Abstract
Purpose
The purpose of this study was to evaluate the outcome of flexible intramedullary nailing for unicameral bone cysts in terms of function and osseous consolidation.
Methods
Twenty-two unicameral bone cysts in children's long bones were treated by flexible intramedullary nailing. In 13 cases the bone cyst was diagnosed in a traumatic event leading to a pathologic fracture. Fifteen patients were referred to our clinic after failed conservative treatment. In 16 patients the cyst was located in the humerus, and in 6 patients in the femur. Mean duration of follow-up after surgery was 24 months.
Results
According to Capanna's criteria healing was obtained in 20 cases with a mean time of 16 months. Sixteen cysts healed completely. Four lesions were classified as grade 2, meaning that residual radiolucencies were radiographically visible at the latest follow-up. Two recurrences of humeral cysts were seen at 16 and 18 months postoperatively. The complication rate was minimal.
Conclusion
Due to the immediate stabilization of the lesion aftercare becomes facile. This method allows prompt mobilization and early weight bearing without the necessity of a plaster cast. Further it prevents effectively the most common complication, a re-fracture or a pathologic fracture. Therefore we propose this surgical procedure as the treatment of choice for unicameral bone cysts in children's long bones.
Introduction
Unicameral bone cysts are a common bone lesion in children. First described by Virchow in the nineteenth century, several etiologies for the pathogenesis have been discussed including intramedullary entrapped synovial tissue [1], localized failure of ossification [2] or venous blockage leading to restrained blood supply [3, 4]. Commonly the lesion is found in the proximal part of the femur and humerus at the age of skeletal immaturity. The majority of unicameral bone cysts in the humerus is diagnosed in the event of a pathologic fracture [5]. The main goal of treatment is prevention of pathologic fractures and support of the healing process.
While earlier wide resections with or without the combination of bone grafts were performed, current concepts are based on less invasive and less aggressive treatment strategies [6]. Intramedullary nailing offers prompt stabilization of the lesion through a standardized operation technique and allows early mobilization. Plaster casts are not needed. A variety of other treatment options such as bone grafting, steroid and bone marrow injections or percutaneous drillings have been described, but were reported with recurrence rates up to 40% [7–9].
The current study presents our results of flexible intramedullary nailing of unicameral bone cysts in children's long bones.
Materials and methods
Twenty-two children with unicameral bone cysts of the humerus or femur were treated surgically with the standard technique of flexible intramedullary nailing of long bones [10]. Localization of the humeral cyst was in 14 cases the proximal third and in 2 patients the diaphysis, respectively. Ten were adjacent to the humeral epiphysis. The femoral cysts were either located in the pertrochanteric (three cases) or subtrochanteric region (three cases). In 13, cysts were discovered in the event of a pathologic fracture, while 8 lesions were detected in radiographs for local pain or sprains. One cyst was diagnosed incidentially. In all cases the diagnosis was confirmed histologically. The average interval between diagnosis and surgery was 9 days. Fifteen patients were referred to our clinic after being treated conservatively in another institution. Mean follow-up after surgery was 24 months (range 12–38). Prior to surgery parents provided informed consent to participate in the study, which was approved by the research committee of the institution.
Surgical technique
Through a minimally invasive approach cortical bone was exposed and the bone biopsy obtained under fluoroscopic control. We forbore from additional curettage and steroid infiltration of the lesion since to our knowledge there is no evidence of increased healing rates for such procedures in combination with intramedullary nailing.
After reduction of the pathologic fractures flexible titanium pediatric nails (Synthes®, Bettlach, Switzerland) were inserted in retrograde fashion in all cases, consistent with the classic surgical technique first described by Métaizeau et al. Prior to wound closure stability of fixation was checked under the image intensifier. Finally care was taken to reduce any subcutaneous prominence of the implants.
Postoperative management
Weight bearing was allowed depending on the stability. In case of a pathologic fracture of the femur non-weight- bearing walking was started during the hospital stay. Humeral lesions were treated with progressive mobilization the 1st day after surgery. Plaster casting was not used in any case. Even in metaphyseal humeral lesions two retrograde inserted nails provided sufficient biomechanical stability to allow mobilization without further external protection. Sports were permitted as soon as healing of the fracture was observed. Clinical and radiographic controls were performed at 6 and 12 weeks and further after 6–12 months. We used the following criteria described by Capanna et al. [11] to classify bone cyst healing: (1) healed, cyst completely filled with bone; (2) healed with small residuals of radiolucencies; (3) recurrence of an initially healed cyst with increasing signs of radiolucencies and cortical thinning; (4) no response after surgery.
Results
Out of the 22 unicameral bone cysts treated with intramedullary nailing 16 were located in the humerus and 6 in the femur. The average interval between diagnosis and operation was 9 days. Mean age at the time of surgery of the 15 male and 7 female patients was 9 years (range 6–15). Thirteen patients were presented in the event of a pathological fracture (Fig. 1). All cases were histologically confirmed.
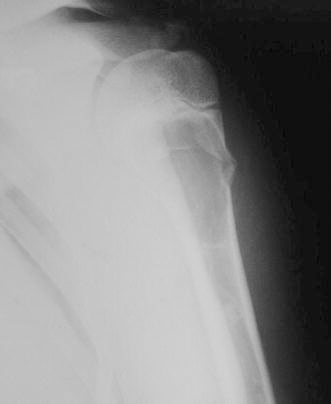
A 12-year-old boy with a pathologic fracture of the proximal humerus after a fall from the skateboard on his left shoulder. The roentgenogram reveals the cortical lesion in the lateral area of a unicameral bone cyst
According to the Classification of Capanna [3] 16 unicameral bone cysts healed completely within 14 months (Fig. 2). Four lesions were classified as grade 2, meaning that residual radiolucency was observed radiographically at last follow-up. Two recurrences were seen 16 and 18 months after initial treatment when the nails were still in place. These two patients are still followed clinically and radiographically on a regular basis.
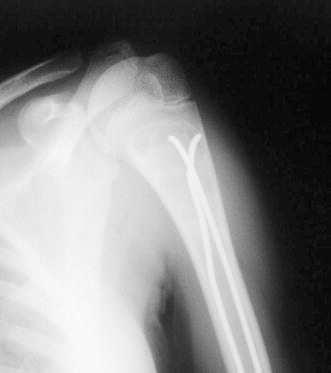
Roentgenogram of the same patient as in Fig. 1. Twelve months after elastic stable intramedullary nailing complete healing of the fracture and the unicameral bone cyst is observed
There was no case where flexible intramedullary nailing showed no effect of treatment (grade 4).
In the group of 15 patients who were referred to our institution after failed conservative treatment, 4 presented a pathological fracture and 2 an unicameral bone cyst without cortical lesion. Results of these referred patients are summarized in the numbers above.
In ten patients implants were removed after a mean of 21 months (range 19–23) postoperatively.
Final radiographic controls revealed no deformity greater than 5° in saggital and frontal planes. The complication rate was minimal and included superficial infection at the nail entry site, which was treated locally and by means of oral antibiotics in six cases. The mean hospital stay was 4 days.
Physeal damages could be prevented in all cases by following the standard insertion technique. Growth of the operated bone was found to be normal in all patients postoperatively. Until the latest follow-up no patients had sustained a re-fracture or a new pathologic cortical lesion. Neither deep infection nor neurovascular injuries occurred.
Discussion
Unicameral bone cysts are associated with pathological fractures in up to 75% [12]. The healing potential of the cyst has been reported to be higher after a fracture, but complete cure can only be expected in about 10% [5].
Earlier performed wide resections have been abandoned due to high morbidity rates of this surgical technique [6]. Further surgical treatment options include curettage and bone grafting or intralesional steroid injection. Farber reported in a series of 59 patients a healing rate of 53% when treated with curettage and bone grafting compared to 70% when treated with steroid injection [7].
Steroid injections were first described by Scaglietti et al. [13, 14] who reported a success rate of 90%. Recurrence of the cyst following intralesional steroid injection is as high as 13%, and treatment requires most commonly several injections [8, 9, 14].
In a series of 79 patients where steroid injections were compared with injection of bone marrow, no advantage of one or the other method could be shown [9]. A more recent report from Rougraff et al. [15] followed 23 patients after percutaneous injection of a unicameral bone cyst in the humerus or femur with demineralized bone matrix combined with autogenous bone marrow. After an average of 5 weeks patients reported significant pain relief, and return to unrestricted activities was noted after 6 weeks. In all but five cases only one injection was needed to achieve healing, which is a remarkable difference to fewer reports of corticosteroid injections where up to six interventions had to be performed [14].
The concept of decompression of the cyst's cavity was introduced by Cohen in 1960 [3] and is based on the hypothesis that venous obstruction leads to intramedullary accumulation of interstitial fluid and later cavity formation. Depending on the location of the bone cyst different methods in order to achieve decompression have been performed using K-wires, cannulated screws or flexible intramedullary nails [16, 17].
In 2000 Roposch et al. [17] reported a success rate of 94% with intramedullary nailing for 32 unicameral bone cysts. Two recurrences were noted after initial healing.
A French study compared steroid injections with intramedullary nailing for solitary bone cysts and disclosed no difference in terms of healing time, but a higher complication rate in the steroid injection group [18]. They concluded that intramedullary nailing should be preferred in weight-bearing segments.
It is unclear if insertion of the nails and consecutive decompression of the cyst may lead to migration of pathological tissue, provoking recurrences. After clinical and radiographic evaluation of the 22 cases of this series, we have no evidence to support this theory.
Our study confirmed the proposed benefits of flexible intramedullary nailing. The results of this series is consistent with those described in the literature. Shortcomings of our study are the smaller patient number and shorter follow-up as well as the lack of a control group treated with another technique.
Elastic stable intramedullary nailing offers primary definitive treatment of the unicameral bone cyst and can be achieved with a safe and standardized technique. Internal stabilization offers immediate mechanical stability and early weight bearing of the affected segment while the cyst is decompressed. Aftercare becomes generally facile, which we consider to be an important factor in the setting of low educational and socioeconomic status of our patients. Healing rates in our study are consistent with those reported in the literature [17, 18]. No re-fracture was detected after intramedullary stabilization.
Conclusion
Flexible intramedullary nailing is an effective and safe procedure for the treatment of unicameral cysts in the humerus and femur. Facile aftercare, low morbidity and effective prevention of refracturing make it the treatment of choice for this kind of lesion in our service in a so-called developing country.
