Abstract
Chronic kidney disease defined and staged
It has recently been proposed that the term ‘renal failure’ be discarded in favor of ‘kidney disease’ for two reasons. First, pet owners know what a kidney is, but many are unfamiliar with the medical term ‘renal.’ Thus using the term ‘kidney’ facilitates communication between veterinarians and clients. Secondly, there has never been complete agreement on the specific meanings of renal insufficiency and renal failure. By using the term ‘kidney disease’ and staging the severity of disease, it is possible to greatly facilitate understanding, communication and application of management guidelines for patients.
Kidney disease is defined as the presence of functional or structural abnormalities in one or both kidneys. 1 It may be recognised by reduced kidney function or the presence of kidney damage. Kidney damage is defined as either: microscopic or macroscopic pathology detected by biopsy or direct visualization of the kidneys; or markers of damage detected by blood or urine tests or imaging studies.
The severity of kidney disease varies greatly depending on the magnitude of kidney involvement.
Patients with chronic kidney disease (CKD, as defined below) can be categorized into stages along a continuum of progressive disease. 3 The International Renal Interest Society (IRIS) has proposed a four-tier system for staging CKD in dogs and cats (see box, page 196). 4 The staging system was developed by a panel of experts in veterinary nephrology, rather than specific clinical studies, and its use has been advocated by the American and European Societies of Veterinary Nephrology and Urology. The stage is based on the level of kidney function signified by at least two sequential determinations of serum creatinine concentration obtained in a well hydrated patient fasted for 12–24 h. Ideally, serum creatinine concentrations should be determined at least twice over 1–2 weeks to stage CKD. As a variety of factors affect serum creatinine concentrations, published reference ranges are often exceedingly broad. Using the IRIS staging system, some patients classified as having mild renal azotemia (stage 2) may have serum creatinine values within published reference ranges. As a consequence, the patient's overall clinical status should be considered when interpreting serum creatinine concentration and other laboratory tests and when planning patient management. In particular, the serum creatinine concentration must be interpreted in the light of a concurrently obtained measure of urine concentrating ability (urine specific gravity or osmolality). In the absence of urinary obstruction, serum creatinine values > 1.6 mg/dl (140 μmol/l) are likely to indicate kidney disease when the patient's urine specific gravity is < 1.035. Daily production of creatinine in the body is determined largely by the muscle mass of the individual, so care must be taken in interpreting values obtained from animals with reduced muscle mass; for example, elderly cats with CKD and poor muscle mass may have lower than expected serum creatinine concentrations. 5
CKD is defined as kidney damage present for at least 3 months, with or without decreased glomerular filtration rate (GFR), or a > 50% reduction in GFR persisting for at least 3 months. 2
Stages of feline CKD
For full details of the staging system, see the International Renal Interest Society's website: Error! Hyperlink reference not valid.
P = proteinuria (protein:creatinine ratio [UPC] > 0,4), NP = non-proteinuria (UPC < 0.2), BP = borderline proteinuria (UPC 0.2–0.4]
N = minimal risk of complications, L = low risk of complications, M = moderate risk of complications, H = high risk of complications, nc = no complications, c = complications, RND = risk not determined (blood pressure not measured)
The IRIS has proposed to further subclassify patients with CKD according to their magnitude of proteinuria and systemic blood pressure. Proteinuria and hypertension appear to influence prognosis; however, the impact of therapeutic intervention to lessen proteinuria and hypertension on long-term prognosis is still uncertain.6–9 Classification of patients as proteinuric necessitates determining the urine protein:creatinine ratio (UPC) and eliminating the presence of hemorrhage, inflammation and/or infection. Feline patients are classified as proteinuric when their UPC > 0.4. Values for UPC between 0.2 and 0.4 are classified as borderline proteinuric, while UPC values < 0.2 are classified as non-proteinuric. Ideally, UPC values between 0.4 and 1.0 should be confirmed using several urine samples obtained over 2–4 weeks. With respect to blood pressure, the IRIS has proposed that patients be further staged according to the degree of risk of end-organ damage and whether there is current evidence of such damage or complications. 4
Goals and limits of therapy for CKD
Conservative medical management of CKD consists of supportive and symptomatic therapy designed to correct abnormalities in fluid, electrolyte, acid-base, endocrine and nutritional balance. Therapy aims to minimize the clinical and pathophysiological consequences of reduced kidney function. In general, this type of management should not be expected to halt, reverse or eliminate renal lesions responsible for CKD. Therefore, management strategies are most beneficial when combined with specific therapy directed at correcting the primary cause of the kidney disease such as hypercalcémic nephropathy, bacterial urinary tract infections and obstructive uropathy. Efforts should be directed at detecting and treating active primary kidney diseases in addition to managing the various pathophysiological and clinical consequences of CKD.
Medical management guidelines provided here are intended for pets with compensated disease; not for patients unable to eat or accept oral medications because of severe uremia. Clinical signs of uremia must be corrected before instituting the general principles of medical management. The goals of medical management of CKD are to:
ameliorate clinical signs of uremia;
minimize disturbances associated with excesses or losses of electrolytes, vitamins and minerals;
support adequate nutrition by supplying daily protein, calorie, mineral and other nutrient requirements; and
modify progression of kidney disease. 2
These goals are best achieved when recommendations are individualized to the patient's needs on the basis of clinical and laboratory findings. Because CKD is progressive and dynamic, serial assessment of the patient and modification of therapy in response to changes are essential parts of the management strategy.
Evidence-based veterinary nephrology concepts
Evidence-based medicine (EBM) represents a major, although largely untested, intellectual advance when making clinical decisions and determining patient care.10–12 EBM has been defined as the integration of the best research evidence with clinical expertise and patient values. 10 Best research evidence means clinically relevant research, especially from patient-centered clinical studies. Clinical expertise refers to the use of clinical skills to identify each patient's unique health status, establish a diagnosis, and determine the risks and benefits of potential interventions. For veterinary medicine, the concept of patient values must include the unique preferences and expectations of each owner. In addition, if a therapeutic intervention is not readily available, then it is unlikely to benefit the patient. The basic tenet of EBM is that integration of these elements (clinically relevant research, clinical expertise, patient/owner preferences, and availability of resources) will result in the formation of a diagnostic and therapeutic alliance that optimizes clinical outcomes and quality of life. 10
In the past, information based on pathophysiological rationale and data from models of kidney disease were often used to justify clinical recommendations in cats with CKD. The proliferation of randomized controlled clinical trials has led to an increase in the quantity and quality of clinically valid evidence. When possible, veterinarians should use information derived from systematically conducted, rigorously controlled clinical studies to make diagnostic and treatment decisions. Of course, not all recommendations can be based on such studies so it is important to recognize the inherent limitations of less rigorous forms of evidence. One method of accommodating concerns regarding these limitations is to assign a score defining the strength and quality of the recommendation. The classification scheme proposed for veterinary clinical nutrition 13 may be useful for establishing rules of evidence for recommendations regarding veterinary nephrology. These guidelines categorize the quality of evidence into grades I to IV based on applicability to clinical case management (see box below). Grades I and II are evidence with the highest quality for application in the clinical environment, whereas grade IV would be evidence with the lowest quality.
The quality and strength of evidence can be used to make a recommendation about use of a specific therapeutic modality. Although EBM does not always lead to a definitive answer, it does provide a framework for making decisions and understanding the risk-benefit relationship of various therapeutic or preventive plans.
Quality of evidence grading guidelines
Applying evidence-based concepts to therapeutic decisions for CKD
A grade I to IV scoring system 13 was used to systematically evaluate the quality of published evidence for the use of 13 categories of interventions in cats with CKD, as discussed below. The strength of evidence was also assessed in making a final recommendation for use of a specific treatment modality.
It is important to note that the use of any specific therapeutic strategy hinges not only on the quality and strength of evidence summarized here but also on the clinical expertise of the individual veterinarian, owner preferences and available resources. In addition, the impact of providing unnecessary or unproven treatments on the pet-owner relationship should be considered. Treatments that are undesirable to the pet or owner may be disruptive to that relationship. As providing high quality health care to pets is based on the pet-family bond, it is important to avoid inadvertently disrupting this relationship when recommending therapy.
Fluid therapy
Progression of CKD is accompanied by decreases in GFR, worsening azotemia and ultimately uremia. Long-term administration of subcutaneous balanced electrolyte solutions has been advocated in patients with CKD to prevent dehydration, thereby maximizing renal blood flow and GFR, increasing urine output and ameliorating clinical manifestations of dehydration and uremia.2,14,15 Subcutaneous administration of balanced electrolyte solutions is usually reserved for cats with advanced (stages 3–4) CKD prone to dehydration.
Preliminary studies have been completed in healthy adult cats using intravenous fluids and various diuretics. 16 In healthy cats, the renal effects of mannitol were superior to those of furosemide and dopamine together when used as an adjunct to fluid diuretic therapy. 16 Additional studies with fluid therapy are required to assess physiological and clinical parameters in animals with CKD. Use of diuretics should be limited to patients with uremic crises rather than cats with stable CKD. Anecdotal reports suggest that many cat owners can give subcutaneous fluids successfully in the home environment for a long period of time. Hypertension is a well-recognized complication of CKD in cats and it is unknown if excessive sodium chloride delivered by parenteral fluids will exacerbate clinical problems associated with hypertension or kidney disease. For example, every 100 ml of lactated Ringer's solution provides 13 mEq sodium, which is approximately eight times the 24 h maintenance requirement for sodium in healthy or diseased cats.17,18 Although empirical evidence suggests that some individual cats may benefit from long-term subcutaneous fluid therapy, no controlled clinical studies exist to determine whether such therapy prolongs survival and improves quality of life in cats with CKD.
FLUID THERAPY
Summary of the evidence
Calcitriol therapy
The kidneys are responsible for converting 25-hydroxycholecalciferol to its most active metabolite, 1,25-dihydroxycholecalciferol, also known as calcitriol. Calcitriol is one of the major hormones responsible for calcium metabolism along with parathyroid hormone (PTH). Among calcitriol's important functions is modulation of PTH activity at the transcriptional level. 19 As production of 1,25-dihydroxycholecalciferol is typically impaired in CKD, calcitriol deficiency may be one factor promoting renal secondary hyperparathyroidism. Parathyroid hormone has been proposed to act as a ‘uremic toxin’ and supplementing calcitriol may ameliorate a variety of supposed adverse effects of excess parathyroid hormone in patients with CKD. A study found that 8/26 cats with CKD had renal secondary hyperparathyroidism as detected by elevated serum PTH concentrations. 20
Use of calcitriol in patients with CKD is described in numerous textbooks and reviews.21–23 Investigators have reported that in cats with CKD receiving calcitriol therapy, patients: (1) were brighter and more alert, (2) had improved appetites, (3) were more physically active, and (4) lived longer. 21 These findings were based on an uncontrolled survey of veterinarians who used calcitriol in their practice. A study of 10 cats with CKD showed that serum PTH concentrations were not significantly different after 14 days of calcitriol administration, regardless of whether calcitriol was administered daily or intermittently. 24 Adverse effects of calcitriol administration (specifically ionized hypercalcemia) were not observed in this short-term study.
However, many of the beneficial effects of calcitrioi therapy in patients with CKD may be mediated through activation of vitamin D receptors on many tissues rather than modulation of PTH activity alone. 25 A 1-year randomized controlled clinical trial examined the effect of low-dose calcitrioi therapy on progression of CKD and clinical signs in cats. 26 In this study, calcitrioi was ineffective in altering renal mortality or improving appetite, activity or quality of life in cats with stages 2–4 CKD. In contrast, a 1-year randomized controlled clinical trial examining the effect of low-dose calcitrioi therapy on progression of CKD and clinical signs in dogs demonstrated that calcitrioi therapy was associated with a significant reduction in all-cause mortality compared with placebo. 2
CALCITRIOL THERAPY
Summary of the evidence
Antihypertensive therapy
Hypertension is a well recognized complication of CKD in cats. Mild to moderate systemic hypertension was originally reported in 17/28 cats that had spontaneous CKD. 27 More recent data suggest that the prevalence of hypertension in cats with CKD may be about 20%. 28
Sustained systemic hypertension can result in hypertensive retinopathy with retinal detachment, hemorrhage and blindness (Fig 1). Cats with such severe ocular manifestations probably reflect only a small percentage of pets with CKD and hypertension. More subtle ocular lesions such as retinal edema, retinal vessel tortuosity and subtle retinal hemorrhages may be much more common. Hypertension-related central nervous system disorders (eg, seizures, loss of balance, abrupt changes in personality, obtundation, etc) have also been observed.29–31 Management of hypertension reportedly limits postoperative neurological disorders following renal transplantation in cats. 32

Retinal Image from a 10-year-old spayed female domestic shorthair cat with acute blindness. Chronic kidney disease and hypertension were diagnosed
Hypertension may also damage other organs including the kidneys, heart and blood vessels. A small study in cats with CKD suggested that glomerulosclerosis is more severe in hypertensive cats compared with normo-tensive cats. 33
Initiation of therapy for hypertension has been advocated for cats with clinical signs consistent with pressure-related end-organ damage (eg, hypertensive retinopathy with retinal detachment, acute-onset neurologic signs) and/or blood pressure values that persistently exceed 180/120 mmHg.4,34 However, the touted renoprotective benefit of antihypertensive therapy in cats is largely extrapolated from observations in humans and experimental studies in animals. The potential benefits of intervention in patients without clinical signs might include retarding progression of kidney disease, prolonging survival and reducing the incidence of hypertensive retinopathy and encephalopathy In one study, proteinuria was the only variable significantly related to survival in hypertensive cats. 8
Although specific evidence-based guidelines for treatment of systemic hypertension have not been definitively established for cats, studies have provided information on the effectiveness of some antihypertensive treatments. Currently, the calcium channel antagonist amlodipine besylate appears to be the drug of choice for managing hypertension in cats with CKD. Antihypertensive effects have been noted in uncontrolled clinical observations on the use of amlodipine in cats with spontaneous kidney disease.8,31,35,36 Blood pressure control with amlodipine appears to influence survival in hypertensive cats in a positive manner and lower blood pressures at the time of diagnosis indicate that treatment is more likely to be effective. 8 Treatment with amlodipine can result in a significant reduction in proteinuria and, as mentioned, the level of proteinuria appears to be related to survival in hypertensive cats. 8 Another study showed that amlodipine administration decreased systemic arterial blood pressure and dramatically reduced the prevalence of ocular lesions attributable to hypertension in cats with an induced model of renal failure. 37 In this last study, all cats were also fed a therapeutic renal food throughout the study period.
In contrast to amlodipine, angiotensin converting enzyme (ACE) inhibitors and 3-blocking agents do not appear to be effective as sole agents for long-term management of systemic hypertension in cats.38,39 However, one study showed that the ACE inhibitor benazepril is well tolerated when administered with amlodipine to hypertensive cats and may assist in managing cats with poorly controlled blood pressure. 40 Amlodipine also appears to have intrinsic antioxidant activity. 41 It is currently unknown whether this in vitro antioxidant activity results in significant improvement in endothelial function in patients with CKD or provides substantive clinical benefits.
ANTIHYPERTENSIVE THERAPY
Summary of the evidence
ACE inhibitor therapy
Systemic and renal changes that are observed in patients with kidney disease may contribute to the progression of renal injury (Figs 2 and 3). Frequently implicated changes include increased systemic arterial pressure (systemic hypertension), increased intraglomerular pressure (glomerular hypertension), glomerular enlargement (glomerular hypertrophy) and altered glomerular perm-selectivity. Evidence suggests that therapy with ACE inhibitors preserves glomerular structure and function in patients with kidney disease. Administration of ACE inhibitors to rodents with reduced renal mass revealed that renoprotection is associated with lowering of glomerular capillary pressure, blood pressure and glomerular size.42,43 Systematic reviews and meta-analysis of clinical studies of ACE inhibitor use in human patients have revealed beneficial effects in terms of slowing progression of non-diabetic kidney disease.44,45 This beneficial effect seems to be mediated by factors in addition to decreasing blood pressure and urinary protein excretion and is greater in patients with proteinuria.44,46
The ACE inhibitor benazepril has been licensed in several countries for use in managing cats with CKD. 47 Two studies examined the physiological effects of benazepril in cats with induced kidney disease. Systemic arterial and glomerular capillary pressures were shown to be reduced and GFR was increased by such therapy.48,49 However, the reduction in systemic blood pressure was small and a beneficial effect in reducing proteinuria was not evident. These initial studies failed to detect any evidence that administering benazapril resulted in long-term structural or functional renal protection. 50
Data have recently been reported from randomized controlled clinical trials of benazepril use in cats with spontaneous CKD.49,51–54 In two controlled studies, benazepril reduced proteinuria in cats with spontaneous CKD; however, it did not significantly prolong survival time.51,54 Cats with a UPC > 1.0 had mean (± standard deviation) survival times of 402 ± 202 days with benazepril (n = 4) compared with 149 ± 90 days with placebo (n = 9); however, this difference was not statistically significant. 51 Cats with initial UPC > 1.0 treated with benazepril had a significantly better appetite compared with cats treated with placebo. 51 While administration of ACE inhibitors lessens proteinuria in cats with CKD and proteinuria is a prognostic indicator for cats with CKD, it has yet to be established whether reduction of proteinuria with use of ACE inhibitors improves the long-term prognosis in cats with CKD. 50
In a separate study, treatment with enalapril and benazepril did not change plasma renin activity, aldosterone concentration and indirect systolic arterial blood pressure in cats with hypertension associated with CKD. 39 However, another study showed that benazepril is well tolerated when administered with amlodipine in hypertensive cats and may assist in managing cats with poorly controlled blood pressure. 40

Lateral (a) and ventrodorsal (b) abdominal radiographs of a cat with chronic kidney disease and bilateral renomegaly. Lymphoma, polycystic kidney disease and feline infectious peritonitis were considered as potential causes. Diagnostic evaluation confirmed the presence of lymphoma

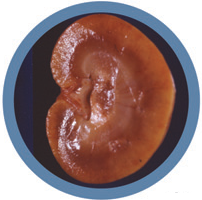
Kidneys from a cat that died as a result of acute progression of chronic kidney disease. Necropsy confirmed the presence of renal hypoplasia (small kidney) and renal hypertrophy (larger kidney)
ACE INHIBITOR THERAPY
Summary of the evidence
Erythropoietic hormone replacement therapy
Low packed cell volume (PCV), erythrocyte count and hemoglobin are characteristic of cats with moderate to advanced CKD.2,55 The anemia is normocytic, normochromic, hypoproliferative and proportional to the severity of the kidney disease. The principal cause is hypoplasia of erythroid elements of the bone marrow secondary to inadequate production of erythropoietin by the kidneys. Shortened erythrocyte life span, erythropoietic inhibitor substances in plasma, chronic gastrointestinal blood loss, nutritional abnormalities (eg, iron deficiency) and bone marrow fibrosis may further exacerbate anemia in some patients with CKD. Recent studies in humans indicate that hypoxia from anemia of kidney disease may contribute to progression of CKD because the anemia reduces oxygen delivery within the kidney, further promoting hypoxia and progressive renal damage from oxidative stress. 56
Hormone replacement therapy using human recombinant erythropoietin (rHuEPO) has been shown to be effective in correcting anemia of CKD in cats. Uncontrolled clinical trials indicated a substantial improvement in appetite and quality of life associated with this treatment. 57 Unfortunately, development of antibodies directed against rHuEPO has limited the effectiveness of this therapy in a substantial number of patients. As a consequence, it is best to select carefully those cases most likely to benefit from rHuEPO treatment. Generally, hematocrit or PCV guidelines can be used to judge the severity of anemia; symptomatic cats with PCV < 20% are the best candidates. 55 In addition, the degree of azotemia, expected rate of progression of CKD, appetite and willingness to eat therapeutic renal foods, and rate of progression of anemia must all be considered in the risk-benefit analysis of when to start therapy. 2 Gastrointestinal blood losses may contribute to anemia in patients with CKD and should be investigated before making the decision to use rHuEPO therapy.
Darbepoietin-α is a longer acting form of rHuEPO that has been used in a limited number of cats with anemia of CKD. Compared with regular rHuEPO, darbepoietin has a longer half-life and greater potency enabling the same clinical efficacy with less frequent administration. 58 Although its use has not been supported by clinical studies in cats with CKD, anecdotal reports indicate that darbepoietin is similar in efficacy and safety to erythropoietin, with the possible benefit of a reduction in the incidence of neutralizing antibodies.
The efficacy and safety of recombinant feline eyrthropoietin therapy was recently evaluated in cats with anemia of CKD and those with CKD and red cell aplasia induced by rHuEPO therapy. Most cats demonstrated erythroid hyperplasia, reticulocytosis, increased hematocrit and improved quality of life (appetite and energy level) with treatment. Unexpectedly, some cats that initially responded to feline recombinant eyrthropoietin therapy subsequently developed anemia that was refractory to additional treatments. 59 Unfortunately, the recombinant feline erythropoietin used in this study is not currently available as a commercial product.
The effect of renal transplantation on erythropoiesis and serum erythropoietin concentrations in cats with CKD has been evaluated. 60 Although the erythropoietic response was highly variable in cats after renal transplantation, anemia resolved in most cats within 2 months after surgery, suggesting that hormone replacement therapy is not needed in this subset of cats.
ERYTHROPOIETIC HORMONE REPLACEMENT THERAPY
Summary of the evidence
Potassium supplementation
An association between polyuric renal failure and hypokalemia has been recognized in cats by several investigators.61–63 Hypokalemia occurred in 19% of cases in a clinical series of cats with spontaneous kidney disease and was moderate to severe in more than half of these patients. 64
There is limited evidence that hypokalemia may be a cause of and contributing factor to CKD in cats, rather than simply a consequence of the disease. In an uncontrolled study, evidence of renal lesions and dysfunction developed in 3/9 cats fed a potassium-restricted, acidifying food for several months. 65 However, it was not clear whether potassium depletion or hypokalemia preceded the onset of kidney disease. In another study, 4/7 cats with induced CKD fed a food containing 0.3% potassium (dry matter basis) developed hypokalemia but four cats with normal renal function fed the same food did not develop hypokalemia. 66 Muscle potassium content has been shown to be decreased in normokalemic cats with spontaneous CKD, indicating that a total body deficit of potassium may develop well before the onset of hypokalemia. 67 The latter findings support the concept that reduced renal function precedes the development of hypokalemia.
In many cats with CKD and hypokalemia, renal function may improve after potassium supplementation and restoration of normokalemia, suggesting that hypokalemia may be associated with a reversible, functional decline in GFR. Renal function was shown to be adversely affected in normal cats when an acidified, low-potassium food was fed. 68 In that study, potassium depletion and acidosis appeared to have additive effects in impairing renal function. Routine supplementation with low oral doses of potassium has been recommended for all cats with CKD. 62 This recommendation appears to be based on the hypothesis that, in some cats with CKD, hypokalemia and potassium depletion might promote a self-perpetuating cycle of declining renal function, metabolic acidosis and continuing potassium losses. It is proposed that potassium supplementation may stabilize renal function before potassium depletion exacerbates the disease.
The potential benefit of potassium supplementation has been examined; however, the clinical benefits of such therapy remain to be proven.67,69 Although the value of providing supplemental potassium to cats with CKD and normokalemia has not been established, it is clear that muscle potassium and probably total body potassium stores may be reduced in at least some cats with CKD, presumably putting them at risk of hypokalemia. Feeding acidified foods or dietary acidiflers to cats with CKD may exacerbate their tendency to develop potassium depletion. 70 However, unpublished studies in cats with induced CKD failed to confirm an adverse effect of mild to moderate metabolic acidosis on hypokalemia or renal lesions. 71 There also appears to be an inverse relationship between serum potassium concentrations and blood pressure in cats. 72
POTASSIUM SUPPLEMENTATION
Summary of the evidence
The kidney accounts for 10% of the whole body oxygen consumption and is a site of significant aerobic metabolism that produces reactive oxygen species as by-products. 73 Increased free radical production and antioxidant depletion have been reported in human patients with CKD. 74 Increased free radicals appear to cause renal injury and increased oxidative stress may contribute to the progression of CKD.75–77
In a study, cats with spontaneous CKD were fed a dry food supplemented with the anti-oxidants vitamins E and C, and 3-carotene for 4 weeks. When compared with healthy cats, cats with stage 2 CKD had a tendency to develop oxidative stress. 78 The antioxidant supplements significantly reduced DNA damage in cats with CKD as evidenced by reduced serum 8-hydroxy-2′-deoxyguanosine (8-OHdG) concentrations, and comet assay parameters of DNA damage. Serum 8-OHdG concentrations generally reflect oxidation of DNA and comet assay shows the breakdown of DNA structure in the cells measured.
Cats with early spontaneous CKD show a tendency towards enhanced oxidative stress, which may worsen as CKD progresses. Dietary supplementation with antioxidant nutrients such as vitamin E, vitamin C and á-carotene significantly reduced oxidative damage to DNA in cats with spontaneous CKD. Based on limited evidence, cats with CKD might benefit from antioxidant fortification of therapeutic renal foods. Randomized controlled clinical studies are needed to confirm the potential benefits of dietary antioxidant supplementation on progression of CKD and important clinical outcomes (survival, quality of life).
Alkalinization therapy
Metabolic acidosis appears to be a common complication of CKD in cats,61,64 and alkalinization therapy designed to correct metabolic acidosis may be an important part of the overall management of such patients. A cross-sectional study involving 59 cats with CKD showed that over half of patients with severe disease had acidemia and low plasma bicarbonate concentrations.79,80 These data also suggested that biochemical evidence of severe metabolic acidosis does not generally occur in cats until late in the course of CKD. 79 As discussed earlier, there is also a putative relationship between hypokalemia, potassium depletion, chronic metabolic acidosis and CKD in cats. 81
Alkalinization therapy has been recommended for patients with moderate to severe metabolic acidosis associated with CKD based on pathophysiological justification and extrapolation from findings in other species. Potential benefits of alkalinization therapy in patients with CKD include:
improving clinical signs that may be caused by uremic acidosis;
preventing the catabolic effects of metabolic acidosis on protein metabolism, thereby promoting adaptation to dietary protein restriction;
limiting skeletal changes resulting from bone buffering; and
Chronic metabolic acidosis appears to impose an unnecessary metabolic risk that can easily be corrected by administration of potassium citrate or sodium bicarbonate when acidosis is appropriately confirmed.
In an investigation of cats with induced CKD, an acidifying (AD) or non-acidifying (NAD) diet was fed for 39 weeks. 71 Hyperchloremic metabolic acidosis developed in the AD group (mean venous pH = 7.27, compared with 7.33 in the NAD group); the net acid excretions in this group were six-fold higher than in the NAD group. Cats with induced-CKD fed the AD for 6 months did not develop progressive glomerular dysfunction or renal tubulointerstitial injury when compared with cats fed a NAD. This suggests that levels of dietary acidification typically used in manufactured adult maintenance foods may not promote progression of feline CKD. A double-masked placebo-controlled cross-over study examined the effect of supplementing the diet with potassium gluconate (2 mEq twice daily) for 12 weeks.69,83 This regimen had no effect on venous blood pH or bicarbonate ion concentrations although it did result in an increase in urine pH. No other controlled clinical trials have been performed to confirm that appropriate alkalinization therapy will significantly alter the progression of disease or clinical signs in cats with spontaneous CKD. Most therapeutic renal foods used in the management of CKD have increased dietary buffering capacity and are already less acidifying than many standard feline maintenance foods.
ALKALINIZATION THERAPY
Summary of the evidence
Dietary phosphorus restriction and intestinal phosphate binders
Phosphorus is retained in CKD, eventually resulting in hyperphosphatemia, which in turn promotes renal secondary hyperparathyroidism. The role of dietary phosphorus intake and hyperphosphatemia in pets with spontaneous CKD was first discussed nearly 30 years ago.84,85 Today, there appears to be a consensus of opinion that phosphate retention is a major cause of progression of CKD in many species. 9 In human beings with CKD receiving hemodialysis therapy, the adjusted relative risk of mortality was stable in patients with serum phosphate concentrations below 6.5 mg/dl, but increased significantly above this level. 86 Similar data for mortality risk associated with hyperphosphatemia in cats with spontaneous CKD are lacking. Nonetheless, treatment targets for serum phosphorus concentrations have been established for cats with CKD: serum phosphorus concentration is recommended to be maintained below 4.5 mg/dl (1.45 mmol/1), 5.0 mg/dl (1.6 mmol/1) and 6.0 mg/dl (1.9 mmol/1) in cats with stages 2, 3 and 4 CKD, respectively. 9
Hyperphosphatemia appears to be a reliable clinical indicator of hyperparathyroidism in cats with CKD.87,88 Hyperphosphatemia is detected in approximately 60% of cats with CKD, with the prevalence increasing as renal function declines. In a study of cats with advanced CKD, the prevalence of renal secondary hyperparathyroidism was reported to be 84%. 88 In this study, 87% of cats with clinical signs and 47% of clinically normal cats with only biochemical evidence of CKD were diagnosed with renal secondary hyperparathyroidism. Hyperparathyroidism was even detected in nine cats with CKD having normal serum calcium and phosphorus concentrations.
In a model of induced kidney disease in cats, high dietary phosphorus intake (1.56% dry matter) for up to 11 months was associated with renal mineralization, fibrosis and mononuclear cell infiltration. 89 Low levels of phosphorus intake (0.42% dry matter) were not associated with these histological abnormalities. Progressive renal dysfunction was not detected in either group during the timeframe of the study. In at least some cats with spontaneous CKD, dietary management with low-phosphorus feline renal foods alone may normalize hyperparathyroidism. 88
Intestinal phosphate binding agents may be useful in further reducing phosphate retention and hyperparathyroidism in cats with CKD when nutritional management alone (therapeutic renal foods) is insufficient in achieving serum phosphorus concentration targets. However, experimental or controlled clinical studies establishing the effectiveness of adding intestinal phosphate binding agents to dietary phosphate restriction in cats with CKD are limited. Clinical reports and anecdotal evidence suggest that Intestinal phosphate-binding agents are useful in reducing serum phosphate concentrations, especially in uremic, hyperphosphatemic animals.9,22 Lanthanum carbonate octahydrate has recently been developed as an intestinal phosphate binding agent and studied in azotemic, nor-mophosphatemic cats with a model of CKD.90 Addition of this agent to a moist high-phosphorus (2.2% phosphorus, dry matter basis) feline maintenance food fed to cats with induced CKD resulted in reduced phosphorus digestibility and increased phosphorus excretion. 90 Controlled clinical studies of this and other phosphate binders to confirm effectiveness in slowing progression of spontaneous CKD in cats have not been reported.
Intestinal phosphate binders are not well tolerated by some cats and may impair food intake. These agents must be given with every meal to be effective, which may decrease owner acceptance and usefulness of this therapy.
DIETARY PHOSPHORUS RESTRICTION AND INTESTINAL PHOSPHATE BINDERS
Summary of the evidence
Therapeutic renal foods
Therapeutic foods have been used for over 50 years in veterinary patients with CKD. Compared with typical commercial and homemade pet foods, therapeutic renal foods usually have reduced protein, phosphorus and sodium, and increased dietary buffering capacity, soluble fiber, B-complex vitamins, antioxidants, potassium and omega-3 fatty acids. 81 Veterinarians are often confronted with the decision of whether to recommend switching to a therapeutic renal food or to continue the current diet with the view that eating any food is better than risking reduced food intake by attempting a potentially unwanted dietary change. This clinical challenge underlines the importance of assessing the quality and strength of evidence underlying the use of therapeutic renal foods.
Several published clinical trials have provided evidence in support of feeding therapeutic renal foods when managing cats with stages 2-A CKD. A retrospective study compared the survival times of cats newly diagnosed with CKD that had been fed a normal diet or one of seven different types of therapeutic feline renal foods. 91 In this study, the median survival time of 175 cats with CKD that received conventional foods was 7 months, whereas the median survival time of 146 cats with CKD fed one of the therapeutic renal foods was 16 months. 91 A prospective study comparing feeding a renal food with not making a dietary change, showed a striking enhancement of survival time associated with feeding the renal food. 92 The control group in this study was composed of cats that refused to eat the renal food and continued their usual diet. A principal limitation of this study is that cats electing not to consume the renal food may have had an intrinsically worse prognosis unrelated to the food consumed. However, the magnitude of the difference in outcome (median survival time was increased nearly 2.5 times when the renal food was fed) suggests that the clinical benefit of feeding the renal food was likely to be real.
The effectiveness of a therapeutic renal food in cats with stages 2 and 3 CKD was evaluated by a randomized controlled clinical trial. 93 This study examined whether clinically important benefits accrued when cats with CKD consumed a renal food compared with a standard feline maintenance food. Other than being randomly assigned to either the renal food or the maintenance food, cats were managed in an identical manner with respect to other treatment interventions. Cats fed the maintenance food had a significantly greater number of uremic episodes (26%) compared with cats fed the renal food (0%). In addition, a significant reduction in renal-related mortality was observed in cats fed the renal food (0% versus 22%). Importantly, significant adverse effects of feeding the renal food were not detected in the study and cats fed the renal food maintained body weight and body condition during the 2-year study period.
Seemingly, the greatest problem with advocating renal foods for cats with CKD has been acceptance of the food. In most instances this can be overcome by carefully correcting metabolic complications of CKD and gradually introducing the renal food over several weeks (see box, page 206). In a recent clinical trial, most cats with CKD (90%) readily accepted and continued eating a renal therapeutic food using a gradual transition period and were no more likely to refuse the renal therapeutic food than a more typical adult maintenance food. 93
THERAPEUTIC RENAL FOODS
Summary of the evidence
Assisted feeding
Malnutrition is usually detected as weight loss, declining serum albumin or total plasma protein concentrations, anemia and evidence of decreased muscle mass. In patients with CKD, malnutrition usually results from inadequate food intake. Commercially available foods designed for patients with CKD contain sufficient protein, calories and other nutrients to sustain adequate nutrient intake when consumed in appropriate quantities. Some cats with stages 3 and 4 CKD fail to eat sufficient food voluntarily, regardless of palatability or nutrient content. 94
When malnutrition is evident or suspected, clinical recommendations often include a stepwise approach designed to facilitate adequate food intake.2,95 The first step is to ensure that metabolic and other medical causes of decreased appetite have been corrected including dehydration, gastrointestinal hemorrhage, metabolic acidosis, hypokalemia, anemia, urinary tract infection and drug-associated anorexia. When metabolic and other medical causes of anorexia have been excluded or corrected, therapy for uremic gastioenteritis should be initiated. A study has shown that hypergastrinemia is common in cats with naturally developing CKD and may contribute to gastric hyperacidity, uremic gastritis, gastrointestinal tract bleeding and associated clinical signs of anorexia and/or vomiting. 96 Therapy for gastrointestinal complications of uremia usually includes administration of an H2 antagonist such as famotidine, which may be combined with an anti-emetic and a gastric mucosal protectant such as sucralfate. 97
If therapy for uremic gastroenteritis fails to restore normal appetite, assisted feeding should be considered. Long-term use of esophagostomy or percutaneous gastrostomy tubes has been successful for delivering food, extra water and medications to patients with CKD. Anecdotal reports suggest that tube feeding can reverse the progressive weight loss associated with CKD and patients can have extended periods of improved quality of life.2,55,95
ASSISTED FEEDING
Summary of the evidence
10 tips to encourage acceptance of therapeutic ranal foods
Dialysis
In human medicine, hemodialysis is the most common means of providing replacement or supplemental renal excretory function. Hemodialysis has been used successfully to manage clinical signs of uremia in cats,94,98–100 Although hemodialysis is primarily indicated for managing cats with potentially reversible acute renal failure, there may be patients with CKD for which hemodialysis should be considered as a suitable adjunct to other forms of therapy, specifically in preparing cats for possible renal transplantation. Hemodialysis is most likely to be beneficial when serum urea nitrogen concentrations exceed 90 mg/dl (32 mmol/l urea) and serum creatinine concentrations exceed 8 mg/dl (700 μmol/l).98,99
Recent investigations have focused on recruiting the gastrointestinal tract as a means of excreting wastes normally eliminated by the kidney; in essence, enteric dialysis. Polymers designed for oral administration adsorb uremic toxins and excess fluid in the gastrointestinal tract for excretion in the feces. 94 These polymers have therapeutic potential as another extra-renal clearance mechanism to be used in conjunction with hemodialysis or other forms of therapy in patients with CKD. Further controlled clinical studies with oral polymer therapy are anticipated. In addition, a probiotic product purported to enhance gastrointestinal excretion of nitrogenous waste products has recently entered the veterinary market. The manufacturer proposes that enhanced intestinal clearance of these nitrogenous wastes will ameliorate clinical signs of uremia.
Renal transplantation
Renal allograft transplantation has become a viable therapeutic option for cats with CKD. Long-term immunosuppression with a combination of oral corticosteroids and ciclosporin has proven successful in cats, although regular monitoring is required.101,102 However, severe and often fatal complications of renal transplantation may occur in cats.32,103–108
Recommended criteria for selection of feline transplant recipients include:
early decompensated CKD for which conventional therapy is no longer effective;
weight loss of no greater than 20% of healthy body weight;
no history of recent urinary tract infection;
no concurrent serious medical conditions (eg, inflammatory bowel disease);
no evidence of cardiac dysfunction;
negative tests for chronic systemic viral infections. 109
Other criteria to evaluate when considering renal transplantation include the emotional and financial commitment by the owner to immediate and long-term care of the animal, as well as access to a veterinarian familiar with managing transplant recipients should complications arise.
Summary of evidence grades supporting recommendations for therapy of feline CKD

DIALYSIS
Summary of the evidence
RENAL TRANSPLANTATION
Summary of the evidence
KEY POINTS
