Abstract
Objectives
In low-income countries, snakebites are frequently managed in rural areas in health centers with severely constrained resources. Many healthcare providers in these settings have limited access to the numerous and relatively expensive laboratory studies used to diagnose envenomation. The relatively simple and inexpensive 20-minute whole blood clotting test (WBCT) has been recommended by several international organizations for the diagnosis of certain venomous snakebites. This study proposes to confirm the utility of the WBCT as the sole laboratory diagnostic tool to determine systemic envenomation in hematotoxic snakebite management in severely resource-constrained areas of the world.
Methods
The authors reviewed all 110 cases of snakebite during a 6-year period in a small hospital in rural Ecuador using the WBCT.
Results
All cases presented within 24 hours of snakebite. Twenty cases revealed normal coagulation with no clinical evidence of systemic envenomation. Ninety cases had no evidence of clot formation (positive WBCT) at 20 minutes, suggesting systemic envenomation. Of these 90 cases, according to a classification scale, 54 were mild, 26 were moderate, and 10 were severe envenomations requiring transfer to tertiary care. All mild and moderate systemic envenomations were successfully treated at the rural hospital. All severe envenomations were treated initially with antivenom before transfer to tertiary care. One patient with severe envenomation died in tertiary care.
Conclusions
The WBCT was predictive of the presence or absence of systemic envenomation from snakebite in our region. The WBCT guided the successful management of mild and moderate systemic envenomation, and spared patients with no evidence of systemic envenomation from potential side effects of antivenom.
Introduction
Worldwide it is estimated that every year several million persons are bitten by snakes, with envenomations ranging from 421,000 to 1,841,000 and with as much as 94,000 deaths and even greater permanent disabilities resulting. 1 Snakebite primarily affects frequently marginalized rural populations such as agricultural workers, children, and indigenous peoples, for which it is included on the World Health Organization’s list of neglected tropical diseases. 2 This public health problem is greatest in countries in which healthcare systems are oftentimes challenged at many levels to manage snakebite. Furthermore, snakebite’s rural predominance is precisely where national healthcare systems are weakest.
In northwest Ecuador, the town of Pedro Vicente Maldonado (PVM), on the western slopes of the Andes at an altitude of 600 m, is the geographic center of a catchment area that ranges in altitude from 200 m (tropical) to 1300 m (subtropical) along the equatorial line. Hospital PVM is a small, 15-bed hospital that serves this area and generally the only hospital that regularly stocks antivenom.
In northwest Ecuador, Bothrops asper (lancehead, equis) and Lachesis muta (bushmaster, verrugosa, pudridora) from the Crotalinae (pit viper) subfamily are likely responsible for the majority of severe venomous snakebites. 3 The geographic distribution of Bothrops ranges from Argentina to Mexico, whereas Lachesis spp. are found from Central America to Bolivia and southeastern Brazil. 4
Bothrops spp. are the most dangerous venomous snakes in Ecuador. 5 East of the Andes, Bothrops atrox is most important. 6 However, west of the Andes, B. asper is the major threat. Bothrops is considered highly dangerous for its size (>2 m in length; head size, >9 cm), quantity of venom injected through its long fangs (potentially >2 cm), population density and reproductive capacity, immobility and camouflage during daylight, willingness to bite when disturbed, and frequent association with human dwellings. 7 L. muta are the longest vipers in the world (>3 m), demonstrate typically passive behavior, and hunt nocturnally. Venom from both of these pit vipers displays proteolytic, hemorrhagic, myotoxic, and clotting activity. Complications are described elsewhere, but include coagulopathies resulting in hemorrhage or thrombosis, limb loss, renal failure, shock, and ultimately death (Figure). 8
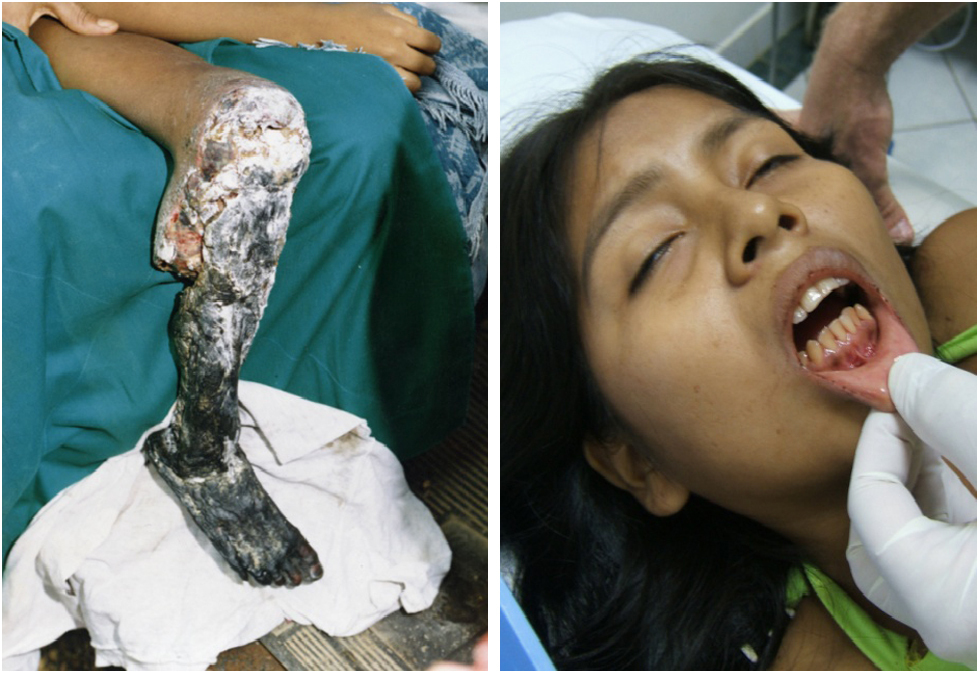
Bothrops spp. envenomation complications: left, necrotic leg secondary to direct necrotic effects of B. asper venom 1 week after envenomation; and right, gingival bleeding 4 hours after envenomation (photographs by D. Gaus).
In rural tropical and subtropical areas where these species exist, the frequently severely constrained healthcare infrastructure is challenged with the task of diagnosing and managing venomous snakebite with limited resources. Conversely, tertiary-care hospitals in large urban areas generally have limited experience with venomous snakebite. The 20-minute whole blood clotting test (WBCT) has been recommended by several institutions for the early diagnosis and management of venomous snakebites in such low-resource settings. 9
The WBCT is used as a marker to determine systemic toxicity, as incoagulable blood is a telltale sign of systemic envenomation. The test requires 3 to 5 mL of fresh blood from venipuncture placed in a new, clean, dry glass test tube. It is maintained undisturbed at room temperature for 20 minutes, at which time it is tipped to determine whether clotting has occurred. If the specimen clots, the patient is determined not to have suffered a systemic hematotoxic envenomation, and no antivenom is required. Conversely, if the specimen does not clot, the patient is assumed to have systemic hematotoxic envenomation. This study reports on the utility of the WBCT in a rural hospital in a low-income country.
Methods
We retrospectively reviewed all 110 snakebites that presented to Hospital Pedro Vicente Maldonado (HPVM) during a 6-year period from April 2005 to September 2011. This hospital has standardized electronic medical records, simplifying the identification of all snakebite cases using snakebite, intoxication, and snake accident (all in Spanish).
The standardized procedure followed for all possible snake envenomations included a confirmatory history, physical examination, and WBCT at the time of presentation to the emergency department. A positive WBCT (no clot at 20 minutes) was followed with the placement of a peripheral intravenous catheter. Severity was based on a classification scale created by the hospital that combined that of the manufacturer’s antivenom prescribing information and a commonly used toxicology textbook in Ecuador, used consistently over the 6-year period (Table 1).10,11
Classification scale of severity of hematotoxic envenomation and corresponding initial antivenom dose
WBCT, whole blood clotting test.
Each vial of antivenom is reconstituted with 10 mL of normal saline and can neutralize a minimum of 25 mg of Bothrops. asper or Bothrops atrox venom and 20 mg of Lachesis muta venom. But total required dose per patient can vary widely.
Vials of Probiol polyvalent lyophilized antivenom, produced in Colombia for Bothrops spp, Crotalus, and Lachesis, were reconstituted and mixed in 100 to 250 mL (depending on the number of vials used initially) of normal saline solution and piggybacked onto the peripheral intravenous infusion set with a stopcock. 10 The calculation of the number of vials was based on severity of case and size of the patient (children generally paradoxically requiring more antivenom) according to the manufacturer recommendations. Six hours after antivenom administration, the WBCT was repeated. If positive, the rationale for antivenom administration was repeated, followed by another WBCT at 6 hours after administration. This process was repeated until the WBCT turned negative.
A negative WBCT (presence of clot at 20 minutes) at presentation resulted in observation and repeat WBCT if the alleged snakebite was within 3 hours of presentation to the emergency department.
Patients with a positive WBCT underwent urinalysis for hematuria, and serum creatinine levels were measured for renal dysfunction. Patients were maintained without oral food intake. Intravenous fluid resuscitation and analgesia were used on an as-needed basis. No medications were administered intramuscularly (high risk of hematoma formation if systemic envenomation present). Antibiotics were not administered prophylactically. Nonsteroidal anti-inflammatory medications were avoided. All patients classified as severely envenomated received the initial bolus of antivenom, but all were transferred to tertiary care.
Patients with a positive WBCT also routinely received an antihistamine (diphenhydramine 25 mg) and hydrocortisone 100 mg intravenously before antivenom administration. We used this pharmacotherapy in an attempt to minimize antivenom side effects based on the following: the manufacturer of the specific antivenom used in the study recommends pretreatment with antihistamine; one study suggested a possible benefit to reduce acute adverse reactions through this combination at the time this current study commenced 12 ; a significant risk of potentially life-threatening, adverse reactions to antivenom exists; pretreatment intradermic testing with antivenom to predict adverse reactions is unreliable; and these 2 pharmacologic agents have a low side effect profile. More-recent studies have shown the use of combined hydrocortisone and antihistamine to be ineffective at preventing such reactions. 13
Results
One hundred-ten snakebites presented to HPVM during a 6-year period from April 2005 to September 2011 (Table 2). The majority of patients were farmers, either actively working (typically with a machete) or walking through fields on trails, although 26 patient charts did not reveal the activity at the time of the snakebite. Peak months for bites were December to February, coinciding with the local rainy season. All 110 patients presented to HPVM within 24 hours of their alleged snakebite. Ninety cases demonstrated a positive WBCT (absence of clot at 20 minutes), suggesting systemic envenomation. One severely envenomated patient died shortly after arriving at the hospital before transfer to tertiary care could be arranged or antivenom administered, presumably from an intra-abdominal bleed, for which we excluded that patient from the study. The family refused autopsy. Two of the severe cases presented with neurologic deficits consistent with intracranial hemorrhage. Antivenom was administered during transportation to tertiary care in each case. One patient perished and 1 survived. No other deaths were recorded among the other transfers, resulting in a total of 1 death in the study group.
Results of 110 patients evaluated for hematotoxic envenomation
WBCT, whole blood clotting test.
One additional patient died immediately on arrival to hospital before treatment.
Eighty-eight of the patients (80%) were bitten on the extremities. Bite location was more prominent in the lower extremities (47 patients or 53%) than the upper extremities (37 patients or 42%). Of the 90 snakebites identified as systemic envenomation, 40 were identified as likely Bothrops spp, 2 were likely Lachesis, and 48 were unidentified. We acknowledged that definitive identification by rural communities is uncertain. We strongly suspected that most unidentified bites were Bothrops spp. Although a small number, 15 of the snakes were killed and brought in, all of which were Bothrops spp. Additionally, antibody to Lachesis spp was present in only 18% compared with 60% for Bothrops spp in a study of 223 indigenous Ecuadorians, albeit in eastern Ecuador. 14
The WBCT was predictive of the presence of systemic envenomation in each case. In patients with a negative WBCT, suggesting no systemic envenomation, their clinical presentation also did not suggest a significant envenomation (absence of frank bleeding; no significant edema at the alleged site of snakebite). The WBCT in patients with mild-to-moderate systemic envenomation was useful in ongoing management after the initial administration of antivenom, guiding repeat dosing of antivenom. In the 10 patients classified with severe envenomation with an appropriate snakebite history, the WBCT was not performed initially to expedite antivenom administration before transfer to tertiary care.
Discussion
The World Health Organization and other international institutions promote the use of the WBCT as a diagnostic tool in the initial management of suspected venomous snakebite. 15 Our study supported this recommendation. Our review of 110 cases managed either completely (90%) within our rural hospital or initially with subsequent transfer to tertiary care (10%) confirmed the utility of this simple but effective test. A negative WBCT spared the patient of exposure to potentially life-threatening adverse reactions (described elsewhere) to antivenom. 16 In patients from areas with endemic venomous snakes, an appropriate history of snakebite, and clinically severe systemic envenomation, proceeding directly to antivenom therapy without prior WBCT prevented delay in providing life-saving therapy.
Furthermore, our experience illustrated that in the ongoing management of mild and moderate systemic hematotoxic envenomation, the WBCT continued to be a useful clinical tool to guide subsequent antivenom therapy. It permitted identification of systemic envenomation in patients without other evidence of systemic venom toxicity, allowing earlier administration of potentially lifesaving antivenom. We must point out, however, that the WBCT is not diagnostic for neurotoxicity, and pit vipers with neurotoxic venoms are not known to be from the area serviced by our hospital. But in other regions, some pit vipers produce neurotoxic venom components. Most also produce components that cause local tissue injury and coagulopathy (and, thus, are likely to produce a positive WBCT), but a few (eg, North America’s Mohave rattlesnake, Crotalus scutulatus), as well as most members of the family Elapidae (coral snakes, cobras, mambas, sea snakes, and their kin), can produce potentially life-threatening paralysis hours after biting, without coagulopathy or other signs and symptoms. Thus, the WBCT may not be as reliable to detect systemic envenomation in areas of the world where such snakes are found.
The WBCT appeared to be useful in a low-income country in which more-sophisticated laboratory analysis was likely to be limited, particularly in remote or rural areas where these bites occur with greater frequency. This study suggested that more-sophisticated laboratory testing such as prothrombin time, international normalized ratio, partial thromboplastin time, fibrinogen, fibrinogen split products, and others may not be required.
The combination of the complexity of snake venom and the antivenom’s dangerous side effects demand significant clinical skills for successful snakebite management. Perhaps the greatest contribution the WBCT can make to clinical practice is to ensure that patients without systemic envenomation do not receive antivenom, sparing them potential adverse drug effects and preserving a valuable, limited resource.
During this study, we transferred all severely envenomated patients to tertiary care after initial stabilization and antivenom administration in the event that a life-threatening bleed would occur for which we were not prepared at a rural hospital. The 1 death that occurred was predictable at the time of presentation to our hospital. One patient with an intracranial bleed survived in tertiary care without ventilator support. The remaining severely envenomated patients all survived after transfer to tertiary-care facilities. In retrospect, some of these severely envenomated patients could likely have been managed at our rural hospital. We observed that if they were stable after initial fluid resuscitation and infusion of antivenom at the time of transfer, they remained stable in tertiary care.
In Ecuador, most medical education occurs in urban areas where snakebite is infrequently encountered. Hospital PVM trains family physicians in a 3-year program in which snakebite management is a required skill. We are unaware of another formal medical residency program in Ecuador that provides appropriate venomous snakebite management skills. In fact, most government physicians working in rural ministry of public health facilities are not residency trained, exacerbating this knowledge gap. Because of snakebite envenomation’s public health impact, we suggest that rural healthcare personnel in countries such as Ecuador receive training in this area.
We understand that management of a venomous snakebite victim who presents with hypotension and hemorrhage can be intimidating for even experienced physicians. Healthcare workers need appropriate skills, medications, and referral systems for this complex condition. The WBCT is a relatively simple, inexpensive test that physicians can use in many settings to make important clinical decisions about hematotoxic snakebite management.
Limitations
The uncertainty involved in snake identification, particularly retrospectively, could potentially have resulted in the misidentification of species, given the unreliable knowledge distinguishing one species from another. Living in this rural area, we have discovered at least anecdotally that local inhabitants are quite accurate with their snake identification. Nevertheless, the uncertainty persists.
Conclusions
This study confirms the utility of the WBCT as a useful tool in the management of hematotoxic snakebite. It permits identification of systemic envenomation in patients without other evidence of systemic venom toxicity, allowing earlier administration of potentially lifesaving antivenom. The WBCT can also ensure that patients without systemic envenomation do not receive antivenom. It supports the idea that small rural hospitals in Ecuador and other low-income countries with well-established treatment protocols and the availability of appropriate antivenom can successfully manage hematotoxic systemic snakebite envenomation in a timely fashion with a potentially great impact on morbidity and mortality.
Footnotes
Acknowledgment
The authors would like to thank the physicians and nurses who participated in the management of these snakebites during the period of the study.
☆
Sources: No outside support was received.
