Case presentation
An 18-year-old volunteer on a sustainable development expedition in the Shinyanga Region of Northwestern Tanzania experienced a painful erythematous lesion on her right forearm, which we noted had 6 pale papules. There was an identical corresponding lesion on her upper right arm, which “kissed” when her elbow was fully flexed (Figure 1).
The volunteer was young and fit with no significant medical history. The only medication she was taking regularly was Malarone (atovaquone/proguanil hydrochloride, GlaxoSmithKline [GSK], Middlesex, UK) for antimalarial prophylaxis.
The volunteer had worked on a building site, performing work that involved carrying cement blocks, an activity that left several participants with abrasions in similar areas of the forearm. The patient had not sustained such an abrasion before the appearance of the lesions but had been in close contact with the cement blocks and other building materials.
Volunteers lived entirely outside, sleeping in large, army-style “sleeper tents” under personal mosquito nets. They followed strict rules, including wearing long clothing and N,N-diethyl-meta-toluamide (DEET) insect repellent to prevent mosquito and other insect bites. The volunteer did not have any recollection of an insect bite or sting to the affected area.
What is your diagnosis? How would you manage this case?
Initial differential diagnoses
Our initial differential diagnoses included a localized reaction to an insect bite or sting and contact dermatitis from cement materials. Treatment therefore consisted of oral paracetamol and chlorphenamine. We also provided the patient with a topical antihistamine cream to use as required.
During the next 24 hours, the white papules started to coalesce to form pustules (Figure 2). Suspecting a secondary bacterial infection, we switched the treatment to a topical antibiotic cream (fusidic acid). The lesions were cleaned and dressed daily as the participant continued to work on the building site.
Despite treatment with topical antibiotics, the lesions did not improve during the following 48 hours. The forearm pustules began to discharge, and an area of spreading erythema evolved, surrounding the initial lesion and raising suspicion of erysipelas or cellulitis (Figure 3). The border of the erythema was marked, and oral antibiotics (flucloxacillin) were commenced.
During the next 24 hours, the erythema decreased, and the lesion improved significantly: discharge of pus stopped, and the lesion began to show signs of healing within 48 hours. Although secondary infection was evident and was treated successfully by oral antibiotics, the initial provocation was unclear.
What was the diagnosis?
Two weeks after presentation, the volunteer was discussing the lesion with our guide who was well versed in the local flora and fauna of rural Tanzania. He suggested that the lesion was caused by contact with the Nairobi fly (Figure 4).
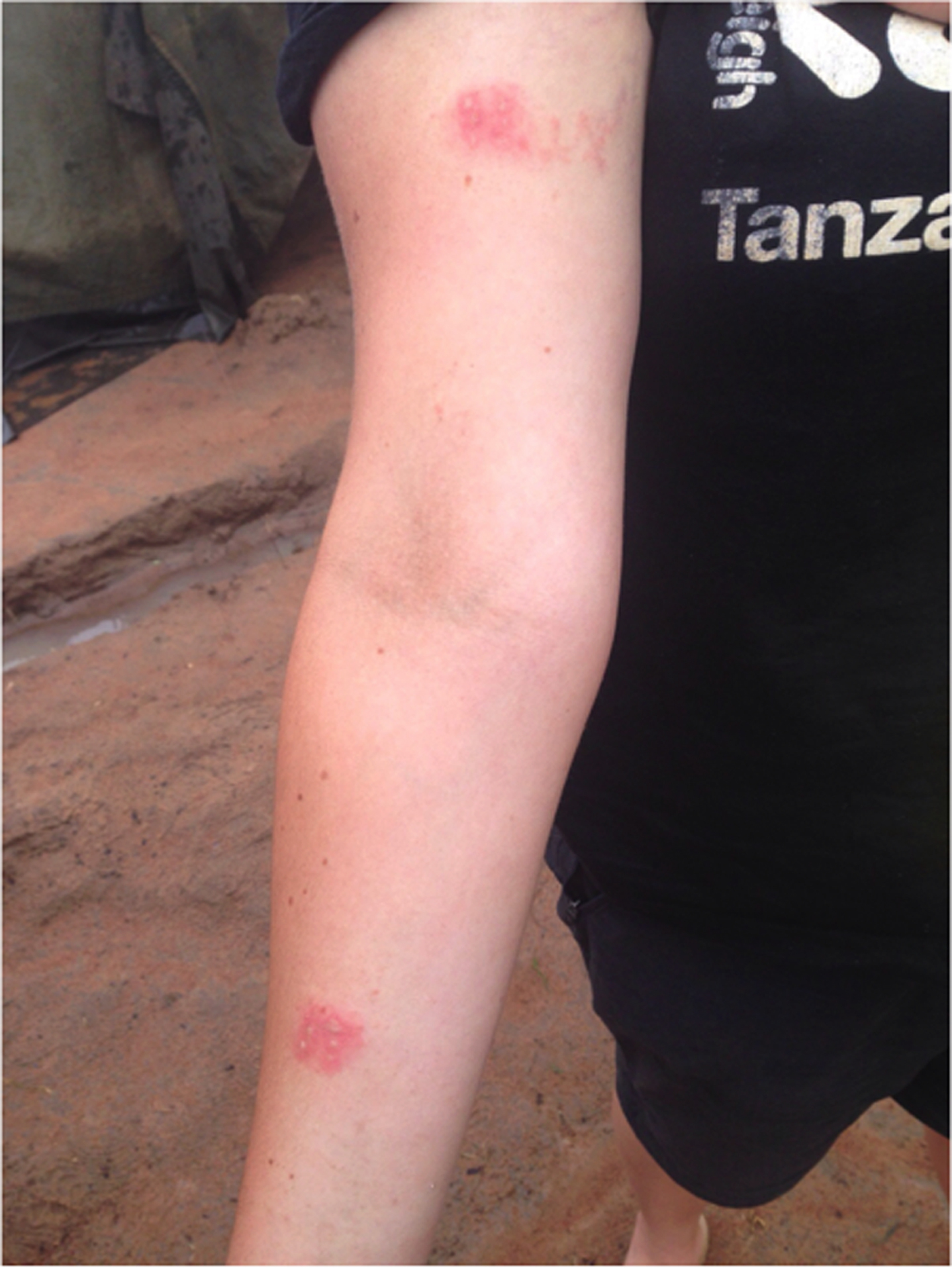
Initial presentation: painful and erythematous contiguous lesions on the right upper arm and forearm.
The diagnosis was a skin reaction to the toxic haemolymph from the Nairobi fly, with spread of the cytoxic secretion, pederin, via bending the elbow, resulting in a “kissing lesion.” Secondary bacterial infection is a common sequela due to contamination of broken skin.
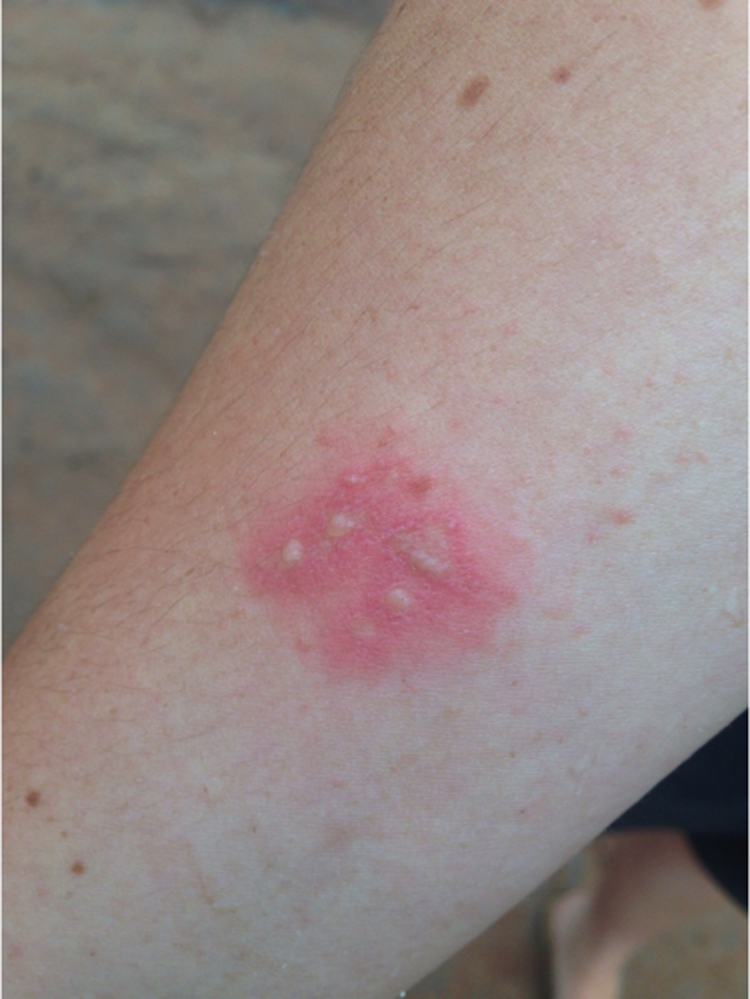
Pustules on the right forearm.
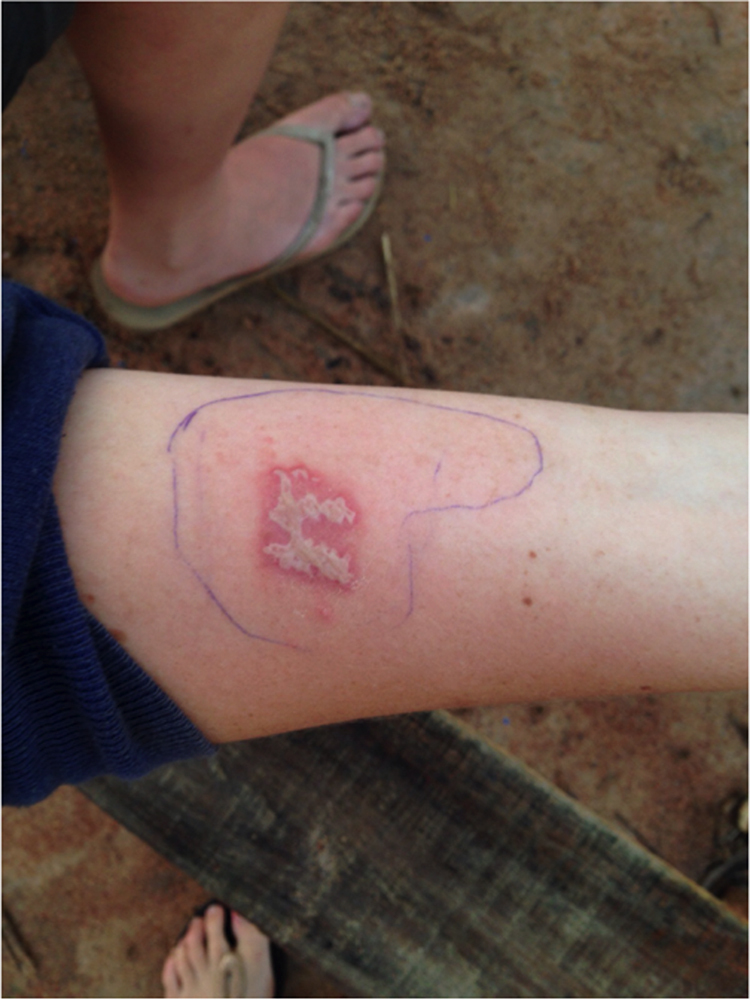
Consolidation of pustules with a surrounding area of erythema on the right forearm, gradually reducing following the initiation of oral antibiotics.
How should this case be managed?
The East African species of Nairobi fly are actually rove beetles and are unable to fly. 1 They also do not bite or sting, 1 and this is why there was no recollection of a possible reason for the lesion in the patient’s history. As our experienced guide informed us, the lesions occur after exposure to cytotoxic pederin, which is released when the beetle is crushed against human skin. 1 In this case, elbow flexion resulted in a kissing lesion because the area was not immediately washed and transfer of pederin occurred.
Our choice of treatment options in this case was not optimal. Topical antihistamine cream seemed to be of little assistance. Similarly, topical fusidic acid did not improve the lesions or prevent the secondary infection that followed. Although the lesion was largely covered, chance of infection in the expedition environment was high and possibly exacerbated by regular application of topical creams. We are now aware that thorough washing and the application of cold compresses, followed by application of topical steroid cream and oral antihistamine, is the standard treatment for Paedrus dermatitis. 1 Severe or persistent cases also have been reported, for which oral prednisolone and intralesional triamcinolone acetonide injection also may be considered. 2
Cases of Paedrus dermatitis tend to occur in the rainy seasons of tropical and temperate climates, 1 as was the case for our patient, with the lesion occurring in November, during one of the Tanzanian rainy seasons. The beetles like the moist decaying vegetation of marshes and agricultural fields. 1 Our camp was set on the agricultural fields belonging to a local school.
We would like to raise awareness of this unusual skin condition in the hope that early recognition will prevent complications such as secondary bacterial infection.
Follow-up at 8 weeks after initial presentation showed the lesion continuing to heal well, with an area of hypopigmentation (Figure 5). This has also has been described in the literature. 1

Nairobi fly, a species of rove beetle from the genus Paedrus (US Army Public Health Command). 3
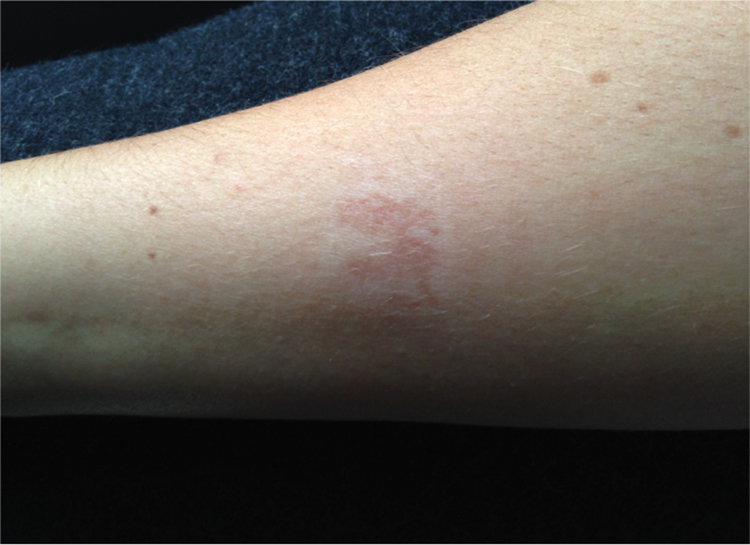
Forearm lesion 8 weeks after initial presentation denotes healing with an area of surrounding hypopigmentation.
Key learning points
In rural Tanzania, the Nairobi fly can cause Paedrus dermatitis, presenting as linear, vesiculobullous, or pustular lesions, which may be “kissing” in nature. The lesions can appear “out of the blue.” Without any obvious provocation, clinical knowledge of the condition is essential. There is great value in consulting with knowledgeable local people. The first-line treatment is thorough washing and the application of cold compresses, followed by topical steroid cream and oral anti-histamine; in severe or persistent cases, oral or intralesional steroids also can be used.
Acknowledgments: Florence Deasy, Raleigh International Volunteer, Tanzania Expedition 15K, Leons Mlawila, Raleigh International Trek Guide, and Tanzania Expedition 15K.Author Contributions: Drafting of manuscript, critical revision of manuscript, and approval of final manuscript (SJM, HJB).
Financial/Material Support: None.
Disclosures: None.
