Abstract
A 24-year-old female developed, in infancy, progressive right upper and lower limb muscle and soft tissue contractures and had a diagnosis of melorheostosis made on X-ray and pathological specimens. At the age of 11 years she began to have pain in the right hip and lower limb and this later became the dominant feature. She ultimately required amputation through the right hip joint and prosthetic fitting. She now has independent mobility with her prosthesis and has had no recurrence of pain. Her right arm remains flexed, shortened and contracted, but some hand function is retained. A review of the medical literature is discussed.
Introduction
Melorheostosis is a rare sporadic, bone dysplasia of unknown etiology and of variable severity. It usually affects one limb or part thereof. It manifests clinically during later childhood with subcutaneous tissue induration and dimpling of the skin, pain, joint swelling, contractures of the muscles and soft tissues overlying the affected bones and occasionally severe, articular ankylosis (Beauvais et al. 1977; Lateur 1998).
It has a characteristic X-ray appearance of irregular, hyperostotic changes of the bone cortex, usually on one side of the bone resembling melting wax dripping down a candle and the name is derived from the Greek melos for member and rhein for flow. This patient is unusual because she had multiple bones affected in both her right upper and lower limbs and pelvis and she required amputation. The authors can find only one other case report in the medical literature of melorheostosis affecting both the arm and leg and no reports of this condition in the prosthetic literature to date (Mariaud-Schmidt et al. 2002).
Case history
At birth this patient's limbs appeared normally developed and equal in length. However at the age of 5 weeks her mother noticed dimpling of the skin on her right thigh. As the months and years passed she was noted to have increasing right elbow, hip and knee flexion which progressed unrelentingly. She required an O'Connor extension prosthesis for the right leg at the age of 7-years. At the age of 10 years the right hip and knee were fixed in flexion at 55° and 65°, respectively and the foot fixed in equinus. Her right elbow was fixed almost in 30° degrees flexion with the forearm pronated and the fingers partially flexed.
During childhood she had x-rays taken which showed evidence of melorheostosis in her right hand, wrist, ulna, radius and humerus and also her hip, femur, tibia, ankle and foot. In addition there were foci in her left femur. (Figure 1). She developed thickened, shiny skin over her right thigh and right side of the abdomen. Otherwise her development was normal and she attended mainstream school.
At 16-years of age she had marked shortening of the right upper and lower limbs. The right sided contractures had progressed to such a degree that she was unable to derive benefit from the extension prosthesis, using instead a gutter crutch on the right and a standard crutch on the left with a swing through gait. The right hip and knee were noted to be in 80° and 90° of flexion respectively and the foot fixed in equinus. The right upper limb had 50 and 30° fixed flexion at the elbow and wrist respectively with the fingers significantly flexed. The skin over the right leg and abdomen was markedly thickened and taut. Neurological examination of the upper and lower limbs was normal within the range of muscle and soft tissue contracture. Debilitating, intermittent, sharp pain in the right leg, which had started at the age of 11 years, was becoming the biggest problem for her.
By the age of 17-years she was unable to lie on the right side and she was sleeping at night in a chair due to the severity of the pain and the posture of the right leg. The right thigh was swollen, pale and cold. She was regularly reviewed at both orthopaedic and pain management clinics. However, her pain worsened and in her own words she was “utterly miserable”. A Magnetic Resonance Imaging scan of the lumbosacral region showed no evidence of nerve entrapment. Her pain was not considered to be vascular in origin but more likely secondary to the bone involvement.
After much deliberation between the patient, orthopaedic surgeons, rehabilitation consultant and her clinical psychologist, a right hip disarticulation amputation was advised. In view of the significant fixed flexion at the hip joint a trans-femoral amputation would not have been of benefit to her. No guarantee could be given to the patient that this would resolve the pain. The amputation was carried out at the age of 18-years. Histology of specimens taken at the time of surgery showed irregular, dense, hyperostotic, cortical bone with loss of the normal architecture in keeping with melorheostosis.
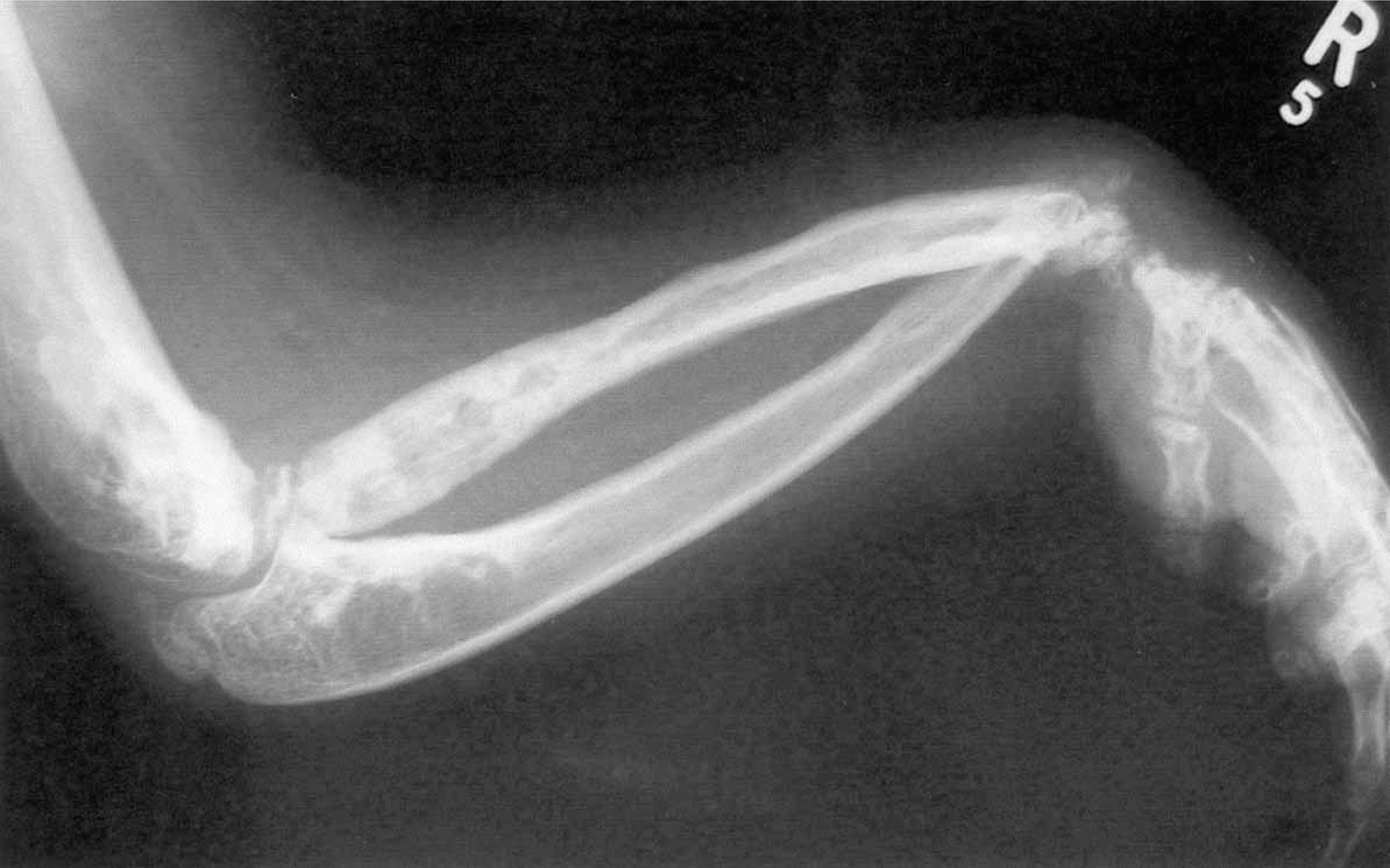
A plain X-ray showing the distal end of the right humerus, the radius and ulna and the hand. Note the irregular cortex: like candle wax dripping, clearly seen on the shaft of the radius bone.
Outcome
After the amputation she had complete resolution of her bony pain, although there was residual phantom pain which has been gradually resolving. She was fitted with a hip disarticulation prosthesis after 3 months.
She is now 24-years of age and she has only occasional phantom pains which she manages by resting. She can walk unaided for miles, SIGAM grade F (Ryall et al. 2003). She is now completing a higher university degree and she has no regrets about having the amputation.
Her right arm has never been painful and it remains fixed and contracted, but does not seem to be worsening. (Figure 2). She uses it in a functional way for carrying, feeding, and squeezing a toothpaste tube.
Discussion
Melorheostosis was first described by Leri and Joanny (1922) and it has also been recognized in antiquity (Leri and Joanny 1922; Kelley and Lytle 1995). Its severity can range from an incidental finding on an X-ray to severe deformity and pain. It is said to affect mainly the long bones of the upper and lower limbs and less frequently the hand and foot and very rarely the axial skeleton (Freyschmidt 2001). The diagnosis is typically made on X-ray and supported by histology. Computerized Tomography and Magnetic Resonance Imaging (MRI) are not usually needed, although a positive MRI result may obviate biopsy (Greenspan and Azouz 1999). Occasionally bone scintigraphy is needed to differentiate melorheostosis from other rare bone disorders like osteopoikilosis as the former shows increased radionuceotide uptake and the latter no increased uptake.

This picture shows the right arm in its relaxed position. Note the significant flexion at the elbow and wrist and three of the fingers.
It can coexist with changes in the overlying skin and malformations of blood vessels and lymphatics. This unusual condition can also be associated with nephrotic syndrome, carpal tunnel syndrome and renal artery stenosis (Roger et al. 1994; Igiesias et al. 1994). There is one report in the very recent literature of the occurrence of osteosarcoma in a melorheostostic femur (Murphy et al. 2003).
This patient has shown a severity of the condition not so far reported in medical literature with regard to the total dysplastic involvement of the bones of the right leg, right side of the pelvis, and the right arm and foci also in the left head of femur and left side of the pelvis.
This patient never had treatment, either bracing or surgery, for the contractures during childhood as it is not considered to be responsive to these measures (Campbell et al. 1968). Pain is not usually a significant problem in childhood but, as this patient has demonstrated, it can come on in later childhood and be the most disabling feature (Youngs et al. 1979). The pain can respond to simple analgesics, peripheral nerve blocks and even sympathectomy. This patient had initial benefit with simple analgesics and latterly Amitriptyline. Peripheral nerve block was considered, but this measure alone would not have given a successful long-term outcome as it was becoming clear that the right leg due to its flexed, cumbersome posture was inhibiting sleep, mobility and socializing and it would be better removed. The decision to proceed with amputation was deferred for several years, but this became the obvious treatment after many discussions with the patient.
This patient has had an excellent outcome from surgery and prosthetic fitting with total resolution of the pain and a high level of mobility reached.
