Abstract
We present a case report of a patient, affected by post-polio syndrome and cuff tear arthropathy of his right shoulder, who underwent reverse shoulder arthroplasty. A previous radial deficiency was unmasked in the post-operative follow-up, with passive elbow bending when the forearm was put in an antigravitational position. A precise preoperative neurological evaluation is mandatory in shoulder replacement in order to estimate the functional outcome after surgery.
Introduction
The reverse shoulder prosthesis was developed for the management of patients with refractory rotator cuff tear arthropathy especially with humeral antero-superior escape and pseudoparalysis.1 Reverse shoulder arthroplasty can restore shoulder elevation in case of severe deficiency of the rotator cuff. The contraindications known are: Non-functional deltoid muscle, insufficient glenoid bone stock, active infection, allergy to metals and severe neurological deficiencies.2 To our knowledge, there are few reports3,4 in the literature about patients with neurological deficiencies sustaining reverse shoulder arthroplasty. We present a case report of a patient, with previous history of poliomyelitis, who underwent reverse shoulder arthroplasty for severe cuff tear arthropathy.
Case report
A 73-year-old man, suffering from poliomyelitis during childhood, with a persistent deficiency of several muscular area of the right emisoma, developed a progressive debilitating pain and complete loss of function of right shoulder (dominant arm), in the last four years, with a painful pseudoparalysis in the last 12 months. X-ray, Magnetic Resonance Imaging (MRI) and electromyography (EMG) were performed to investigate the anatomic and functional patterns of the patient. Imaging showed a severe cuff tear arthropathy with humeral antero-superior escape and narrowing of acromion-humeral space (Figure 1); MRI showed a degenerated full-thickness tear of the rotator cuff with a still good quality of the deltoid.
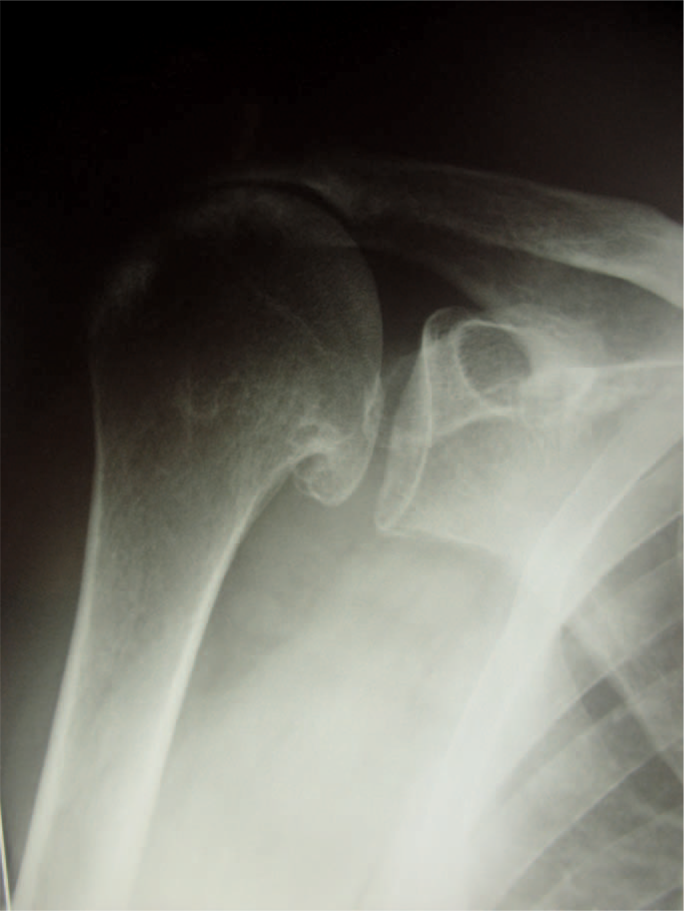
Severe rotator cuff arthropathy.
EMG showed a post-polio pattern with wide motor unit potentials and reduced recruitment in all muscle; ulnar, median and axillary nerve appears to have some preserved functionality, radial nerve was not investigated. Conservative treatment (physiotherapy, steroid injections, painkillers) did not get any good results. The patient completed several questionnaires (DASH5, SPADI6) to focus his functional status and symptoms, and was evaluated by performing the Constant Score7 and Simple Shoulder test.8
We considered two therapeutic options: Arthrodesis or reverse shoulder replacement.
The reason for performing an arthroplasty in this patient, instead of performing shoulder fusion, was based on the patient request to have a moving shoulder and some pain relief. Shoulder arthrodesis is not without its problems, with aching symptoms as a consequence of excessive use of the scapular stabilizing muscles and cervical arthritic symptoms.3 Furthermore, in the literature, shoulder fusion is indicated for a completely flaccid and afunctional arm;9 contrarily, in this case, function of deltoid and other muscle were preserved.
The patient underwent reverse shoulder arthroplasty (Delta III, De Puy, Leeds, UK, glenosphere 36 mm, cemented stem size 3, polyethylene cup +6 mm); intra-operatively we found a massive rotator cuff tear, involving supraspinatus and infraspinatus tendons: subscapularis and teres minor tendons were intact. The operative procedure was standard and the post operative X-ray showed good positioning of the implant's components (Figure 2). Post-operative rehabilitation started after two weeks, with progressive wearing off of the sling. The patient was physically and radiographically evaluated at 1 month, 3 months and 1 year after the operation.
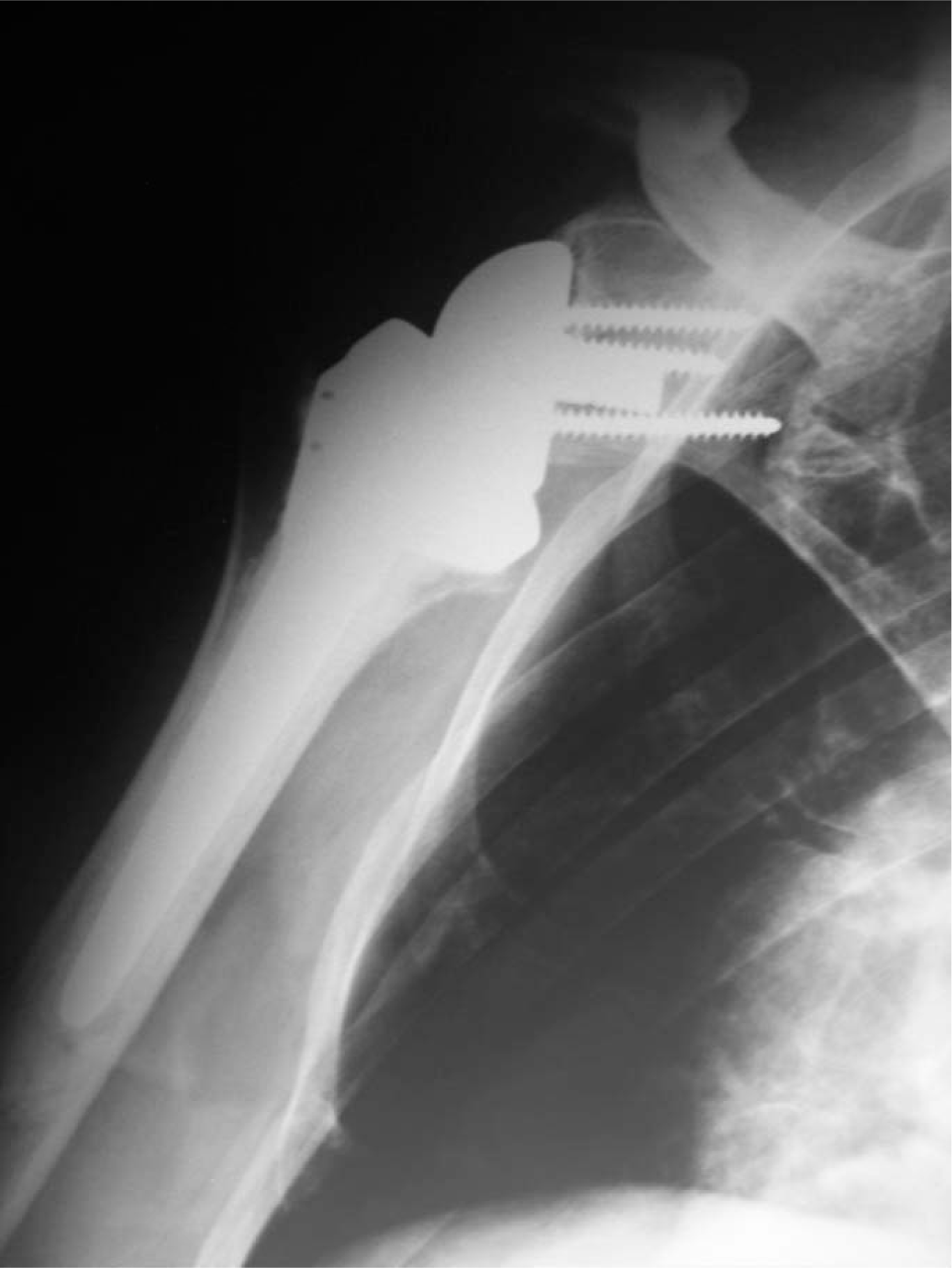
Post-operative X-ray shows good positioning of the components.
On the first clinical evaluation he reported a substantial relief of pain and improvement of function. On the second visit, progressing in physiotherapy, the patient reported an increase of shoulder range of movement, but was not satisfied about daily living activities, particularly in over-shoulder activities.
When asked to elevate his arm, the patient's forearm falls on his face, despite his attempts to keep his elbow extended, by external-rotation of the forearm (Figures 3 and 4).
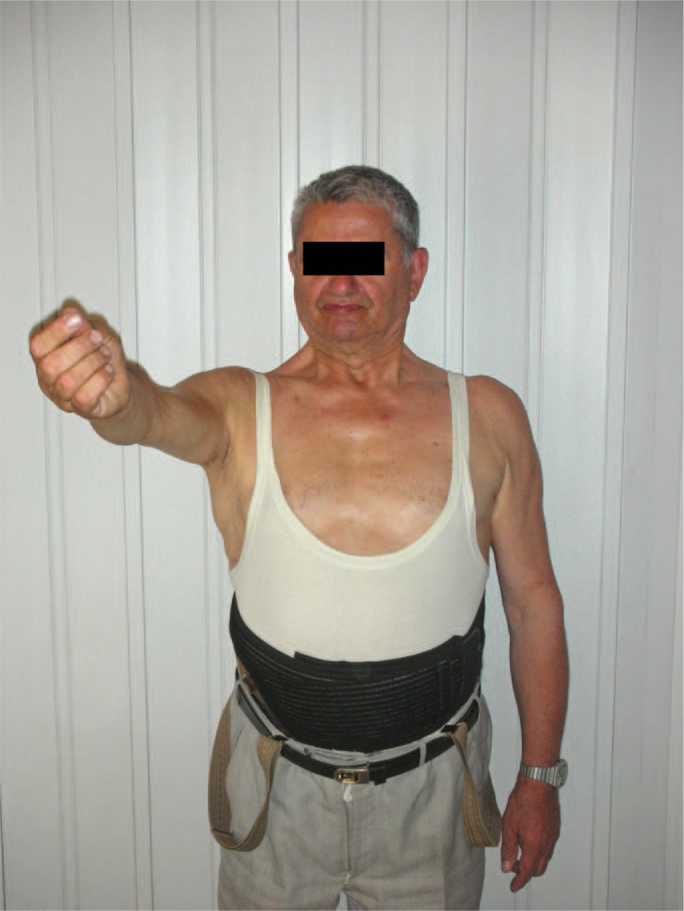
Patient extra-rotates forearm to avoid forearm-fall.
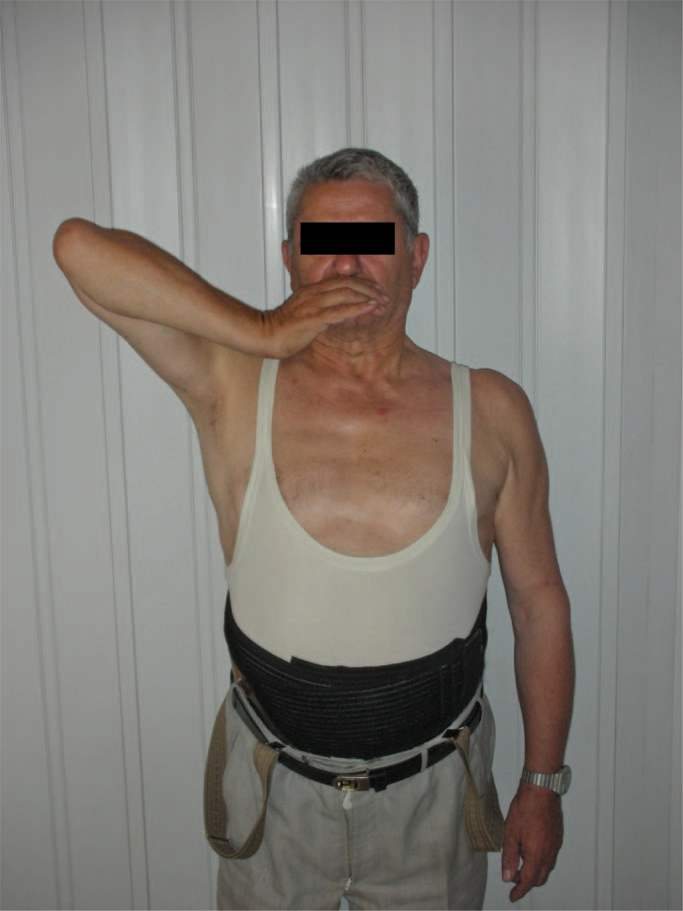
At more than 90° of elevation, forearm falls.
A clinical deficiency of the triceps was detected and a new EMG was performed showing a neurological deficiency of radial nerve.
The patient continued physiotherapy, with no substantial improvement of his disability after one month. After one year, the patient completed two self-administrated questionnaire (DASH, SPADI), Constant Score and Simple shoulder test. DASH improved from 72.6 to 55.3%; DASH-work improved from 70 to 45. SPADI score improved from 86 to 64. Constant score improved from 9 to 46 points. SST score improved from 0 to 3.
On clinical exam, the patient could elevate and abduct the arm 100°, normal internal-rotation (T12) and 5° of external rotation. His passive shoulder range of movement was complete and pain-free.
Discussion
Reverse total shoulder arthroplasty is becoming more and more popular, especially in Europe and recently in the United States. This treatment is currently considered to give superior functional results compared with other types of treatment for patients with severe cuff-tear arthropathy.10
However, because the rate of complications is higher than standard hemiarthroplasty and total shoulder arthroplasty, this procedure has specific indications that are important limits from the forensic point of view.11
Neuropathic arthropathy could be an indication for reverse prosthesis: In glenoid deformity secondary to brachial plexus birth palsy,12 this procedure has been used with good results.13
This case illustrates triceps muscle dysfunction as a possible factor that limits the outcome of patients with cuff-tear arthropathy, resulting in a persistent limitation of over-shoulder activities.
Neurological disease should be completely evaluated before surgery, but the presence of a radial nerve deficiency does not represent alone an absolute contraindication to reverse shoulder replacement.
In this case, the patient should be informed about the expected results he can achieve, pointing out the possible functional limitations due to his pre-surgery pathology.
If the objective of surgery is essentially pain relief, reverse shoulder prosthesis can be considered a proper solution and some kind of function improvement can be expected.
In our case, it was exactly this functional improvement that unmasked triceps disability; before surgery the patient could elevate and abduct his arm only a few degrees and the triceps was difficult to evaluate: The gravity was enough to extend the elbow. Pain also limited passive elevation and internal rotation of the shoulder, so physical examination was not completely helpful.
After surgery, he could move pain-free but triceps disability results in a passive elbow bending when the forearm is put in an anti-gravitational position (over shoulder). The patient was satisfied and did not want to undergo any other treatment.
In literature, an orthotic treatment (customized dynamic splinting) has been suggested for radial nerve palsy but was not requested in this case. The deltoid muscle is the engine of the shoulder reverse replacement, but the triceps is important too: Radial nerve dysfunction could limit the outcome of shoulder reverse arthoplasty even if it does not represent a contraindication. We do not know the amount of the risk of neurological damage during this procedure, but a tricipital deficit is as important as a deltoid disfunction for the outcome of the replacement. In our case the EMG confirmed that the triceps disfunction was a consequence of the polio disease and not of the surgery procedure; in fact, the absence of any neurologic deficit at the wrist and the hand confirms the origin of the symptoms.
In conclusion, a precise preoperative neurological evaluation is mandatory in shoulder replacement in order to estimate the functional outcome after surgery.
