Abstract
Keywords
Borderline personality disorder (BPD) is a severe mental disorder that usually emerges during adolescence [1]. BPD in adolescence is associated with marked psychopathology and functional impairment [2] and is prospectively associated with diverse functional and psychopathological poor outcomes, including a future diagnosis of BPD, increased risk for axis I disorders (especially substance use and mood disorders), interpersonal problems, distress and reduced quality of life [3]. Moreover, the functional impairments found in adolescents with BPD persist for decades [4]. Adolescents with BPD commonly seek clinical help [2, 5] and we have previously outlined the case for developing early intervention strategies for BPD [3] and a method for identifying patients for such programmes through screening [6].
The Helping Young People Early (HYPE) programme is a specialized early intervention programme for BPD at ORYGEN Youth Health [7], the government-funded youth mental health service for Western metropolitan Melbourne, Australia. We have previously reported data from the first randomized controlled trial of early intervention for adolescents with subsyndromal or full-syndrome BPD [8], conducted at the HYPE clinic. This trial compared the effectiveness of two active, manualized interventions: cognitive analytic therapy (CAT) [9] or manualized good clinical care (GCC) (McCutcheon L et al.: unpublished data, 2000), in addition to the comprehensive HYPE service model of care. CAT and GCC were both effective in reducing the pre-chosen measures of psychopathology, parasuicidal behaviour and global functioning. There was evidence that patients allocated to CAT improved more rapidly but there were no significant differences between the outcomes of the treatment groups at 24 months on the pre-chosen measures.
The effectiveness of both structured interventions and the relatively small differences found between the two raises the question as to whether the comprehensive service model itself might be an effective ingredient of care. This is pertinent to three recent randomized controlled trials of psychotherapeutic interventions for BPD in adult samples [10–12] that have used active comparison groups, rather than comparison to treatment as usual. Although these studies report differential responses for the interventions tested, the active comparison interventions were also effective. For example, Giesen-Bloo et al. reported statistically and clinically significant improvements for both schema-focused therapy and transference-focused psychotherapy on all measures after 1, 2, and 3 year treatment periods [11].
The present paper reports a quasi-experimental comparison of CAT and GCC to a non-randomized historical control sample, who received historical treatment as usual (H-TAU) in the same clinical service, immediately prior to the implementation of the HYPE clinic and the aforementioned randomized controlled trial. Primary outcome measures were identical to those in the randomized controlled trial. We predicted that, compared to H-TAU, GCC and CAT would each perform significantly better in: (i) decreasing borderline psychopathology, general psychopathology (internalizing and externalizing psychopathology), parasuicidal behaviours (suicide attempts and non-suicidal self-injury [13]); and (ii) improving social and occupational functioning.
Methods
Participants
The characteristics of the 110 participants (CAT, n = 41; GCC, n = 37; H-TAU, n = 32) are shown in Table 1.
Baseline sample characteristics
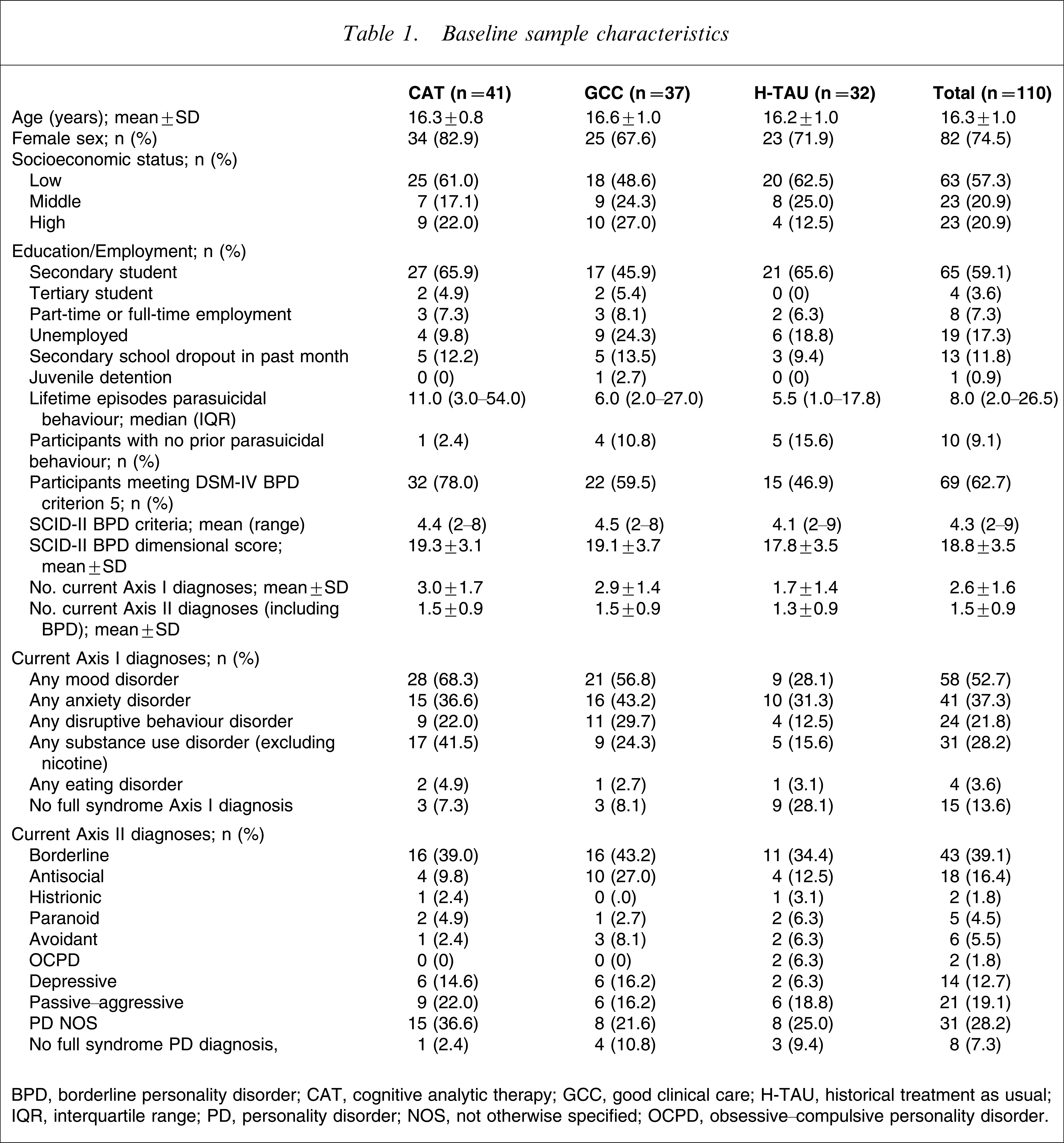
BPD, borderline personality disorder; CAT, cognitive analytic therapy; GCC, good clinical care; H-TAU, historical treatment as usual; IQR, interquartile range; PD, personality disorder; NOS, not otherwise specified; OCPD, obsessive–compulsive personality disorder.
CAT and GCC groups
These groups are described in detail elsewhere [8]. Briefly, participants were aged 15–18 years, sufficiently fluent in English, had 2–9 DSM-IV [1] BPD criteria, and had one or more of the following childhood risk factors for young adult personality disorder: any personality disorder (PD) symptoms, any disruptive behaviour disorder symptoms, low socioeconomic status, depressive symptoms, history of abuse or neglect.
Exclusion criteria were (i) mental retardation; (ii) psychiatric disorder due to a general medical condition; (iii) pervasive developmental disorder; (iv) severe primary Axis I disorder that should be the principal focus of treatment (e.g. medically unstable anorexia nervosa or severe obsessive–compulsive disorder); and (v) more than nine sessions of specialist mental health treatment in the previous 12 months. Potential participants were not approached if they had sustained psychosis and met criteria for ORYGEN's Early Psychosis Prevention and Intervention Centre [7].
Historical treatment-as-usual sample
This historical comparison sample was selected from a separate cohort of 101 participants in a longitudinal study of the temporal stability of personality disorder in youth [14]. All members of this cohort had attended the generalist older adolescent outpatient programme at ORYGEN's predecessor from March 1998 to July 1999, immediately prior to the implementation of the specialized BPD service and randomized controlled trial. Thirty-two individuals retrospectively met the same inclusion and exclusion criteria applied to CAT and GCC, except for prior specialist mental health treatment for all participants and the childhood risk factors for young adult PD in eight participants.
Procedure
The study was approved by the North Western Health Care Network Behavioural and Psychiatric Research and Ethics Committees. After complete explanation of the study procedures, written informed consent was obtained from all participants and a parent or guardian, where appropriate.
The assessment and randomization procedure for the randomized controlled trial is described elsewhere [8].
Research assessments were conducted independently of the interventions. The procedure is described elsewhere for the randomized controlled trial [8] and for H-TAU [14]. For the randomized controlled trial, assessments were blind to treatment allocation and for the H-TAU group, follow-up assessments were conducted blind to baseline status.
Figure 1 shows the flow of participants through the randomized controlled trial and through H-TAU. CAT and GCC participants were assessed at four fixed time points: baseline (n = 78), 6 months (n = 70), 12 months (n = 70) and 24 months (n = 68). Assessments were completed for at least three of the four time-points in 92% of the sample. All H-TAU participants were assessed at baseline and at 24 months only.
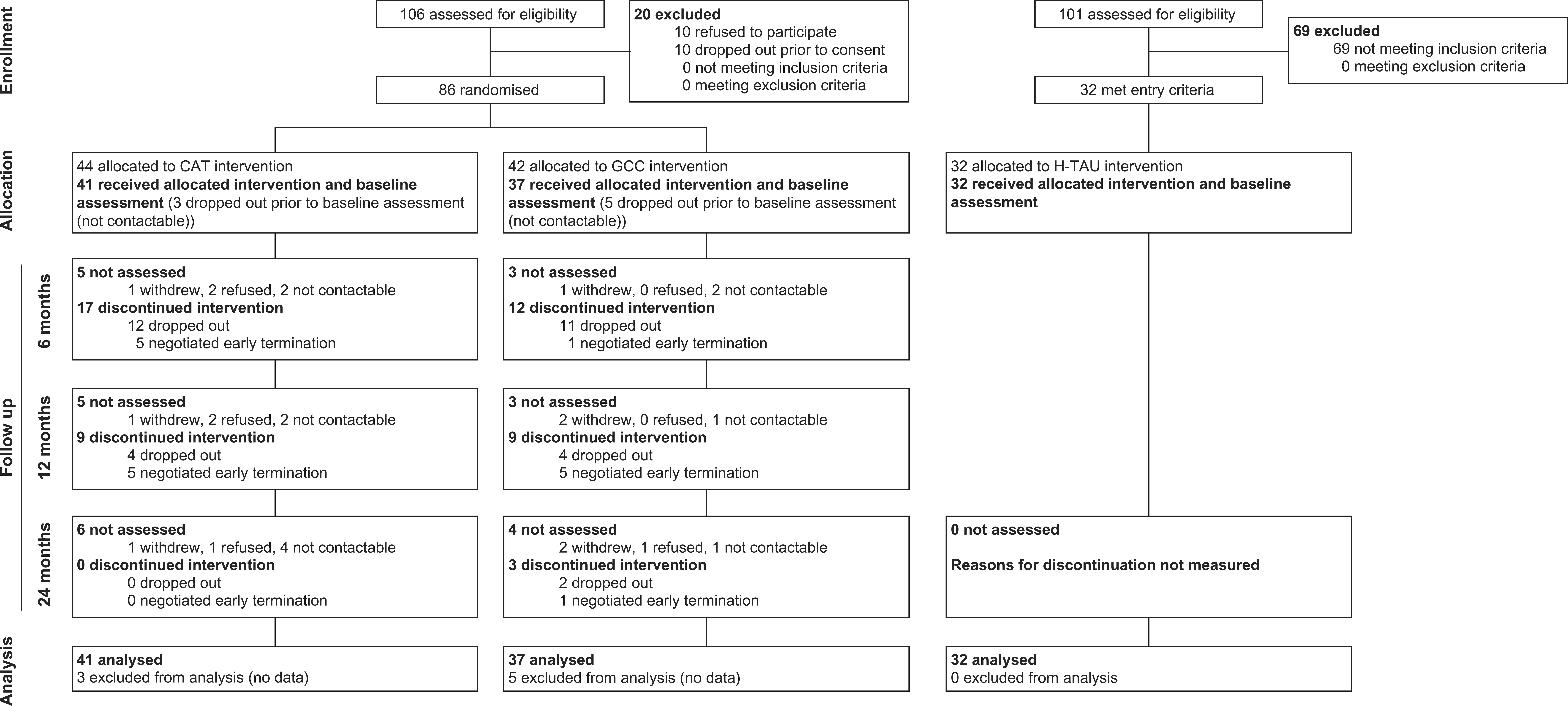
Trial profile
Diagnostic interviews
Diagnoses were obtained using the Structured Clinical Interview for DSM-IV Axis I disorders–patient version (SCID-I/P) [15], the Kiddie Schedule for Affective Disorders and Schizophrenia for School-Age Children–Present and Lifetime version disruptive behaviour disorders module [16] and the full Structured Clinical Interview for DSM-IV Axis II disorders (SCID-II) [17]. For the H-TAU sample, the SCID-I/P drug and alcohol module was substituted with the corresponding Composite International Disgnostic Interview-Auto module [18]. In keeping with previous research, a PD criterion was scored positive if it was present for 2 years and did not occur exclusively during an Axis I disorder [19]. Also, antisocial PD criterion A (age ≥ 18 years) was ignored and PD not otherwise specified was defined as either nine positive PD criteria across any PD domains or falling one criterion short of caseness for a specific PD diagnosis but having two additional criteria from any other PD domain [2].
Outcome measures
Primary outcome variables were defined a priori. We anticipated that, compared to H-TAU, CAT and GCC would show a greater reduction in psychopathology and parasuicidal behaviour (suicide attempts and non-suicidal self-injury [13]) and greater improvement in global functioning.
Psychopathology
The SCID-II BPD dimensional score was derived by summing the nine SCID-II items, scored 1 = absent, 2 = subthreshold or 3 = present. Scores range from 9 to 27. For follow-up assessments, each BPD criterion was rated for the interval between assessments.
Internalizing and externalizing psychopathology scores were derived from the Youth Self-Report (YSR) questionnaire [20], a widely-used instrument [21], which assesses behavioural and emotional functioning in 11–18-year-olds. It has 112 items, rated 0 = not true, 1 = somewhat or sometimes true, and 2 = very true or often true. The Young Adult Self-Report [22] (YASR) is an analogue of the YSR for 18–30-year-olds, containing 116 items, rated using the same YSR response format. Because some of the items of the internalizing and externalizing subscales differ between the YSR and YASR, in keeping with previous research [2], we calculated the mean item scores for each scale to ensure comparability. The resulting score ranged between 0 and 2.
Parasuicidal behaviour
Parasuicidal behaviour was assessed on semi-structured interview (developed by the investigators and available upon request) that included enquiring into each form of parasuicide and the number of episodes. The number of episodes was then coded as: none, monthly, weekly and daily.
Global functioning
Global functioning was assessed using the widely used Social and Occupational Functioning Assessment Scale (SOFAS) [23].
Treatment conditions and clinicians
CAT and GCC consisted of up to 24 weekly sessions. H-TAU was unrestricted and consisted of at least some of the following: assessment, case management with limited assertive outreach, individual and/or family interventions, activity groups and psychiatrist referral with or without pharmacotherapy.
Clinicians
The three randomized controlled trial clinicians (two female, one male) were cognitive behaviour therapy trained, 6 year degree clinical psychologists (standard for Australia), with at least 2 years post-training experience. In order to control for therapist effects (e.g. sex, training, experience), they delivered both randomized controlled trial interventions and the accompanying case management.
H-TAU clinicians were typical for a multi-disciplinary Australian child and adolescent mental health team and consisted of one or more staff from the disciplines of clinical psychology, psychiatry, nursing, social work, and occupational therapy.
Cognitive analytic therapy
CAT is a time-limited, integrative psychotherapy developed in the UK over the past 25 years by Ryle and Kerr [24]. CAT arose from a theoretical and practical integration of elements of psychoanalytic object relations theory and cognitive psychology, developing into an integrated model of development and psychopathology. CAT has been adapted specifically for the treatment of BPD [9].
Standardized good clinical care
GCC is a modular treatment package, developed specifically for this study (McCutcheon L et al.: unpublished data, 2000) and explicitly designed to control for some factors commonly believed to be effective in psychotherapy (availability, accessibility and duration of therapy, institutional prestige and general factors associated with receiving therapy [12]).
GCC was designed to deliver standardized, high-quality, team-based clinical care that might be achievable in mental health services in more economically developed countries. It used a simple problem-solving model [25] for all participants, with additional modules determined by the co-occurring problems (e.g. depression, anxiety or anger management) identified by patient and/or therapist. Some modules included basic cognitive behavioural concepts.
Common elements to the HYPE treatment model
Both CAT and GCC utilized, and had equal access to, common elements of the HYPE model of care. This team-based model of care includes (i) rigorous diagnosis of BPD and other personality pathology in young people; (ii) assertive case management integrated with the delivery of psychotherapy; (iii) active engagement of families or carers, with psychoeducation and up to four sessions of family intervention; (iv) general psychiatric care, with specific assessment and treatment of co-occurring psychiatric syndromes (comorbidity), including the use of pharmacotherapy (where indicated); (v) crisis team and inpatient care, with a clear model of brief and goal-directed inpatient care; (vi) access to an activity group programme that is shared with other programmes at ORYGEN Youth Health; (vii) individual and group supervision of staff; and (viii) a quality assurance programme.
Treatment integrity for CAT and GCC
In addition to treatment manuals, expert training and supervision, all randomized controlled trial sessions were audio recorded. Independent ratings found good adherence and competency for CAT and GCC, along with clear differentiation between the two interventions [8].
Treatment of missing data and statistical methods
Data analysis was by intention to treat. Missing values for CAT and GCC on outcome measures due to withdrawal or non-attendance subsequent to baseline were assumed to have occurred at random, given completely observed pre-treatment scores. Missing values for H-TAU at times 2 and 3 had not been measured at those time points and therefore could be regarded as strictly ignorable. Ten multiply imputed data sets were generated using the PAN package [26] in the R statistical program [27], for which the imputation model was the same as the one used in the actual statistical modelling of the data.
Treatment differences and change over times were analysed by using the xtmixed procedure in Stata version 9.2 for Windows (StataCorp, College Station, TX, USA) for the continuous total BPD, SOFAS, internalizing and externalizing outcome measures and by using the gllamm package for the ordinal categorical parasuicidal behaviour. The four time-points were coded as −1, −0.75, −0.5, 0 in all models, thereby implying that regression coefficients involving time measured the linear rate of change from baseline to 24 month follow up and that regression intercepts referenced group differences at the last follow-up point (no evidence of non-linear change in the CAT and GCC groups was observed).
A linear random-intercept model best fitted the SOFAS and internalizing measures, whereas total BPD and externalizing outcomes were best represented by a linear random-intercepts-and-slopes model. Parasuicidal behaviour was best fitted by a logistic proportional odds random-intercepts model. Effects for all outcome measures were adjusted by additionally incorporating into all fitted models time-varying covariates for (i) total SCID-II antisocial personality disorder score; (ii) presence of a mood disorder; and (iii) presence of a substance-use disorder.
Only primary model parameters directly relevant to the study objectives are presented here due to space limitations. They are (i) main effect group differences at 24 months (indicating whether one group was better or worse than its comparison group at the final follow up); (ii) the linear rate of change from baseline to final follow up for the three groups (i.e. simple regression slopes [28], which indicate the extent to which each group improved or deteriorated over the 24 months); and (iii) group differences in this rate of change (indicating whether the rate of improvement or deterioration in one group was substantially stronger than its comparison group). Pairwise comparisons for all three groups are presented here for ease of inspection, with the redundant group comparison being obtained using the Stata lincom procedure applied to parameter estimates and standard errors from the fitted model. All model parameters for continuous outcome measures are presented here as partial standardized effects, whereas those for the categorical measures of parasuicidal behaviour are presented as conditional odds ratios (ORs). Complete tables of all modelling results are available upon request.
The 10 multiply imputed data sets provided 10 sets of model parameter estimates and their standard errors. These values were averaged over all 10 imputed data sets using the Rubin rules for scalar estimands [29] to obtain mean multiply imputed model parameter estimates. Finally, 95% confidence intervals were calculated for all parameter estimates using the Rubin Student's t approximation [29].
Results
Treatment received
The median number of therapy sessions received was 13.0 (interquartile range (IQR) = 8–23) for CAT and 11.0 (IQR = 4.5–23) for GCC. The median number of individual non-therapy contacts (e.g. case management and psychiatrist appointments) was 33.0 (IQR = 20.5–54.0) and 32.0 (IQR = 18.5–52.5), respectively. There were no significant differences between CAT and GCC on the number of therapy sessions or non-therapy contacts at any of the three follow-up time points (all p > 0.05). The median interval from enrolment to discharge was 42.9 weeks (IQR = 24.1–58.3) for CAT and 39.4 weeks (IQR = 20.6–52.1) for GCC. The median number of contacts of any type per week was 1.4 (IQR = 0.9–1.8) for CAT and 1.3 (IQR = 0.8–1.6) for GCC.
H-TAU patients received a median of 15.0 (IQR = 6.8–40.3) service contacts. Of these, 10.0 (IQR = 3.3–22.8) were individual contacts, consisting of either or both psychotherapy and case management (not recorded separately). The median interval from enrolment to discharge was 26.5 weeks (IQR = 8.5–56.3) and the median number of contacts (of any type) per week was 0.7 (IQR = 0.5–1.1).
Baseline comparisons
Multiply-imputed summary statistics at all four time-points for the three groups are presented in Table 2 for the four continuous outcomes measures (means and SDs) and in Table 3 for parasuicidal behaviour (proportions in each category). Robust one-way ANOVAs using Welch's test indicated no statistically significant baseline differences between treatment groups at the 5% level on all four outcome measures (all p > 0.10). There was no statistically significant association at baseline between treatment group and the frequency of parasuicidal behaviour (χ2(6, n = 108) = 5.59, p = 0.47). Any differences in rate of change over time and group differences at final follow up may therefore be reasonably inferred to reflect treatment differences, rather than baseline group differences.
Continuous outcome measures
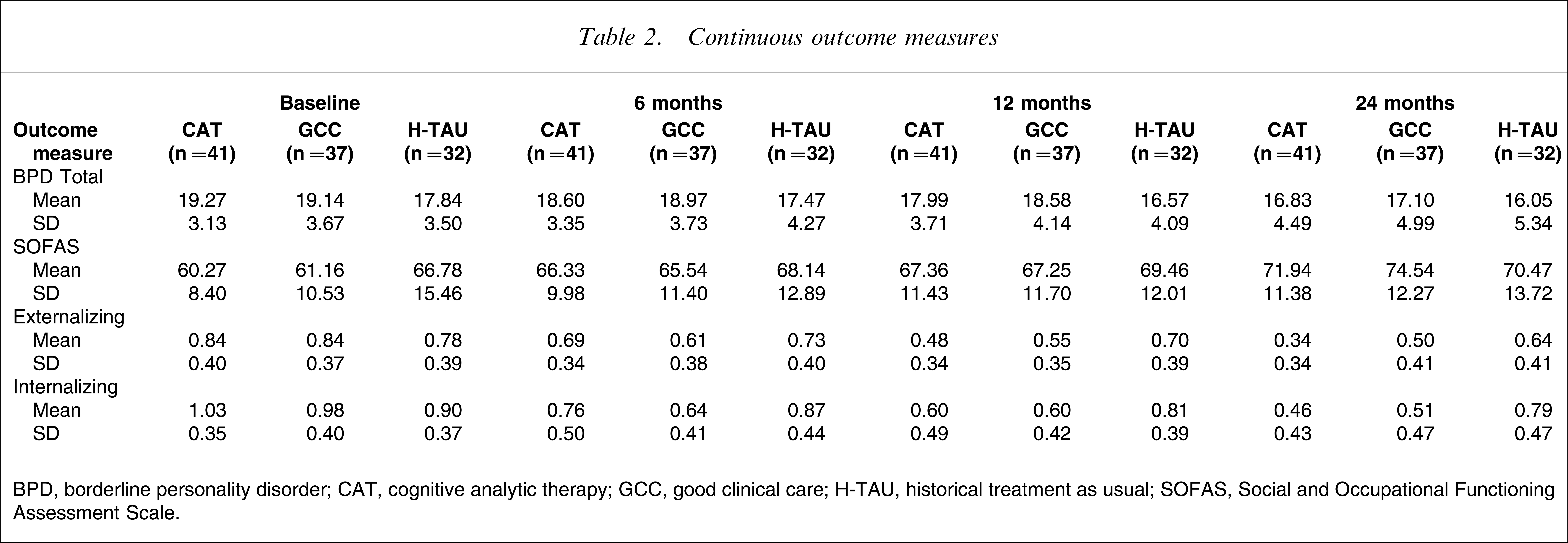
BPD, borderline personality disorder; CAT, cognitive analytic therapy; GCC, good clinical care; H-TAU, historical treatment as usual; SOFAS, Social and Occupational Functioning Assessment Scale.
Group proportions for frequency of parasuicide
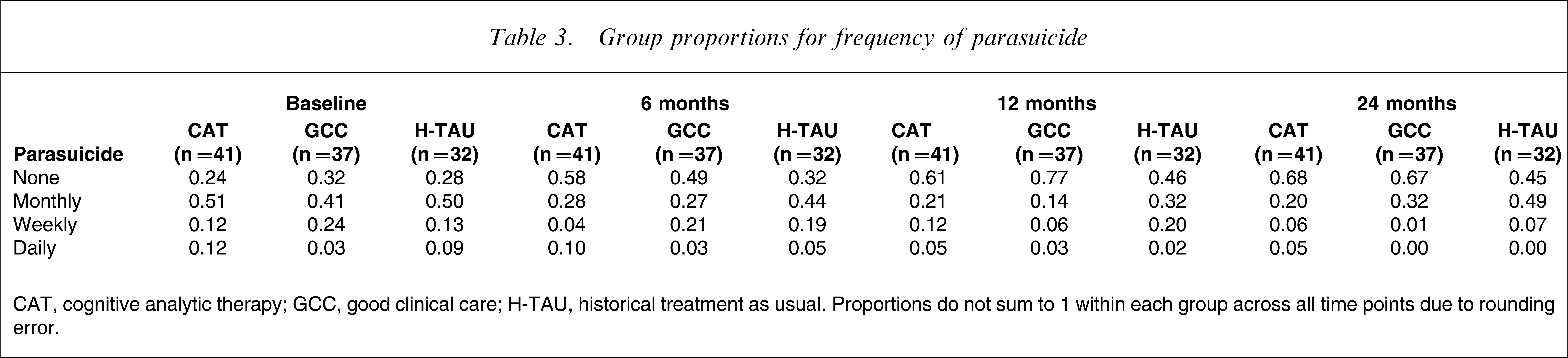
CAT, cognitive analytic therapy; GCC, good clinical care; H-TAU, historical treatment as usual. Proportions do not sum to 1 within each group across all time points due to rounding error.
Longitudinal treatment effects
All three treatment groups demonstrated improvements over the 2 year period from baseline to final follow up (Table 4). The CAT group evidenced a median improvement in absolute terms over all continuous outcome measures of 1.07 SDs, followed by GCC (0.84 SD) and H-TAU (0.64 SD). Moreover, treatment groups showed a substantial reduction over time in the odds of a higher frequency of parasuicidal behaviour incidents (OR = 0.11 times for CAT, 0.09 times for GCC, and 0.23 times for H-TAU).
Longitudinal modelling of outcome measures†
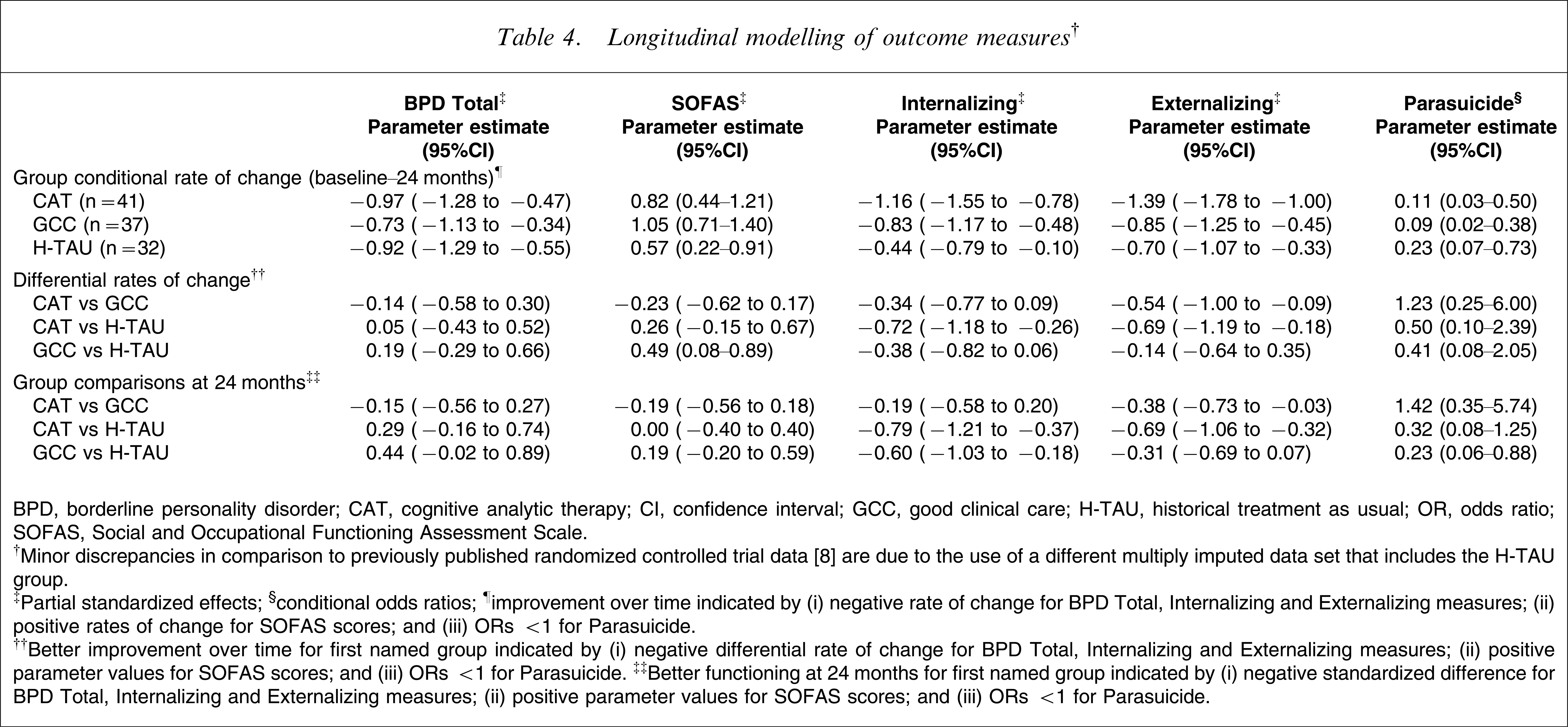
BPD, borderline personality disorder; CAT, cognitive analytic therapy; CI, confidence interval; GCC, good clinical care; H-TAU, historical treatment as usual; OR, odds ratio; SOFAS, Social and Occupational Functioning Assessment Scale.
†Minor discrepancies in comparison to previously published randomized controlled trial data [8] are due to the use of a different multiply imputed data set that includes the H-TAU group.
‡Partial standardized effects; §conditional odds ratios; ¶improvement over time indicated by (i) negative rate of change for BPD Total, Internalizing and Externalizing measures; (ii) positive rates of change for SOFAS scores; and (iii) ORs <1 for Parasuicide.
††Better improvement over time for first named group indicated by (i) negative differential rate of change for BPD Total, Internalizing and Externalizing measures; (ii) positive parameter values for SOFAS scores; and (iii) ORs <1 for Parasuicide. ‡‡Better functioning at 24 months for first named group indicated by (i) negative standardized difference for BPD Total, Internalizing and Externalizing measures; (ii) positive parameter values for SOFAS scores; and (iii) ORs <1 for Parasuicide.
Differential rates of change
Table 4 shows that the expected rate of improvement was faster for CAT compared to GCC in both externalizing (−0.54 SD) and internalizing (−0.34 SDs) pathologies, although the upper bound of the respective 95% confidence intervals indicated that this differential rate may at worst be slight. CAT also showed a better improvement rate in both internalizing (−0.72 SDs) and externalizing (−0.69 SDs) pathologies compared to H-TAU. The other notably better rate of improvement was for GCC over H-TAU in SOFAS (0.49 SDs). There was no meaningful and substantial difference between groups in their rates of change over time for BPD total scores and for frequency of parasuicidal behaviour.
Group comparisons at final follow up
Table 4 also lists sizeable differences at final follow up that favoured CAT over GCC in externalizing psychopathology (−0.38 SDs) and CAT over H-TAU in both internalizing (−0.79 SDs) and externalizing (−0.69 SDs) pathologies. In addition, GCC was better than H-TAU at 24 months on internalizing psychopathology (−0.60 SDs). The odds were notably smaller (OR = 0.23) for GCC than for H-TAU of more frequently performing parasuicidal behaviour at 2 years. Group differences at 24 months on total BPD and SOFAS ranged from being on average negligible for CAT versus H-TAU on SOFAS (0.00 SDs) to small–medium in size for GCC versus H-TAU on total BPD (−0.44 SDs).
Discussion
The major findings to emerge from the present study are that both CAT and GCC (in addition to HYPE) were more effective than H-TAU in improving some pre-chosen outcome measures and that CAT yielded the greatest median improvement on the four continuous measures. At 24 month follow up, CAT had lower standardized levels of and a significantly faster standardized rate of improvement in both internalizing and externalizing psychopathology, compared to H-TAU. GCC also had lower standardized levels of internalizing psychopathology and a faster rate of improvement in SOFAS, compared to H-TAU at 24 month follow up. As with the previous randomized controlled trial findings [8], it should be noted that, on average, patients in all treatment groups demonstrated significant and clinically substantial improvement.
These findings suggest that adding either CAT or GCC to the comprehensive, team-based HYPE service model yields substantial benefits over H-TAU, with CAT yielding more substantial benefits. When considered in the context of the results from the previous randomized controlled trial [8], these findings suggest that common elements of HYPE, namely the service model within which individual psychotherapy is delivered, might be an important and effective ingredient of care. If this is the case, reforms to clinical services, using existing resources, might be equally or more important than the delivery of any specific brand of psychotherapy. These reforms might be more readily achievable in typical mental health systems where workforce issues and training are usually problematic.
The actual amount of time spent with CAT and GCC patients was almost identical, whereas H-TAU patients received less care. Compared to CAT or GCC, the duration of H-TAU was approximately two-thirds and patients had approximately half the number of contacts per week. Although the duration of care might be related to outcome, it is likely that duration is confounded with the type of treatment. One of the features of the HYPE interventions was their reorganization of existing clinical resources into a coherent, team-based model of assertive care. All three interventions were delivered by salaried staff with fixed caseloads, so increasing the frequency of contacts in the HYPE interventions did not require additional funding. H-TAU had the same level of resources available for patient care, including access to crisis care, inpatient care, group activity programmes and other service elements. These service elements, however, were used less efficiently and were not organized into team-based care with an explicit model of collaboration, problem solving, universal assertive case management, thorough diagnosis of personality pathology, meticulous attention to treatment of co-occurring mental state pathology, family involvement and group supervision, all of which were common to CAT and GCC. This underscores our assertion that there is much more to early intervention for BPD than only formal psychotherapy.
What then might be the specific value of either CAT or GCC? The present study and the randomized controlled trial focused on the patient outcomes of psychopathology, parasuicidal behaviour and social and occupational functioning. Among the factors that were not measured was the value of a specific treatment orientation to individual clinicians and/or teams. Both CAT and GCC offered team-based care with a common purpose. The HYPE clinicians, however, reported developing a preference for CAT over GCC during the randomized controlled trial. They reported that the CAT model of BPD and its treatment helped to foster team and individual confidence, communication and functioning, acting as a lingua franca for the HYPE programme. This is likely to have benefited both arms of the randomized controlled trial, because the same clinicians delivered both CAT and GCC. Further studies are required using independent groups of therapists to assess the HYPE model as a treatment package versus generic high-quality care, along with studies examining the component parts of the model.
Both HYPE and the adolescent outpatient service that conducted H-TAU operated as frontline, real-world clinical services that accepted referrals from the community and had few exclusion criteria. The HYPE clinic continues to operate in this way. This enhances the external validity of the study, increasing confidence that these reforms are relevant to child and youth mental health services. There are caveats, however, regarding this quasi-experimental comparison with H-TAU, which are discussed in the following section and which will need to be addressed in future studies.
Limitations
The sample size, although comparable to other published trials, was still relatively small and limited reliable detection of small–medium treatment effects. It would have been preferable to conduct a complete randomized controlled trial, randomizing patients to TAU contemporaneously with CAT and GCC. Being a quasi-experimental design, there are important caveats with regard to all comparisons to H-TAU. First, participants were not randomized to H-TAU. Second, H-TAU was not contemporaneous with CAT and GCC, introducing possible cohort effects apart from the intended effect of reforming services for BPD (the focus of the research questions). But these are unlikely to explain the differences because neither the intrinsic characteristics of the patients nor the availability of resources changed over this time. Using the same therapists to deliver both treatment conditions allowed for rigorous control of some therapist effects (gender, experience, personality) in the randomized controlled trial. Therapist effects cannot be ruled out in explaining the observed differences in comparison with H-TAU. Third, H-TAU patients were enrolled in a research study but not explicitly enrolled in a treatment trial and might not have experienced the expectations that might accompany randomized controlled trial enrolment.
Conclusion
Early intervention for subsyndromal or full-syndrome BPD is effective. CAT and GCC delivered in addition to the HYPE model were superior to treatment as usual. This suggests that reform of existing services using the HYPE model might yield substantial improvements in patient outcomes. A randomized controlled trial of the HYPE model versus TAU is required to definitively confirm these findings.
Footnotes
Acknowledgements
This work was supported by grants 98–0198 from the Victorian Health Promotion Foundation, Melbourne, Australia and grant 990748 from the National Health and Medical Research Council, Canberra, Australia. ORYGEN Research Centre is supported by the Colonial Foundation, Melbourne, Australia. The authors thank all participants in this study and the staff of ORYGEN Youth Health. Particular thanks go to Dr Anthony Ryle, Dr Ian Kerr, Ms Eva Burns-Lundgren, Dr Dawn Bennett, Dr Jackie Withers and the Association for Cognitive Analytic Therapy (UK) for training and supervision in CAT. Thanks also go to Assoc. Professor John Gleeson for supervision of Standardized Good Clinical Care, Dr Andrew Court for independent psychiatric assessments, Dr Carol Hulbert, Ms Helen Mildred and Dr Denise Charman for advice on the implementation of the study and to Professor Anthony Jorm and Dr Sarah Hetrick for comments on an earlier version of this manuscript. The funding organizations played no part in the design and conduct of the study or the collection, management, analysis and interpretation of the data or in the preparation, review or approval of the manuscript.
