Abstract
It is a sign of weakness to combine empirical and logical arguments, for the latter, if valid, make the former superfluous. —Bertrand Russell [1]
The preceding paper [2] offered the following two propositions:
1. The faculty of mind is contingent upon the functioning human brain; in this sense mind and brain constitute two aspects of a unity. At a fundamental level there appears to be an ‘identity’ between specific mental states and specific brain states upon which they are contingent.
2. Any attempt to explain the subjective essence of a mental state or process in terms of a brain state or process must inevitably fail as it leaves out the ‘mind’ that we seek to explain. Discourse about mental states is not reducible to discourse about brain states, and therefore brain states and mind states are not identical. (If x is identical to y then any property of x is also a property of y, and vice versa. Subjective mental events and objective brain events have distinct and differing properties.)
The preceding paper suggested that there are good grounds for accepting both of these propositions: (1) on the basis that it is the hypothesis that best fits the currently available scientific data; (2) on the basis that it is a self-evident truth. It also acknowledged the logical difficulty in entertaining both propositions simultaneously. Strictly speaking they do not constitute a solution to the mind–brain problem, which as a metaphysical problem may be insoluble. They are proposed as the most satisfactory formulation of the problem possible given the limitations of our knowledge and/or understanding.
This second paper argues that, if these paradoxical propositions are accepted, they carry important theoretical and practical implications for concepts of causal explanation and aetiology as they are applied to the mind and psychiatric disorders.
Causality and a unity theory
If we accept proposition one, that mental states and brain states constitute ‘double aspects’ of a unity, this suggests that in some fundamental way they are the same thing, or they arise as different manifestations of a unitary phenomenon (double aspect theory). If they constitute such a fundamental unity then one cannot simply be said to cause the other. We may say that the existence of mind is contingent upon the existence of certain states of the brain, but it seems doubtful that it can be meaningfully said that brain states cause the mind states that they ‘coexist’ with, or for that matter, that mind states cause the brain states that they ‘coexist’ with. Rather we might say mind states are the brain states thatthey ‘coexist’ with.
Despite apparent widespread acceptance of some form of identity or unity theory within science in general and psychiatry in particular, its potential incompatibility with the idea that, at a given moment in time, mental activity is caused by brain activity (rather than simply contingent upon it) is apparently not often appreciated. Discourse and practice in psychiatry often carry an implicit assumption of brain activity causing mental activity; sometimes to the extent of relegating mind to the position of an epiphenomenon. Consider, for example, a clinician who tells a depressed patient (in whom there are no specific primary organic factors), that the depression is caused by a ‘biochemical imbalance’ in the brain. This statement recognizes the existence of something of the mind (the experience of depression), while relegating this to a secondary, or ‘epiphenomenal’, role to brain biochemistry. It suggests that the patient's mental experience of depression (the same argument holds for any mental experience), is caused by a set of other (whether observed or presumed) physical events taking place within the brain. However, it would make just as much, or just as little, sense to say that the experience of depression was causing the biochemistry or physiology of the brain to become disturbed. Within the framework of a unity, identity, or double aspect theory, neither of these propositions is logically defensible as it stands.
To the extent that a theory of mind is epiphenomenal it attributes causality to the brain, and excludes the attribution of causality to the mind, but if we are serious about some form of unity theory, it follows that in the unfolding sequence of brain/mind events, mental events have, in principle, the same causal status as brain events. As stated mental events cannot simply be regarded as caused by the activity of the brain, because mental events are the activity of the brain.
If it is incoherent to speak of brain activity causing mental activity (at least in cross-sectional time), how then are we to speak about causality, and by implication aetiology, in relation to brain and mind, and to psychiatric disorder? I suggest causality is most usefully considered in relation to the mind–brain system as a whole, and if formulations of psychiatric causality are proposed, they must be consistent with concepts of causality employed in science generally. Within a dynamic system, evidence for causality is found in the identification of a set of reliable antecedent conditions/events that would seem to, or can be utilized to, predict subsequent conditions/events. The concept of causality carries the idea of something over and above this temporal juxtaposition of events, and a theory of cause is a formulation as to what this something is. Implicit in the concept of cause in a dynamic system is the passage of a period of time, however, brief or infinitesimal.
To say that the brain events cannot be considered to cause mental events is not to say that identified events that cause change or disturbance in the brain do not cause change or disturbance in the mind; it is obvious that they do. Equally, identified events which cause change or disturbance in the mind cause a corresponding change or disturbance in the brain. The situation might be represented symbolically as follows, where Me stands fora ‘mental event’ and Be stands for the ‘brain event’ upon which that mental event is contingent:
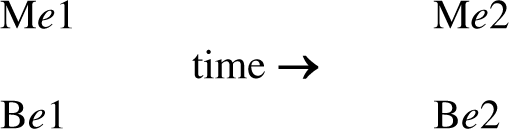
If a cause can be conceptualized as operating upon the mind to produce Me1 it simultaneously produces Be1. If a cause can be conceptualized as operating upon the brain to produce Be1 it simultaneously produces Me1. Me1/Be1 may then act causally to produce a second event in the mind–brain system, Me2/Be2. [Of course, while all mental events will be contingent upon brain events, not all brain events need be linked with contingent mental events. For example, the following sequence is possible: Be (n) → Be (n + 1)/Me (n + 1).]
To consider an example of the construction of a simple, but valid, causal model: a patient sustains a head injury with subsequent emotional disturbance and memory loss. There is a case for supposing that the immediate and determinate cause of the mental disorder is the physical injury. This conclusion is suggested by the fact that an unusual physical event, the head injury, was followed by, and seemed linked with, a disturbance of mental function. The cause is conceptualized as acting in longtitudinal time. That the head injury was the cause of the disturbance would seem a reasonable working hypothesis, and for practical purposes might be regarded as confirmed on the basis of supporting evidence, for example: (i) evidence of physical damage to the brain resulting from the injury; and (ii) the fact that similar mental disturbance has been observed in the past to be associated with the sort of injury to the brain sustained by the patient. That events of apparent cause and effect have previously conformed to a similar pattern supports the assumption of cause and effect on this occasion. Such a pattern may justify the formation of an inductive theory of causes and effects of this type.
If the brain injury was a random event outside the patient's control, then we have an example of an unintentional and physical brain-impinging event causing a disturbance in the ‘mind-brain system’. In this instance a commonsense understanding of causality would not emphasize the mind, but rather emphasize that there was an identified physical cause. It would make common sense to say that the cause operated via its impact upon the brain, leading to a disturbance of the mind–brain function.
Consider, in a similar way, an event impacting upon the mind–brain system that would usually be described as operating via the mind. A person, following news of a bereavement, is precipitated over a period of weeks into a melancholic depression. In this situation support for the hypothesis that the bereavement was the proximate and determinate causal factor might be gained from: (i) evidence from the patient's description of his/her experience of a link between the bereavement and the depression; and (ii) the fact that similar mental disturbance has previously been observed associated with the experience of bereavement.
The identified causal factor, the bereavement, is a piece of knowledge or something given to awareness. Its impact derives from its meaning for the patient in terms of his or her mental life and social matrix of relationship. It is an essentially mind-impinging event causing a disturbance of the mind–brain system. Although our mind– brain theory entails that there will be a neural ‘substrate’ of this meaningful impact, a commonsense understanding of causality would not emphasize the brain, but rather emphasize that there was an identified mental cause. It would make common sense to say that the cause operated via its impact upon the mind, leading to a disturbance of the mind–brain function.
There is both meaning and economy in saying that the effect of the head injury is via the brain, and the effect of the bereavement is via the mind. It would make little sense to say that the effect of the head injury was via the mind and the effect of the bereavement was via the brain.
The bereavement example is more complex than the head injury because bereavements are a less reliable cause of depression than head injuries are of impaired mental function. So in the bereavement example there must also be important vulnerability factor(s) within the patient. Assuming there are no specific organic factors contributing to vulnerability, then because the cause can be conceptualized as operating via the mind, it follows that the vulnerability factor(s) must also be able to be conceptualized as existing within the mind; logically it cannot be otherwise. This is simply to recognize that a bereavement can only impact upon a mind if it is experienced as meaningful. It is implicit in our mind–brain identity theory that the vulnerability factor(s) must also be represented in the brain, but if we wish to conceptualize the aetiology of the depression in this particular situation we can only meaningfully do so in terms of the interaction of the news of the bereavement and the vulnerability within the patient's mind . The logical implication of this is that an aetiological formulation based on identified neural processes, although possible in theory, will lack meaning.
If causality is to be considered in the genesis of psychiatric conditions then, as argued, this can only be done through the exploration of putative antecedent conditions or forces that lead to apparent alterations in the mind– brain system. Given that aetiology represents the sum of causal factors the same argument applies to the consideration of aetiology.
Aetiology and a unitary theory
Related to the tendency within psychiatry to relegate mind to an epiphenomenal position rather than to accept the implications of a unitary theory, is the assumption that evidence of physical brain disturbance is sufficient to establish a physical aetiology for a mental illness.
In principle a unitary theory predicts that anymental ‘disturbance’ is accompanied by a corresponding ‘disturbance’ of that part of the brain that underlies mentation, and vice versa. It follows that, in principle, neither the presence of brain disturbance nor the presence of mental disturbance would, in itself, be sufficient to establish either a physical or mental aetiology. Some other evidence will always be necessary.
The presence of physical brain disturbance alone can constitute reasonable and sufficient evidence of a physical aetiology only if that physical disturbance is in some way characteristic (pathognomonic) of a proven physical aetiology. For example, the presence of the characteristic morphological changes of Alzheimer's disease in a patient with clinical dementia would seem a reasonable basis upon which to make this diagnosis, and to assume the operation of the physical aetiological factors (known or unknown) associated with this disorder.
Obviously the presence of apparently irreversible structural changes influencing brain function is suggestive of possible physical aetiology, however, factors operating via the mind cannot be dismissed without further evidence. If we consider schizophrenia, it is often assumed that because apparently pathological changes can reliably be detected in the brains of patients with this clinical diagnosis, then the aetiology of the disorder mustbe ‘physical’ in the first instance, even if the specific nature of the purported physical cause(s) is not known. If the structural changes detected in the brain have an irreversible aspect, then in a commonsense way we might say that these changes are the immediate cause of the disturbed mind–brain function, but this does not establish aetiology. Unless the changes can be recognized to be a consequence of a proven physical aetiology, the possibility cannot be excluded that they represent the manifestations of the impingement of some ‘psychosocial’ factors, such as the developmental matrix of relationships. At present it would seem that the supporting evidence that would establish schizophrenia as a disorder of proven physical aetiology in all, or even many, cases is lacking.
If the logical constraints upon establishing grounds for causal and aetiological theories within the mind–brain system that have been put forward here are valid, they are not widely recognized within the psychiatric literature. Journals frequently publish papers where inference that aetiology is ‘biological’ is made on the grounds that some biological, brain feature of a mental disorder has been (apparently) reliably identified. Mental illnesses are frequently reduced to ‘neural’ illnesses: consider the following opening sentence of a paper on brain imaging in psychiatry, and published in Science [3]. ‘Psychiatrists have known for at least 100 years that mental illnesses must be fundamentally due to perturbations of normal neural activity in the brain’. While this statement may at first glance seem plausible this is appearance rather than reality. ‘Fundamentally due to’ suggests a cause, and as already argued there is logical difficulty in the description of brain events as causing mental events per se.
Even if we gloss over this ‘in principle’ logical difficulty, there is still no apparent reason why brain events are always more ‘fundamental’ than mental events. In this quotation the mental events in question are mental illnesses, and the brain events are ‘perturbations of normal neural activity’. As has been argued, if some kind of irreversible neural disturbance were present, it might make sense to speak of a mental illnessbeing ‘fundamentally due to’ this neural disturbance in crosssectional time. However this would not, in itself, establish that the mental illness was ‘fundamentally due to’ some physical/neural causal aetiological factor. Furthermore if no such irreversible change in brain structure or function is present in a particular mental illness, no prima facie case exists to support the claim that the neural events must be more fundamental than the mental events. There is greater explanatory economy to say, of at least some mental illnesses, that they are fundamentally due to perturbations of ‘normal’ psychological activity. Whether a description using neural terms or mentalistic terms has the greatest utility in formulating a ‘fundamental’ explanation depends on the nature of the mental illness.
The proper study of the mind
Turning now to proposition two, as stated at the beginning of the paper; if we accept that neuroscientific data and the data of mental experience are two different windows upon the unity referred to as the mind–brain system, we are left with the mystery that they appear to constitute ontologically distinct points of view. It follows that discourse in terms of one cannot be reduced to the other, and the two are not simply interchangeable, a reality which often seems to be lost sight of. It may be that the best we can hope to achieve is a descriptive correlation between the two. Neuroscience can, at least in theory, tell us a great deal about the neural correlates of a conscious experience, but it cannot tell us, at least not directly, anything about the inherent nature of that experience.
Despite those such as Kendell [4] who reject theterm ‘mental illness’ in favour of ‘psychiatric illness’ (Kendell rejects the concept of ‘mental’ in favour of thedescription ‘psychiatric’), mental illnesses are called mental illnesses for a good commonsense reason; namely that they are, for the most part at least, experienced in the mind. The construct ‘mental illness’ reflects this fact, and from the patient's viewpoint the existence of suchan ‘illness’ state is established through his or her awareness of parameters that reflect mental activity, either directly (‘psychological symptoms’) or indirectly (‘behavioural signs’).
Causal and aetiological theories in psychiatry are constructed in terms of mental processes, brain processes or both together (attempts to establish behavioural or sociological aetiological theories are usually instances of theories framed in terms of subjective meaning, that is in terms of the mind). In practice, the patient usually experiences, and the psychiatrist often judges, the presence of mental disturbance in terms of subjectivelymeaningful ‘mental’ phenomena. In these situations only aetiological formulations in terms of mental processes will be of the same ontological order as the primary phenomena under consideration.
In a patient where an aetiological formulation in terms of mental process is possible, this will inevitably be more meaningful (so long as the formulation is a correct one), and therefore offer greater coherence in the particular case, than an aetiological formulation in terms of brain process. A formulation in terms of the mind avoids falling into the ontological ‘explanatory gap’. In other patients, aetiological formulation in terms of mental processes is either not possible or insufficient. Such cases require aetiological theories formulated in part or whole in terms of primary brain processes. To the extent that it is not possible to formulate a sufficient explanation in mentalistic terms (that is in terms of meaning, or the ‘dynamics’ of the mind), then further explanation must be sought in terms of neurophysiological processes in the brain that have an independent aspect. A factor(s) extraneous to the inherently integrated mind–brain system must be exerting an effect via the brain. That is, a physical/organic factor is added to the sequence Me1/Be1→Me2/Be2, and is exerting its effect via ‘B’. For example, in a state of alcohol intoxication, a factor operating independently of the normal integration of the mind–brain system, introduces an element of randomness into the system. It might be predicted that this randomness would be detected as an interference with mental process, and experience confirms that mental capacities are diminished in alcohol intoxication. Similarly, the symbolic richness and meaningfulness of the world of a patient with Alzheimer's disease gradually diminishes with the progression of the disease.
In the hypothetical case of the patient who became depressed following news of a bereavement, it is in theory possible to describe the development of the depressive state of the mind–brain system in neural terms. This would involve documenting the sequence of neurophysiological events, presumably involving many millions of neurones, over time. Such a task would hardly be practical, but an alternative would be to formulate a simplified model documenting the general patterns of brain activity. If such processes can be documented in the brain, then could the vulnerability to depression be conceptualized as residing in the brain? While it must in theory be possible to conceptualize the vulnerability of the mind–brain system to depression in neural terms, as already suggested, such conceptualization will lack meaning.
Neural processes that underlie the presentation of apparent mental disturbance or disorder must presumably either be part of an ongoing sequence of integrated mind–brain activity, or represent a primary organic pathology. Old age, for example, is a specific organic factor that, being linked with a general impairment of cerebral function, may contribute to the vulnerability to depression. If we assume, in our patient, the absence of significant organic aetiological factors requiring description primarily in neural terms, then as has been argued, because bereavement is an experience that impacts upon the mind, the patient's vulnerability to the experience must be able to be conceptualized in mentalistic terms (presumably in terms of the nature of the patient's attachments). The premorbid state of cerebral functioning that confers vulnerability to depression is presumably therefore the neurophysiological correlate of the premorbid state of mental functioning that confers the vulnerability to depression.
It is evident that, in this hypothetical case, only explanation in terms of psychological processes, including the psychological vulnerability factors within the patient's mind, will lead to an aetiological formulation which is inherently meaningful (in the sense of offering understanding rather than a ‘mechanistic’ material explanation), and also potentially meaningful to the patient (whether in fact such a correct formulation is meaningful to a patient will depend upon his or her capacity to understand it). However accurate any model of the process of the patient's altered brain function over time might be, any attempt to employ it in a comprehensive explanatory sense will inevitably take on an arbitrary and reductive quality. It will not be inherently obvious how the documented brain phenomena ‘explain’ the mind phenomena (the patient's experience), because the relationship between them is one of correlation established by observation, rather than one established on the basis of the apprehension of inherently meaningful links.
To restate, because of the ontological ‘explanatory gap’ between formulations in mentalistic terms and formulations in neural terms, a formulation in terms of mind will, if correct, introduce or elucidate the meaning of the patient's experience and behaviour in a waythat ‘explanation’ in terms of constitution or neurophysiology cannot do. I emphasize, ‘if correct’, because: (i) an aetiological formulation in terms of mental processes may be more or less correct or incorrect. An incorrect formulation will not, of course, elucidate the meaning of the patient's experience and behaviour, and may obscure that meaning; and (ii) I am not suggesting that aetiological formulation in terms of mental process is possible for all mental illness, but in any instance where such formulation is possible it will inevitably offer a level of understanding which formulation in terms of neural processes cannot.
Perhaps our hypothetical depressed patient consults the clinician who formulates the cause of his depression asa ‘a biochemical imbalance in the brain’. It may not be unreasonable to postulate that there is a state ofbiochemical ‘imbalance’ in the patient's brain, but can this in any sense logically constitute the ‘cause’ of the disorder?
The fact that what initiated the ‘disorder’ (bereavement) is meaningfully conceptualized in mentalistic terms (the dynamics of the mind), would suggest seeking understanding of the developing state, at least in the first instance, in terms of processes that can be characterized in mentalistic terms. This would mean adopting a working hypothesis that the ‘biochemical imbalance’ is the brain representation in cross-sectional time of a disturbance within an integrated mind–brain system. So long as a sufficient explanation of the patient's clinical presentation can be formulated in mentalistic terms, then from a logical viewpoint an aetiological formulation in terms of neurophysiology, however accurate, remains redundant to meaningful explanation. It may be a valid explanation but it will not be a meaningful one. One might say therefore that it would lack explanatory power.
A principle of explanatory economy could be postulated as follows: it is only when formulation in terms of the dynamics of the mind falls short of providing adequate explanation that it becomes necessary to postulate a neurophysiological causal factor acting independently of an integrated mind–brain system. It would contradict this principle to postulate an explanation primarily in neurophysiological terms in the absence of evidence that some primary and therefore independent pathophysiological process has supervened.
The presence of biochemical disturbance alone in the brains of depressed patients is not sufficient to justify the assumption of a physical/neural aetiology. Supporting evidence will always be required. Where a ‘biochemical imbalance’ idea is employed as a kind of a prioriaetiological ‘theory’, such reasoning is inimical to the process of inquiry and analysis, in other words the process of thinking about, that is necessary to elucidate meaning. In practice the acceptance of this kind of ‘biochemical’ thinking about, for example, depression is often associated with a closure that fails to recognize the possibility of other, potentially more coherent, and clinically more fruitful, avenues of investigation.
The invocation of any aetiological theory without specific and sufficient supporting evidence contributes to premature closure. The ‘concrete’ and measurable aspect of brain events in comparison with mental events may make neural formulations appear attractive, perhaps because they seem easier to grasp than psychological formulations, but as our theory of mind and brain assumes that neural disturbance and mental disturbance accompany one another, we should be aware of the fallacy of invoking physical/organic aetiological theories on the basis of identified neural disturbance without supporting evidence.
I have referred to the possibility of formulating disturbances in the mind–brain system either in terms of neurophysiological processes or in terms of mental processes, the ‘dynamics of the mind’. The nature of the empirical methods employed in order to characterize neurophysiological processes are well known and their conceptual validity apprehended relatively easily. In contrast the empirical methods employed in order to characterize dynamic mental processes are less well known, and their conceptual validity apprehended with greater difficulty. They are essentially the elements of an analytic approach to mental phenomena which seeks to establish meaning, whether employed in psychoanalysis, in analytic psychotherapy or in an observational context. This paper has assumed the validity of such ‘psycho-analytic’ methods, but there remains contention within psychiatry as to the validly of knowledge attained by interpretive methods. Yet it is self-evident that meaning is only conferred upon human experience through interpretation. Pataki [5] points to the ‘explanatory work’ done in ordinary narrative ‘by commonsense “mentalistic” concepts like love, hatred, fear, belief, feelings of weakness and dependence, and so on. These are the concepts we commonly use to make sense of ourselves and others. They are immensely rich concepts’, and they are ‘basic, in (roughly) this sense: it is impossible to see how any description of human action (or of society) can be made without them and their kind in a way which will preserve its subject.’
It is beyond the scope of the paper to enter further into the question of how the validity of knowledge attained through interpretive methods may be established. This would lead inevitably to consideration of the validity of the concept of ‘unconscious’ mental processes.
Mind over matter?
I believe that there is a bias within psychiatry against the investigation of the patient's mind. Without any conceptualization of the dynamic processes occurring within the disordered mind, it is difficult to formulate any aetiological theory that takes factors operating via the mind into account, and difficult to approach treatment via the mind. This results in an explanatory vacuum which neural models are often invoked to fill. Wherever it is possible to formulate a correct aetiology in terms of mental processes, and if a clinician is able to do so, then, for the reasons outlined, this will possess a maximum explanatory economy. It will certainly be meaningful in a way that a ‘neural’ formulation cannot be.
This does not amount to suggesting that mind is more important in psychiatry than brain. A psychiatrist needs to understand about brains and about minds, and there are different forms of psychiatric practice. It is an argument for the utility of giving consideration to the processes taking place within the patient's mind. I have attempted to base this argument upon (i) what seems a reasonable formulation of the mind–brain problem given current knowledge; and (ii) drawing out the implications of this formulation in clinical situations. The main conclusions reached are: (i) that neural brain activity cannot in principle be regarded as causing mental activity (or vice versa), and therefore more evidence or information will need to be considered if the causal relationships between ‘mind’ factors and ‘brain’ factors are to be elucidated in a particular case, or in a particular psychiatric condition; and (ii) that because of the ‘explanatory gap’ between descriptions in mentalistic terms and descriptions in neurophysiological terms, wherever an explanatory formulation of a mental illness in mentalistic terms is possible, this will carry greater explanatory power (meaning) than a formulation in terms of disturbed neural function. If an explanatory formulation in terms of mental processes does not seem possible, or is insufficient, then a formulation in terms of some other primary neural process is necessary.
We have two windows to view the mind–brain system, observation of the brain and observation of the mind. The observation of mental contents and processes, either through introspection or second-person observation, offers a privileged and readily available point of access. It is both the obvious and the logical point to begin investigation into the nature of mental disturbance. Despite this psychiatry appears increasingly preoccupied with the idea of getting at some ‘essence’ of mental disorder through brain research. While we must have an understanding of the manifestations of primary disturbances of the brain in order to understand many psychiatric illnesses, and while we must have an understanding of the pathophysiology of the brain that supervenes in some psychiatric illnesses, this does not mean that a brain focus will serve well to gain understanding of all psychiatric illnesses. Because of the ‘explanatory gap’ we are faced with when we try and understand mind in terms of brain, a ‘mind’ focus will better serve understanding in the absence of specific independent or irreversible pathophysiological disturbances.
Footnotes
Acknowledgements
I am grateful to the Melbourne philosopher Tamas Pataki for his helpful critique of this paper.
