Abstract
Introduction
The aim of this study, was to develop an artificial neural networks (ANNs) model for predicting successful surgery outcome in lumbar disc herniation (LDH).
Materials and Methods
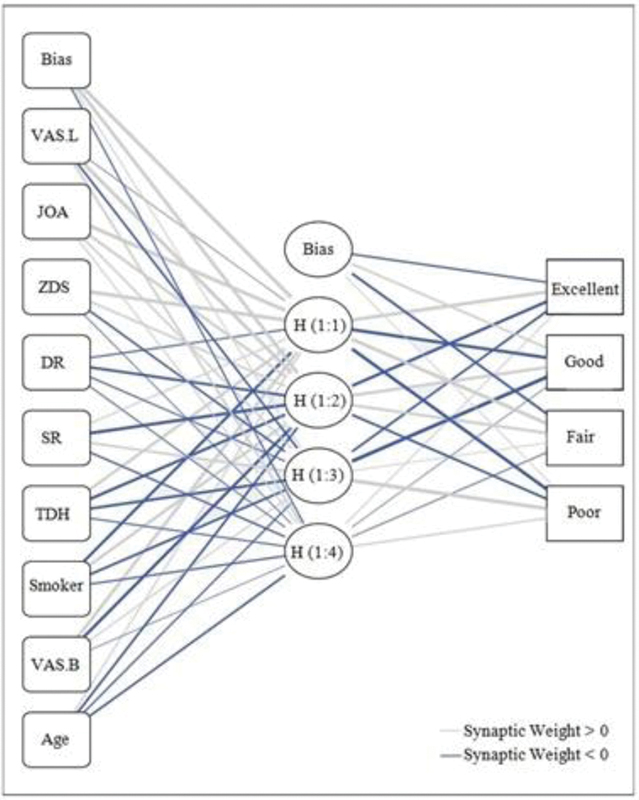
An ANN model and a logistic regression (LR) model were used to predict outcomes. The age, gender, duration of symptoms, smoking status, surgical level, visual analog scale of leg/back pain, the Zung depression scale, and the Japanese Orthopaedic Association score, were determined as the input variables for the established ANN model. The Macnab classification was used for outcome assessment. ANNs on data from LDH patients, who had surgery, were trained to predict 2-year successful discectomy using several input variables. Sensitivity analysis to the established ANN model was used to identify the relevant variables. For evaluating the two models, the area under a receiver operating characteristic curve, accuracy rate of predicting, and Hosmer-Lemeshow (H-L) statistics were considered.
Results
A total of 203 (96 male, 107 female, mean age 48.3 ± 9.8 years) patients were categorized into training, testing, and validation datasets consisting of 101, 51, and 51 cases, respectively. Surgical successful outcome was categorized as: excellent, 32.0%; good, 40.9%; fair, 20.7%; and poor, 6.4% at 2-year follow-up. Compared with the LR model, the ANN model showed better results: accuracy rate, 95.8%; H-L statistic, 41.5%; and AUC, 0.82% of patients, respectively.
Conclusion
The findings show that ANNs can predict successful surgery outcome with a high level of accuracy in LDH patients. Such information is of use in the clinical decision-making process.
None declared
Fardon DF, Milette PC; Combined Task Forces of the North American Spine Society, American Society of Spine Radiology, and American Society of Neuroradiology. Nomenclature and classification of lumbar disc pathology. Recommendations of the Combined task Forces of the North American Spine Society, American Society of Spine Radiology, and American Society of Neuroradiology. Spine 2001;26(5):E93-E113
Li YC, Liu L, Chiu WT, Jian WS. Neural network modeling for surgical decisions on traumatic brain injury patients. Int J Med Inform 2PO.069;57(1):1–9
Bishop CM. Neural Networks for Pattern Recognition. Oxford, UK: Clarendon; 1995
Azimi P, Benzel EC, Shahzadi S, Azhari S, Mohammadi HR. Use of artificial neural networks to predict surgical satisfaction in patients with lumbar spinal canal stenosis. J Neurosurg Spine 2014;20(3):300–305
Price DD, McGrath PA, Rafii A, Buckingham B. The validation of visual analogue scales as ratio scale measures for chronic and experimental pain. Pain 1983;17(1):45–56
Azimi P, Mohammadi HR, Montazeri A. An outcome measure of functionality and pain in patients with lumbar disc herniation: a validation study of the Japanese Orthopedic Association (JOA) score. J Orthop Sci 2012;17(4):341–345
Zung WW, Richards CB, Short MJ. Self-rating depression scale in an outpatient clinic. Further validation of the SDS. Arch Gen Psychiatry 1965;13(6):508–515
Macnab I. Chapter 14. Pain and disability in degenerative disc disease. Clin Neurosurg 1973;20:193–196
Cross SS, Harrison RF, Kennedy RL. Introduction to neural networks. Lancet 1995;346(8982):1075–1079
Rughani AI, Dumont TM, Lu Z, et al. Use of an artificial neural network to predict head injury outcome. J Neurosurg 2010;113(3):585–590
Finneson BE. A lumbar disc surgery predictive score card. Spine 1978;3(2):186–188
