Abstract
We tested the hypothesis that bidimensional measurements of right ventricular (RV) function obtained by cardiac magnetic resonance imaging (CMR) in patients with pulmonary arterial hypertension (PAH) are faster than volumetric measures and highly reproducible, with comparable ability to predict patient survival. CMR-derived tricuspid annular plane systolic excursion (TAPSE), RV fractional shortening (RVFS), RV fractional area change (RVFAC), standard functional and volumetric measures, and ventricular mass index (VMI) were compared with right heart catheterization data. CMR analysis time was recorded. Receiver operating characteristic curves, Kaplan-Meier, Cox proportional hazard (CPH), and Bland-Altman test were used for analysis. Forty-nine subjects with PAH and 18 control subjects were included. TAPSE, RVFS, RVFAC, RV ejection fraction, and VMI correlated significantly with pulmonary vascular resistance and mean pulmonary artery pressure (all
Keywords
Pulmonary arterial hypertension (PAH) is characterized by pulmonary vascular remodeling that results in a progressive increase in pulmonary artery pressure and vascular resistance, eventually leading to right ventricular (RV) failure. Increased intracavitary pressure in the RV initially leads to elevated wall stress and adaptive myocardial hypertrophy, followed by contractile dysfunction and maladaptive cavity dilatation with disease progression. RV response to the increased afterload is a major determinant of survival in subjects with PAH.1–3 Thus, serial assessment of RV function with indices such as RV ejection fraction (RVEF) may be important for patient management. 4
Echocardiography is routinely used in the clinical assessment of RV function (RVF) in PAH. However, evaluation of RVF with echocardiography is challenging due to the complex shape of the RV and its trabeculated and thin myocardium. 5 In addition, optimal imaging windows may not be attainable in up to 25% of patients. In spite of these limitations, echocardiography is extremely valuable as a screening modality for the diagnosis of PAH because of its wide availability and low cost. Earlier studies have shown that tricuspid annular plane systolic excursion (TAPSE) by echocardiography is a fast and easily obtainable measure of RVF 6 that predicts survival in patients with PAH.7–9
Reliable, noninvasive evaluation of the RV in patients with suspected PAH is feasible with cardiac magnetic resonance imaging (CMR). CMR accurately assesses RV structure and function, providing precise bidimensional (2D) and three-dimensional (3D) volumetric measurements of both ventricles. CMR has been validated for the RV and is considered the gold standard method for determining RVF.10–12 CMR-derived ventricular mass index (VMI) has been shown to predict prognosis in PAH.13,14 However, calculation of VMI requires time-consuming manual or semiautomated contouring of the left ventricle (LV) and RV. On the other hand, TAPSE by CMR is a 2D measurement that is simple and quick to obtain and has a high correlation with RVEF in healthy subjects.15,16 Therefore, we hypothesized that 2D measures by CMR would have the same prognostic value as 3D measures, such as VMI, but would be faster to obtain and more reproducible. The objectives of this study were to compare the utility of 2D measurements of RVF in assessment of prognosis in PAH by evaluating 2D and 3D measures in healthy control subjects and patients with PAH; comparing 2D measurements of RVF (TAPSE and others) and standard 3D RVF measurements with invasive measurements obtained by right heart catheterization (RHC); determining whether 2D measures can be used for prediction of survival and whether they are equivalent to the 3D approach; and determining inter- and intraobserver agreement and time needed for analysis for 2D and 3D measures by CMR.
METHODS
This prospective study was Health Insurance Portability and Accountability Act compliant and was approved by our institutional review board. From April 2004 to February 2013, 49 consecutive patients with PAH were enrolled after referral for a clinically indicated RHC. Inclusion criteria were PAH by RHC, defined as a mean pulmonary artery pressure (mPAP) ≥25 mmHg with a pulmonary capillary wedge pressure (PCWP) ≤15 mmHg 10 and the ability to undergo CMR. Exclusion criteria included chronic thromboembolic disease and obstructive or restrictive lung disease, as described elsewhere, 8 among others. Eighteen healthy control subjects underwent the same CMR protocol but were not subjected to RHC. History of previous treatment for PAH was recorded.
CMR acquisition
CMR for this study was performed on a 3-T (MAGNETOM Trio, Siemens Healthcare, Erlangen, Germany) system using a body coil array. Retrospectively gated segmented gradient echo (FLASH) cine short-axis images including both ventricles from base to apex (repetition time [TR]/echo time [TE], 64.2/2.97 milliseconds; slice thickness, 6 mm; flip angle, 18°; acquisition matrix, 256 × 192; field of view [FOV], 360 mm) and cine four-chamber images (TR/TE, 52.2/2.82 milliseconds; slice thickness, 8 mm; flip angle, 12°; acquisition matrix, 256 × 192; FOV, 360 mm) were acquired.
RHC
Subjects with PAH underwent RHC within 24 hours of CMR. Standard hemodynamic parameters were measured. Mean (end-expiratory) right atrial pressure, pulmonary capillary wedge pressure (PCWP), and pulmonary arterial pressure were recorded, and thermodilution cardiac output was obtained and reported as the average of at least three values with <20% variation. Mixed venous oxygen saturation was determined while patients were breathing room air. Heart rate and noninvasive blood pressure were recorded during the procedure. Stroke volume (SV), defined as cardiac output/heart rate; cardiac index, defined as cardiac output/body surface area; stroke volume index (SVI), defined as cardiac index/heart rate; pulmonary vascular resistance (PVR), defined as (mPAP-PCWP)/cardiac output; and RV stroke work index, defined as (mPAP–right atrial pressure) × SVI, were calculated.
Image analysis
Quantification of the RVF was obtained using commercially available software (Qmass version 6.2.2 and Mass 5.1, Medis, Netherlands).
2D analysis
Assessment of the RVF was performed using cine four-chamber images. TAPSE was calculated by measuring the displacement of the lateral tricuspid valve annulus toward the apex between end-diastolic (ED) and end-systolic (ES) phases (Fig. 1). RV fractional shortening (RVFS) was calculated as follows:

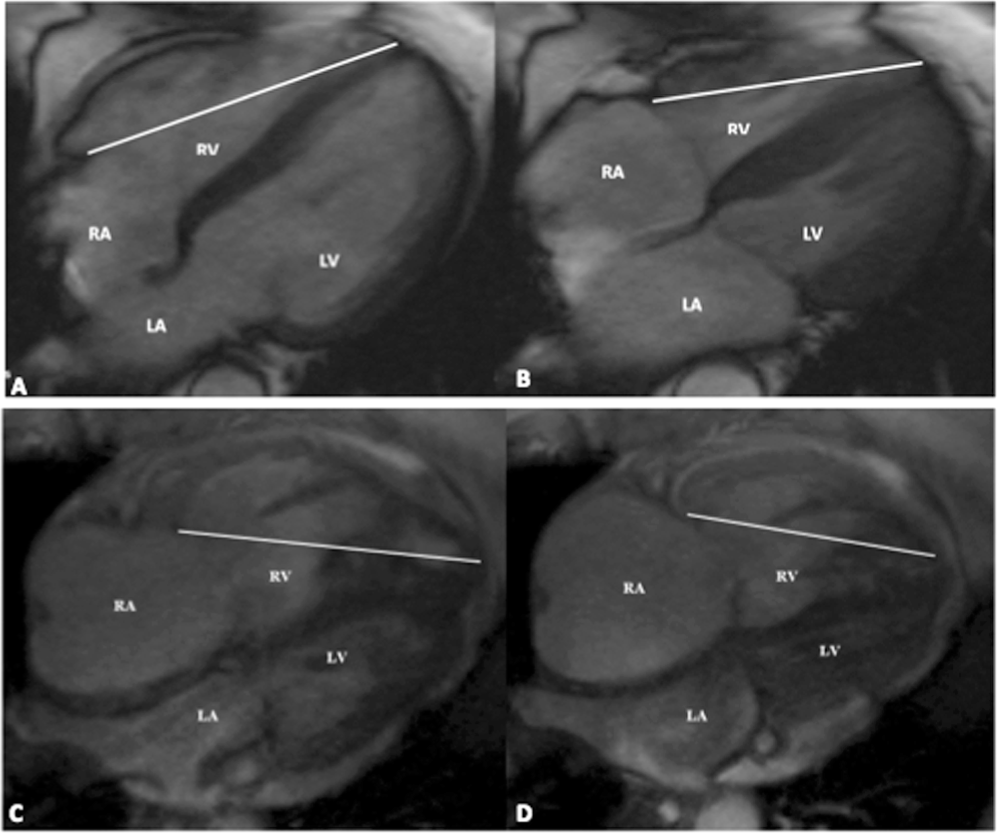
Fifty-year-old male (
Right ventricular fractional area change (RVFAC) was calculated by measuring percentage change as follows:
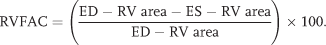
3D analysis
Assessment of the RVF was performed using contiguous cine short-axis images covering the entire RV and LV. The RV and LV epicardial and endocardial ventricular borders were manually contoured in end systole (smallest LV volume) and end diastole (largest LV volume) for functional analysis. Papillary muscles and trabeculations were included in the blood pool volume as described elsewhere.17,18 Morphologic and functional parameters were normalized to body surface area. RVSV and RVEF were calculated as SV = RVED volume - RVES volume, and RVEF (%) = (RVSV/RVED volume) × 100. Ventricular mass index (VMI) was calculated as the ratio between RVED mass and LVED mass.
Reproducibility analysis
A subset of 36 patients was analyzed by two readers (with 2 years and 8 months of experience in CMR, respectively). Imaging analysis time was recorded for each case. Intraobserver agreement for 2D and 3D measures was assessed by blinded repeat analysis of the images 1 month after the initial analysis by reader 1.
Statistical analysis was performed with MedCalc (Ostend, Belgium). Variables were summarized by mean ± standard deviation and were compared using independent
RESULTS
Forty-nine patients with PAH were enrolled. Table 1 summarizes the demographic characteristics, RHC data, and differences in 2D and 3D CMR measures between control subjects and subjects with PAH. Table 2 shows the relationship between 2D and 3D measures by CMR and hemodynamic measures by RHC. Table 3 shows the differences between CMR and RHC findings in subjects with scleroderma-associated PAH (SSc-PAH) and idiopathic PAH (IPAH). Patients with IPAH had higher mPAP at RHC (49 ± 14 mmHg vs. 39 ± 11 mmHg;
Demographic characteristics, hemodynamic test results, and cardiac magnetic resonance imaging (CMR) findings for patients with pulmonary arterial hypertension (PAH) and control subjects
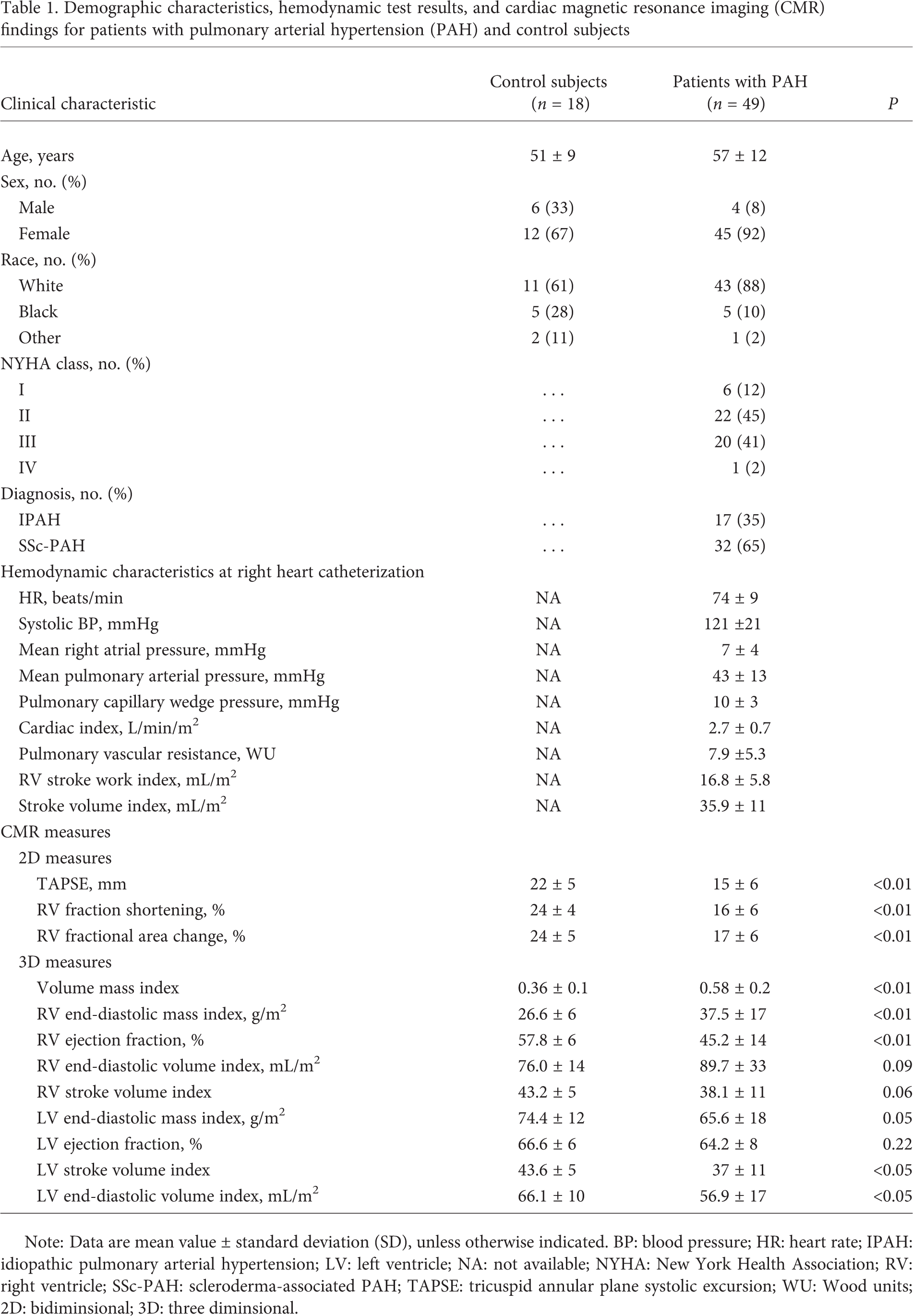
Note: Data are mean value ± standard deviation (SD), unless otherwise indicated. BP: blood pressure; HR: heart rate; IPAH: idiopathic pulmonary arterial hypertension; LV: left ventricle; NA: not available; NYHA: New York Health Association; RV: right ventricle; SSc-PAH: scleroderma-associated PAH; TAPSE: tricuspid annular plane systolic excursion; WU: Wood units; 2D: bidiminsional; 3D: three diminsional.
Correlation between bidimensional (2D) and three-diminsional (3D) volumetric cardiac magnetic resonance imaging measures and invasive hemodynamic parameters
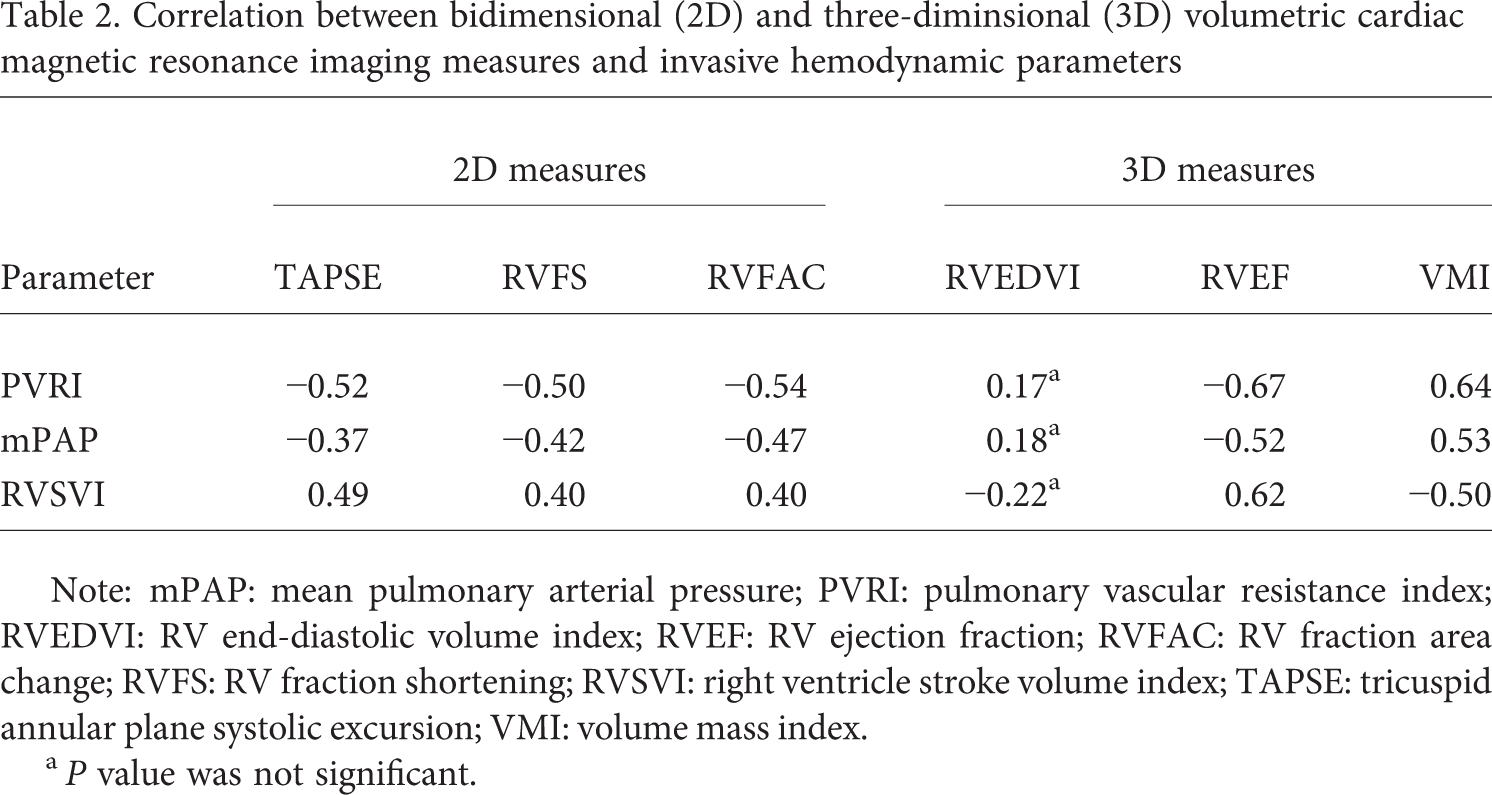
Note: mPAP: mean pulmonary arterial pressure; PVRI: pulmonary vascular resistance index; RVEDVI: RV end-diastolic volume index; RVEF: RV ejection fraction; RVFAC: RV fraction area change; RVFS: RV fraction shortening; RVSVI: right ventricle stroke volume index; TAPSE: tricuspid annular plane systolic excursion; VMI: volume mass index.
Differences between cardiac magnetic resonance imaging (CMR) and right heart catheterization findings in subjects with scleroderma-related pulmonary arterial hypertension (SSc-PAH) and idiopathic pulmonary arterial hypertension (IPAH)
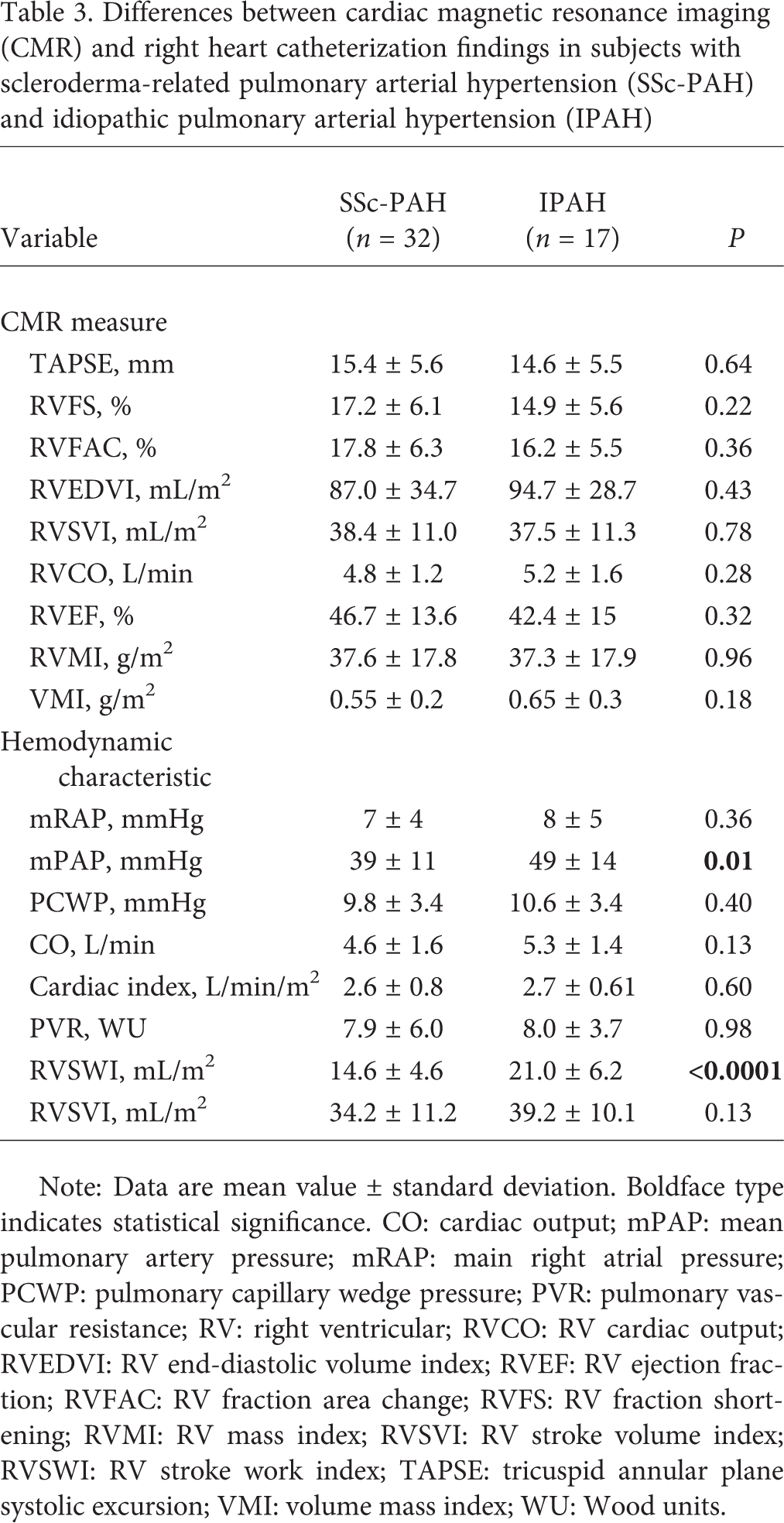
Note: Data are mean value ± standard deviation. Boldface type indicates statistical significance. CO: cardiac output; mPAP: mean pulmonary artery pressure; mRAP: main right atrial pressure; PCWP: pulmonary capillary wedge pressure; PVR: pulmonary vascular resistance; RV: right ventricular; RVCO: RV cardiac output; RVEDVI: RV end-diastolic volume index; RVEF: RV ejection fraction; RVFAC: RV fraction area change; RVFS: RV fraction shortening; RVMI: RV mass index; RVSVI: RV stroke volume index; RVSWI: RV stroke work index; TAPSE: tricuspid annular plane systolic excursion; VMI: volume mass index; WU: Wood units.
CMR and survival
Individuals with PAH were followed up for a mean of 2.5 ± 1.6 years after CMR evaluation. Twenty-one subjects (43%) died during this follow-up period. Univariate Cox regression analyses were performed to evaluate the relative strength of association of demographic, hemodynamic, functional, and morphologic parameters and treatment status with survival. Table 4 shows the strength of association of mortality with study parameters expressed as continuous variables. There was a significant association between mortality and age, New York Heart Association class, RHC measures of PVR and cardiac index, and all 2D CMR measures of RVF (TAPSE, RVFAC, and RVFS). Interestingly, there was a trend but not a significant association between mortality and RVEF or VMI. ROC curves were used to generate thresholds with the optimal sensitivity and specificity for prediction of death. The optimal ROC-derived cutoff values for prediction of death were 18 mm for TAPSE, 16.7% for RVFS, 18.8% for RVFAC, 44.1% for RVEF, 0.55 for VMI, and 37.7 mL/m2 for SVI. ROC curve analysis showed moderate-to-good prediction of mortality for TAPSE (area under the ROC curve [AUC], 0.77 [95% confidence interval (CI), 0.63–0.88]), RVFS (AUC, 0.75 [95% CI, 0.60–0.86]), RVFAC (AUC, 0.74 [95% CI, 0.60–0.86]), RVEF (AUC, 0.65 [95% CI, 0.50–0.79]), VMI (AUC, 0.59 [95% CI, 0.44–0.73]), PVR (AUC, 0.73 [95% CI, 0.58–0.84]), and SVI (AUC, 0.61 [95% CI, 0.46–0.74]). There were no significant differences between the AUC of TAPSE compared with RVEF (
Univariate Cox regression analyses to evaluate the relative strength of association of demographic, hemodynamic, functional, and morphologic parameters and treatment status with survival
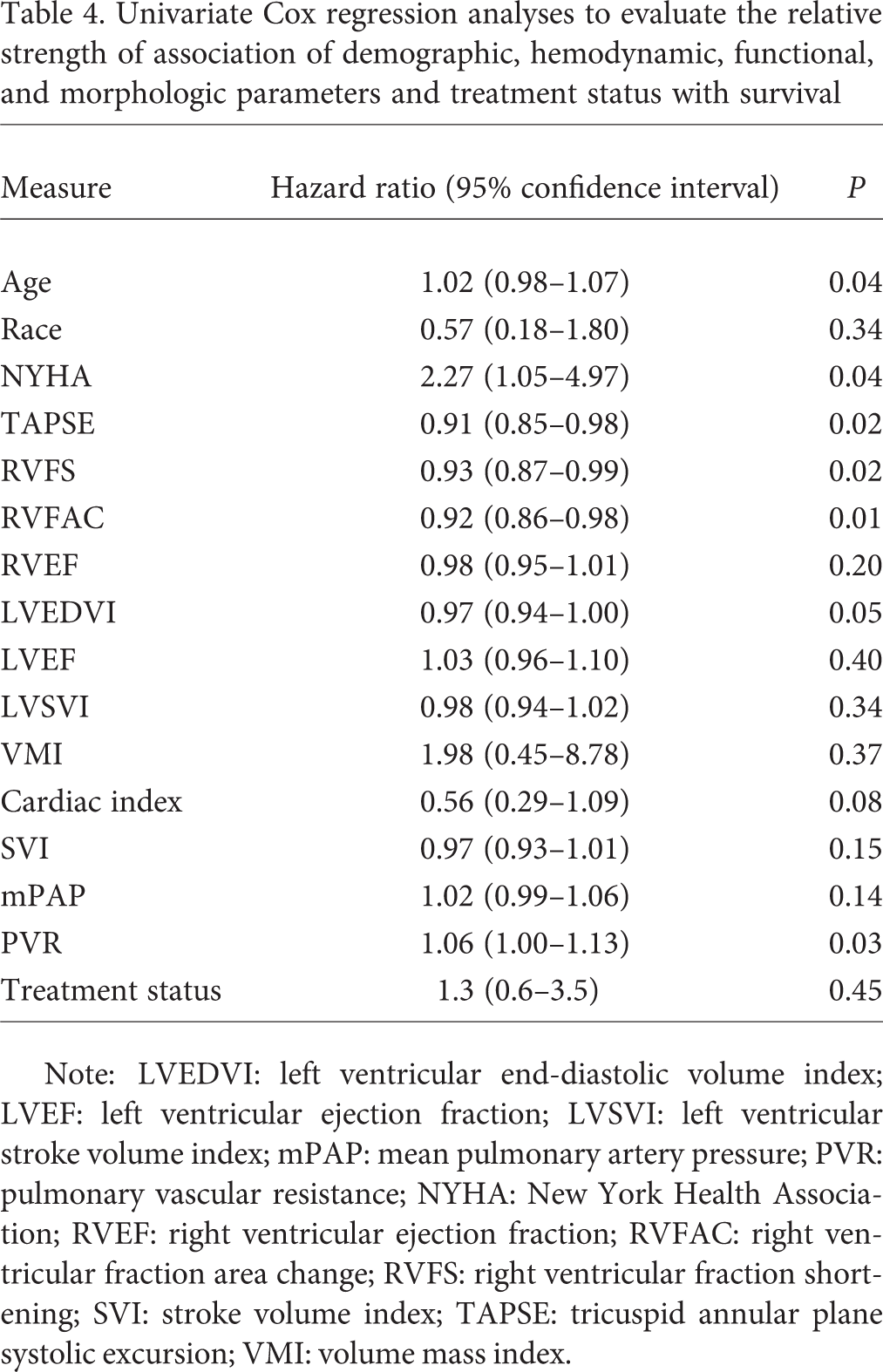
Note: LVEDVI: left ventricular end-diastolic volume index; LVEF: left ventricular ejection fraction; LVSVI: left ventricular stroke volume index; mPAP: mean pulmonary artery pressure; PVR: pulmonary vascular resistance; NYHA: New York Health Association; RVEF: right ventricular ejection fraction; RVFAC: right ventricular fraction area change; RVFS: right ventricular fraction shortening; SVI: stroke volume index; TAPSE: tricuspid annular plane systolic excursion; VMI: volume mass index.
Kaplan-Meier survival curves demonstrated good survival prediction for TAPSE and SVI using ROC-derived cutoff values. However, there were no significant differences in survival between groups separated by ROC-derived cutoffs for RVEF and VMI (Fig. 2). Univariate and repeated bivariate Cox regression analysis of dichotomized variables are shown in Table 5 and Table 6. TAPSE remained a significant predictor of mortality after adjusting for potential confounders.
Univariate Cox regression analyses to evaluate the relative strength of association of demographic, hemodynamic, functional, and morphologic parameters and treatment status with survival with variables dichotomized according to the optimal receiver-operating characteristic curve threshold for prediction of death
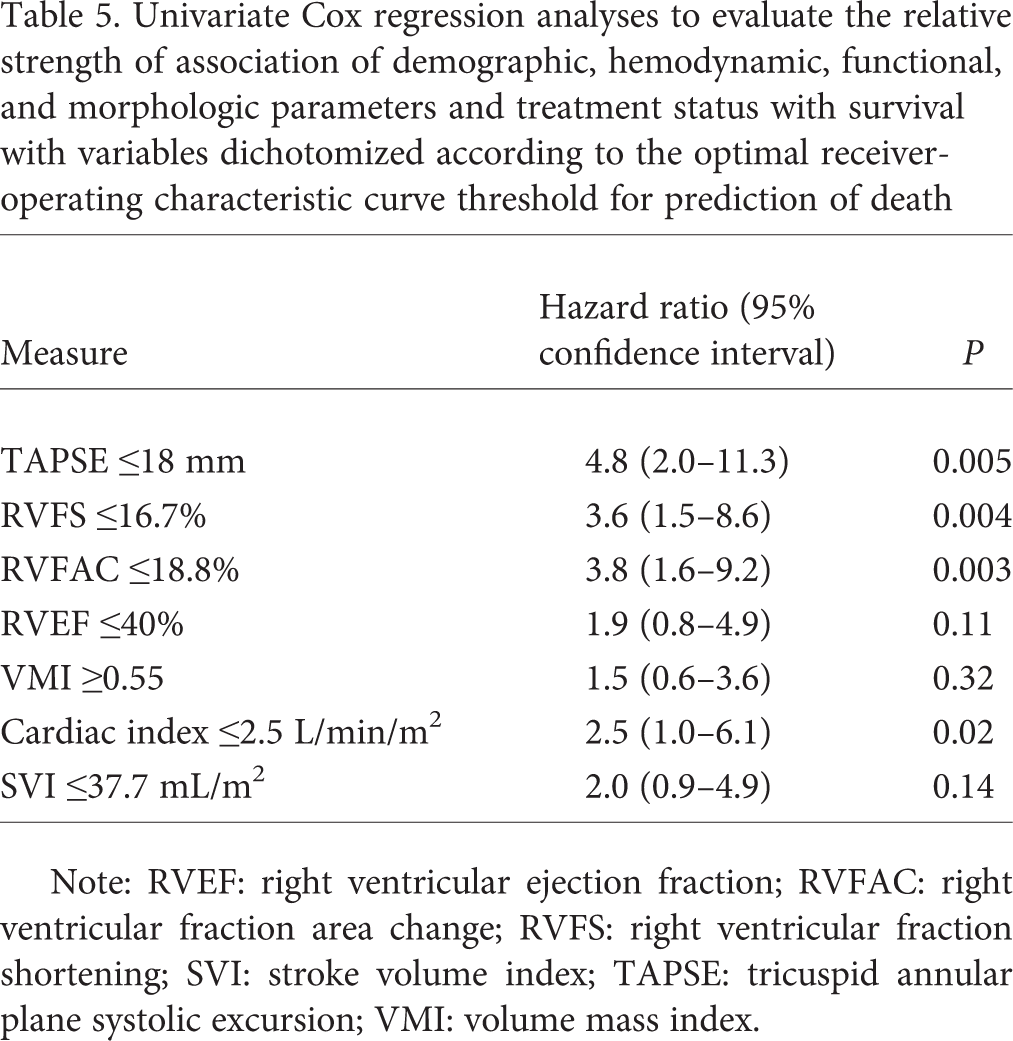
Note: RVEF: right ventricular ejection fraction; RVFAC: right ventricular fraction area change; RVFS: right ventricular fraction shortening; SVI: stroke volume index; TAPSE: tricuspid annular plane systolic excursion; VMI: volume mass index.
Repeated bivariate cox regression models for risk of death in the cohort
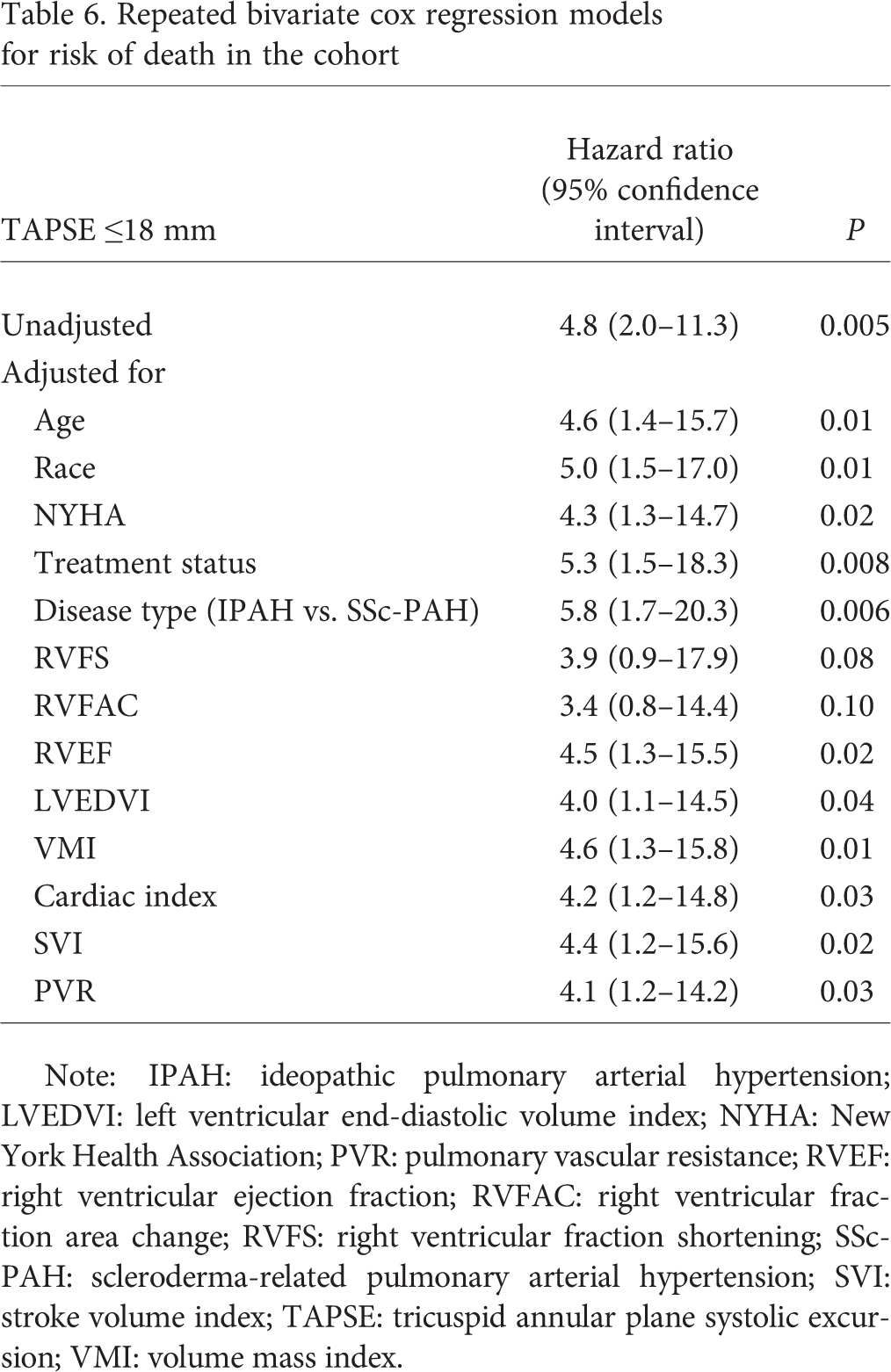
Note: IPAH: ideopathic pulmonary arterial hypertension; LVEDVI: left ventricular end-diastolic volume index; NYHA: New York Health Association; PVR: pulmonary vascular resistance; RVEF: right ventricular ejection fraction; RVFAC: right ventricular fraction area change; RVFS: right ventricular fraction shortening; SSc-PAH: scleroderma-related pulmonary arterial hypertension; SVI: stroke volume index; TAPSE: tricuspid annular plane systolic excursion; VMI: volume mass index.
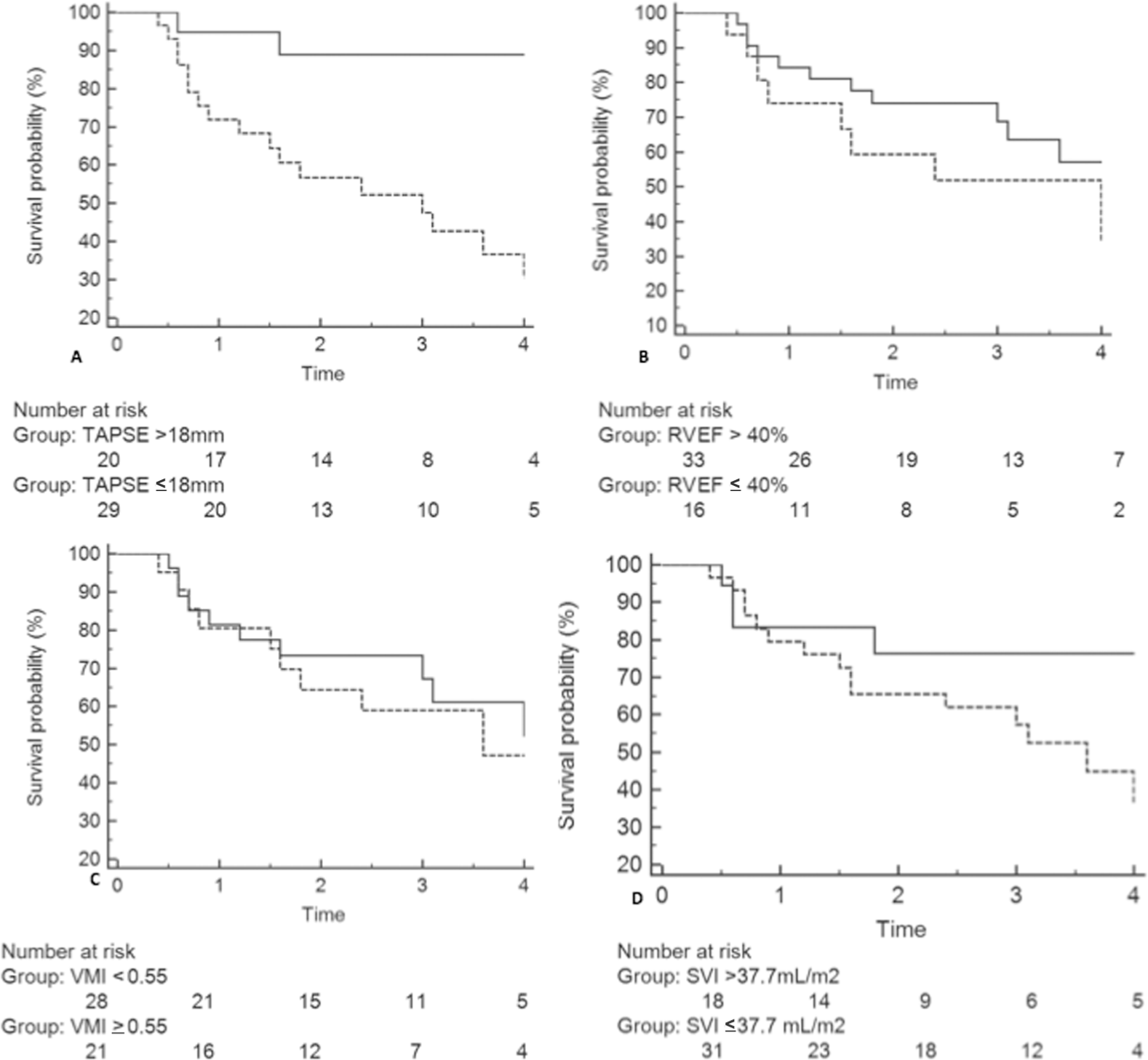
Kaplan-Meier survival curves in a cohort of 49 patients with pulmonary arterial hypertension for both two-dimensional and three-dimensional cardiac magnetic resonance imaging (CMR) measures.
Treatment
Although all patients received PAH-specific therapy on the basis of our program treatment protocol during the follow-up observation period, 15 patients (31%) were treatment naive and 34 patients were receiving treatment within 3 months before baseline CMR. All treatment-naive patients had SSc-PAH, and 8 had TAPSE <18 mm. Of the 34 treated subjects, 19 received single-therapy (prostacyclin [PGI2], 1 patient; calcium channel blockers [CCB], 2 patients; endothelin receptor antagonist [ERA], 5 patients; phosphodiesterase inhibitor [PDEi], 11 patients); 10 patients received dual therapy (ERA + PDEi, 9 patients; PGI2 + PDEi, 1 patient); and 5 patients received triple therapy (CCB + ERA + PDEi, 2 patients; ERA + PGI2 + PDEi, 3 patients). Direct comparison of survival in treatment-naive versus treated patients showed no difference in survival for treated patients (median survival, 4.3 years) compared with treatment-naive patients (median survival, 3.1 years;
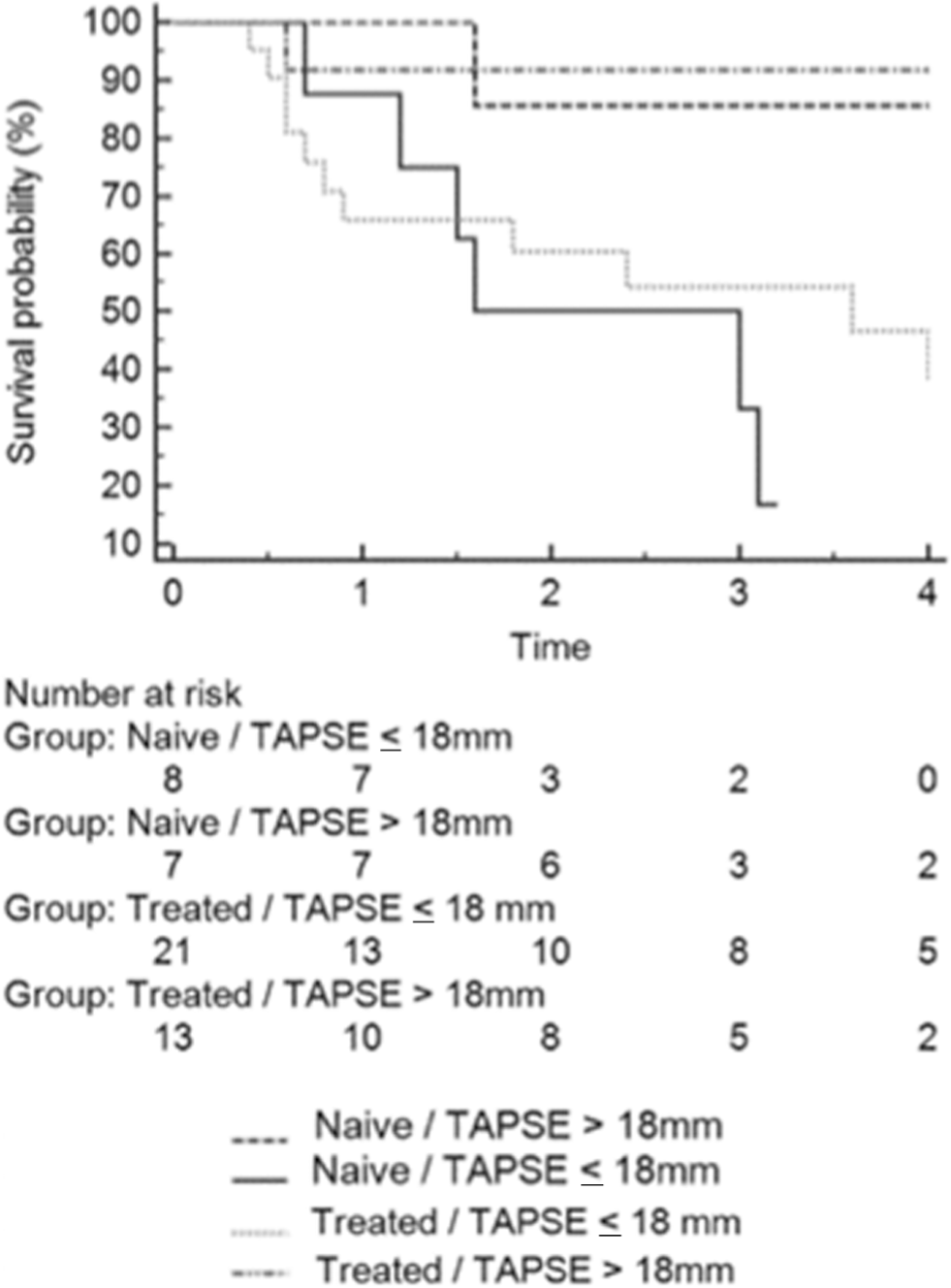
Kaplan-Meier survival curves for treated and treatment-naive patients with pulmonary arterial hypertension with respect to cardiac magnetic resonance imaging (CMR) categorized by tricuspid annulus plane systolic excursion (TAPSE) above and below 18 mm (
CMR reproducibility
Mean time imaging analysis for 2D measures was 90 ± 20 seconds per case compared with 25 ± 6 minutes for the 3D measures analysis. There was excellent intraobserver and interobserver correlation for TAPSE, RVFS, and RVFAC (intraobserver:
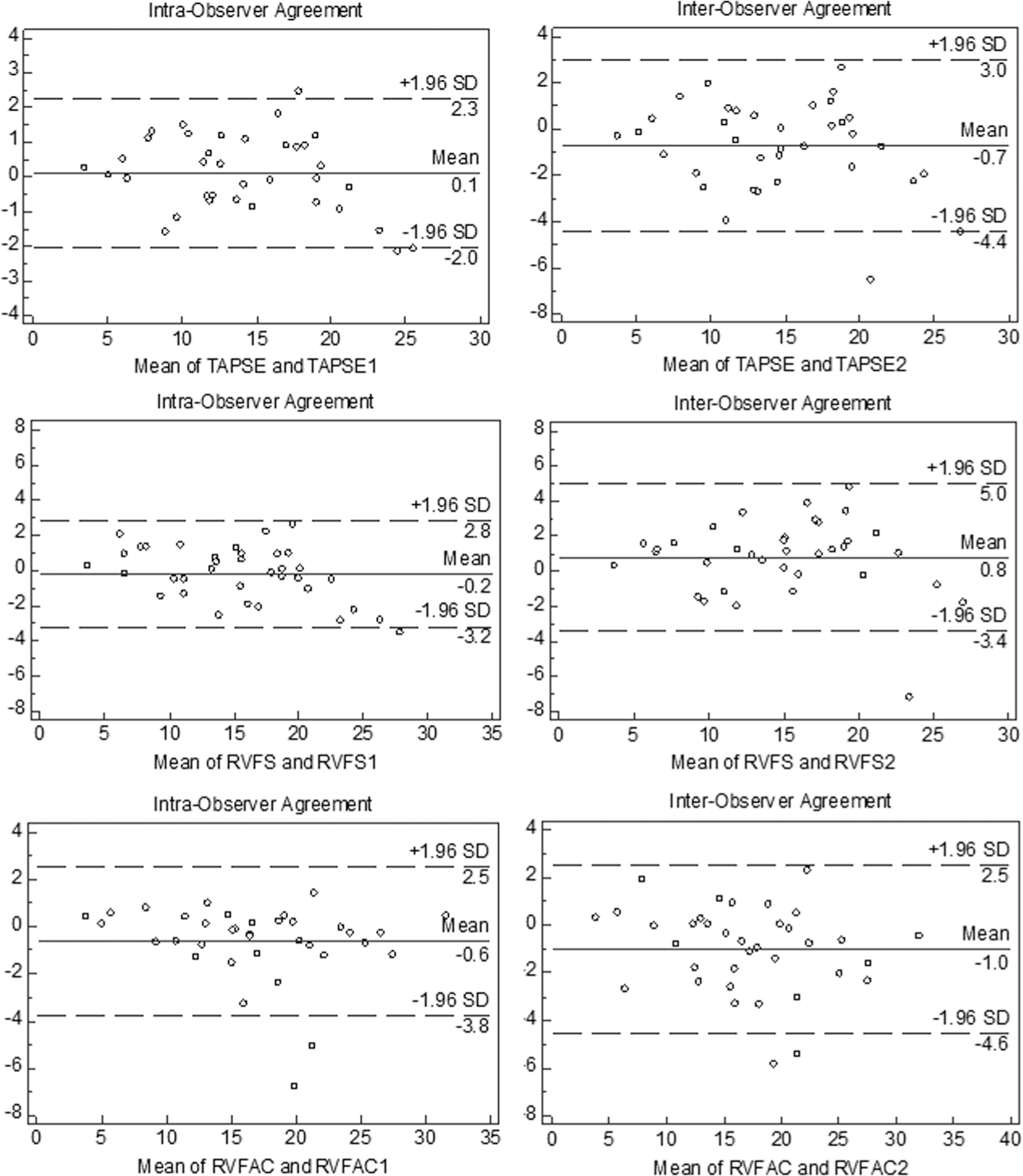
Bland-Altman plots demonstrate the intraobserver (tricuspid annulus plane systolic excursion [TAPSE] and TAPSE1) and interobserver (TAPSE and TAPSE2) agreement by two-dimensional assessment for TAPSE (mm), right ventricular (RV) fractional shortening (RVFS; %), and RV fractional area change (RVFAC; %). Horizontal solid line represents mean differences, and dashed line represents 95% limits of agreement. SD: standard deviation.
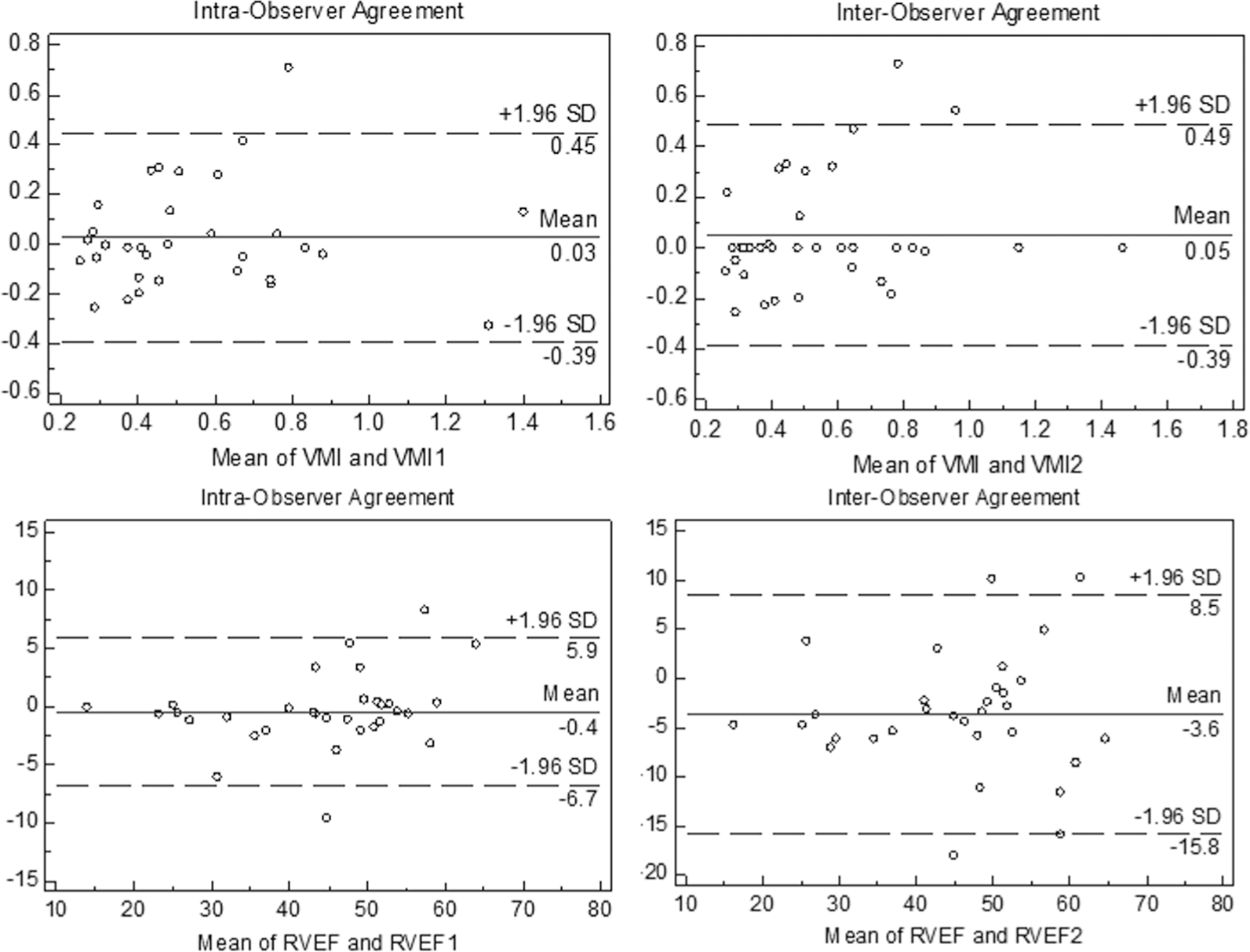
Bland-Altman plots demonstrate the intra- and interobserver agreement by three-dimensional assessment for ventricular mass index (VMI) and right ventricular ejection fraction (RVEF; %). Horizontal solid line represents mean differences, and dashed line represents 95% limits of agreement. SD: standard deviation.
DISCUSSION
In this study, we found that TAPSE, RVFS, and RVFAC by CMR were associated with invasive measures of pulmonary hypertension severity and RVF in patients with PAH. These 2D measures are reproducible strong predictors of survival, with significant time saving over 3D analyses.
Our results confirm that RV dysfunction is reflected by both 2D and 3D measures and that each modality correlates well with invasive hemodynamic measures of PAH severity. In our cohort, there was an inverse relationship between TAPSE and RV afterload, demonstrated by higher PVR in subjects with reduced TAPSE. TAPSE was shown to correlate with reduced RVSVI, which is comparable to a previous study showing that longitudinal RV displacement by echocardiography predicted a reduced RVSVI in patients with PAH. 7 This maladaptive RV response to elevated pulmonary arterial pressure is well described and is believed to be a major contributor to mortality in patients with IPAH and SSc-PAH. 2
CMR and survival
TAPSE obtained by echocardiography and VMI obtained by CMR have previously been shown to be predictors of mortality in PAH.7–9,13,14 We found that CMR-derived TAPSE measurements have similar prognostic value with improved survival prediction compared with VMI. An earlier study evaluating TAPSE by echocardiography has found an optimal cutoff point of 18 mm for survival prediction, 7 which is identical to our cutoff point of 18 mm derived from ROC analysis. In addition, other studies that have evaluated the use of TAPSE by CMR to diagnose pulmonary hypertension and to monitor RVF in acquired heart diseases have used similar cutoff points, ranging from 15 to 18 mm.15,21 In our cohort, TAPSE <18 mm was associated with a nearly 5-fold increased risk of death, whereas a 4-fold increased risk was associated with RVFS <16.7% and RVFAC <18.8%. This relationship persisted when adjusting for potential confounders such as age, treatment status, and disease type. Surprisingly, the association of TAPSE with survival remained even when controlling for invasive and noninvasive morphologic and hemodynamic measures previously demonstrated to predict outcome in PAH, such as RVEF, cardiac index, and SVI. Not surprisingly, TAPSE was also strongly associated with RVF, assessed by both RHC and CMR parameters.
Similar to earlier studies, we found a significant correlation of VMI with mPAP and PVR, both of which are invasive measures of PAH severity.14,22 Our VMI cutoff point of 0.55 is similar to that identified in earlier studies by Swift et al.
23
(0.4), Hagger et al.
14
(0.56), and Saba et al.
22
(0.6). Interestingly, in contrast to the earlier studies by Rajaram et al.
13
and Hagger et al.,
14
we found only a trend toward increased VMI and survival, which did not reach statical significance (
Treatment
Even though some patients were treatment naive at the time of CMR, all patients received treatment during the observation period. Therefore, it is not surprising that there were no significant differences in survival between groups. As expected, when we grouped our cohort according to whether they were treatment naive or treated and then stratified them by whether they had TAPSE above or below 18 mm, TAPSE remained a powerful survival predictor in both groups. Furthermore, TAPSE remained significantly associated with outcome when controlling for treatment status.
Reproducibility
Analysis of 2D measures by CMR took significantly less time than did analysis of 3D measurements (one-tenth of the time). These findings suggest the unique value of using TAPSE for rapid prognostic assessment in PAH compared with more labor-intensive 3D measures. The interobserver reproducibility between the 2D CMR measures was high with excellent agreement, consistent with earlier reports.12,15,21 Bland-Altman plots demonstrated low inter-and intraobserver variability, with limits of agreement (1.96 SDs) ±3–4 units from the mean for each measurement (±3.7 mm for TAPSE, ±4.2% for RVFS, ±3.5% for RVFAC). Intra- and interobserver agreement was slightly better for 2D measures than for 3D measures. Correlation coefficients for both RVEF and VMI were high; however, the 95% limits of agreement were broad (±0.44 from the mean for VMI, ±12.2% for RVEF), indicating a higher degree of variability for these measures. Although it is considered the gold standard for volumetric analysis for the RV, manual contouring of the RV cavity by CMR is more challenging than manual contouring of the LV cavity, as reflected by increased measurement variability. 24 This is in part attributable to differences in contouring of the highly trabeculated RV endocardial surface or differences in identification of RV chamber on short-axis views near the tricuspid annulus. 24
Our study has limitations. First, there was a relatively limited sample size; therefore, conclusions about the relative strengths of survival prediction for various measures are made with caution. Second, 71% of deaths occurred among patients with SSc-PAH; therefore, it is uncertain whether the ability of CMR TAPSE to predict survival is generalizable to all patients with PAH or has prognostic significance only for patients with SSc-PAH. It is not surprising that the deaths occurred in the SSc-PAH group, given the known higher mortality rates associated with SSc-PAH compared with IPAH. 25 However, an earlier echocardiographic study demonstrated the prognostic significance of TAPSE in a mixed cohort of patients with pulmonary hypertension, 6 and therefore, we suspect that the CMR results would have similar generalizability to all patients with PAH.
We did not measure transverse shortening of the RV, a 2D marker that has recently been suggested to have greater value for monitoring response to therapy and survival prediction than longitudinal shortening assessed by TAPSE. 26 However, we would suspect that changes in transverse shortening in our cohort would be reflected by differences in RVFAC. In our cohort, RVFAC was a strong predictor of survival, and its performance was similar to that of TAPSE.
Given the similarities between magnetic resonance imaging and echocardiography for survival prediction, one might argue against the merit of performing expensive and time-consuming CMR examinations for patients with PAH. Echocardiograms were unavailable to perform a direct head-to-head comparison with CMR for efficacy of survival prediction in our cohort; therefore, it is uncertain whether there are any differences between the two modalities in this respect. However, we believe CMR has several advantages, including more reliable evaluation of the RV due to a lack of user dependence, need for adequate imaging windows, and the ability to assess additional novel imaging biomarkers of RV performance. These include RV strain, pulmonary transit time, myocardial perfusion, and myocardial delayed enhancement.27–31 The relative importance of these biomarkers for treatment decisions and survival prediction remains an active area of research.
In this study, we evaluated outcomes in a cohort of patients that included patients receiving treatment and patients who were treatment naive. This is a potential limitation, because the imaging parameters discussed could have different prognostic ability in these two groups. Multivariate analysis was not performed for treated and treatment-naive subgroups separately because of the small sample size. However, we think it is probable that 2D measures of RVF are prognostically important in both groups, as indicated by Kaplan-Meier survival analysis performed separately for both groups (Fig. 3).
Conclusion
TAPSE by CMR is a simplified measure of RVF that can be obtained with high interobserver agreement and in significantly less time compared with labor-intensive 3D measures, allowing rapid assessment of RVF and patient prognosis. CMR measures of RVF and morphology are strong, independent predictors of survival in PAH and correlate with invasive measures of pulmonary hemodynamics.
Footnotes
ACKNOWLEDGMENTS
This work has been presented in part at the 98th Scientific Assembly and Annual Meeting of the Radiological Society of North America (Chicago, IL; November 2012), abstract 12032983; the annual meeting of the American Roentgen Ray Society (Washington, DC; April 2013), abstract E061; and the Royal Australian and New Zealand College of Radiologists’ 64th Annual Scientific Meeting (Auckland, New Zealand; October 2013), abstract R-0171.
