Abstract
Purpose
In this study, we investigated the outcome of Legg-Calve-Perthes disease in children presenting under 6 years old. Firstly, we wished to know the outcome in terms of femoral head deformity in this age group. Secondly, we investigated the potential for improvement in femoral head deformity with growth and remodelling after the Perthes lesion had healed. Thirdly, we assessed the ability of Herring's lateral pillar classification to predict femoral head deformity in this age group.
Methods
The outcome in this group was assessed using Stulberg's classification of femoral head deformity and compared to that for older children with Perthes seen at our institution over the same period. To investigate the potential for improvement of Stulberg grade with growth we assessed the hips at the stage of final healing (Waldenstrom IV) and again at skeletal maturity. To assess whether Herring's classification of lateral column collapse is predictive of deformity at this age we recorded the Herring class A, B or C at the time of maximum fragmentation and compared this to Stulberg grade.
Results
Out of a total of 127 children (131 hips) seen at our institution, 67 children (69 hips) presented before the age of 6 years. The number of Stulberg III and IV hips was 14 (20%) and 10 (15%), respectively. Chi-squared test of age against outcome confirmed that the younger children overall had a better outcome (P < 0.001). Stulberg grade did not improve predictably after the stage of final healing. Twenty-three hips graded as Stulberg III and IV at Waldenstrom IV were reassessed at skeletal maturity. Three changed from Stulberg III to IV and five changed from Stulberg IV to III, but none had improved to Stulberg I/II. Herring's classification was predictive of outcome, with 96% of Herring A hips having Stulberg I or II outcome, 61% of Herring B hips having Stulberg I or II outcome, while 60% of Herring C hips (18 hips) had significant femoral head deformity, and 10 hips Stulberg III and 6 hips Stulberg IV.
Conclusions
Perthes in children presenting before 6 years of age can result in significant femoral head deformity which does not predictably improve with time. The risk of a poor outcome can be predicted by Herring's classification of lateral pillar collapse.
Introduction
The purpose of this study was to assess the outcome of Perthes’ disease in children presenting under the age of 6 years of age and to examine the validity of Herring's lateral pillar classification in predicting the likelihood of femoral head deformity in this age group.
Outcome was assessed using Stulberg's classification of femoral head shape. Outcome was recorded at the stage of final healing (Waldenstrom's stage IV) and repeated at skeletal maturity to discover if there was any significant change in femoral head shape with growth.
We compared our results with recently presented series from Dimeglio and Herring and drew conclusions over the best predictors of significant femoral head deformity in this age group. In this study, we confirm that Lateral pillar C hips do not necessarily have a good prognosis in the child presenting under 6 years of age.
Materials
A total of 127 children (131 hips) were seen at our institution from 1983 to 2003. Of these, 67 children (69 hips) were under the age of six years of age at presentation; none of these children were treated surgically for containment, but some were treated with Atlanta brace. The older groups were often treated surgically at differing stages of Perthes and with a variety of interventions (8/29 of age 6–8 years and 18/33 of age 8 and over). Operations included Salter's innominate osteotomy with or without varus osteotomy of the proximal femur, proximal femoral osteotomy alone; varus, valgus, Cheung and Sugioka type osteotomies and Shelf acetabuloplasty; the choice depending on the aim of surgery; containment or reconstruction and also the preference of the treating surgeon.
Methods
Age at onset of Perthes’ disease was obtained from clinical notes.
A single observer used standard antero-posterior pelvic radiographs for all data collection. Herring's lateral pillar classification [1] was recorded at the stage of maximal epiphyseal fragmentation. We did not include Herring's recent introduction of an intermediate subgroup B/C as data was collected prior to this publication [2]. Femoral head deformity was assessed using Stulberg's classification [3], distinguishing between grade III (Fig. 1) and grade IV (Fig. 2) by the presence of 1 cm or more of flattening of the femoral head. Stulberg's classification was used twice. Firstly at Waldenstrom's stage IV of final healing (all hips) and secondly at skeletal maturity (all except six children who were not yet skeletally mature). Twenty-three hips (23/24) graded as Stulberg III or IV and presenting before age 6 were skeletally mature at the time of the study and we were therefore able to assess change in Stulberg's classification with growth in these young children.
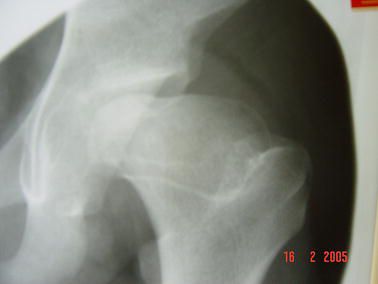
Deformed femoral head classed as Stulberg III
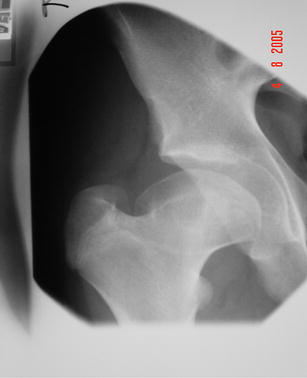
Deformed femoral head classed as Stulberg IV
Statistical methods
Continuous data were presented in the form of mean and associated standard deviations, and categorical data were presented in the form of percentages. Differences with respect to continuous variables were assessed using t tests when normally distributed. Assumptions pertaining to normality were also taken into consideration and, when violated, non-parametric statistics were applied. Association between categorical data was assessed using chi-squared statistics and when expected frequency counts were <5 then Fisher's exact statistic was used. A P value <0.05 was considered to depict a significant difference and all analysis were conducted using SPSS 12.0.
An analysis of numbers needed to treat for the Herring C hips is included.
Results
A total of 127 children (131 hips) were studied. The age at presentation ranged from 16 months to 13 years with a mean age of 6 years (SD = 2.5). Male to female ratio was 4:1. The age range at presentation for males was from 18 months to 13 years with mean age of 6 years (SD = 2.5) and for girls from 16 months to 11 years with mean age of 6 years (SD = 2.3). Sixty-seven children (69 hips) were found to be under the age of 6 years at presentation. All children with active disease, multiple epiphyseal dysplasia, or history of developmental dysplasia of the hip, and all children lost to follow up were excluded from this study. Twenty-seven children (29 hips) were between the age of 6 and 8 years, and 33 children (33 hips) over the age of 8 were included. None of the hips were classed as Stulberg V. The relationship between age at onset of the disease and the resultant outcome was explored (Table 1).
Frequency distribution between age and resultant outcome (hips)

In children under the age of six, 45 hips (64%) had a good outcome with hips classed Stulberg I and II. The 14 hips (20%) classed Stulberg III and the 10 hips (14%) classed Stulberg IV had a poor outcome. In children between the age of 6 and 8 years, 10 hips (35%) had a good outcome; classed Stulberg I and II, five hips (18%) were classed Stulberg III and 14 hips (47%) Stulberg IV. Children over the age of 8 years tended to have a poor outcome with 12 hips (36%) classed Stulberg III and 17 hips (52%) classed Stulberg IV. Statistical analysis of the association between age and outcome (Table 1) using chi-squared test, produced a P value < 0.001 confirming the greater chance of a favourable outcome in the younger child. Subsequent analysis was confined to children under the age of 6 years.
Children presenting under the age of 6 years were placed into one of three groups using Herring's lateral pillar classification at the time of maximum fragmentation. This varied in time from the first radiograph obtained at presentation to 2 years post presentation with an average of 10 months after presentation. The outcome for each group at time of healing was recorded (Table 2).
Frequency distribution of Herring groups and Stulberg outcome at time of healing

The majority of hips (96%) classed as Herring Group A had a good outcome (Stulberg I/II), while hips (60%) which were classed as Group C had an average or poor outcome (Stulberg III/IV). Statistical analysis of the association between Herring group and Stulberg class, using Fisher's exact test, produced a P value <0.001.
A child with a Perthes lesion classed as Herring C was nine times more likely to develop a poor outcome (Stulberg IV) than a child with a Herring A lesion.
Stulberg's classification for 23 hips presenting under the age of 6 years, with an average or poor outcome (Stulberg III, IV), was recorded at skeletal maturity. Fifteen hips maintained the same grading as at the time of healing, while in three cases the Stulberg grading worsened from III to IV. In five cases, the Stulberg grading improved from IV to III. None of the hips improved from Stulberg III/IV to Stulberg I/II.
Discussion
Deformity of the femoral head following Perthes disease increases the likelihood of osteoarthritis in adult life. Stulberg's classification, which aims to quantify the risk of arthritis, combines two elements: firstly, the shape of the femoral head, round, oval or flat, and secondly, the presence of acetabular incongruence in the child who is too old to achieve acetabular accommodation of femoral head deformity. The rare type V hip which Stulberg found had the worst outcome in terms of risk of osteoarthritis in adulthood [3].
Herring's lateral pillar classification is predictive of final head shape and can be useful in deciding which hips should be treated surgically, in an attempt to prevent severe femoral head deformity and improve the long term outcome of the Perthes hip. For children presenting before 6 years, Perthes’ has been regarded as a benign disorder and, until very recently, studies of outcome and the predictive value of Herring's classification have tended to exclude this age group. Following a review of our cases of Perthes, it became apparent that there were significant numbers of poor outcomes in children presenting under 6 years old and we therefore undertook this study.
In our series of children who presented under the age of 6 years, 96% (25 hips) of hips in Herring group A had a good outcome (Stulberg I, II), 61% (8 hips) of hips in Herring group B had a good outcome, with only 1 hip grading as Stulberg IV, while 60% (18 hips) of hips in Herring group C had significant deformity of the femoral head (10 hips were Stulberg III and 8 hips were Stulberg IV).
Twenty-three hips with Stulberg III and IV deformity at the stage of healing were reassessed at skeletal maturity. Three hips had changed from Stulberg III to IV and five from Stulberg IV to III; none of these hips moved from Stulberg III/IV to I/II.
Two important points emerge. Firstly, the outcome in this age group, although overall better than in the older child, is not universally good and Herrings’ classification is as useful as it is in the older child in identifying which hips will develop important deformity. Comparing our data to the data for Herring C hips in Herring's original paper [1], the risk of a Stulberg IV hip is only marginally less in the under 6-year-olds compared to Herring's series of older children. Approximately one in six cases classified as Herring C will have persistent flattening of the femoral head (Stulberg IV) in our series, which is not much better than the 19% of older children with Herring C who subsequently developed Stulberg IV deformity reported in Herring's original description of the lateral pillar classification.
In our series, children under 6 years who are classified as Herring C are nine times more likely to develop a Stulberg IV head deformity than those that are Herring A, and six times more likely than Herring A and B. Therefore, Herring's Lateral Pillar classification is useful in predicting the radiological outcome in this age group.
Secondly, in our series, hips moved in both directions between Stulberg III and IV from the time of final healing (Waldenstrom IV) to skeletal maturity, but none moved from III/IV to grade II. Therefore, deformity at the stage of complete healing will not predictably improve with subsequent growth and may even deteriorate. We therefore suggest that Stulberg's classification can be useful in providing prognostic information at the time of completion of healing, but is not as predictive as at skeletal maturity. We did note, however, that some improvement in femoral head shape with growth was reported in younger patients in a previous paper of Herring's [4].
The recognition of poor outcome in the young child is not a new finding and has been well documented in several studies [5–8]. However, the use of Herring's classification in this age group has not been reported until recently.
Dimeglio and Canavese presented a series of 166 hips to a Pediatric Society of North America (POSNA) meeting (Ottawa, Ontario, Canada, 13–15 May 2005) comparing Catterall class with Stulberg outcome. All 50 cases of Catterall 1 and 2 hips were Stulberg I/II at maturity and 9 of 51 Catterall 4 hips were Stulberg IV at maturity. Surgical versus non-surgical treatment had no influence on outcome.
Herring also presented 166 hips to a POSNA meeting the following year (San Diego, Calif., U.S.A., 2–6 May 2006) comparing his modified classification with Stulberg outcome. Unfortunately, it is not possible to directly compare the series as the distribution of Stulberg III/IV for Herring group B/C was not defined in the published abstract. However, the predictive value of the classification is clear with 104 out of 110 hips graded Herring A or B having Stulberg I/II outcomes and 27 out of 56 hips graded Herring B/C or C having Stulberg III or IV outcomes. Again, Herring's series did not show any improvement in Stulberg class comparing surgical with non-surgical treatment.
Comparing the numbers of Stulberg I–IV hips between the three series shows a slightly greater prevalence in our series of the higher Stulberg classes (Table 3). The range of prevalence was 65–77% Stulberg I/II and 7–14% Stulberg IV for the three sets of data.
Prevalence of Stulberg class in three series of children with Perthes presenting before age 6 years

Comparing positive predictive values for each series it appears that Herring C is the best predictor of Stulberg IV outcome and also of Stulberg III and IV outcomes.
The confirmation of persistent femoral head deformity, which can be predicted using Herring's classification in this age group, raises the question as to whether surgical treatment should be considered in selected cases despite a young age at presentation. With so much uncertainty as to how to best treat children with Perthes’ at any age it is tempting to be nihilistic in the management of the younger child as the expectation is of a favourable outcome without the need for intervention. However, it is now clear that not only are some children presenting before 6 years going to develop significant deformity of the femoral head, but that the risk of this can be stratified using Herring's or Catterall's system of classifying the extent of head involvement.
However, confounding factors need to be considered before advocating surgical treatment.
Firstly, treatment may be unnecessary because of acetabular remodelling and accommodation of the deformed femoral head, Stulberg V hip being at one end of a spectrum with the Stulberg IV hip not having the same risk of osteoarthritis in the young child as in the older child. However, theories of osteoarthritis as a result of impingement would suggest that a deformed femoral head is unlikely to have normal longevity despite adaptive subsequent acetabular development.
Secondly, surgical treatment in the young child may be ineffective, although it would be difficult to understand why this should be the case as treatment by containment should if anything be aided by subsequent acetabular remodelling and, hence, would be expected to be more effective in the younger child. Should treatment be offered to this group of patients? Neither Herring nor Dimeglio found any difference in outcome comparing surgical and non-surgical treatment. It may be that conventional surgical treatment is not helpful in these younger children, but the expectation of a good result may have confounded the possible benefit of surgical intervention in the more severely affected cases (Herring C) and, as clearly shown by Joseph [9] in older children, the efficacy of surgical treatment is related to the timing of intervention. It may be that it was already too late to attain benefit from surgery by the time a decision to treat had been made in these young children. Although it is noted that some of Herring's cases received treatment before full fragmentation.
While the results of these three studies clearly do not advocate surgical intervention in young children, it is now possible to identify a subgroup of children presenting with Perthes’ before the age of 6 years who are at increased risk of significant femoral head deformity. If it were assumed that treatment was effective in preventing a Stulberg IV hip and all Herring C hips were treated in our series, a ‘numbers needed to treat’ (NNT) analysis requires 3.7 (100/27 = 3.7) patients to be treated to prevent each Stulberg IV outcome, as only 27% of Herring C hips developed Stulberg IV deformity.
If early intervention is defined as surgery before the lateral pillar has collapsed, then the benefit of early intervention would be significantly reduced by the need to treat all cases to prevent deformity which would occur in a small minority of cases if no treatment were offered. NNT analysis then requires 6.9 patients to be treated to prevent each case of Stulberg IV deformity (100/14.5 = 6.9) as only 14.5% of all cases developed Stulberg IV deformity.
To progress the treatment of Perthes’, we will need to identify cases at risk of significant deformity at an early stage and offer treatment which is low risk but effective in preventing femoral head deformity.
The declaration of a hip as a Herring C on plain radiographs takes time; 10 months on average in our series. Studies of Magnetic Resonance Imaging demonstrating lateral column revascularisation [10–12] have suggested that it may be possible to identify femoral heads at risk of lateral column collapse many months earlier than at present using plain radiographs.
Research into non-surgical treatments to prevent femoral head deformity by inhibition of osteoclasis with Bisphosphonate [13] or RANKL (Receptor Activator of NF-kB Ligand) inhibition [14], may in the future offer effective non-surgical treatments for Perthes'.
Clearly recommendations to alter practice at this time would be premature, but the recognition that the risk of severe femoral head deformity can be assessed using Herring's classification improves are ability to predict outcome in this age group and may become an important consideration in the formulation of future treatment protocols for children under 6 years old who present with Legg-Calve-Perthes'.
Conclusions
Herring's lateral pillar classification is useful in predicting the likelihood of developing significant femoral head deformity following Perthes’ disease in children under the age of 6 years; those classified as Herring C have nine times the risk of a Stulberg IV deformity as those that were Herring A, and six times the risk for those that were Herring A or B. The risk of developing a Stulberg IV hip deformity from a Herring C lateral column collapse is only slightly less for the child under 6 years than for the older child. Hips that are classified as Stulberg III or IV at the stage of final healing (Waldenstrom's stage IV) do not predictably improve in shape with growth and may deteriorate from the stage of final healing to the time of skeletal maturity.
Footnotes
Acknowledgements
We would like to express our gratitude to all the reviewers, particularly reviewer 2, whose most incisive comments have directed us to a much more sensible discussion and interpretation of the data.
