Abstract
Acute pulmonary hypertension leading to right ventricular failure and circulatory collapse is usually caused by thromboembolic obstruction of the pulmonary circulation. However, in rare instances, other causes can be associated with a similar clinical presentation. We present and discuss the clinical histories of two patients with acute right ventricular failure due to an atypical cause of pulmonary hypertension, disseminated pulmonary tumor embolism.
Keywords
The acute onset of pulmonary hypertension (PH) associated with right ventricular (RV) failure is generally caused by deep venous thrombosis followed by proximal embolization of the pulmonary circulation. Much less commonly, other pathological processes can result in pulmonary vascular occlusion and acute PH, as illustrated by the report of two patients with massive obstruction of the distal pulmonary vasculature by circulating tumor cells followed by acute RV failure and death.
CASE REPORTS
Patient 1 was a 67-year-old man with a history of nonmetastatic bladder cancer treated by cystectomy 9 months before presentation and a recent uncomplicated incisional hernia repair. He presented to a community hospital with dyspnea and general weakness. Physical examination, chest radiograph, and electrocardiogram findings and laboratory test results were unremarkable except for a urine culture positive for Escherichia coli. Treatment with oral ciprofloxacin was started. After 3 days, the patient's condition deteriorated, with worsening dyspnea and hypotension. Computed tomography (CT) of the chest was described as unremarkable and, in particular, ruled out pulmonary embolism or pneumonia. The patient was admitted to the intensive care unit (ICU) for possible urosepsis and was treated with piperacillin-tazobactam and norepinephrine. Because of further deterioration of his condition, he was transferred to our institution. On arrival, severe hypoxemia, lactic acidosis (lactate level, 15 mmol/L), and muscular exhaustion were noted, and urgent endotracheal intubation was required. The procedure was complicated by severe hypotension and pulseless electrical activity cardiac arrest. A transesophageal electrocardiogram (ECG) obtained during cardiopulmonary resuscitation (CPR) revealed massive RV dilatation. CPR was stopped after 45 minutes due to refractory cardiac arrest. Clinical diagnosis was cardiogenic shock due to acute RV failure of unknown etiology. Postmortem examination revealed innumerable carcinomatous microemboli massively showering pulmonary capillaries, which explained the resulting PH. As a consequence, myointimal hyperplasia and thrombosis of medium-sized arteries were observed, as was capillary congestion (Fig. 1A-1D). Tumor microemboli were also found in massively dilated hepatic sinusoids, the heart, the spleen, and the pancreas. Despite extensive sampling, tumor cells were found only within vessels, without any parenchymal infiltration. Tumor cells had stain findings positive for cytokeratin 7 and 20, compatible with an urothelial origin.
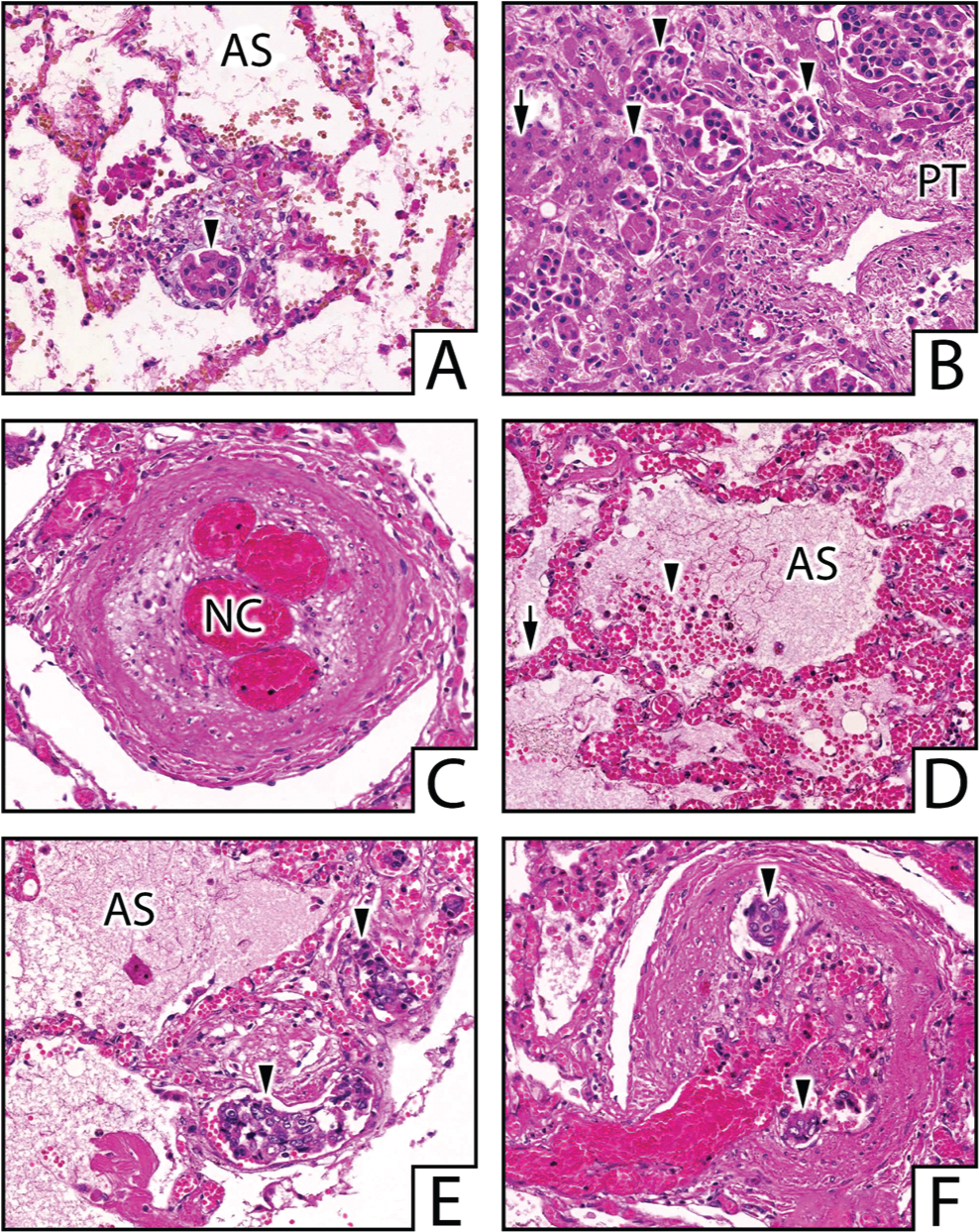
Disseminated tumor microembolisms in case patient 1 (A–D) and case patient 2 (E, F). A, Lung parenchyma showing alveolar spaces (AS) separated by alveolar septae, one of them being thickened by a dilated capillary containing a gland-shaped tumor embolus (arrowhead). B, Liver parenchyma showing a portal tract (PT) and normal hepatocytes (arrow). Sinusoids are massively dilated by tumor emboli (arrowheads). C, Lung parenchyma, showing a medium-sized arterial vessel with a recanalized thrombus with intimal neocapillaries (NC). D, Lung parenchyma with edema, hemorrhage (arrowhead), and hemosiderophages into AS. Alveolar septae show congestive capillaries (arrow). E, Lung parenchyma showing AS separated by alveolar septae being thickened by dilated capillaries containing multiple tumor microemboli (arrowheads). F, Lung parenchyma with a medium-sized arterial vessel showing a recanalized thrombus with intimal neocapillaries containing tumor emboli (arrowheads). All images stained with hematoxylin and eosin, captured at high magnification (400×).
Patient 2 was a 52-year-old woman with no relevant medical history. She presented with a 3-month history of weakness and diffuse back pain and was admitted for worsening dyspnea. Physical examination revealed a mass in the left breast. ECG and chest radiograph findings were unremarkable. Thoracoabdominal CT was negative for pulmonary emboli but revealed bilateral pulmonary interstitial infiltrates, liver nodules, and osteolytic vertebral lesions. Because of severe hypoxemia and hemodynamic instability, the patient was admitted to the ICU. Echocardiography revealed massive RV dilatation, and a pulmonary artery catheter demonstrated severe PH (mean pulmonary artery pressure, 57 mmHg) with low cardiac output (3 L/min). The patient was treated with inhaled nitric oxide, intravenous milrinone, and norepinephrine for rapidly worsening RV failure and refractory cardiogenic shock, which led to death after 3 days. Our clinical diagnosis was metastatic breast cancer with PH and acute RV failure of unknown etiology. Autopsy revealed a primary ductal breast carcinoma with widespread metastases. Similar to our first case, microscopic evaluation of the lungs showed massive obstruction of the distal pulmonary vasculature by multiple tumor microemboli, which provided the rationale for the acute RV failure (Fig. 1E, 1F).
DISCUSSION
Disseminated microvascular pulmonary tumor embolism usually has a fulminant course, 1 as illustrated by our two clinical cases. In this condition, pulmonary capillaries are obstructed by tumor cells. Secondary thrombosis of larger arteries as well as myointimal hyperplasia contribute to the resulting PH. 2 These irreversible changes lead to increased pulmonary vascular resistance and right heart failure. For the two patients whose cases are presented herein, most emboli seen on postmortem examination consisted of tumor cells, either isolated or in small clusters of 1–3 cells blocked in numerous alveolar capillaries. The overall tumoral circulating mass was thus important and involved all five lobes homogenously. Secondary arteriolar remodeling was present but played a limited role in vascular volume occlusion.
It is worth mentioning that many other mechanisms may promote the development of PH in patients with cancer, although none of these causes could be traced in our patients. First, cancer is a well recognized risk factor for chronic thromboembolic pulmonary hypertension. 3 Second, chemotherapy may induce PH, as illustrated by reports of severe precapillary PH induced by the tyrosine kinase inhibitor dasatinib 4 and of veno-occlusive diseases associated with various chemotherapy, including mitomycin, bleomycin, and carmustin as well as gemcitabine. 5 In addition, various chemotherapeutic agents, as well as radiation therapy, may elicit cardiotoxicity, resulting in left-heart dysfunction and postcapillary PH. 6 Also, pulmonary toxicity associated with various anticancer therapies can lead to altered lung function 7 and subsequent hypoxia-associated PH. Finally, mechanical compression of pulmonary vessels by metastatic hilar lymph node, which may increase pulmonary arterial pressure, has also been reported. 8
Disseminated pulmonary tumor embolism is a common autopsy finding in patients with cancer, but it is rarely diagnosed premortem. 2 It should be suspected in a patient with cancer who has dyspnea, hypoxemia, and unexplained PH. 9 Our two cases should be a reminder for the reader that such disease might occur in any patient with controlled or uncontrolled neoplasia. Contrast-enhanced CT and pulmonary angiography are not helpful to detect microemboli, and their negative predictive value is low. Ventilation and perfusion scans might be of interest; however, they are typically difficult to perform for patients whose conditions are unstable.10,11 Aspiration cytology of pulmonary arterial blood is invasive but may confirm the diagnosis in some cases. 12
Treatment possibilities for diffuse pulmonary vascular metastasis are extremely limited. Early initiation of targeted chemotherapy is the only therapeutic option. Although its efficiency remains very low, 13 favorable outcomes can be seen in highly chemosensitive tumors, such as choriocarcinoma or nephroblastoma. 14 In those cases, temporary cardiopulmonary support with extracorporeal membrane oxygenation may be discussed.
