Abstract
We aimed to adapt the shared medical appointment (SMA) model to the care of pulmonary hypertension (PH) patients and evaluate patient satisfaction. Our SMA team included a PH specialist, a PH nurse, and one research fellow. Eight to twelve PH patients with a family member were invited during office visits and by phone calls. Attendance was verified and encouraged by phone calls and informational letters. The meetings started with a 30-minute presentation on various PH topics, which was followed by each patient's individual visit and a focused examination in front of the group, allowing group questions and interaction. Of the total number of patients (
INTRODUCTION
Chronic illness is a major public health concern contributing to death, morbidity, and disability of many Americans. More than 90 million Americans are living with one or more chronic illnesses, and these chronic illnesses cause 70% of all deaths in the United States and account for more than 75% of the nation's medical care costs. 1
To better deal with chronic illnesses, shared medical appointments (SMAs) were developed by Dr. Edward Noffsinger at Kaiser Permanente Medical Center in San Jose, California, in 1996. The SMA is a model of care that involves multiple patients being seen as a group. It provides a unique way of delivering patient care in a group setting. Representing a biopsychosocial and multidisciplinary team-based approach to medical care, SMAs are meant to enhance quality and outcomes, improve patient-physician relationships, increase productivity and access to care, and enhance both patient and physician professional satisfaction. 2
As patients with chronic illness, pulmonary hypertension (PH) patients particularly require intense education, counselling, lifestyle modification, and complex pharmacological management, all of which take a significant amount of provider time. These interventions are difficult to achieve in the current healthcare system, where less time per patient visit is a result of increasing pressure on physicians. Historically, medical institutions have been structured to treat acute episodic health problems; however, they are poorly equipped to handle chronically ill patients who require complex services. 3 SMAs provide patients with increased interaction time with their provider. A group of 8–12 patients is able to spend 120 minutes (or more) interacting with their provider instead of the usual 10–15-minute individual appointment. SMAs incorporate all the components of individual appointments, including one-on-one medical evaluations, but allow more time for patient education and promotion of self-management.4,5 When group visits were provided to patients with inadequate insurance and type 2 diabetes, emergency department visits were significantly reduced. 6 Other researchers have also found a reduction in emergency care services after implementation of an SMA for diabetic patients and older, chronically ill health maintenance organization members.7,8 Moreover, in patients with heart failure, an SMA significantly improved postintervention knowledge scores and improved self-care compared with patients who received one-on-one care. 9
Although the SMA model has its roots in primary care, similar appointments can be offered in the milieu of specialty care for patients sharing similar medical conditions. In a 6-month, multidisciplinary, SMA approach for the care of heart failure patients, Lin et al. 10 showed that the enhanced counselling and patient education provided in these meetings significantly improved self-care and medication compliance and decreased the incidence of depression. In addition, enrollment in the cardiac rehabilitation program significantly increased, in large part because of patients describing the improvements in their quality of life after completing the program. The encouragement and positive reinforcement of the other members encouraged frustrated patients to continue with cardiac rehabilitation. In patients with chronic obstructive pulmonary disease, De Vries et al. 11 found significantly increased exercise tolerance after SMAs compared with that in patients managed by traditional office visits.
Because PH is a progressive disease with a profound impact on the life of patients and their family members and because of the previously mentioned possible benefits, we initiated the SMA model in our Pulmonary Hypertension Clinic. To our knowledge, this is the first time SMA is described in PH patients or other patients with rare pulmonary disorders. This article describes an adaptation of the SMA model to a rare pulmonary disorder as well as the study of this model for PH patients' care and its effects on patient satisfaction.
METHODS
We custom designed the follow-up SMA model to the needs, practice style, and patient constituency of pulmonary patients and specifically to PH. To the traditional 90–120-minute patient group visit, we added an educational session and a “questions and answers/support group” period.
The SMA team included a PH specialist, a PH nurse, and one research fellow. Two months before the first meeting, we secured administration support, drafted the necessary documents, and established the team roles, agenda, and census goal and enrollment strategy. Eight to 10 PH patients with their caregivers/family members were invited during office visits and by phone calls. The invitees were chosen mainly from established patients, with a few new patients each visit. Attendance was verified and encouraged by phone calls and informational letters, including a list of current medications to be updated by the patient. On the day of the meeting, vital signs were taken, and signed Health Insurance Portability and Accountability Act waiver consents were collected. The meeting started with a 30-minute presentation on various PH topics (Table 1). The physician then called each patient for an individual visit and a focused examination in front of the group (see Fig. 1). The focused exam consisted of a lung and heart exam without removal of clothing (dropping the stethoscope through the collar or from bellow the shirt); ear, nose, and throat exam as indicated; and evaluation of lower extremity edema. The physician directed the visit, allowing group questions and interaction. The next patient and caregiver were then called. The meeting ended in a casual, nondirected support-group-style lunch session, during which the team worked on fostering intergroup communication and sharing of experiences. A questionnaire was completed by the patients at the end of the meeting. The protocol was evaluated and approved by the Cleveland Clinic Florida Institutional Review Board (CCF IRB 9035).
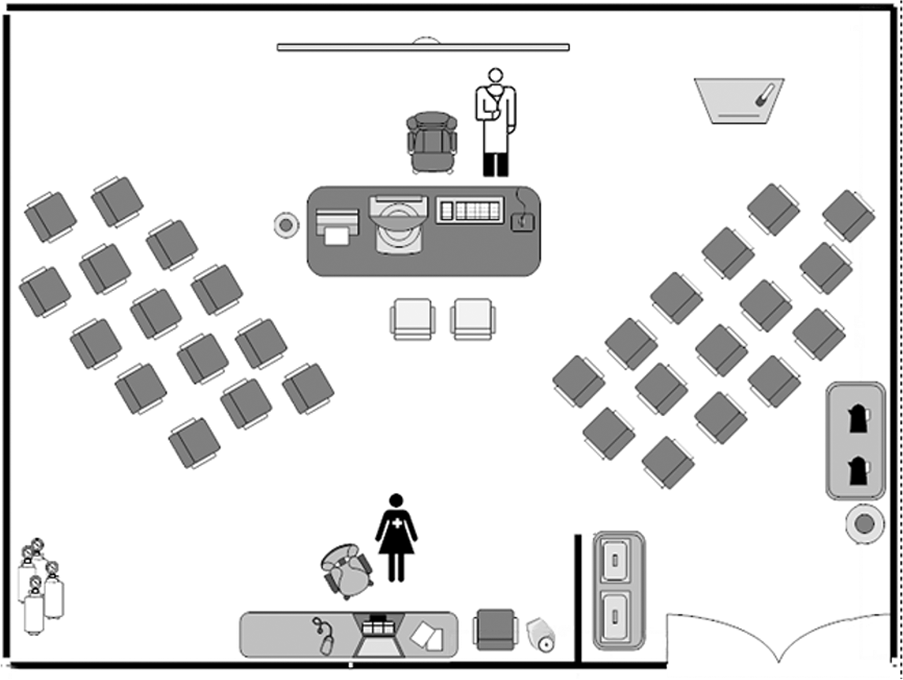
Setting of the room for the pulmonary hypertension shared medical appointment.
List of topics covered in a shared medical appointment

Actelion Pharmaceuticals US, 5000 Shoreline Court, Suite 200, South San Francisco, CA 94080, USA.
RESULTS
Seven separate SMAs were conducted in the Pulmonary Hypertension Clinic at Cleveland Clinic Florida over 10 months. The number of attendees was approximately 8–10 patients each month, and at our last four meetings the attendance rate was 100%. Eight to 12 patients were scheduled for each monthly visit, and attendance rates were between 71% and 100% for each visit. Eleven patients returned for a second SMA visit, and 3 returned for a third.
A total of 53 patients participated in these meetings (Table 2); the mean age was 65 years, and the majority were women (74%). Eighty-one percent of the participants were white, and 42% were receiving oxygen. Forty-four patients belonged to PH group I; of these, 23% had idiopathic disease, and 53% had PH related to connective tissue disease. Functional assessment of the patients at study enrollment, on the basis of World Health Organization (WHO) classification, was as follows: 6% class I, 36% class II, 43% class III, and 15% class IV. At enrollment, 15% of participants were on a one-drug treatment regimen, and 81% were on combination therapy. Twenty patients (37%) were receiving combination therapy with 2 different drugs, and 23 (43%) were receiving combination therapy with 3 different drugs. Of the patients receiving combination therapy, 93% were on a regimen that included a phosphodiesterase inhibitor, 81% were on one that included an endothelin antagonist, and 67% were on one that included a prostanoid.
Baseline characteristics of the study population
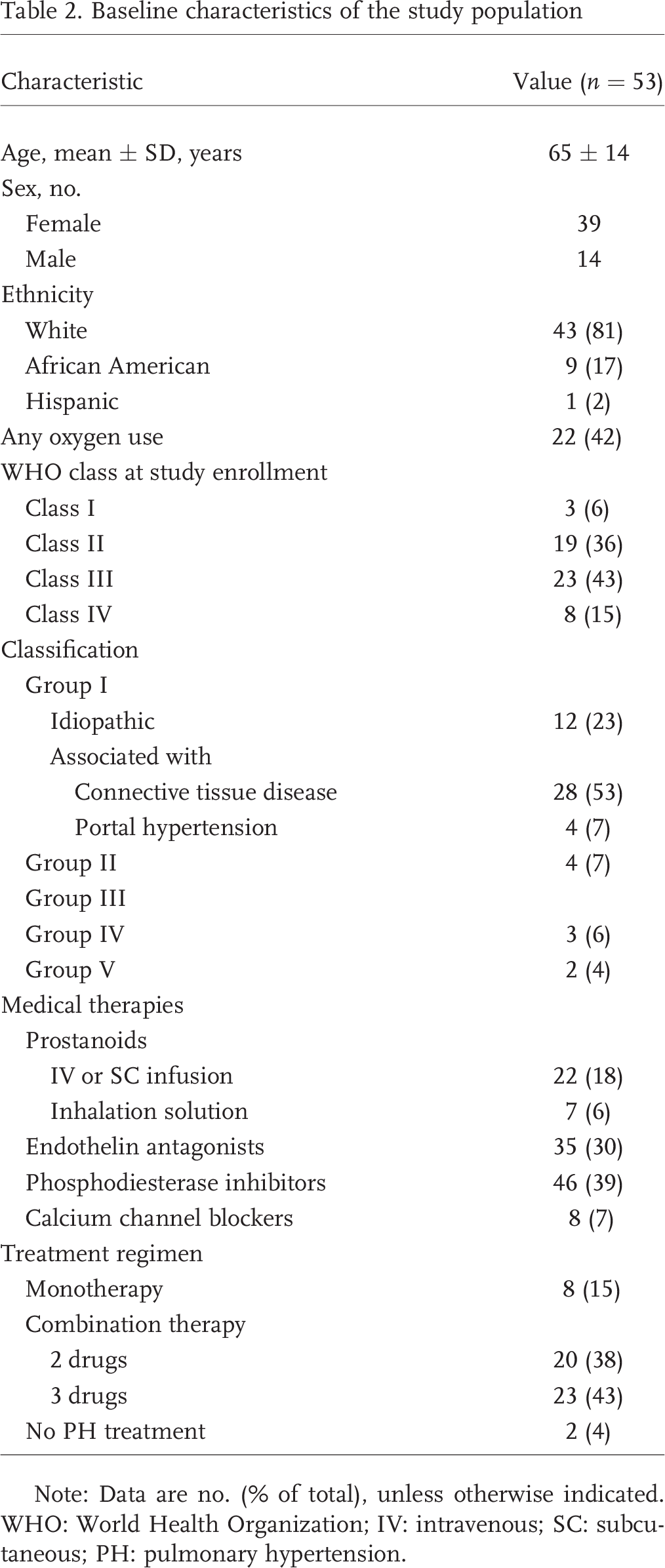
Note: Data are no. (% of total), unless otherwise indicated. WHO: World Health Organization; IV: intravenous; SC: subcutaneous; PH: pulmonary hypertension.
Previous knowledge of the group visit/SMA model was declared completely by 31%, to some extent by 38%, and very little to nothing by 35% of the patients. Of the total, 71% had only once or never met other patients with PH before coming to the group visit. Most of the patients were excited by (46%) or willing to try (52%) the new visit model, and none stated being doubtful or reluctant.
The majority of our patients expressed no concerns with privacy either before or during the meeting (76% and 88%, respectively). After the SMA, 63% of patients remained in the same category of concern. The 37% of patients who changed their degree of privacy concerns moved only one category, either downgrading (35%) or increasing (2%) their degree of privacy concerns (
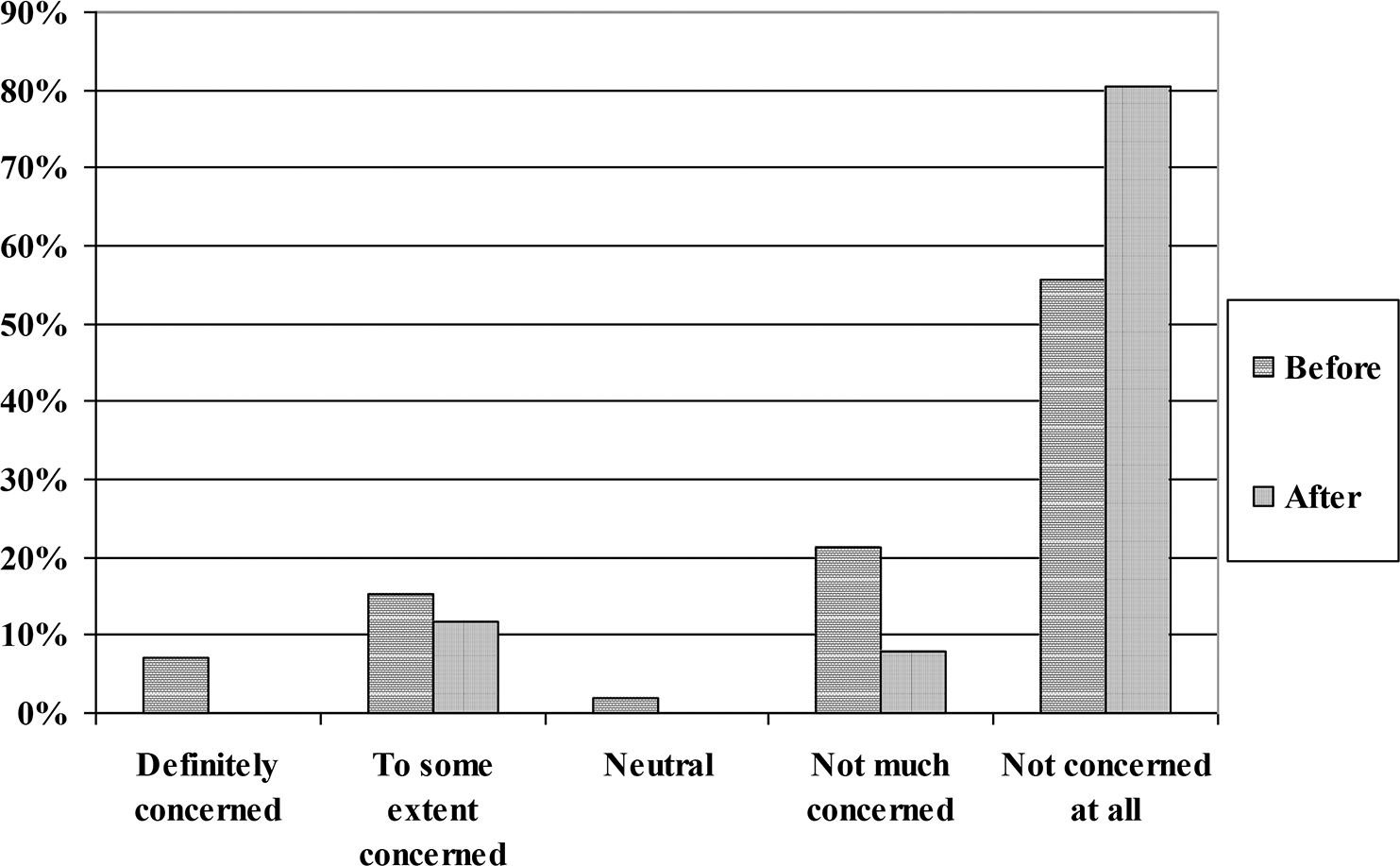
Privacy concerns before and after the pulmonary hypertension shared medical appointment.
Eighty-eight percent of participants stated completely liking the idea of receiving a lecture during the group visit, and 94% found the information received during the meeting useful; 100% acknowledged that they were given the opportunity to ask questions.
During the SMA, 96% of patients thought social interaction with other patients was facilitated. Sixty-nine percent declared that it was definitely easy to connect with other patients, 25% said that it was easy to some extent, and 6% said that it was somewhat easy.
When asked about improvement in their understanding of the disease because of being around other people with the same condition, 73% stated completely, 17% stated to some extent, and 2% stated somewhat yes. Only 8% did not find they had an improvement in their disease understanding by being with other people with the same disease. The likelihood of changing treatment on the basis of conversation with other patients was stated to be from very likely to likely to some extent by 25% and as unlikely by 45%, with 30% stating that they do not know or could not respond. Ninety percent of the patients thought that they learned from listening to other patients' experiences during the discussion of their cases with the physician.
Overall, the care provided was rated as excellent to very good by 98% of the patients. Ninety-four percent of patients declared that they would attend a future SMA (Fig. 3), with 59% stating a preference, either complete or to some extent, for the SMA over the private visit (Fig. 4).
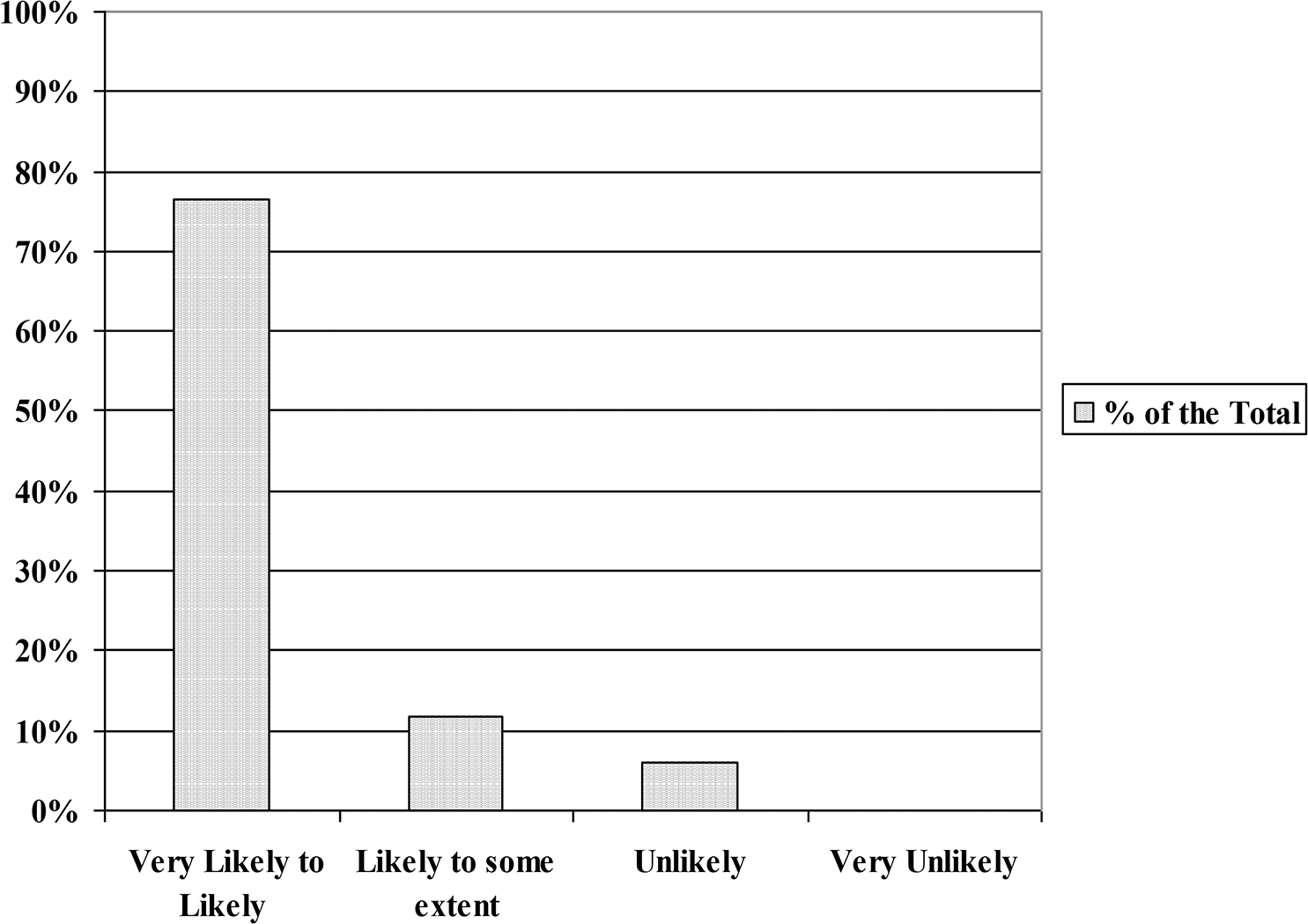
Likelihood of attending another pulmonary hypertension shared medical appointment.
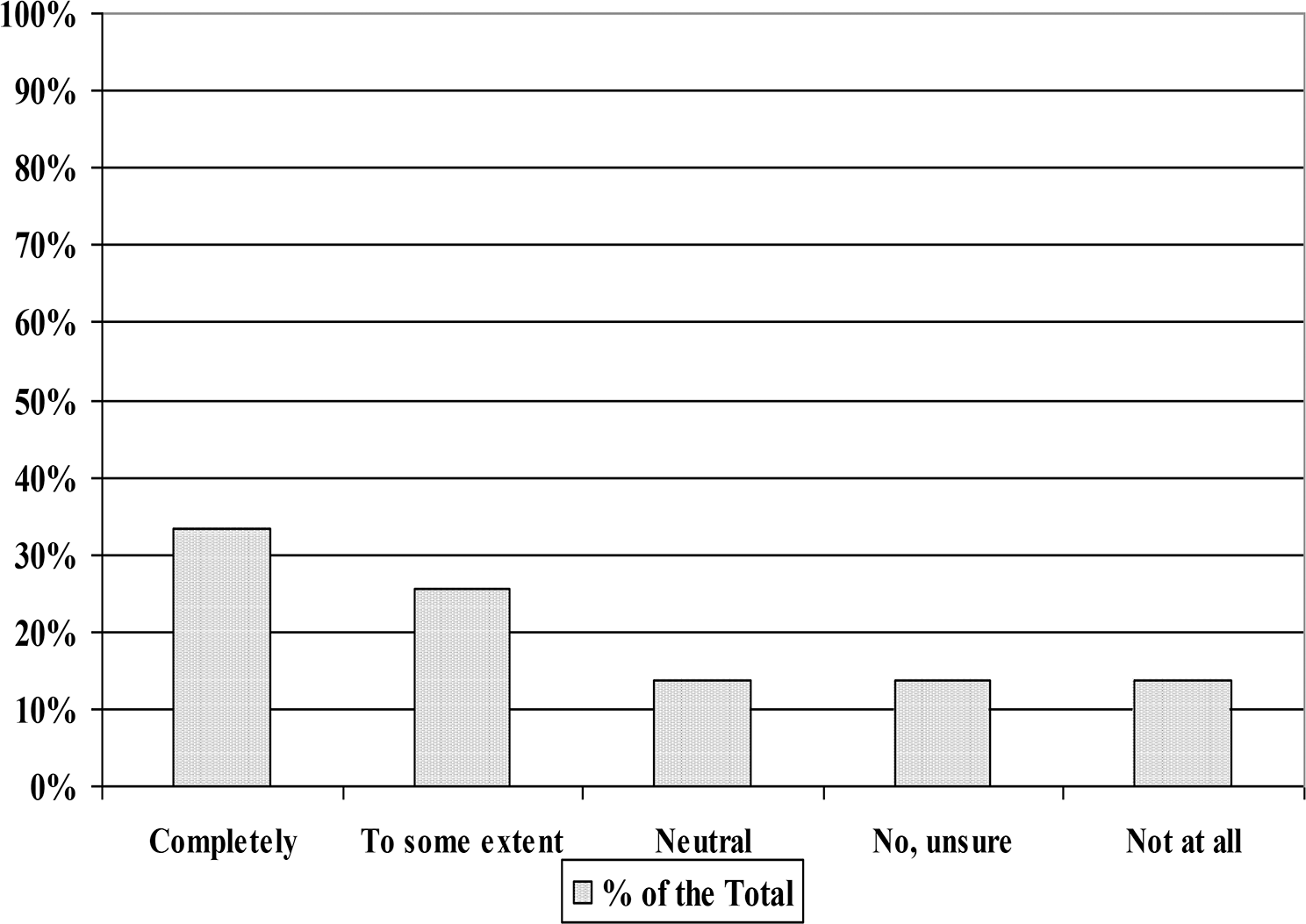
Preference for the pulmonary hypertension shared medical appointment over the private visit.
Most of our patients positively embraced the idea of trying this new type of visit, and most of the time no more than 15 patients needed to be contacted to schedule a total of 10 patients per visit. The maximum quantity of patients needed to be contacted at one time was 20. Approximately 5 of the contacted patients straightaway expressed disapproval of the SMA concept and did not agree to participate. The majority of the patients who denied participation expressed that it was due to the long distance to the clinic, unavailability of a family member or caregiver who could bring them to the appointment on the specific day of the SMA, or other personal commitments that precluded them from coming to an SMA on a Tuesday morning. The no-show rate was approximately 9%, which reflects our clinic's general patient no-show rating (10%). A comprehensive rating of the coordination of care, physical comfort, emotional support, quality of information, and length of visit of the SMA is detailed in Figure 5.
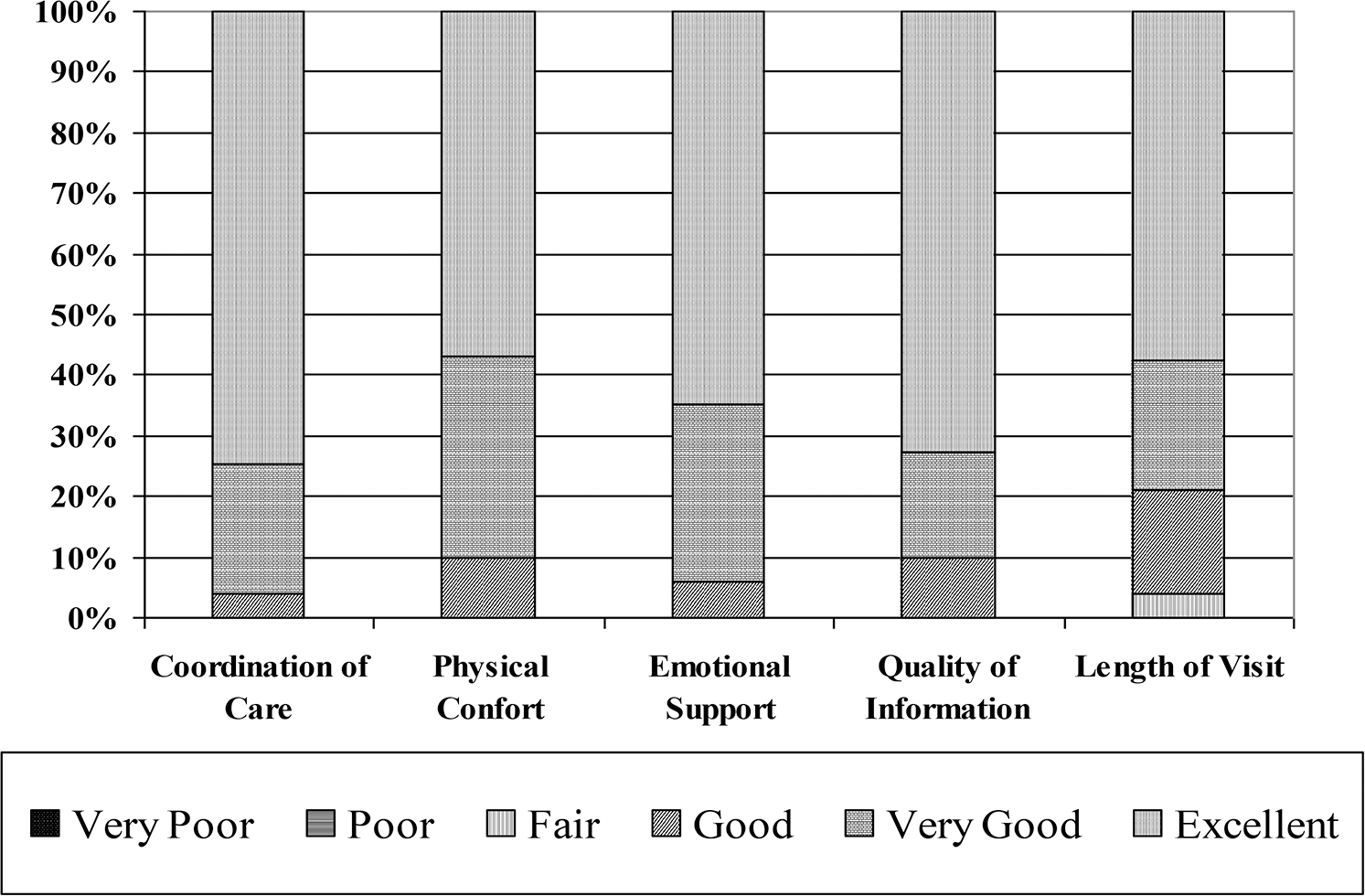
Comprehensive rating of the pulmonary hypertension shared medical appointment.
DISCUSSION
In this pilot project, we aimed to describe the implementation and efficacy of a group visit program in the case of a rare pulmonary disorder, PH. We assessed the patient's perceptions of the meetings to gauge satisfaction.
The SMA was well received by our PH patients. In spite of the availability of support groups locally, most of our patients declared not to know other patients with PH before coming to the SMA and thought that it was easy to connect with other patients and that social interaction was facilitated by this type of meeting. In addition, privacy concerns were not a significant detractor either before or during the group visits. These findings, in addition to the fact that the emotional support received during the SMA was rated as excellent by the majority of the participants, highlight the group visit as a useful venue to promote patient support in PH, especially for those who cannot or choose not to attend support groups.
We found that having PH patients with a wide variability of associated comorbidities and treatment modalities facilitated patient education during our group visits, as patients and family members actively joined the discussions most of the time. In this setting, the patients engaged each other to learn about their health issues by asking questions and participating in conversations with other patients who have similar issues. Our patients verbalized that after the SMA visit they felt better informed and more involved in their plan of care. One of the biggest challenges in the management of PH patients occurs at the time of advancing therapy or when transitioning to intravenous or inhaled prostacyclins. We found that 25% of patients declared that they would be very likely to likely to agree to change or to seek to change their medication regimens on the basis of interaction with kindred patients in the SMA. In practice, we have found it useful to send our noncompliant or hesitant patients to the SMA so they could see the consequence of advanced disease and also to allay some of their fears, particularly of the rare adverse events of liver toxicity of endothelin antagonists or the challenge of the use of inhaled, subcutaneous, or intravenous prostacyclins.
Here we studied the SMA in the context of a rare disease. The patients found particularly useful the education that was otherwise sparse in other healthcare settings and appreciated seeing other patients with the same disease, some for the first time. Other rare diseases in pulmonary medicine may benefit from this model, including α-1 antitrypsin deficiency, lymphangiomyomatosis, Wegener's granulomatosis, sarcoidosis, and idiopathic pulmonary fibrosis. Another use of the SMA can be in diseases where the same educational content is delivered repeatedly to different patients. In this context, perhaps the job of the physician is also made easier, with other benefits of the SMA—such as networking and peer support—also reaped by the patients. This would perhaps be seen in the treatment of obstructive sleep apnea, asthma, or chronic obstructive pulmonary disease, in which educating the patient about the disease is a big part of day-to-day private visits.
This study and the SMA model have significant limitations. Some conversations are meant to be had in private, and certainly we believe that this model of interaction with patients is best intermingled with regular private visits, where more sensitive personal and family issues can be addressed without fear of altered response by patients. It is probable that some relevant but embarrassing medical issues are withheld by patients in the SMA. Written comments were indeed submitted by the patients suggesting a preference for alternating private with group visits for their follow-up appointments. Learning to effectively deal with sharing confidential and personal health information can be tricky in the initial phases of appointments. Reassuring patients about the supportive environment can build participation.
Group visits are not specifically covered by Medicare and some private health insurance plans because billing codes for group visits are not established. While the Current Procedural Terminology Editorial Panel has suggested that physicians use the evaluation and management code 99499 (“unlisted evaluation and management service”) to report individual claims for Medicare patients participating in group visits, there are reports in the literature that this can be risky since it is a miscellaneous code for which no set value is assigned, and therefore it may not be reimbursed by insurers. 5 There should be no issues with billing each patient as an individual follow-up, as we did, and to bill according to appropriate levels of service delivered supported by adequate documentation. At our institution, 8–10 patients would have been seen during the 2.5 hours of the group visit, and in that sense no particular cost savings was accomplished. This may be achieved by attending to a greater number of patients at a lower billing.
This study focused on the responses of the patients who came to the appointments. Even though the majority of patients who declined the appointments did so because of logistical issues and previous commitments, certainly satisfaction of the patients who attended could suffer from selection bias. This logistical obstacle also presents as a limitation of the SMA model, as the offerings would almost certainly be limited to certain times during the week or more likely to some other specific recurring times and dates. We offer in Table 3 a stepwise approach to starting an SMA program. A more detailed description of the logistics, organization, and implementation processes of the SMA can be found in appendixes 1 and 2 (available online). Because of the duration of study and the numbers involved, it was not possible to evaluate the impact of the SMA on outcomes, including mortality or morbidity. SMA outcomes for other disease states have been reviewed elsewhere, revealing mixed but overall encouraging results. 12
Recommended steps to implement the shared medical appointment (SMA) model in the care of pulmonary hypertension (PH) patients

Overall, responses were very positive. This model allows PH patients to increase their understanding of the disease process while integrating peer support, promoting social interaction, and addressing patients' emotional needs.
Footnotes
ACKNOWLEDGMENTS
Dr. Franck Rahaghi, the principal investigator, had access to all the data and oversaw the integrity of data collection, analysis, and reporting. We thank the dedicated staff of the Cleveland Clinic Florida's Pulmonary Department, especially Deborah Schrager, Mark Hendrix, and Charlene Negron.
