Abstract
Horner's syndrome involves a triad of eyelid ptosis, miosis, and facial anhidrosis that results from disruption of the oculosympathetic pathway. Acquired Horner's syndrome is associated with a variety of medical conditions including Pancoast tumor and carotid dissection. We report the unique case of a 47-year-old man presenting with Horner's syndrome 4 weeks after black widow spider envenomation. Workup did not reveal any alternative explanatory etiology. We hypothesize that late sequelae of black widow spider envenomation secondary to autonomic nerve injury or retrograde axonal transport after mechanical inoculation may have led to an acquired defect in the oculosympathetic pathway resulting in a Horner's syndrome. This case introduces a rare cause of Horner's syndrome and highlights the importance of environmental exposures in the evaluation of these patients.
Introduction
Horner's syndrome is a well-recognized clinical triad of eyelid ptosis, miosis, and facial anhidrosis caused by disruption of the oculosympathetic nerve pathway as it courses from the hypothalamus to the eye. Acquired Horner's syndrome is known to be associated with a variety of medical conditions including brainstem stroke, 1 carotid dissection, 2 and Pancoast tumor, 3 as well as other more rare entities.
Case Presentation
A 47-year-old construction worker had a witnessed spider bite while clearing a pile of brush. Reporting an occupational familiarity with this species' distinctive appearance, he identified it as a black widow (Latrodectus mactans) and promptly brushed it from his right thigh with the back of his hand. Two days after the bite, he had chills, nausea, headache, myalgias, and localized erythema, pain, and diaphoresis on the right thigh. Four days after the bite, concurrent conjunctival irritation developed with hyperemia, chemosis, and epiphora, after which his mother-in-law commented on his left eyelid drooping and anisocoria.
Seven days after the bite, local pain, hyperesthesia, erythema, and mild swelling of the right thigh developed. The patient underwent incision, drainage, and oral antibiotic treatment for presumed secondary bacterial infection. Twenty-one days after the bite, he had recurrent lower extremity cellulitis and was admitted for intravenous vancomycin, after which he was transitioned to oral doxycycline for a 10-day course. During evaluation, left ptosis and miosis was noted. Computed tomography angiography of the head and neck was negative for dissection or aneurysm. Radiography of the chest was without Pancoast tumor. He was referred for outpatient evaluation.
Thirty days after the bite, neuroophthalmologic examination demonstrated 2 mm anisocoria with miotic left eye greater in dim light, and left eyelid ptosis with obscuration of the iris but sparing the pupil. He also reported anhidrosis over a left V1 distribution. Workup was negative for explanatory systemic abnormalities, and he was diagnosed with acquired Horner's syndrome secondary to black widow spider envenomation.
Discussion
Horner's syndrome includes the triad of partial ptosis, ipsilateral miosis, and anhidrosis (Figure). Interruption of the sympathetic pathway to the eye and face results in decreased sympathetic innervation of the pupil dilator, the Mueller muscle of the upper eyelid, and the inferior tarsal muscle of the lower eyelid. Sympathetic innervation originates in the posterior hypothalamus and descends in first-order central neurons ipsilaterally in the reticular formation of the brainstem. These nerves descend in the spinal cord, terminating from C8 to T2 in the ciliospinal center. Second-order peripheral preganglionic neurons exit the spinal cord through ventral roots and travel over the lung apex to the superior cervical ganglion. Sudomotor and vasoconstrictor fibers exit at this level before where third-order neurons exit and travel along the internal carotid artery to the cavernous sinus. These fibers exit along the ophthalmic division of the trigeminal nerve to innervate the pupil dilator and the Mueller muscle.
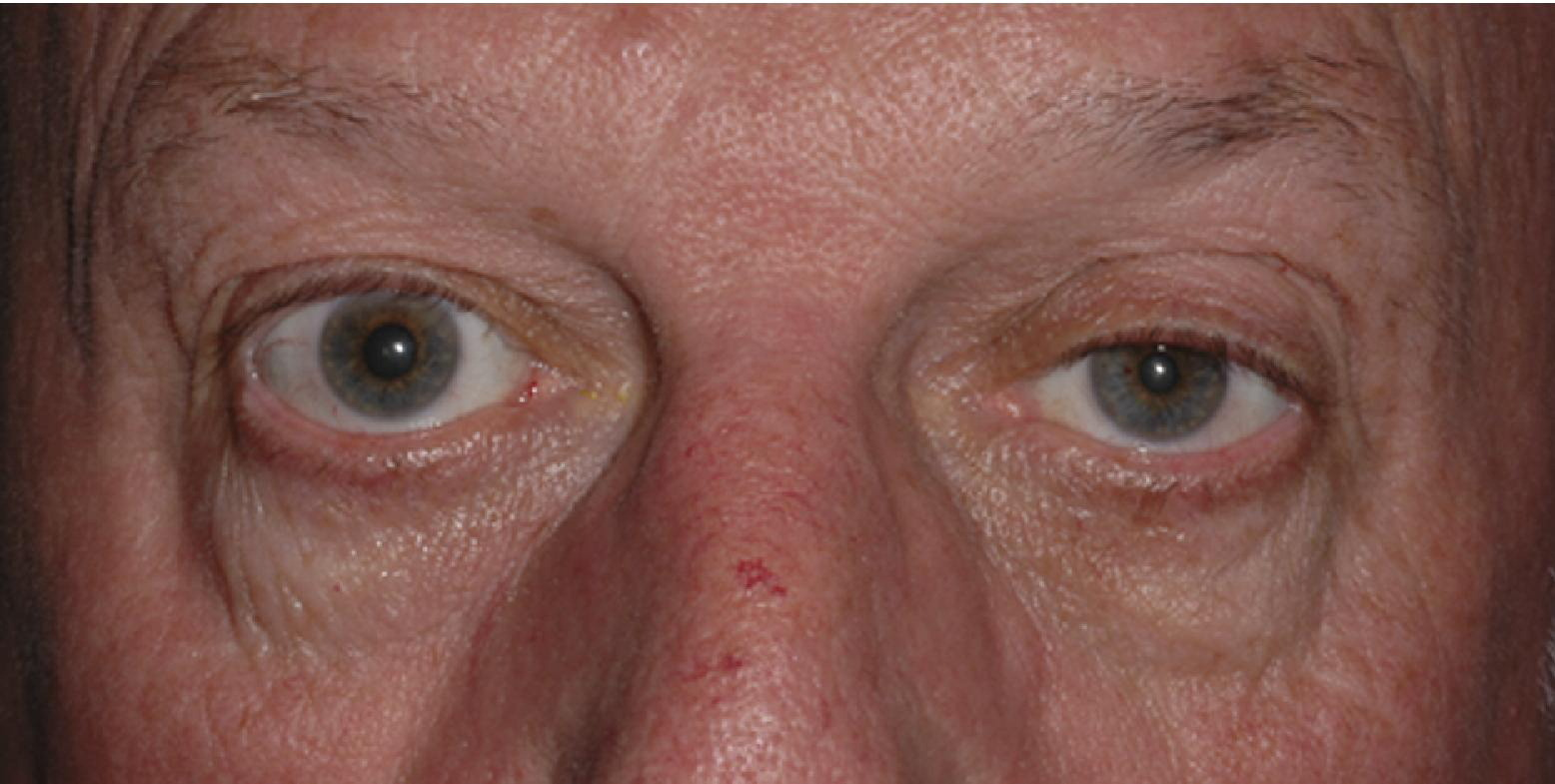
A representative photograph of a patient with left ptosis and miosis consistent with left-side Horner's syndrome demonstrates the pathology present in this case.
Disruption at any point of this circuit results in clinical Horner's syndrome. Acquired causes include brainstem infarction, 1 carotid artery dissection, 2 Pancoast tumor, 3 and neck trauma. 4 Less common causes include intrathecal anesthetic such as in obstetrical procedures, 5 thyroid malignancy 6 or complications of thyroidectomy, 7 and cervical nerve root block. 8 One prior case has reported an association between black widow spider envenomation and subsequent development of Horner's syndrome. Similar to our case, the patient presented approximately 1 month after the initial envenomation; however, in this prior case, the systemic response to the initial bite was more robust and required several days of inpatient hospitalization. 9
Black widow spiders (Latrodectus species) are 1 of 2 venomous spiders found in North Carolina. Black widows are highly recognizable given their characteristic red “hourglass” shape on the abdomen of the female. The venom is a potent neurotoxin (alpha-latrotoxin) that alters the structure and function of nerve terminals by affecting calcium metabolism. A massive calcium uptake across plasma membranes causes rapid and large releases of acetylcholine, noradrenaline, dopamine, and gamma-aminobutyrate. That results in small end-plate action potentials that ultimately block neurotransmission and result in degeneration of the affected nerve terminals, likely due to depletion of synaptic vesicle contents. 10
Clinical response varies in severity and depends on a number of factors such as the size of the spider, time of year, location of bite, number of bites, and physical condition of the patient. Most bites occur when the spider is disturbed in objects such as clothes, furniture, sheds, and woodpiles. 11 Black widow spiders control the amount of venom they inject by using striated muscle to squeeze a metered amount of venom into the victim. 12 The bite is usually painful, and within hours, victims typically have local pain that gradually worsens along with local sweating and sometimes piloerection. Three quarters of patients bitten have only local symptoms and signs and do not progress to systemic envenomation. 13 In the minority of cases, no local reaction occurs, and generalized or remote pain or sweating is observed. 11 Muscle cramps, spasms, fasciculations, and patchy paralysis have also been noted. 12 Symptoms last an average of 3 to 6 days, although myalgias and malaise may persist for weeks. 14
In this case, as has been previously proposed, 9 it is possible that sympathetic fiber damage in this patient occurred as a late sequela of autonomic nerve injury. Autonomic abnormalities have been demonstrated in patients after spider envenomation and include both sympathetic and parasympathetic abnormalities. 15 Long-term effects of black widow spider envenomation have also been shown to persist well after the initial envenomation. 16 Damage could have occurred along central or preganglionic nerve fibers of the oculosympathetic pathway before the superior cervical ganglion given the facial anhidrosis. The patient's symptoms stabilized and improved over the 4 weeks of follow-up, suggesting an acute nerve injury sustained at the time of the envenomation. It is difficult, however, to explain the laterality of the patient's symptoms through such a systemic process.
Alternatively, we cannot exclude the possibility that direct mechanical inoculation of the eye resulted in secondary nerve injury. In contrast to the prior report, in this case, the patient reported wiping the spider from his leg with his hand at the time of envenomation. Identification of the spider as a black widow is limited by having to rely solely on the patient's subjective report. Precise localization of the lesion to a preganglionic versus postganglionic process is also limited by the lack of provocative testing such as cocaine or hydroxyamphetamine. However, it is plausible that direct toxic exposure to the eye from contact of spider body fluid could have resulted in a localized inflammatory response and subsequent asymmetric conjunctival irritation and periorbital edema, as documented in previous studies.17,18 It is also possible that after mechanical inoculation, in a method similar to tetanus and botulinum toxin, 19 central nerve injury may have resulted from retrograde axonal transport leading to the unilateral Horner's syndrome.
Conclusions
This unique case of Horner's syndrome after black widow spider envenomation highlights the importance of reviewing environmental exposures in the acute presentation of Horner's syndrome. In the case of ophthalmologic exposure, treatment should consist of liberal irrigation of the eye, analgesia, and protection to allow for rapid recovery. 18 Although the exact pathophysiologic mechanism of this disease has not yet been defined, this patient's symptoms stabilized and improved over a 5-week period after envenomation.
Footnotes
Acknowledgments
We would like to thank Dr Timothy J. Martin, Associate Professor of Surgical Sciences, Ophthalmology, and Neurology, for his contributions, specifically for providing the representative picture of a patient with Horner's syndrome.
