Abstract
This retrospective file review outlines a case study of an 84 year-old man with a transtibial amputation for vascular disease who underwent an ipsilateral total hip replacement (THR). The question being addressed was how surgical techniques, rehabilitation processes and outcomes of joint arthroplasty would need to vary in a case of an ipsilateral dysvascular amputees. The surgery and associated rehabilitation was undertaken for groin pain, falls and reduced mobility due to mechanical osteoarthritis of the hip. The surgical technique and post-operative multidisciplinary rehabilitation is described in detail. Information on exercise regimes, length of stay and follow-up data on function, driving and pain management is presented. The literature is reviewed and all known cases of THR in amputees as well as data on survival of dysvascular amputees is presented. In light of advances in secondary prevention of vascular disease and cardiovascular surgical techniques, amputees with vascular disease may be living longer than they were 20 years ago. They may be beginning to experience the issues associated with aging such as osteoarthritis of the large joints. This case review and others in the literature may suggest that survival rates for vascular amputees be reviewed.
Keywords
Introduction
The median survival of atherosclerotic below knee amputees has been reported as 1 year and 6 months, and for those with amputation due to diabetes, 1 year 8 months (Pohjolainen and Alaranta 1998). This compares poorly with the 5-year survival rates of newly diagnosed breast cancer patients which in the 1990s was 84% (Webb et al. 2004).
The main risk factors for the development of mechanical osteoarthritis remain age, previous trauma or previous infection (Sharma et al. 2006). There have been reports in the literature of total hip replacements (THR) for amputees following trauma mostly on the contralateral side (Prickett and Scanlon 1976). Salai et al. (2000) reported five cases of ipsilateral THR in transtibial amputations, all for subcapital fracture, while Nejat et al. (2005) described five cases of THR in amputees, one for hip osteoarthritis in a dysvascular amputee on the contralateral side.
THR is a common procedure in the geriatric population and was first successfully performed by Charnley in the 1960s in the UK (Toledo-Pereyra 2004). According to the Australian Orthopaedic Association's Joint Replacement Registry (2005), 29,165 hip replacements were undertaken in 2003 – 2004 and 88.4% for primary osteoarthritis.
In the light of the poor survival of patients with dysvascular causes for their amputation it is unusual to see orthopaedic problems associated with aging. To our knowledge this is the first reported case of elective total hip replacement for ipsilateral primary osteoarthritis in a dysvascular amputee.
Case description
In June 2003, an 84-year-old right-handed war veteran was referred for severe right groin pain. His pain seemed to occur on weight-bearing, radiated down to the knee; he reported falls, and over the previous four weeks had mobilized only with the aid of a walking-frame.
He had a background of right below-knee amputation secondary to peripheral vascular disease (1983), perforated duodenal ulcer, well-controlled hypertension and gout.
The patient's premorbid level of functioning had been independent for all personal activities of daily living. He had assistance with heavy cleaning and vacuuming twice weekly and supervision for showering three times per week. He was independently mobile with a walking stick and used a Patella Tendon Bearing (PTB) prosthesis with SACH foot, endoskeletal shank and a pelite liner which was suspended with a prepatellar strap. He was able to don and doff his prosthesis independently, undertake all the instrumental activities of daily living and drove a modified vehicle.
On examination, he was 84 kg, his right hip was irritable and exhibited a restricted range of movement which included 0° internal rotation. Internal rotation of the hip reproduced his pain. X-ray and CT scan of the right hip showed marked loss of joint space in the superior aspect of the hip with subchondral cyst formation and sclerosis (consistent with advanced osteoarthritis).
He was commenced on oral non-steroidal anti-inflammatories and regular paracetamol, he had tight flexors of the hip which were stretched daily and weak gluteal and hamstring muscles which were strengthened. Ten days after admission, the patient reported less pain although his functional level had not changed. The patient was keen to avoid surgery, requested discharge home; however, over the ensuing 2 – 3 days at home the pain returned. He was readmitted for surgery.
A right total hip arthroplasty was performed three weeks after his initial admission (see Figure 1). A posterior surgical approach was used and large bearing metal-on-metal prosthesis was used (50 mm Birmingham Modular head). The choice of the hip prosthesis minimized the risk of dislocation and a surgical release of the psoas muscle was not undertaken. There were no post-operative complications.
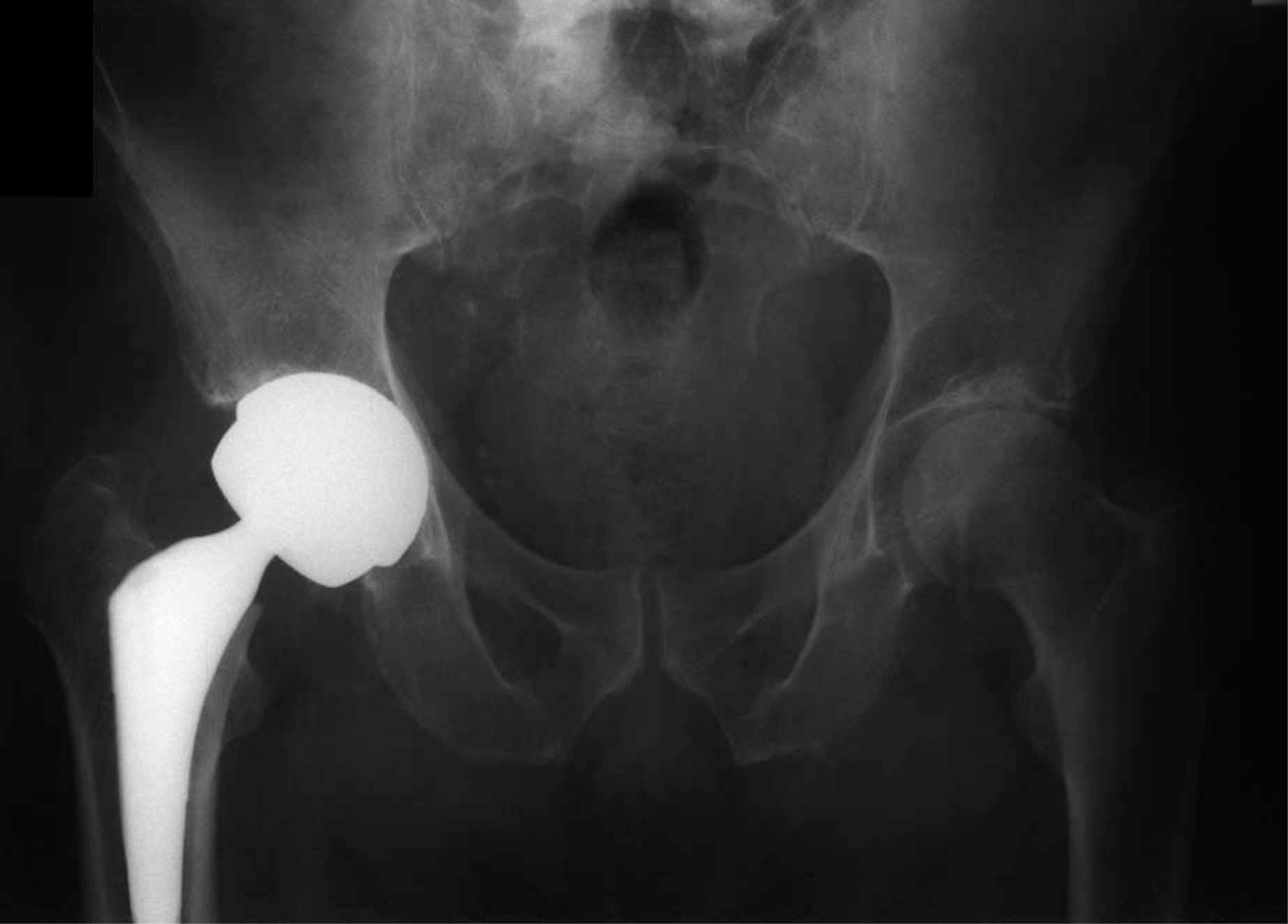
Metal on metal total hip replacement with 50 mm Birmingham modular head was chosen to minimise the risk of dislocation.
The patient was readmitted to rehabilitation on day 5 post-operatively and commenced gait retraining, progressing on to stair practice and endurance training. He was able to don his prosthesis on day 8 post-operatively and at discharge 30 days post-operatively, he was mobilizing with a pick-up frame and was able to undertake all premorbid activities independently.
Six weeks post-operatively the patient was mobilizing with a pick-up frame and a flexed posture, his walking speed has decreased from discharge. He demonstrated a 20° hip flexion contracture with a positive Thomas' test. At that stage he had limitation in all hip movements and he commenced a home-based physiotherapy program, focusing on prone lying, longer strides and increase in activity levels.
Three months post-operatively, he showed much improvement in gait with a walking-stick and his range of movement in the hip improved significantly with internal rotation 5°, external rotation 10°, abduction 35°, adduction 10°, flexion 95° and extension 20°. He no longer reported any pain.
Discussion
Current practice in Australia would favour conservative therapy in cases of high surgical risk such as the dysvascular amputee (Fleisher et al. 2006). Many may argue that pain killers and motorized mobility devices may have controlled this patient's pain sufficiently to preserve his quality of life and avoid surgery. However, in this case the patient opted for surgery.
In his Finnish series, Pohjolainen and Alaranta (1998) demonstrate the 12 months survival rate for vascular amputees as 43%, and for diabetic amputees it was 38%. In a Japanese study of 45 diabetic transtibial or transfemoral amputees 24.1% survived 3 years compared to 93% of those with foot or ankle amputations (Shirai et al. 2006).
Whilst there are no Australian figures available on mortality in vascular amputees, Australian patients with existing peripheral vascular disease, with an ankle-brachial index (ABI) of <0.9, had a 67% increase rate of cardiac death compared with an ABI of 0.9 – 1.4 (Norman et al. 2006).
It is interesting to note that most papers on ipsilateral or contralateral joint replacement in amputees are in patients whose amputation was due to trauma, congenital conditions or infection. Kulkarni et al. (1998) reported, in 44 traumatic amputees that 61% suffer osteoarthritis of the ipsilateral hip compared to 23% of the contralateral hip. This compared with 11% suffering hip osteoarthritis in the normal population.
Furthermore, Sadeghi et al. (2001) reports that abnormal activity of hip muscle in the amputee, during gait, may be responsible for changing forces across the ipsilateral hip joint. They note that, on the ipsilateral side, the hip flexors, extensors and external rotators become the main power generators while the abductors and adductors the main absorbers, in stark contrast to the contralateral side. This may explain the different rates of osteoarthritis identified by Kulkarni et al.
However, the poor survival rates of vascular amputees make total hip replacement for osteoarthritis in this group less common. Over the last 20 years, vascular amputees in developed countries have benefited from secondary prevention of vascular disease, improved cardiovascular surgical techniques, and a greater emphasis on exercise, so that many dysvascular amputees are enjoying improved survival rates (Trower 2006). As they survive for longer many vascular amputees are likely to face some of the musculoskeletal aspects of aging such as osteoarthritis (Fiatarone-Singh 2006).
In this case, the patient used a number of medications and non-medical techniques to minimize his risk of cardiac disease and stroke. He used aspirin and clopidogrel for cardiac/stroke prevention, his blood pressure was well controlled with a betablocker and his cholesterol was controlled with pravastatin. Furthermore, he had a supportive family who were proactive regarding his disease prevention, he was an active prosthetic user and maintained his weight to below 84 kg (with prosthesis) and BMI below 25.
The post-operative rehabilitation of an amputee with an ipsilateral hip replacement needs to address the likely development of contractures at the hip and knee. The pain of osteoarthritis is likely to have minimized this patient's desire and ability to walk forcing him to be chairbound most of their day. A focus on the stretching of the hip flexors and knee extensors needs to be added to the usual regime for post-total hip replacement physiotherapy. Gait is an important factor to consider as the optimal premorbid gait may not have been limited by pain for 3 months. Pain levels at the hip will inhibit stride length and hip extension in the hip replacement population (Nikolajsen et al. 2006); one would expect that in amputees this will have an accentuated affect on gait (Schmalz et al. 2002).
Conclusion
To the authors' knowledge this case represents one of the first case reports of ipsilateral hip replacement in a below knee amputee of vascular origin. As increasing age is associated with hip osteoarthritis it may indicate that survival data in vascular amputees may need to be reviewed.
