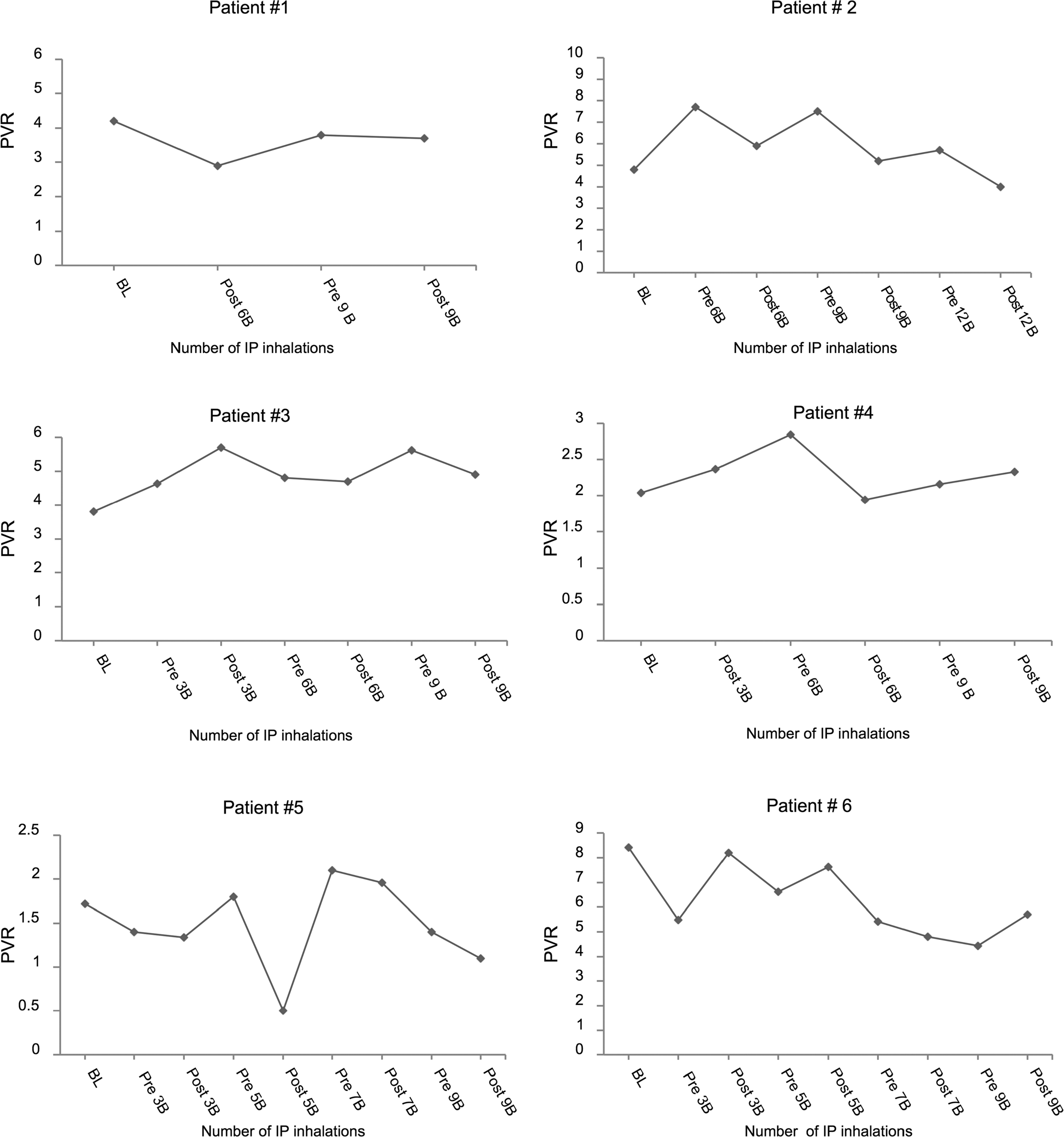
Pulmonary vascular resistance (PVR; Wood units) before and after increasing doses of inhaled prostanoid (IP) in each of 6 patients transitioned from parenteral to inhaled prostanoid. Each measurement was performed before or after an inhalation session of 3–12 breaths per session. Note the wide variation in acute hemodynamic changes with each inhalation session. BL: baseline; Post xB: after inhalation of x breaths of inhaled prostanoid; Pre xB: before inhalation of x breaths of inhaled prostanoid.
Pre- and immediate posttransition hemodynamics recorded during preinhalation phase
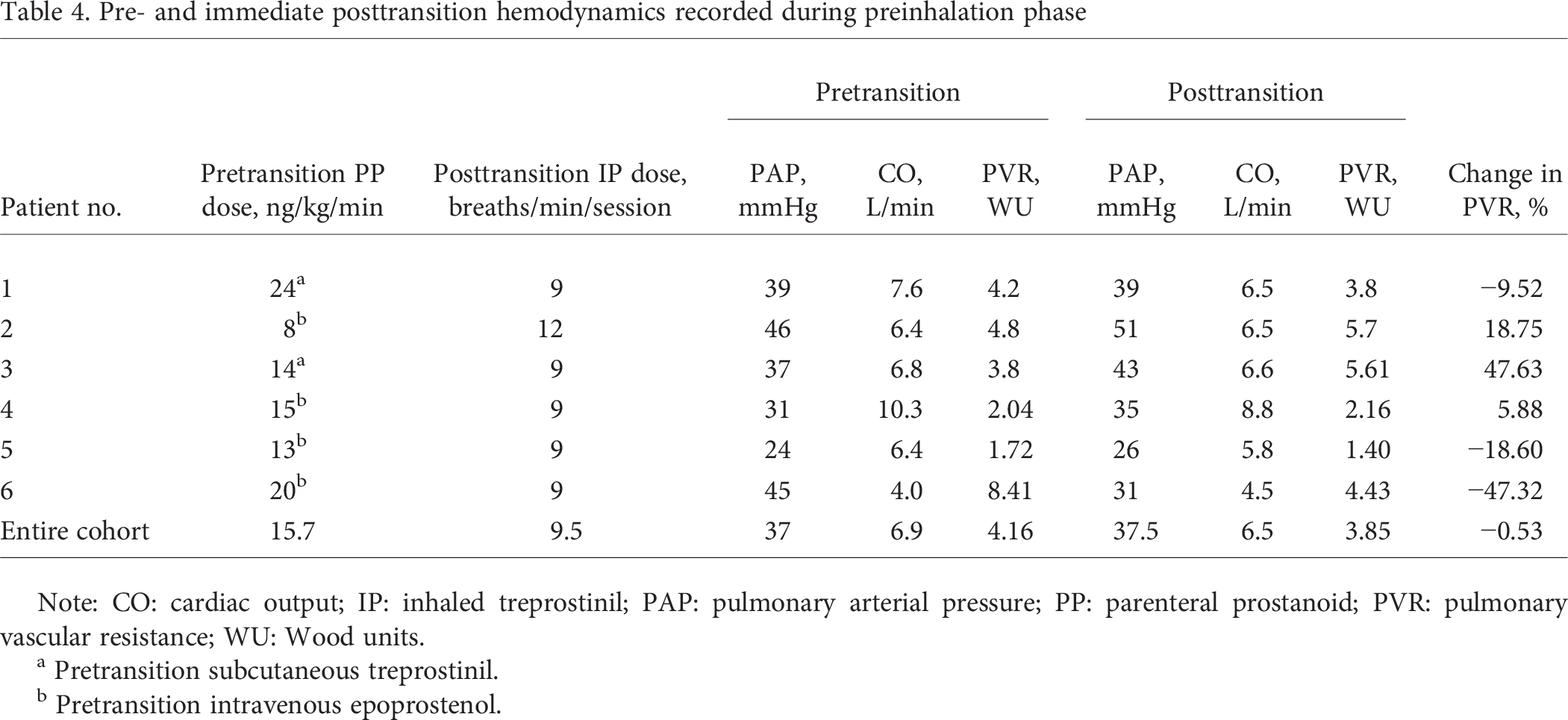
Note: CO: cardiac output; IP: inhaled treprostinil; PAP: pulmonary arterial pressure; PP: parenteral prostanoid; PVR: pulmonary vascular resistance; WU: Wood units.
Pretransition subcutaneous treprostinil.
Pretransition intravenous epoprostenol.
There were no treatment-limiting adverse events. At week 12, WHO FC was unchanged for all 6 patients. In 5 of the 6 patients, 6MWD, peak V̇O2, and V̇E/V̇CO2 were within 10% of their baseline values. In 1 patient (patient 1), 6MWD increased >50% because of a low baseline value from knee pain. The baseline and week 12 exercise capacity, QoL, and BNP levels are shown in Table 5.
Baseline and week 12 data
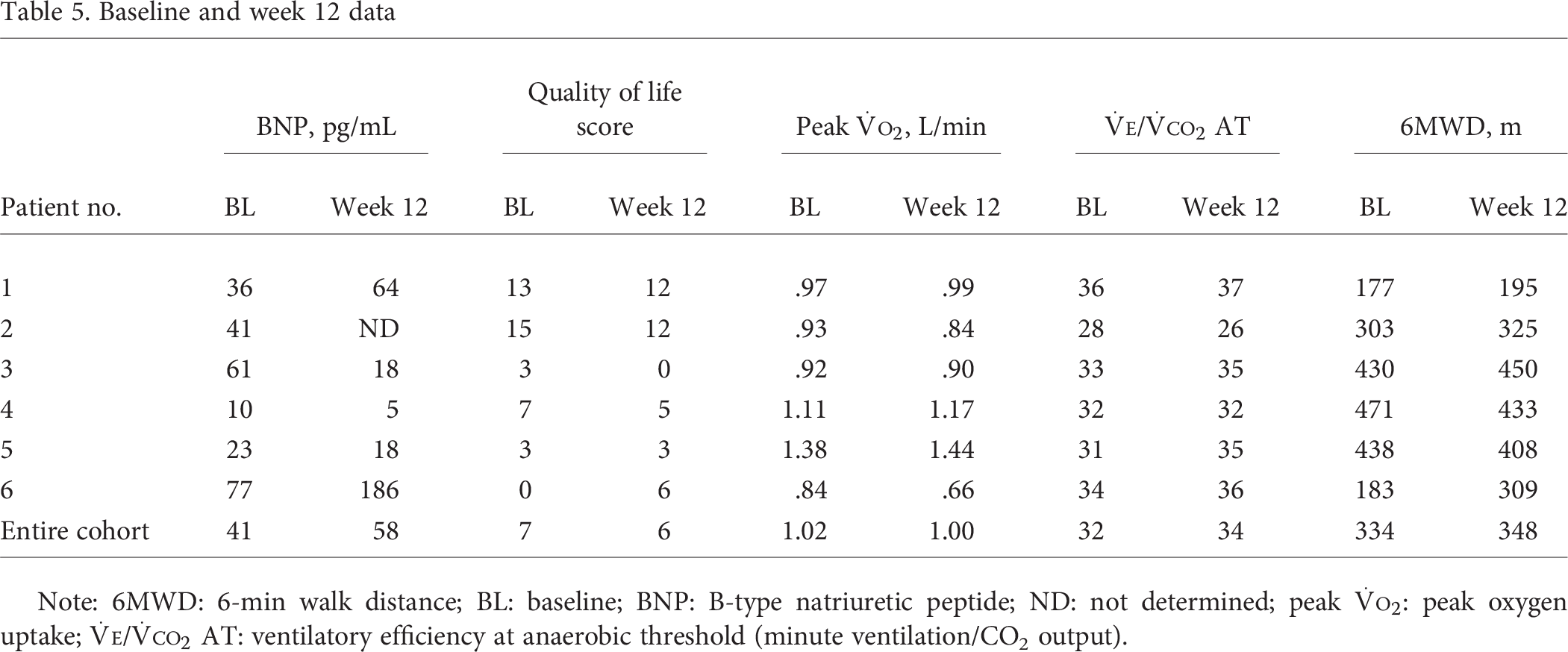
Note: 6MWD: 6-min walk distance; BL: baseline; BNP: B-type natriuretic peptide; ND: not determined; peak V̇O2: peak oxygen uptake; V̇E/V̇CO2 AT: ventilatory efficiency at anaerobic threshold (minute ventilation/CO2 output).
DISCUSSION
Despite an abundance of clinical data supporting the efficacy of parenteral prostanoid therapies for PAH patients,9–16 the limitations of these therapies and the burden on QoL are well described.2,11,17–21 In clinically stable PAH patients receiving parenteral prostanoid therapy, there may be instances in which the patient and their treating physician determine that the patient may be a candidate for transitioning off parenteral PAH therapy. In such patients, the transition protocol that we employed—defining strict inclusion and exclusion criteria, combined with close clinical monitoring—provided us with important knowledge about the hemodynamic and physiologic changes that occur during transition and during inhalation. This is the first study to provide prospective insight into a strict, protocol-driven transition approach to ensure stability in PAH patients during the transition process by the application of disease-specific (i.e., hemodynamics, CPET) and functional (i.e., 6MWD, CPET) methodology. These parameters are sensitive, disease-specific measurements.
Other retrospective studies have examined the transition from parenteral to inhaled treprostinil, using a less rigorous protocol. Raina et al. 8 reported a successful transition from parenteral treprostinil to inhaled treprostinil in 2 patients with PAH. They used a parenteral prostanoid weaning protocol similar to ours, with decreases in increments of 5 ng/kg/min every 6 hours and uptitration of inhaled treprostinil over 3 days. They did not perform the transition with continuous hemodynamic monitoring or CPET. In a retrospective study, de Jesus Perez et al. 22 reviewed the outcomes of 18 PAH patients transitioned from parenteral treprostinil to inhaled treprostinil at their center. They also did not perform the transition with continuous hemodynamic monitoring or CPET, and they noted that 2 (11%) patients required reinstitution of parenteral prostanoids because of their worsening PAH symptoms. None of the above transition studies reported QoL measures.
Our study presents a conceptual framework for successful transition of PAH patients. Careful selection of appropriate patients likely yielded salutary transition results. In addition, the strict inclusion and exclusion criteria, along with the continuous hemodynamic monitoring employed during the transition, likely contributed to the safe transition of our patients from parenteral to inhaled prostanoids.
Considerable hemodynamic variability was observed in our patients during the inpatient transition. However, this variability did not appear to have any clinical impact on the short-term success of the transition. It must be stressed that the lack of near-term hemodynamic and/or clinical worsening after changing therapies in PAH patients does not provide assurance that subsequent worsening will not occur. Rich et al. 23 noted spontaneous hemodynamic variability in pulmonary hypertension patients undergoing continuous hemodynamic monitoring in the pretreatment era (before approval of the first PAH treatment). Similar hemodynamic fluctuations during treatment with another inhaled prostanoid (iloprost) have also been demonstrated by Fruhwald et al. 24 These investigators reported rapid drops in pulmonary arterial pressure (PAP) after iloprost administration after a relatively stable PAP baseline obtained before each inhalation.
Adherence to a strict protocol with close follow-up and repeated measurements of PAH severity markers—such as 6MWD, 25 peak V̇O2, 26 V̇E/V̇CO2, 26 BNP,27,28 and CAMPHOR score 29 —provided reassurance that the PAH disease process was stable during and after the transition. While we cannot determine whether the transitions we performed in this study would have been less risky without hemodynamic and/or physiologic monitoring, despite prior small reports of successful transitions, we believe that a conservative approach to PAH medication changes is prudent, given the high-risk nature of PAH patients, particularly those receiving parenteral prostanoids.
One patient failed to meet one of the hemodynamic inclusion criteria after initial catheterization (PVR < 6 WU); thus, transition was not attempted. However, we considered this patient a transition failure on the basis of an intention-to-treat basis, further supporting the premise that such transitions in PAH patients should be approached cautiously.
Our study was limited to patients meeting strict inclusion/exclusion criteria for our transition protocol. Thus, our results cannot be generalized to patients who do not meet these criteria. In addition, the outcomes of our study may not be generalizable to patients transitioning to other inhaled prostanoids. Finally, formal follow-up of our detailed safety and efficacy measures was limited to 12 weeks. This and the small number of subjects in our study limit application of our findings to a wider PAH population over a longer time period.
Using a strict transition protocol, parenteral prostanoid to inhaled trepostinil transition appeared safe and well tolerated and did not result in clinical deterioration over 12 weeks. Considerable hemodynamic variability noted acutely during transition in our study did not adversely affect successful transition.
