Clinical Presentation
A healthy 33-y-old man was hiking with 2 friends in the Spanish Pyrenees during the summer. In the early afternoon, he reached the high point of the hike (2400 m). Suddenly, he heard a boom and felt something hit his left shoulder. He was unconscious for a few seconds. When he awoke, he was rolling down a slope. He seemed to be paralyzed. He stopped at a flat spot about 15 m below the high point. A few seconds later, he smelled burnt clothing. He was then able to make limited movements and called for help. His left arm was blue for a few minutes. His friends found him and notified emergency services. A rescue helicopter extricated him, with some difficulty because of the weather, and transferred him to an air ambulance. Vital signs were respiratory rate 16·min-1, heart rate 86 beats·min-1, blood pressure 164/76 mm Hg, and oxygen saturation by pulse oximeter (SpO2) 99%. He still had weakness of the legs during extrication that resolved before he reached the hospital.
When the patient arrived at the hospital, he said that something had exploded at his side, knocking him down the mountain. He reported back pain and bruises from the rocks over which he had rolled. On examination he was alert, in no respiratory distress, and able to converse normally. His Glasgow Coma Score was 15. He was diaphoretic. Vital signs were respiratory rate 14·min-1, heart rate 78 beats·min-1, blood pressure 130/77 mm Hg, and SpO2 100% on room air. Peripheral pulses were full and regular. Capillary refill time was <2 s. The chest was nontender without deformity, the abdomen was soft and nontender, and the pelvis was stable. The patient had full range of motion of all extremities. There were no apparent extremity injuries other than contusions. Motor and sensory examination was normal, without weakness or sensory deficits. An electrocardiogram showed normal sinus rhythm without ectopy or ischemic changes.
A peripheral line was placed and fentanyl 150 μg was administered intravenously. The secondary survey revealed erythematous discoloration of the skin, extending from the superior left scapula along a paraspinal course to the right leg and foot, and abrasions of the lower back and left buttock (Figure 1). There were also abrasions where the pants and right shoe were torn. He was transferred to the burn unit for further management.
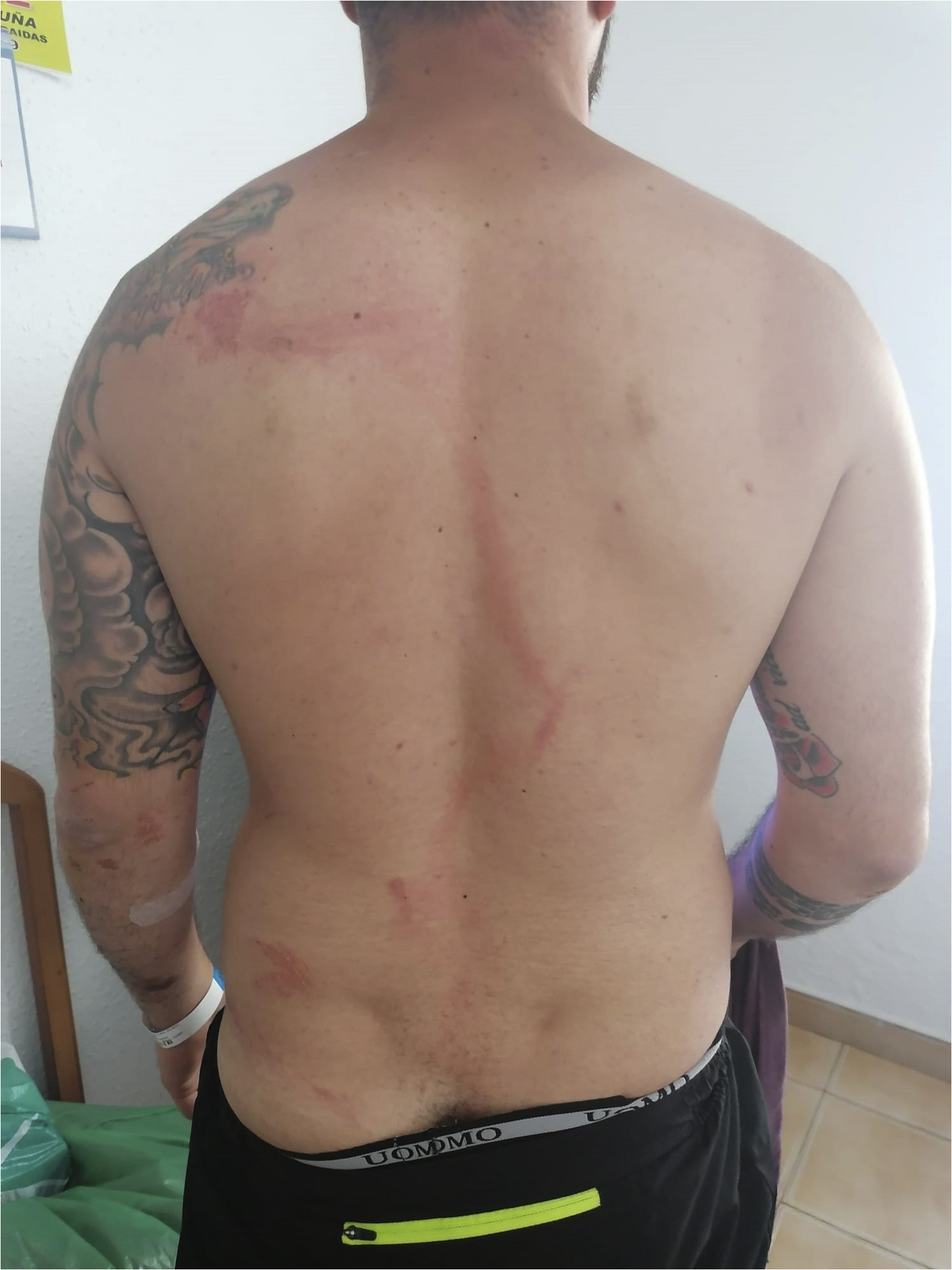
The victim after the event.
What is the diagnosis? How would you manage this condition?
Diagnosis
Lightning injury with keraunoparalysis.
Discussion
On admission to the burn unit, the patient was diagnosed with lightning injury, rhabdomyolysis (creatinine kinase 3497 IU·L-1), and keraunoparalysis (which had resolved). He was discharged, completely recovered, the next day. He did not require further treatment, except for dressing changes for the burn on his back and right leg. Six months later, the patient was seen in follow-up, was still fully recovered, and had resumed an active lifestyle. The only sequelae were scarring of the back and right leg.
Lightning injuries can be fatal, but the vast majority of people struck by lightning survive. Although data are incomplete, lightning causes about 24,000 deaths worldwide every year, with about 250,000 injuries. 1 Long-term medical and psychiatric sequelae are common.
Lightning does not usually cause burns. Most burns from lightning are superficial, caused by vaporization of sweat on the skin and in clothing. Unusual types of burns caused by lightning include punctate and linear burns. Lightning can also produce transient feathering patterns on the skin (Lichtenberg figures) that are not burns. Feathering is pathognomonic for lightning injury but is not always seen. 2
Figure 1 shows a linear burn that took about 10 d to heal. The burn tracked from the area of the left scapula to the right foot, affecting areas that were damp from sweat. The right leg of the pants was destroyed, with burnt areas. The patient recalled that he felt “a kind of electricity” in the left shoulder that went down the back then to the right foot. There was no entrance or exit wound. Entrance and exit wounds are rare in lightning injury because the duration of current is too brief (10–100 ms) to overcome the resistance of the skin. Lightning usually travels over the surface of the skin, a phenomenon known as flashover. 1
The patient explained that he was paralyzed initially and then gradually recovered full movement. Transient neurologic symptoms, including weakness or paralysis, can begin immediately after a lightning strike. Transient paralysis can be caused by keraunoparalysis (lightning paralysis), in which paralysis of 1 or more, usually lower, extremities is associated with intense vaspospasm. If there has been trauma with the possibility of spinal injury, spinal motion restriction should be instituted. This should be maintained if paralysis persists after pallor or pulselessness of the extremity has resolved. 1 Keraunoparalysis generally lasts from 1 to a few hours before resolving spontaneously and completely.
Men are 5 times more likely than women to sustain a lightning injury. Lightning injuries in temperate climates are most frequent during summer months, especially on weekends and during outdoor recreational activities. 3 Most lightning injuries are avoidable. 4 Education on how to prevent lightning injuries has the potential to decrease the numbers of injuries and deaths.
Footnotes
Acknowledgements
Author Contributions: All authors wrote and revised the manuscript.
Financial/Material Support: None.
Disclosures: None.
