Abstract
Objective
(1) To determine if, after using the simulation mannequin SimMan in a wilderness “megacode” exercise, participants believe high-tech simulators are an effective tool for learning wilderness medicine skills. (2) To determine if participants believe high-tech simulation mannequins should be used with more or less frequency in future wilderness medicine exercises.
Methods
After completing a basic training session outlining the capabilities of SimMan and completing a wilderness megacode (defined as a series of progressive conditions that accumulate over time) using SimMan, participants were surveyed to ascertain whether they perceived SimMan to be an effective teaching tool for wilderness medical skills and to determine if they would like SimMan to be used with greater frequency at future wilderness medicine courses. The data were compiled and analyzed using Microsoft Excel.
Results
Participants found the wilderness SimMan experience to be an effective tool with an average score of 3.15 on a scale where 4 is most effective and 1 is least effective. Participants also desired to see high-tech simulation more frequently in wilderness courses with a score of 3, on a scale where 4 is more frequently and 1 is less frequently. There was little difference in responses based on previous experience with simulation.
Conclusions
High-tech simulation is an underused tool for wilderness medicine education. Currently, several barriers exist to its implementation in wilderness medicine. Participants in wilderness courses feel it is an effective tool and would like to see it used more frequently.
Keywords
Introduction
Health care simulation is an emerging branch of health care training that uses a spectrum of equipment that is designed to represent an aspect of clinical care. One end of this spectrum includes high-technology computer-controlled patient simulators. When compared with training with live human actors or low-technology simulators, high-fidelity simulation provides some unique advantages. Simulator training can be characterized as focused, measurable, standardized, and reproducible experiences. Simulators can be programmed to portray various physical exam findings that develop the context of a clinical scenario. High-technology simulators can be used to answer questions with preprogrammed phrases created by instructors and have realistic physical exam findings such as chest rise, lung sounds, palpable pulses, and detectable heart sounds. The airway can be controlled to create laryngospasm and airway edema making the simulator nearly impossible to intubate. The simulator also has numerous interchangeable modules to represent bullet wounds, impalement, and evisceration.
Just as in hospitals where patient simulators are used to present learners with uncommon yet important pathology, they can also be used to reconstruct wilderness situations. It can be extremely difficult to get practice in treating injuries in a true wilderness setting. In a hospital setting, it would be unethical to use improvisational medicine to treat patients in order to get this wilderness or limited resource practice. For example, if a patient required a surgical airway in an emergency department, the practitioner would use the best possible supplies and should not improvise with a pocket knife and CamelBak (Petaluma, CA) tubing. By using simulation in a wilderness setting, learners are confronted with challenging scenarios and are afforded the ability to actually perform many procedures, including cardiopulmonary resuscitation (CPR), needle decompression, and airway management (Figure 1). Although wilderness scenarios can be carried out in the classroom, having to deal with environmental issues such as weather and terrain adds fidelity to the situation.
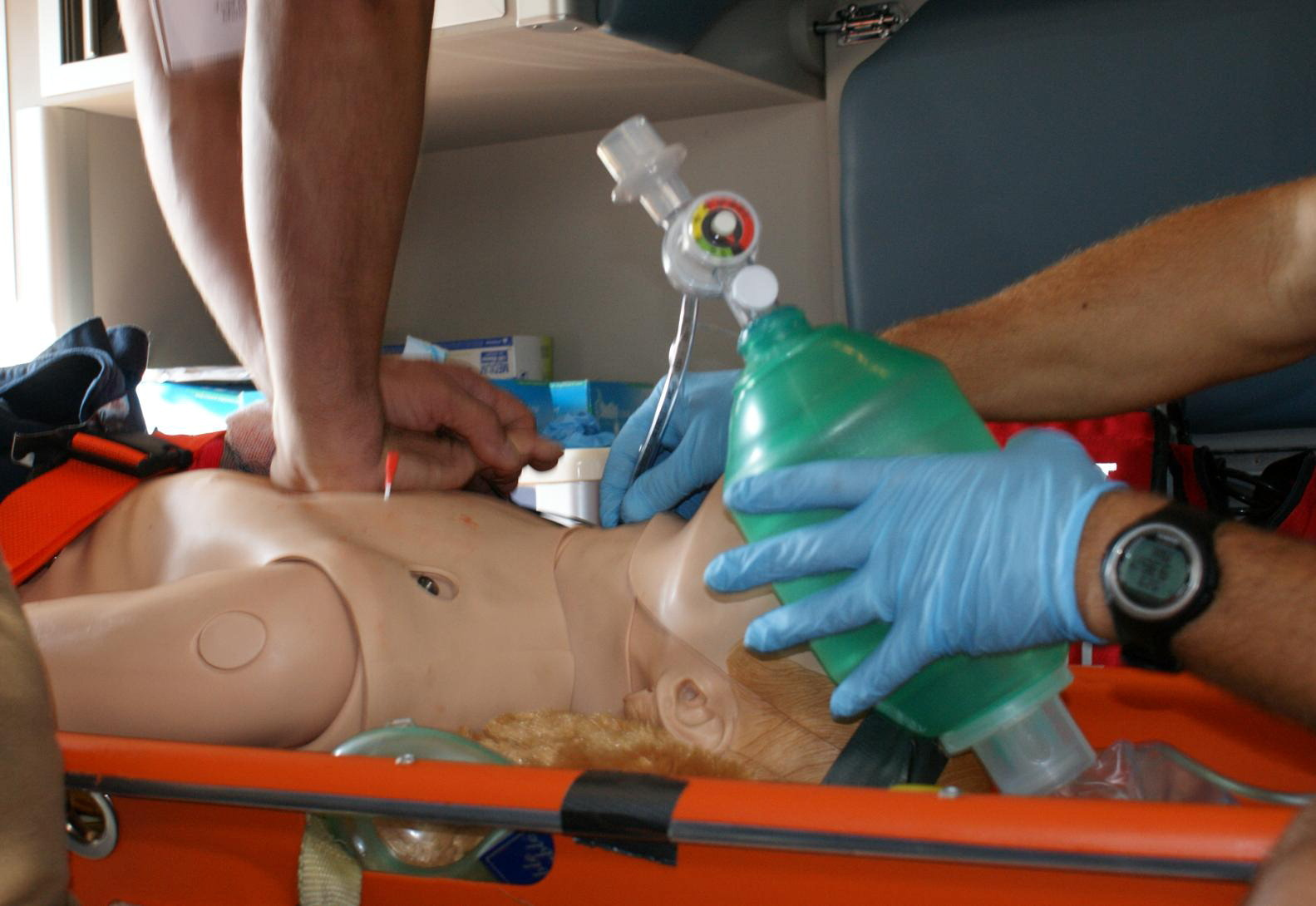
Simulator allows for practice of invasive procedures including cricothyroidotomy and needle decompression.
Materials and Methods
Students enrolled in a traditional Advanced Wilderness Life Support (AWLS; see
Participants were divided into four- or five-person groups, and each group played a role in providing appropriate care using skills taught earlier in the AWLS course. The megacode was designed so that as each group successfully completed a primary and secondary survey, the scene would become unsafe due to an array of environmental factors. In the scenarios, these environmental changes included a forest fire, an aggressive bear, and nearby gunfire. During each scene evacuation, the patient suffered an additional condition that would require the next set of practitioners to evaluate the patient before proceeding. This layering effect of conditions helped promote the megacode scenario offering.
The megacode was designed so that the last group would finally be able to transport the patient to a nearby all-terrain vehicle (ATV). Cardiopulmonary resuscitation was performed during travel on the ATV until the SimMan was finally delivered to a waiting ambulance (Figure 2). With all of the prior caregivers surrounding the ambulance, the final group of providers performed an advanced surgical airway and needle decompression to help stabilize the patient's airway and breathing functions (Figure 3). Because the patient was in need of immediate transportation to definitive care, the patient was transported to an awaiting air ambulance that had landed on the campus as part of the training scenario (Figure 4).

Patient care was continued during transport on an all-terrain vehicle provided by Western Piedmont Community College.
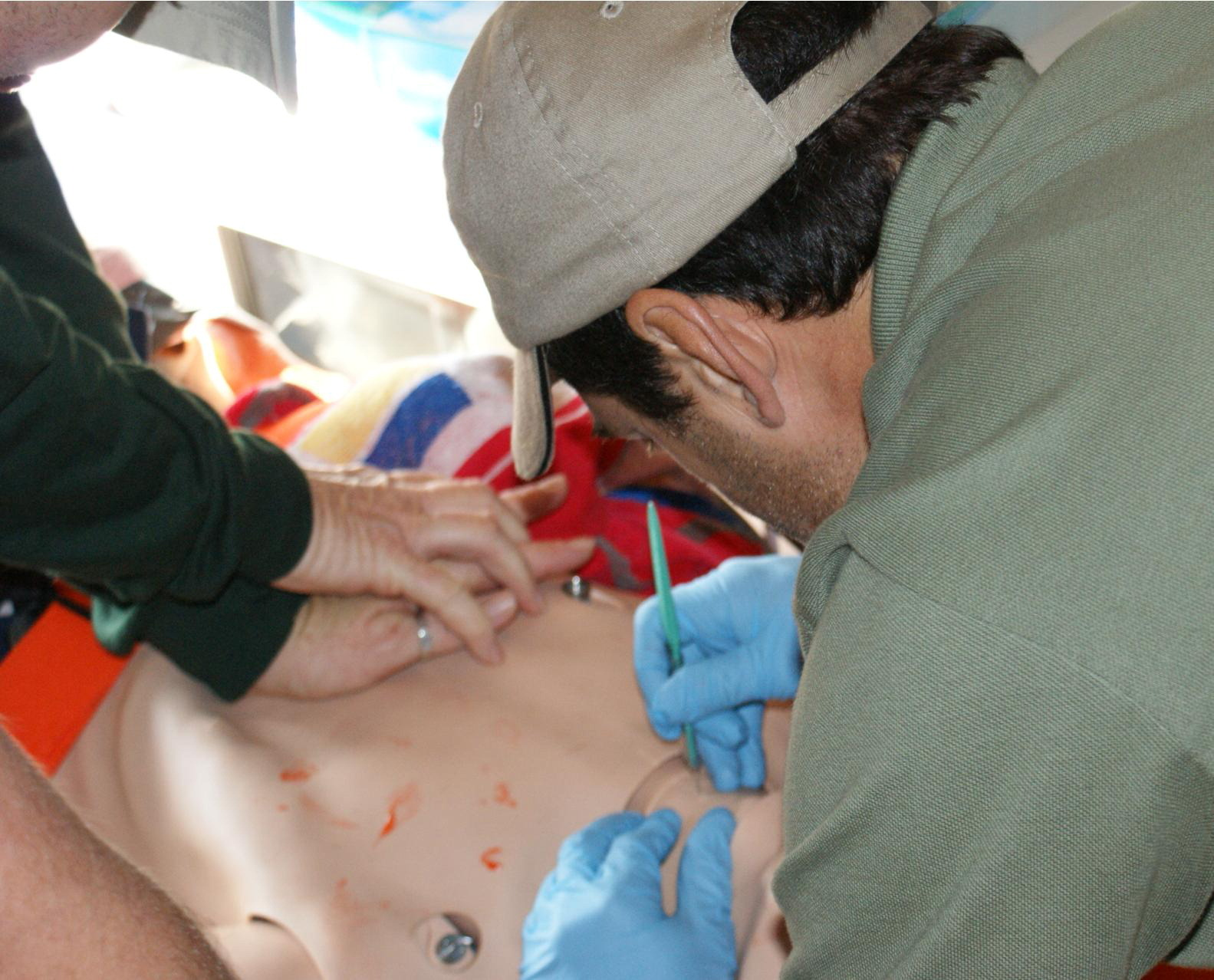
Participants preformed a surgical airway on the simulator.

The simulator was transferred to an air ambulance for transfer to definitive care allowing participants to learn about helicopter safety.
The scenario, which ran for approximately 75 minutes, was followed by a 15-minute group debriefing. This debriefing involved each learner group discussing their treatment decisions based on the patient scenario they encountered. Each group had the opportunity to self-reflect on the care they delivered as well as the care delivered by other groups given the condition of the patient.
After participants completed the course, each participant received an e-mail link to a survey requesting input regarding the various teaching modalities used during the AWLS course and perceived effectiveness. This survey was delivered to participants 5 days after the final day of the course. The survey accepted responses for 2 weeks. The data were compiled and analyzed using Microsoft Excel. The course evaluation forms that each student submitted at the end of the course were also reviewed, specifically with regard to the SimMan wilderness megacode experience.
Results
Twenty-eight participants responded to the survey. When asked how effective the SimMan was as a learning tool, participants ranked it as an average of 3.15 on a scale of 1 to 4, where 4 represented a most effective learning tool and 1 represented a least effective learning tool. Participants ranked their desire to see the SimMan tool used frequently in future AWLS content delivery as an average of 3, where 4 represented much more frequently and 1 much less frequently.
Twenty-four participants also evaluated the SimMan wilderness megacode experience using the course evaluation form, with an average rating of 4.58 on a scale of 1 to 5, with 5 representing excellent and 1 representing poor.
Discussion
High-technology simulation has been shown to be a popular teaching modality when used to help learners attain educational mastery of complex medical content. 1 The AWLS wilderness megacode was designed as a comprehensive scenario to help learner groups synthesize and test many of the skills learned during the prior 3 days of the course. The use of high-technology patient simulation allows the instructors to re-create relevant situations to practice a variety of AWLS skills that could otherwise not be realistically practiced. Based on survey results, the experience seemed to be an effective learning tool for students, and they wished to see it used more frequently in the future.
Several barriers exist to high-fidelity simulation in a wilderness environment. The simulator that was used in this course was the Laerdal SimMan with the portability kit. Equipment failure of the rechargeable battery made it necessary to use extension cords routed through the woods to a vehicle to provide power to SimMan. A hybrid emergency medical services (EMS) vehicle proved an ideal power source (Figure 5), as it could run silently aside from rare periods when the gasoline engine cycled on to briefly recharge the high-voltage battery. The utility of hybrid vehicles in wilderness EMS operations has been described elsewhere, 2 and this represents another novel use of hybrid technology in wilderness medicine. SimMan also must be tethered to a computer, which makes moving the simulator while running much more difficult, which in addition to disconnection from the power supply is why the patient in our megacode became apneic and unresponsive when moved. The requirement for tethering makes use of SimMan in extrication scenarios very difficult. It also limits the distance from usable roads that scenarios can take place. Some fidelity is lost when cords are noted to be running through the woods and an operator must be within feet of the simulator with a computer (Figure 6).

A hybrid vehicle was used to provide power to run the simulator.

Scenarios lose some fidelity when the operator is tethered to the simulator.
When used in a wilderness environment, the simulator was limited to preprogrammed phrases as SimMan does not currently have the wireless technology needed to create on-the-fly responses through an instructor. This limited some of the answers that could be given to learners. Attempts were made to pre-record answers to all anticipated questions, however SimMan was forced in many cases to use canned phrases such as ”I don't know” when more appropriate answers may have aided in progression of the scenario. The use of preprogrammed response is superior to the low-fidelity mannequins that cannot interact at all; however, it is more difficult than human actor scenarios where actors can respond appropriately.
SimMan does not currently have modules to accurately represent orthopedic injuries, which are common in wilderness situations. The open fracture module is unrealistic in that no manipulation or attempts at reduction are successful as the module is hard plastic. The body structure makes splinting less realistic as SimMan lacks joint mobility. There is no way to change extremities to create fractures. SimMan also does not have active bleeding modules, so any bleeding that occurs can only be from moulage placed on the mannequin prior to a scenario.
One of the other obstacles to overcome in the wilderness setting is creating scenarios in which multiple learners can partake. Attempts to overcome this obstacle were made by creating the megacode in which small groups could all participate in the care of a single patient with multiple medical conditions. The main problem encountered during the megacode was a lack of communication between groups, so incoming groups were unsure about the status of the patient. In the future, hopes are to employ wireless camera technology so learners who are not directly participating can observe what is occurring. The importance of hand-off communication about the patient between teams will be stressed with future students. Because of the cost and expertise required to run high-fidelity simulation, it is difficult to have multiple simultaneous scenarios.
It is also difficult to convince some SimMan owners to allow these expensive resources (each unit generally costs over $30 000) to be used in the outdoors. It was found that SimMan's skin could be cleaned effectively (but not necessarily decontaminated) by carefully using soapy water. Scenarios cannot be performed in rainy conditions because of the extensive electronics inside SimMan, which is not a waterproof closed system. However, as the use of simulation in medical education grows, simulators may become less expensive and more resistant to outdoor conditions.
As more and more health care providers are exposed to high-fidelity simulation, it will become easier for students to interface with the technology. Attempts were made to introduce all of the students to SimMan and his capabilities through a short introductory workshop prior to the wilderness megacode. In the megacode, students seemed more comfortable interfacing with the simulator than they were the previous day during the workshop. As many students were accustomed to low-fidelity simulation, they tended to ask the instructor questions about the patient, for example, ”Is he breathing?” Students would be redirected back to the patient asking them to assess for chest rise and breath sounds. As students gain more experience in using simulation, the redirection seems to be needed less frequently.
As the technology improves and high-fidelity simulation becomes more common, scenarios will become more realistic. One of the benefits to this technology is that it can allow medical providers in the field to interface with the EMS personnel so scenarios can allow for the continuity of care that is needed in true wilderness emergencies. With high-fidelity simulators, scenarios can be developed that create unique challenges for both first responders and trained medical professionals who will assume care after extrication.
Limitations of the study include the following: a small sample size; experiences with the simulator by the participants were not uniform; only one type of simulator was used; data reflect postencounter perception of efficacy. The assessment gathered was purely subjective, so further research is needed to determine if the use of SimMan in wilderness training produces a measurable improved performance.
Conclusion
High-technology simulation is a natural fit for wilderness medicine training because of the need for realistic patient simulation and the inability to practice improvised and resource-poor interventions on human subjects. This fit will become even tighter as the technology for simulation continues to evolve and tetherless simulators become available. Participants in high-tech wilderness medicine simulations feel that this mode of training is effective for wilderness medicine education and would like to see it used more frequently. We believe as the technology is strengthened and is more readily accessible, simulation will be a significant wilderness medicine training tool. The ”wilderness megacode” could become an avenue for training both wilderness first responders and EMS personnel as well as general health care students enrolled in optional wilderness medicine courses. Through the experience provided at the AWLS course, participants were able to follow patient care from the initial assessment as the first group located the victim, through transport on a litter through the woods to an ATV, and on an ATV to an awaiting training ambulance. Participants were then able to observe medical providers caring for the patient on a training ambulance and observe the extrication via medical helicopter. Simulators are ideal tools to provide longitudinal training for first responders, emergency medical crews, medical flight crews, and physicians. These tools will only continue to evolve to create more realistic and useful training scenarios.
Footnotes
AWLS megacode
Group 1: Scene safety (embankment with rocks and limbs) CA: Secure scene and move patient to safe area while maintaining C-Spine CA: ABC primary survey will be non-emergent CA: Reassess ABC after moving patient Trans: Team asked to go get additional help Group 2: Femur fracture recognized and treated CA: Scene safety CA: Prompt for ABC CA: Perform secondary survey CA: Recognize femur fracture and create traction splint Trans: Team forced to leave due to approaching forest fire Group 3: No environment changes to patient; forest fire came close to patient CA: Prompt for ABC CA: Scene safety CA: Continue secondary survey and treat burnt hand/forearm CA: Complete wash of arm and apply dressing Trans: Bear approaches Group 4: Bear approaches now isolated victim and mauls patient; patient sustains abdominal evisceration CA: Prompt for ABC CA: Scene safety CA: Primary survey is completed CA: Secondary survey; recognize bear has left and treat abdominal wound CA: Passive warming measures; move off ground or into shade; padding Trans: Hunters are shooting at the nearby bear; scene is unsafe Group 5: Patient has been struck by stray bullet; patient becomes less conscious and moans CA: Prompt for ABC CA: Scene safety CA: Primary survey reveals patient entering hemorrhagic shock CA: Looking for causes to stabilize circulation, team finds hemorrhage on back and apply pressure CA: Recognize bullet wound entry and exit and apply pressure to exit wound CA: Maintain C-spine and sweep the back of the spine for wound CA: Reassess after movement Trans: Team is told they have dropped the patient Group 6: Extrication team dropped patient who received head laceration CA: Prompt for ABC CA: Scene safety CA: Assess scene CA: ABC primary survey will be non-emergent CA: Secondary survey reveals head laceration and requires pressure dressing Trans: Extrication team member steps on beehive Group 7: Patient is attacked by bees and begins to show signs of anaphylaxis; patient remains less responsive CA: Prompt for ABC CA: Scene safety CA: Primary survey reveals upper airway constriction CA: Administer epi via Epi-pen Trans: Group asked to go retrieve Gator to help with extrication Group 8: Patient is stabilized and packaged for extrication CA: Scene safety CA: Prompt for ABC CA: Transport patient safely to ambulance CA: Begin CPR with patient moved to extrication vehicle Group 9: Patient is moved into back of ambulance and is in sinus PEA secondary to hypoxia CA: ABC reveals airway constriction; attempted definitive fails CA: Recognize need for and perform surgical airway CA: Recognize tension pneumothorax and perform needle decompression CA: Recognize sinus PEA/administer atropine/epi CA: Recognize in next rhythm check post 2 min CPR patient is in VF; defibrillate patient Final: Patient returns to NSR and vitals stabilize Group receives information about helicopter safety, LZ selection MedCenter Air lands and patient is loaded After helicopter is turned off, group tours helicopter ABC, airway, breathing, circulation; PEA, pulseless electrical activity; VF, ventricular fibrillation; NSR, normal sinus rhythm; LZ, landing zone; Epi, epinephrine.
You are hiking in the woods during hunting season and you find this guy lying on the ground under his tree stand. Patient is awake and responsive upon arrival. (CA indicates Critical Action.)
